![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
209 Cards in this Set
- Front
- Back
|
what characterizes acute nephitic syndrome?
|
hematuria, HTN, some proteinuria may be present
|
|
|
what characterizes acute nephrotic syndrome?
|
MARKED PROTEINURIA, hypoabluminemia, edema, hyperlipidemia, lipiduria
|
|
|
what is the character of acute renal failure
|
acute onset azotemia with oliguria or anuria
|
|
|
What is the character of chronic renal failure?
|
prolonged uremia
THIS IS THE END RESULT OF ALL CHRONIC RENAL DISEASES so eventually all diseases that cause renal pathology for long period of time will eventually lead to chronic renal failure |
|
|
What can be caused by renal tubular defects
|
polyuria, nocturia, electrolyte disorders
|
|
|
what is azotemia?
|
elevation of blood urea nitrogen and creatinine
|
|
|
what causes azotemia?
|
decreased GFR
-hypoperfusion(prerenal) -urninary outflow obstuction below level of kidney(postrenal) |
|
|
what is prerenal azotemia?
|
azotemia caused by hypoperfusino
|
|
|
what is post renal azotemia
|
azotemia caused by urninary outflow obstuction below level of kidney
|
|
|
what is Uremia?
|
azotemia associated with a constellation of signs and symptomss seen in mnay organs
ie. mental status change due to increased blood urea nitrogen hallmark of chronic renal failure |
|
|
What is considered diminished reserved for the kidney
|
50% GFR
|
|
|
what is considered insuffieciency of the kidney
|
20-50% GFR
|
|
|
what level of GFR is considered failure?
|
less than 20%
|
|
|
what level is considered endstage renal failure
|
less than 5%
|
|
|
what three tests are used on kidney tissue after a core needle biopsy
|
light microscopy eval
immunoflourescence electron microscopy |
|
|
what is the concept behind immunofluorescense testing of kidney biospy
|
many renal disease have antibody in glomeruli
antiantibody tags are used to find these and will light up if present looking for IgG, IgA , IgM, C3, C1q, C4 normal kidneys are Immunoflourescent negative |
|
|
what are the 5 type sof glomerular syndromes
|
acute nephritic syndrome
rapidly progressive glomerulonephitis nephrotic syndrome chronic renal failure asymptomatic hematuria or proteinura |
|
|
what are the signs of rapidly progressive glomerulonephritis?
|
acute nephritis, proteinuria and acute renal failure
|
|
|
what is the required amount of proteinuria to be classified as nephrotic syndrome
|
greater than 3.5gm
|
|
|
which is more common oliguria or anuria in nephrotic syndrome?
|
oliguria
|
|
|
what is characteristic about hypternsion in nephritic syndrome
|
its classically transient
|
|
|
what are the most important diseases that fall under nephrotic disease
|
minimal change disease(lipoid nephrosis)
focal segmental glomerulosclerosis(FSGS) Membranous nephrophathy Membranoproliferative glomerulonephritis(MPGN)- can have BOTH NEPHRITIC AND NEPHROTIC presentatino less important: IgA nephropathy fibrillary GN vs immunotactoid GN secondary glomerulonephritis related to systemic disease |
|
|
what are some example of systemic disease that can cause secondary glomerulonephritis
|
diabetes
amyloidosis SLE drugs infection malignancies |
|
|
what is the peak incidence of minimal change disease?
|
2-6 years
causes 65% of nephrotic children 10% of nephrotic adults MOST COMMON CAUSE OF NEPHROTIC SYNDROME IN CHILDREN |
|
|
what does minimal change disease often follow?
|
respiratory infectinon or vaccination
|
|
|
what type of proteinura is found in minimal change disease
|
Albumin
only albumin |
|
|
what is minimal change disease respond best to
|
steroid treatment
overall good prognosis |
|
|
what are the characteristics of MCD(minimal change) under light microscopy
|
normal glomeruli, tubulointerstiium and blood vessels
proximal tubules may contain lipid Possible lipoid nephrosis |
|
|
what is seen on IF for MCD
|
nothing
|
|
|
what is seen on EM for MCD
|
diffuse foot proccess effacement microvillous and microcystic change no granular electron dense deposit(no immunoglobins)
|
|
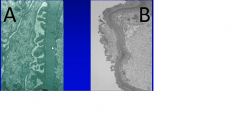
What is the disorder shown in picture B, A is normal
|
B shows foot process effacement indicitave of minimal change disease.
