![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
75 Cards in this Set
- Front
- Back
|
An exaggerated ____ response often predominates in asthma.
|
TH2 (T Helper 2)
|
|
|
What is the main effector function of TH2 cells?
|
Stimulate differentiation of eosinophils
Activate B cells |
|
|
Chronic Asthma associated with allergies has 3 responses mediated by the immune system. What are they?
|
Chronic inflammation
Bronchospasm Airway hyperresponsiveness |
|
|
What are the most effective drugs for chronic tx of asthma?
|
Anti-Inflammatory
|
|
|
What is the best way to minimize systemic side effects from steroids when treating asthma?
|
Inhalation
Less systemic effects since you're targeting the lungs. Also, with inhalation you are using lower dosages |
|
|
"-one/ -lide / -nide"
|
Inhaled Corticosteroids
|
|
|
Beclomethasone dipropionate
Fluticasone Triamcinolone Flunisolide Budesonide Ciclesonide |
Inhaled Corticosteroids
|
|
|
Do inhaled corticosteroids cause bronchodilation?
|
NO!
No direct effect on muscle tension |
|
|
Inhaled Corticosteroids MOA:
|
Potentiate β adrenergic agents by:
↑cAMP and upregulating receptor level |
|
|
What is the most potent and consistently effective long termcontrol medication for asthma?
|
Inhaled corticosteroids
|
|
|
Advantage of using inhaled corticosteroids?
|
Higher local drug concentration than an equivalent dose of systemic corticosteroids
**↓ SIDE EFFECTS** |
|
|
You have started a patient on a long term asthma drug and they complain of an unpleasant taste, oral thrush, difficulty speaking and lots of coughing with worsening asthma after use... what type of drug did you give them?
|
Inhaled corticosteroid
|
|
|
What are some ways we can prevent/reduce adverse effects with the use of inhaled corticosteroids?
|
-Spacers or valved holding chambers
-Rinse and spit after inhalation -Use short acting β2 activator before inhalation --> prevent bronchospasm |
|
|
"Predniso"
|
Oral Systemic Corticosteroids
|
|
|
Prednisone
Prednisolone Methylprednisolone |
Oral Systemic Corticosteroids
|
|
|
Why do you want to minimize the dose of oral steroids?
|
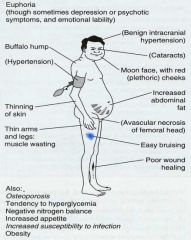
Adverse Effects
|
|
|
When would you use oral systemic corticosteroids for asthma?
|
-Moderate to severe exacerbations of asthma (3-10 days to control severe cases)
-Used for long-term control ONLY in the MOST SEVERE, difficult to control cases (must minimize the dose) |
|
|
What can be used/done to block/inhibit the mediators of mast cells?
|
Prevent Mast Cell Degranulation
Prevent IgE from binding to Mast Cell Block Leukotrienes |
|
|
"Crom"
|
Mast Cell Stabilizers
|
|
|
Cromolyn
Nedocromil |
Mast Cell Stabilizers
|
|
|
MOA of Cromolyn?
Mast Cell Stabilizer |
Prevents degranulation and the relase of mediators
*↓Histamine *↓Leukotriene *↓Cytokines |
|
|
Which Mast Cell Stabilizer affects a broader range of inflammatory cells?
|
Nedocromil
|
|
|
Would cromolyn reverse acute bronchospasm?
|
NO!
|
|
|
Side effects of Mast Cell Stabilizers?
|
Irritate the throat
-Cough -Transient bronchospasm Nedocromil--> unpleasant taste |
|
|
How can you prevent/modify the action of leukotrienes?
|
Affect conversion of Arachodonic Acid to Leukotriene
Inhibit LT1 receptors |
|
|
"-leu/luk"
|
Leukotriene Modifiers
|
|
|
"leu"
|
Leukotriene Modifers
-Zyleutron **Inhibit leukotriene production** |
|
|
"luk"
|
Leukotriene Modifiers
-Montelukast -Zafirlukast **Block LT1 receptor** |
|
|
Which Leukotriene modifiers block the LT1 receptor?
|
-Montelukast
-Zafirlukast |
|
|
Which leukotriene modifier inhibits leukotriene production?
|
Zyleutron
|
|
|
Anti-IgE therapy drug?
|
Omalizumab
|
|
|
What is omalizumab?
|
Recombinant humanized monoclonal antibody to IgE
**Anti-IgE Therapy** |
|
|
When treating with omalizumab, is there allergen induced activation of mast cells?
|
No
|
|
|
What is an adverse side effect of omalizumab?
|
Anaphylaxis
|
|
|
Mast Cell stabilizers are ___ line for Asthma
|
2nd line
|
|
|
Leukotriene Modifiers are taken _____
|
orally
|
|
|
Are leukotriene modifiers good for acute asthma?
|
No
|
|
|
Which members of the population are more responsive to Leukotriene modifiers?
