![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
25 Cards in this Set
- Front
- Back
|
Your patient is a 23-year-old female who presents to your clinic with a:
profuse vaginal discharge, with burning, itching, and chafing. The exudate is slightly green and bubbly. The vaginal mucosa is mildly hyperemic with multiple punctuate lesions on the cervix. A drop of the exudates was examined microscopically which revealed parasites with jerky motility . . . |
Dx:
Trichomonas vaginalis |
|
|
What do Trichomonas vaginalis look like on micro?
|
Trichomonads are globular-like parasites,
slightly larger than a leukocyte, 3 - 5 flagella on the anterior side, an undulating membrane, and a single oval nucleus. |
|
|
In what form are trichomonas found?
|
appear ONLY IN THE
TROPHOZOITE FORM. (i.e., no cysts) ****EXAM |
|
|
the most common curable STD in young, sexually active women
|
Trichomonas vaginalis
|
|
|
Is co-infection with other STDs and trichomonas common?
|
Co-infection with other STDs is common so infection with Trichomonas may indicate high-risk sexual behavior
|
|
|
Do young women usually show signs or symptoms if they are infected with trichomonas?
|
Perhaps 50% of infected females are asymptomatic at the time of diagnosis, but go on to develop vaginitis within 6 months
|
|
|
When will symptoms usually show when a women contracts trichomonas?
|
appear in women within 5 – 28 days of exposure.
|
|
|
How long will symptoms last once infected with trichomonas?
|
Symptoms may persist for weeks or months
|
|
|
How are men affected by Trichomonas?
|
Males are usually asymptomatic,
but infections may affect the prostate and urethra, displaying a thin discharge |
|
|
What are clinical manifestations seen in a women who contracted trichomonas?
|
• frothy yellow/green vaginal discharge (occasionally a bad odor)
• vulvar itching or burning • dyspareunia (pain during the sexual act) and dysuria • Colpitis macularis (strawberry cervix)****EXAM is the finding of punctate hemorrhages and occasionally vesicles or papules on the cervix • elevated vaginal pH (> 4.5) with increased neutrophils |
|
|
What are some complications of trichomonas?
|
increased risk of HIV infection, preterm delivery and other pregnancy problems
|
|
|
How do you Dx Trichomonas?
|
*identification of the motile organisms in the genital tract:
*usually done with a wet mount preparation examined under the microscope. *****WET MOUNT More sensitive detection tests include: culture, rapid antigen detection kits, and use of nucleic acid probes |
|
|
What is the DOC for Trichomonas vaginalis?
|
Oral metronidazole (Flagyl)
is a highly effective treatment, with simultaneous treatment of sexual partners. |
|
|
Who should you give Metronidazole to?
|
Oral metronidazole (Flagyl) is a highly effective treatment,
******with simultaneous treatment of sexual partners. EXAM |
|
|
Why do you give Metronidazole?
|
This is necessary to prevent re-infection
|
|
|
What is an alternative DOC for trichomonas?
|
Tinidazole
may be an alternative drug |
|
|
How are trichomonas and HIV related?
|
Trichomoniasis may increase susceptibility to HIV infection
|
|
|
A young adult female presented with a profuse white vaginal discharge, associated with burning, itching and chafing. She admitted to recently having unprotected sexual intercourse.
|
A what.....
oh no she didn't |
|
|
The inflammatory exudate was slightly yellow/green and bubbly.
There may be a strong odor associated in some cases. |
Vaginal Mucosa:
1. Strawberry” appearance – from punctate hemorrhages 2. Postcoital bleeding can occur. |
|
|
The inflammatory exudate was slightly yellow/green and bubbly.
|
There may be a strong odor associated in some cases
|
|
|
next you look at the vaginal mucosa and find....
|
“Strawberry” appearance – from punctate hemorrhages
& Postcoital bleeding can occur. |
|
|
A drop of exudate was examined microscopically and it showed parasites with jerky movements, undulating membrane and flagella.
|
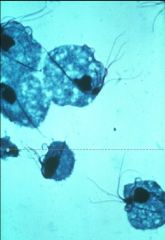
|
|
|
How should you manage this pt?
|
Treat patient with metronidazole
Little or no immunity develops, so re-infection is common Notify and treat sexual partner(s) to prevent re-infection Patients should avoid sexual intercourse until asymptomatic |
|
|
How is this disease transmitted?
|
Sexual intercourse. ****EXAM
There is little evidence for other modes of transmission. |
|
|
What counseling would you give a female patient with trichomoniasis
|
Protected sex.
Also have sexual partners tested and treated*****EXAM |