|
|
|
discribe the epidemeology of focal segmental glomerlosclerosis
|
any age less common in children
10% of nephrotic kids 35% of nephrotic adults -most common cause of nephrotic syndrome in US adults More common in black and hispanic populations |
|
|
what can cause focal segmenteal glomerulosclerosis?(FSGS)
|
idiopathic
IgA nephropathy glomerular scarring loss of renal mass heroin abuse HIV infection, obesity Inherited mutation of podocyte protiens(podocin, alpha actinin) or slit diaphram proteins(nehprin) |
|
|
where is teh primary glomerular lesion in FSGS
|
visceral epithelial damage (foot processes)
|
|
|
what are some differences btw MCD and FSGS
|
FSGS
-nonselective proteinuria -hematuria more likely -reduced GFR -hypertension -poor response to steriods -poor prognosis -positive EF MCD -no hematuria -only albumin -good resoponse to steroids -good prognosis |
|
|
Can FSGS respond to steroids?
|
sometimes, but if it does than patient will need to take steroids for life.
|
|
|
Can FSGS be cured by kidney transplant
|
not always
FSGS may recur with rapid proteinuria occurin after trasnplantation suggests root problem no in the kidneys |
|
|
what occurs in FSGS
|
focal(not all glomeruli) segmental(only a portion of the glomerulus) sclerosis
hyalinosis- (deterioration of glomerular and arteriolar) glomerular and interstitial foam cells increased mesangial matrix with eventual tubular atrophhy and interstitial scarring |
|
|
what is found on IF for FSGS
|
segmental IgM and C3
|
|
|
what will be seen on EM for FSGS
|
similar to MCD you will see foot process effacement microvillus change
you will also see cytoplasmic cysts focal detachment of epithelial cells and sclerosis |
|
|
what are two histologic variants and their meaning for prognosis? FSGS
|
Tip lesion only- good prognosis
collapsing variant - very bad |
|
|
what is associated with collapsing variant FSGS
|
can be idopathic but is a characteristic finding of HIV nephropathy
HIV nephropathy demonstrates sclerosis of the entrei glomerulus in addition ot endothelial tubuloreticular inclusions on EM more common in blacks |
|
|
what is the cause of membranous glomerulopathy?(MN)
|
85% idiopathic
thought to be an autoimmune disease linked to susceptibility genes and caused by antibodies to renal autoantigen 15% is secondary to visceral malignancy, lupus, mucury exposure, drugs, infection or metabolic disorders |
|
|
Who is most affected by MN
|
30% of nephrotic disease in adults
5% in children |
|
|
what is the course of membranous glomerulopathy(MN)
|
starts indolent, but poor response to immunosuppression
40% progress to renal insufficiency and 10% to renal failure |
|
|
where do immune complexes accumulate in MN
|
subepithelial side of basement membrane
|
|
|
what is seen on light microscopy in MN
|
diffuse capillary membrane thickening with SPIKES on special stains
-spikes represent basement membrane material laid down between dense deposits sclerosis and tubulointerstitial scarring |
|
|
what is seen on IF for MN
|
even, diffuse, granular deposits of IgG and C3 in peripheral capillary loops. unlike FSGS the glomerulus is visualized and the capillaries are what light up making a knotted rope appearance.
|
|
|
what is seen on EM for MN?
|
you can see the dense deposits of immunoglobins that cause the membrane to fold up creating the spiky appearance.
|
|
|
what does membranoproliferative mean?
|
membrano-thickened capillary loops
proliferative= glomerular cell proliferation |
|
|
what % of nephrotic syndrome is made up by membranoproliferative glomerulonephritis?
|
10-20% in both kids and adults
|
|
|
what is the clinical course of membranoproliferative glomerulonephritis?(MPGN)
|
slow progression without remmission
50% proceed to chronic renal failure in 10years |
|
|
can MPGN be cured by kidney transplant?
|
no high recurrnce rate in transplants especially in MPGN type II
|
|
|
what are the two types of MPGN
|
type I- majority of cases
type II- dense deposit disease |
|
|
what are the microscopic findings in MPGN
|
large hypercellular glomeruli with a lobular appearance
mesangial and endocapillary cell proliferation duplication of basement membrane = tramtack appearance occasinoal crecent formation |
|
|
what is the cause of MPGN type 1
|
immune complex medicated glomerulonephritis
-subendothelial and mesangial immune complexes that incite a proliverative/inflammatory response INVOVLES BOTH CLASSICAL AND ALTERNATE COMPLEMENT PATHWAYS any immune complex mediated GN can have a membranoproliferative pattern, so classifaiction as idiopathic type I MPGN requires ruling out all possible underlying causes |
|
|
what is the cause of MPGN type II
|
ISSUE WITH ALTERNATE COMPLEMENT PATHWAY ONLY
decreased levels of factor b and properidin 70% of patients have circulating antibody - C3 nephritic factor(C3NeF) C3NeF is a autoantibody that binds to the alternative pathway C3 convertase adn stabilizes it which protectsw it from enzymatic degradation and hypocomplementemia results due to persistant C3 degradation -C1 and C4 still found in normal levels |
|
|
what is one thing found on light microscopy in MPGN type II not found in type I
|
intramembranous riboon like deposits
|
|
|
what is found on IF for type I MPGN?