|
Aspirin-Sensitive Asthmatics
|
|
|
Why would montelukast reduce bronchoconstriction from aspirin induced asthma?
|
Montelukast blocks LT1 receptors that bind to leukotrienes.
|
|
|
When is omalizumab used to treat asthma?
|
SubQ injection every 2-4 weeks
Adjunctive therapy in patients with severe persistent asthma that is INADEQUATELY controlled with the combination of high dose ICS and LABAs |
|
|
What are the three classes of bronchodilators?
|
β2 agonists
M blockers Methylxanthines |
|
|
Metaproterenol
Albuterol Levalbuterol Pirbuterol Terbutaline |
Short Acting β2 Agonists
|
|
|
Salmeterol
Formoterol Arformoterol |
Long Acting β2 Agonists
|
|
|
"-meterol/-moterol"
|
LA β2 Agonists
|
|
|
M Blocker
|
Ipratropium Bromide
|
|
|
What type of β and M receptors are in the lungs? what do they do?
|
β2 --> bronchodilation
M3 --> bronchoconstriction |
|
|
Why is the use of β2 agonists considered functional/physiological antagonism?
|
β2 agonists counteract (bronchodilate) M3 bronchoconstriction
|
|
|
What drug would you use to block M3 receptors causing bronchoconstriction?
|
Ipratropium bromide
|
|
|
β2 agonists can cause palpitations, sinus tachycardia and ↑BP. Why?
|
Higher doses of β2 agonists activate β1 receptors
|
|
|
Adverse Effects
Tremor, HYPOkalemia, palpitations, sinus tachy, ↑BP |
β2 agonists
|
|
|
What is the signaling pathway by which β2 agonists cause bronchodilation?
|
↑cAMP
|
|
|
What enzyme breaks down cAMP?
|
PDE
|
|
|
"-phylline"
|
Methylxanthines
|
|
|
Theophylline
Aminophylline |
Methylxanthines
|
|
|
The chemical structure of Methylxanthine drugs closely imitates what?
|
caffeine
|
|
|
MOA: Methylxanthines
|
Inhibits PDE (especially PDE-4)
Inhibits adenosine receptors |
|
|
MOA: Methylxanthines on smooth muscle cells
|
↑cAMP ---> block adensoine receptors
** smooth m. RELAXATION** |
|
|
MOA: Methylxanthines on T cells, Eosinophils and Mast Cells
|
↑cAMP --> block adenosine receptors
**Anti-inflammatory** |
|
|
Problems with methylxanthines
|
Narrow TI
Erratic bioavailability |
|
|
Are problems with CNS stimulation from methylxanthine use more common in children or adults?
|
Children
|
|
|
Adverse Effects
-Irritate GI mucosa -CNS Stimulation -CV effects |
Methylxanthines
CV and CNS problems stem from Caffeine-like effects |
|
|
What is the drug of choice for treating ACUTE asthma symptoms and exacerbations?
|
Short Acting β2 Agonists
|
|
|
What is the drug of choice for preventing excercise-induced asthma?
|
Short Acting β2 Agonists
|
|
|
What drug is adminstered with SABAs in moderate to severe asthma cases in the ER?
|
ipratropium bromide
(M blocker) |
|
|
Are LABAs recommended to treat acute asthma attacks?
|
NO
|
|
|
Longterm Asthma Therapy
-used adjunct to corticosteroids -may be used before excercise - not recommended as a monotherapy for long-term, persistent asthma -not recommended for acute asthma attacks |
LABAs
|
|
|
Which Methylxanthine drug can be used as an alternative, but not preferred, adjunctive therapy with inhaled corticosteroids for long-term control of moderate or persistent asthma?
|
Theophylline
|
|
|
What are the "quick relief" drugs for asthma?
|
Inhaled SABAs, M blockers -->bronchodilate
Systemic corticosteroids --> anti-inflammatory |
|
|
What drugs can be used long-term for anti-inflammatory effects to treat asthma?
|
-Inhaled Corticosteroids
-Leukotriene Modifiers -Mast Cell Modifiers -IgE-Antibodies |
|
|
What drugs can be used long-term for bronchodilation to treat asthma?
|
LABAs
Methylxanthines |
|
|
Corticosteroids don't work well for COPD. Why?
|
Corticosteroids don't really affect PMNs.
COPD is mostly a PMN-mediated problem |
|
|
Are anti-inflammatory agents useful for COPD?
|
No, don't affect PMNs
|
|
|
What drugs are useful for acute attacks of COPD?
|
SABAs
**If prompt bronchodilation doesn't occur, ADD AN M BLOCKER** |
|
|
What drugs are useful for management of Stable COPD?
|
β2 Agonists
M-blocker Methylxanthine **These are Bronchodilators** |
|
|
When should you use corticosteroids in treating COPD?
|
Add inhaled glucocorticoid to bronchodilator tx for more severe symptomatic COPD (chronic therapy)
Systemic glucocorticoids for acute attacks of COPD |