|
course granular C3, IgG, sometimes C1q and C4 along capillary loops
|
|
|
what is found on IF for type II MPGN?
|
irregular granular or linear foci of C3 only in basement membranes and mesangium
not seen in dense deposits |
|
|
what is the major distinguishing factor seen on EM between Type I and type II MPGN
|
Type I shows subendothelial deposits
Type II shows intramembranous deposist |
|
|
describe secondary MPGN
|
secondary MPGN is immune complex mediated and therefore classified as type I disease
can be caused by SLE hepatitis B and C infections -endocaritis, visceral abscesses, HIV, schisotmaiasis Alpha 1 antitrypsin deficiency malignancies(lympohoma) hereditary complent deficiencies |
|
|
what are the two main catagories of nephritis
|
acute proliferative glomerulonephritis
-poststreptococcal,postinfectious rapidly progressive(crescentic) glomerulonephritis. |
|
|
what is the most common subtype of acute proliferative glomerulonephritis
|
acute post streptococcal is the most common
persistent bacterial infection can also cause a similar glomerulonephritis -infective endocarditis -deep seated abscess -infected shunts most times it will spring up 2 weeks after onset of infection |
|
|
For post streptococcal GN who is most commonly affected
|
children age 6-10 but anyone can get it
|
|
|
what is the mechanism of streptococcal GN
|
antibody mediated
follows infection of certain strains of group A beta hemolytic streptococci(12,4,1) serum complements drops serologic evidence of elevated antibodies (increased ASO titiers) |
|
|
what types of strep infection are most likely to cause post-strep GN
|
group A beta hemolytic strep strains, 12, 4, and 1.
|
|
|
what is the classic nephritic syndrome presentation
|
malaise, fever, nausea, oliguria, hematuria, red cells and casts in urine with a small amount of protein. peri orbital edema and hypterension
|
|
|
what is the classic presentation of Acute post streptocaoccal GN
|
nephritic syndrome developes 1-2 weeks after sore throat mostly in children
|
|
|
what is the prognosis for post infectious (poststrep) acute GN?
|
95% of children recover completely
|
|
|
what is seen on light microscopy for Post infectious GN
|
all glomeruli are involved
enlarged hypercellular glomeruli caused by infiltratino of neutrophils and monocytes, proliferation of enothelial and mesangial cells crescent formation in severe cases interstitial edema and tubular red blodds cell casts |
|
|
what is seen on If in post infectious GN
|
granular capilary loop IgG, IgM and C3.
much more scattered and diffuse than was seen in the nephrotic syndrome ones |
|
|
what is seen on post infectious GN on EM
|
SUBEPITHELIAL HUMPS
not uncommon to see mesangial and subendothelial deposits also |
|
|
what is the course of Rapidly progressive (crescentric) glomerulonephritis(RPGN)
|
severe glomerular injury
rapidly progressive loss of renal function and severe oliguriana dn death in weeks to months if untreated regardless of cause crescent are present in most glomeruli |
|
|
what are the there types of RPGN?
|
type 1-anti GBM antibody-20%
type 2-immune complex-25% type 3-pauci immune-50% |
|
|
what is associated with type 1 RPGN
|
goodpastures syndrome
hypersensistivity reaction |
|
|
what is associated with type 2 RPGN
|
postinfectious GN
SLE Henoch-Schonlein purpura(IgA) |
|
|
what is associated with type 3 RPGN?
|
ANCA
Wegeners granulomatosis microscopic polyarteritis nodosa/microscopic polyangitits |
|
|
discribe the characters of RPGN type I
|
antibody against glomerular basement membrane
can have cross reaction with pulmonary alveolar basement membranes presence of pulmonary hemorrhage associated with renal failure =goodpastures syndrome goodpasture antigen is a peptid within the noncollagenous portino of the alpha3-chain of collagne type IV can be treated with plasmapheresis |
|
|
what is found in RPGN type III
|
lack of anti-GBM or immune complexes
presence of antineutrophil cytoplasmic antibodies are present(ANCAs) in serum -cytoplasmic(C) -perinuclear(P) can be idiopathic or reated to system vasculitis like wegeners or MPN |
|
|
what is the fundamental finding in RPGN on light microscopy?
|
crescent formation-formed by proliferationof parietal cells and influx of macrophages/monocytes into the urinary space leading to eventual obliteration of bowmans space
|
|
|
what is seen on If in post infectious GN
|
granular capilary loop IgG, IgM and C3.
much more scattered and diffuse than was seen in the nephrotic syndrome ones |
|
|
what is seen on post infectious GN on EM
|
SUBEPITHELIAL HUMPS
not uncommon to see mesangial and subendothelial deposits also |
|
|
what is the course of Rapidly progressive (crescentric) glomerulonephritis(RPGN)
|
severe glomerular injury
rapidly progressive loss of renal function and severe oliguriana dn death in weeks to months if untreated regardless of cause crescent are present in most glomeruli |
|
|
what are the there types of RPGN?
|
type 1-anti GBM antibody-20%
type 2-immune complex-25% type 3-pauci immune-50% |
|
|
what is associated with type 1 RPGN
|
goodpastures syndrome
hypersensistivity reaction |
|
|
what is associated with type 2 RPGN
|
postinfectious GN
SLE Henoch-Schonlein purpura(IgA) |
|
|
what is associated with type 3 RPGN?
|
ANCA
Wegeners granulomatosis microscopic polyarteritis nodosa/microscopic polyangitits |
|
|
discribe the characters of RPGN type I
|
antibody against glomerular basement membrane
can have cross reaction with pulmonary alveolar basement membranes presence of pulmonary hemorrhage associated with renal failure =goodpastures syndrome goodpasture antigen is a peptid within the noncollagenous portino of the alpha3-chain of collagne type IV can be treated with plasmapheresis |
|
|
what is found in RPGN type III
|
lack of anti-GBM or immune complexes
presence of antineutrophil cytoplasmic antibodies are present(ANCAs) in serum -cytoplasmic(C) -perinuclear(P) can be idiopathic or reated to system vasculitis like wegeners or MPN |
|
|
what is the fundamental finding in RPGN on light microscopy?
|
crescent formation-formed by proliferationof parietal cells and influx of macrophages/monocytes into the urinary space leading to eventual obliteration of bowmans space
|
|
|
what is seen on IF for type I RPGN
|
linear IgG and C3 in basement membrane
|
|
|
what is seen on IF for type II RPGN
|
granular deposition-lumpy bumpy
|
|
|
what is seen on IF for type III RPGN
|
nothing
|
|
|
what is characteristic of RPGN found on EM
|
rupture of the glomerular basement membrane
|
|
|
discribe IgA nephropathy
|
most common primary glomerulonephritis worldwide
characterized by mesangial IgA deposits IF needed for definitive diagnsosis serum polyermic IgA i sincreased and circulating IgA immune complexes are present in some patients only IgA1 subclass forms the nephritogenic deposits complexed with C3 in the mesangium |
|
|
what are the similarities and differences between IgA nephropathy and infectious GN
|
both present with hematuria after some sort of infection
infectious GN is characterized by IgG IgA nephropathy is characterized by IgA |
|
|
Can IgA nephropathy be cured by kidney transplant?
|
no
|
|
|
what are the indicators for poor prognosis with IgA nephropathy
|
old age
heavy proteinura hypertension crescent formations vascular sclerosis |
|
|
what is unusual about IgA nephropathy hematuria?
|
lasts for several days and then subsides but returns every few months
|
|
|
what is seen on light microscopy for IgA nephropathy?
|
normal with slight mesangial widening and proliferation
proliferation may be segmental rarely overt crescentic GN |
|
|
what is see on IF for IgA nephrophaty
|
mesangial IgA usually codeposits with C3 can extend to loops
|
|
|
what is seen on EM for IgA nephropathy?
|
mesangial or paramesangial electron dense deposits
|
|
|
What is Henoch-Schonlein purpura(HSP)
|
ssytemic IgA mediated vasculitis
causes skin lesions over extensor surfaces of extremeties and buttocks abdominal pain, bleeding and vomiting arthralgias 1/3 get renal dsease -gross or micro hematuria, proteinuria, nephrotic syndrome -IgA deposits in teh glomerular mesangium and seen best by IF |
|
|
who gets HSP
|
most common in kids 3-8 but can occur in any age
prognosis is better in children |
|
|
What is hereditary nephropathy?
|
benign familial hematuria(thind basement membrane disease)
fairly common; alpha3 or alpha4 collagen IV affected glomerulular basement membrane is 150-250nm(normal is 300-400) asymptomatic hematuria, occasional mild proteinuria renal function is normal usually found on routine urinalysis not dangerous |
|
|
what is the syndrome of effects for alphort disease
|
recurrent micro or macrohematuria, varying proteinuria, sensorinural deafness, cataracts, lens dislocations, slow progression to renal failure
|
|
|
who is more likely to get alports
|
males affected more often and more severly than women
|
|
|
how is alports transmited
|
X-linked, autsomal dominant and recessive modes
|
|
|
what is the defect in alports
|
alpha5 chain of collagen type IV
|
|
|
what is the progression of alports
|
age 5-20 symptoms emerge
20-50 renal failure developes |
|
|
what is seen on light micro for alports
|
mesangial hypercellularity and sor scaring
usually mild, segmental tubular atrophy and interstitiual fibrosis interstitial foam cells are common |
|
|
what is seen on IF for alports
|
nothing
|
|
|
what is seen on EM for Alports
|
basemetn membrane thinning alternating with thickening, splitting of the basement membrane, lamination of the lamina densa with basket weave appearance.
|
|
|
what are some diseases that can cause problems for the kidney other than the main ones discussed
|
SLE
Diabetes-hyalinizing arteriolar sclerosis, capilllary BM thickening, mesangial sclerosis and nodular glomerulosclerosis(Kimmestiel-wilson disease) amyloidosis- usually light chain amyloid fibrillary GN- fibrillary deposits that resemble amyloid but are structually different leads to nephrotic sydnrome hematura progressive renal insufficiency recurs in transplants immunotactoid Glomerulopathy- microtubualr deposits patients often have circulating paraprotien monoclonal Ig in the glomerulus |
|
|
what is chronic glomerulonephritis?
|
the endstage form of most renal diseases of the glomerulous
glomeruli are compeltely effeaced by hyalinized connective tissue vasular sclerosis may be porminent there are widespread complications from the uremia such as pericarditis secondary hyperparathyroidism, HTN, with LV hypertorphy |
|
|
what happens when a patient with chronic glomerulonephritis gets dialysis
|
arterial intimal thickening, calcium oxalate cytstal deposition, acurided cystic disease
|
|
|
what diseases most commonly progress to Chronic glomerulonephritis
|
in order of decreases risk:
RAPID PROGRESSIVE GN focal glomerulosclerosis Membranoproliferative GN IgA nephropathy membranous GN poststreptococcal |
|
|
what are the two types of diseases that affect the tubules/interstitum
|
acute tubular necrosis
tubulointerstistial nephritis |
|
|
what is the most common cause of acute renal failure
|
acute tubular necrosis
|
|
|
what are the two types of acute tubualr necrosis
|
ischemic ATN: reversible lesion arising in settings characterized by a period of inadequate blood flow to the kidneys
toxic ATN: direct tubular injury by a variety of drugs and toxins |
|
|
what are the agents most associated with toxic type ATN
|
drugs:gentamicin, cephalosporin, cyclosporine(antibiotics)
contrast agents heavy metals(mucury, lead) organic solvents, hemoglobinuria/myoglobinuria |
|
|
where does the necrosis occur in ATN?
|
ischemic ATN-straight portion of proxima tubuel and thick ascending loop of henle
there will be patchy focal tubular necrosis with skip areas, Tubular casts occlude lumens(casts are rich in protiens) edema and accumulartion of leukocytes within vasa recta areas of epithelial regen evidenced by hyperchromatic nuclei and mitotic figures Toxic ATN- proximal convoluted tubules- similar apperance as ischemis though more diffuse |
|
|
what is seen on light micro for ATN
|
epithelial swelling
tubular casts epithelial cell sloughing regnerative mitotic fiures crystals |
|
|
what is the progression of ATN
|
initiating stage- begins with starting event
maintenance stage-persistan renal failure, oliguria hyperkalemia revovery stage: rising urine volumes; sometimes hypokalemia |
|
|
what is the prognosticator of ATn
|
nephrotoxic ATN tends to do better
septic shock related ATN has a bad prognosis |
|
|
what are the two types of tubulointerstitial nephritis
|
acute-rapid clical onset: interstitial edema, mixed leuikocytic infiltrates(neutrophils,k eosinophils, mononuclear) focal tubular necosis
chronic- mononuclear leukocyte, intetitial fibrosis, tubular atrophy |
|
|
what are some causes of tubulointerstitial nephritis?
|
infections
toxins metabolic disease chronic UTI radiation Neoplasm immunologica reaction vasular disease |
|
|
what is the key thing to remember about end stage renal disease?
|
it doesnt matter the cause glomerular loss or tubulointerstitial disease if the disease progresses to this point they will both overlap and look the same.
|
|
|
what is the cause of pyelonephritis
|
85% caused by a gram neg bacteria(fecal flora) E.Coli, klebsiella, proteus, enterobacter.
infection can come from the blood but it usually comes by ascending from lower urinary tract |
|
|
what are some risks that could predispose someone to pyelonephritis
|
obstuction(kidney stone) , cathaters, diabetes, immunospuresion, pregnancy
|
|
|
what is the presentation of acute pyelonephritis
|
flank pain, fever, dysuria, pyuria, bacteruira
|
|
|
what is the gross appearance of acute pyelonephritis
|
grayish white spots of inflammation and or abscesses
|
|
|
what is the microscopic presentation of acute pyelonephritis
|
neutrophils, tubular necrosis, tubular abscesses,
glomeruli usually spared unless really severe |
|
|
what are the three main complications associated with acute pyelonephritis?
|
papillary necrosis-mainly in diabeticsand those with urinary tract obstuction
pyonephrosis- usualy in setting of complete obstuction where pus fills renal pelvis, calycs and ureter perinephric abscess- extension of the inflammation through the renal capsule into the surrounding tissue |
|
|
how is acute pyelonephritis treated?
|
antibiotics
|
|
|
what is chronic pyelonephritis?
|
chronic tubulointerstitial inflammation leads to discrete corticomedullary scars overlying dilated, blunted, deformed calyces.
|
|
|
what are the two forms of chronic pyeloneprhitis
|
chronic obstuctive-predisposes to repreated infections-enteric bacteria
reflux nephropathy- most common cause results from supimposition of UTI on congenital vesicoureteral reflux and intrarenal reflux |
|
|
what is the appearence of chronic pyelonephritis grossly
|
irregular scarring
halmark is coarse discrete corticomedullary scar overlying dilated, blunt or deformed calyx. |
|
|
what is the microscopic presentaion of chronic pyelonephritis
|
tubualr atrophy, dilation THYROIDIZATION(colloid casts that make its look like the thyroid tissue)
|
|
|
what is the main drug responsible for acute drug induced interstitial nephritis
|
synthetic penicillins
|
|
|
what is the presentatino of acute drug induced interstitial nephritis
|
15 day after exposure to penicillin
develop fever, eosinophilia, skin rash, hematuria, mild protienuria, pyuria, sometimes acute renal failure. |
|
|
what happens in acute drugs induced interstitial nephritis MOA
|
drus acts as hapten binding a compenent of the tubular cells= becomse immunogenic cell injury mediated by IgE and or T cell mediated immune reactions
|
|
|
what causes analgesic abuse nephrophaty
|
phenacetin containing mixtures, acetominophen, aspirin, caffeine, codiene.
usually a mixture of two antipyretics |
|
|
what is the presentation of analgesic abusse nephropahty?
|
chronic tubulointerstial nephritis and rennal papillary necrosis
more common in females with recurrent headaches and muscle pains |
|
|
what causes papillary renal necrosis?
|
diabetes-numerous affected all in same stage
analgesic nephropathy-all papillae affeted different stages of necrosis sickle cell-few affected urinary tract obstuction-variable number affected |
|
|
what will be seen in multiple myeloma in the kidney?
|
bence jones proteinuria and cast nephropathy
amyloidosis light chain depsotino disease hypercalcemia and hyperuricemia |
|
|
what are the renal vasular diseases
|
nephrosclerosis
malignant HTN renal artery stensosis renal infarcts diffuse coritcal necrosis thrombotic microangiopathies |
|
|
what are the 3 examples of thrombotic microangiopathy
|
childhood hemolytic uremic syndrome
adult HUS Idiopathic thrombotic thrombocytopenia |
|
|
what are the characteristics of childhood HUS
|
follows GI or flulike symptoms
presents with ARF, oliguria, hematuria, microangiopathic hemolytic anemia, HTN, neurologic. 75% are infected with verocytotocin producing E. Coli |
|
|
what are teh characters of adult HUS
|
infection(e. coli, typoid fever, shigella) antiphospholipid syndrome, prengancy, vascular renal disease, chemo and immunosuppressant drugs
|
|
|
what are the characters of idiopathic thrombotic thrombocytopenia?
|
PENTAD: fever, neuro sx, hemolytic anemia, thrombocytopenic prupura, thrombi in gomerular capillaries/arterioles
acquired or genetic defect of ADAMTS-13 pretease that normally cleaves vWF multimers leads to enhanced platelte aggregation |
|
|
hydronephrosis is characteristic of what?
|
urinary tract obstuction
|
|
|
what is the presentation of UTO
|
unilateral obstuction silent due to compensation
bilateral obstuction presents with inabliltiy to concentrate teh urine, polyuria, nocturia, distal tubular acidosis, salt wasting, stones, tubulointerstitial nephritsis |
|
|
what are the causes of UTO
|
urethra-tumor, valve sticture
prostate-hyperplasia very common, cancer bladder- calculi, tumors, neurologic ureter- pregnancy, tumors, clots, stones, inflamation, pelvis- stone, tumor, sticture |
|
|
what is the presentation of urolithiasis
|
can arise at any level but most arise in the kidney, 80% unitlateral
males more than females 20s and 30s obstucts outflow, pain when passed into ureter, hematuri(usually from larger stones) ulceration of the affected epihelium. |
|
|
what are the four types of urolithiasis
|
calcium(70%)-radio opaque
triple phosphate/struicte stones(15-20%) staghorn calculi bacteria proteus radio density dependent on amount of calcium present uric acid stones(5-10%) associated with increased uric acid level radiolucent cystine stones(1-2%) usually a genetic defect stones fro at low urinary pH radiolucent |
|
|
what are the cystic disease of the kidney
|
cystic dysplasias
autosomal dominant PKD AR PKD medullary cystic disease aquierd cystic disease simple cysts |
|
|
what is cystic renal dysplasia
|
abnormaility in metanephric differentitation with persistnce of abnormal structures in kidney.
cartilage in the kidney, immature collecting ductules abnormal organization can be uni or bilateral often causes obstuctive problems |
|
|
AD PKD(polycytstic kidney disease) has what characteristics
|
universally bilateral
renal funtion maintained till 40s-50s presents with flank pain, draggin senstation, hematuria, proteinuria, HTN usually progress to renal failure |
|
|
what is the genetic basis of AD PKD
|
PKD1gene, polycystin 1, chromosome 16p13.3 in about 85%
-destroys cell cell and cell matric interactions PKD2gene, polycystin 2, chromosome 4q21 (10%) -integral membrane protien likley related to calcium channel permability PKD1 more severe and presents earlier |
|
|
what is AD PKD associated with
|
hepatic cytsts (40%)
cerebral berry aneurysm (5-10%) mitral valve prolapse or valve anomalies(20-25%) death by HTN or heart disease death by infection death by ruptured aneurysms |
|
|
what is the character of AR PKD
|
childhood type
classically present in the neonatal period with big cystic kidneys and renal failure poor prognosis can present at any stage of childhood |
|
|
what is the genetic basis for AR PKD
|
chromosome 6p21-23
PKHD1 gene for fibrocystin, an integral membrane protein |
|
|
what is seen on gross exam of AR PKD
|
elongated fusiform cyst present at rigth angles to cotical surface
|
|
|
what is the character of medullary sponge kidney
|
lesion consistnig of multiple cystic dilations of the collecting ducts int eh renal medulla
secondary complications -calcifaication with dilated ducts -hematuria -infection -uriniary caluculi renal function is usually normal |
|
|
what are the characteristics of familial nephronophthisis-medullary cystic disease complex
|
progressive renal disorders with onset in childhood
characterized by presence of corticomedullary cysts, though cotical tubular damage is the cause the envtual renal insufficiency this catagory is made up of several distinct genetic disorders grouped by a common patholigic feature. therefore can present AD, AR and sporadically some of the conditions are associated with other conditions |
|
|
what are the 4 varients of familial nephronophthisis-medullary cytsic disease complex
|
sporadic nonfamilial(20%)
familial juvenile nephronophthisis(50%) -AR -NPH1(nephrocystin), NPH2, NPH3 renal retinal dysplasia(15%) -AR adult onset medullary cystic disease(15%) -AD _MCKD1 and MCKD2 |
|
|
what are some common congenital abnormalities of the kidney
|
bilateral renal agenesis
-oligohydraminios, hypolastic lung, defects in extremeits (potter sequence) not compatible with life unitlateral renal agenesis renal ectopia horseshoe kidney Double ureters |
|
|
what are the benign renal tumors
|
papillary adenoma
renal fibroma angiomyolipoma oncocytoma |
|
|
what are teh malignant renal tumors
|
renal cell carcinoma
-classic clear cel -papillary -chormophobe -collecting duct urothelial (transistional cell ca) |
|
|
what is the character of papillary adenoma
|
ogigin in renal tubuels
gross-small MUST BE LESS THAN 5mm cortical encapsulated nodule microscopic-complex branching, papillomatous, clear cuboidal or polygonal cells which are free of atypia benign |
|
|
what is the character of renal fibroma(Hamartoma)
|
small gray whit tumor in teh renal pyramids
friboblastic type cells and collagenous tissue benign |
|
|
what tissue is found in angiomyolipoma
|
smooth muscle
fat thick walled vessles |
|
|
what is angiomyolipoma associated with
|
present in 25-50% of patiens with tuberous sclerosis
|
|
|
what stain is positive in angiomyolipoma
|
H and B 45 melanocytic marker
|
|
|
what is the key EM finding on oncocytoma
|
mitochondria
|
|
|
what is the gross presentation of oncocytoma
|
mahogany brown, homogenous, well encapsulated with central scar
|
|
|
what it the micro presentation of oncocytoma
|
large eosinophilic cells with small round nuclie and ample vaguely granular cytoplasm
|
|
|
what is the character of renal cell carcinoma
|
85% of renal cancers in adults
60 and 70 yo males slightly more than females arises in tubular epithelium risk factors: smoking most important obesity, HTN, unopposed estrogne, asbestos, petroleum produtis, heavy metals, chronic renal failure, acquired cystic dsease and tubserou sclerosis |
|
|
what are the three types of familial Renal cell carcinoma
|
von hippel lindau syndrome
hereditary clear cell carcinoma hereditary papilllary carcinoma |
|
|
what are the characters of von hippel lindau syndrome
|
AD
hemangioblastoma of cerebellum/retina renal cysts renal cell carcinoma genetics - short arm of chromosme 3 |
|
|
what gene is affected in Hereditary familial clear cell carcinoma
|
short arm of chrom. 3
same as VHL but only the kidney is affected |
|
|
what is character of hereditary papillary carcinoma
|
multiple bilateral tumors
MET protooncogene |
|
|
what are the gene basis of the clear cell carcinoma
|
chrome 3
most common subtype of renal cell carcinoma |
|
|
what is the gene basis for papillary carcinoma
|
trisomy 7,16,17 loss of Y tend to have better prognosis
|
|
|
what is the gene basis for chromophobe renal carcinoma
|
multiple chromosomes abnomalities and hypodiploidy, good prognosis
|
|
|
what is the gene basis for collecting duct carcinoma
|
least common subtype
chromosome losses and deletions but no specific gene known |
|
|
what is the classic triad of renal cell carcinoma
|
eostovertebral pain, palpable mass, hematuria
only seen in 10% of cases |
|
|
what is the presentation of renal cell carcinoma
|
classic triad
paraneoplastic syndrome-could cause any of a number of issues tends to metastasize widely(lungs, bones) 5 year survival 45% up to 70% with no metastaic diseaes nephrectomey treatment of choice |
|
|
what is the gross morphology of renal cell carcinoma?
|
yellowish tumor wth focal hemorrhage and necorsis, tends to invade renal vein
|
|
|
what is the micro of renal cell carcinoma
|
clear cell- solid, trabecular, tubular
cells rounded, polygonal rich think walled vascular network in septa |
|
|
what is the character of urothelial cancer of renal pelvis
|
5-10% of renal tumors
manifest earlier due to hematuria or obstuction 50% associated with bladder tumor |
|
|
how can you tell on microscopy of biopsy if urothelial cancer is present?
|
there should be 7 layers if more then its neoplastic
|
|
|
what is ureteritis follicularis
|
aggregates of lymphocyts in teh subeptihelial regions cause a slight elevation of the mucosa producing a fine granular suface
|
|
|
what is ureteritis cystica
|
presence of cysts on teh mucosal surface
|
|
|
what is seen on ureteritis
|
ureterisis follicularis
ureteritis cystica |
|
|
what is sclerosing retroperitoneal fibrosis
|
fibrosis proliferatie inflammatory process that encases teh retroperitoneal stuctures ie kidneys, resulting in hydronephrosis
AKA ormonds disease |
|
|
what is the cause and morphology of cystitis? (bladder infection)
|
cause-ecoli, proeus, enterobacter, mycobacetrial organims, candida albicans, schistosoma haematobuim, tuberclulosis
morphology gross-hypermei of mucosa sometime ulceration microscopic-nonspecific acute or chronic inflammation may be supporuatiev with exudates, chronic fiborsis is possible with chronic cysitsis |
|
|
what is the triad of symptoms for cystitis
|
frequncy/urgency
lower absominal pain dysuria |
|
|
what is associated with hemorrhagic cystitis
|
complication of cheomtherpatuic agent cyclophosphamide and adenovirus
|
|
|
what is malacoplakia
|
peculiar pattern of inflammatory reaction/cystitis related to chronic bacterial infections
|
|
|
what is the morphology of malacoplakia
|
gross-soft, yellow, slightly raised mucosal plaques 3-4cm
micro- infiltration by large foamy macrophages, occasional giant cells and lyphocytes. also see MICHAELIS GUTTMANN bodies |
|
|
what is the pathogenesisi of malacoplakia
|
related to chronic infection by e coli and prteus
defects in phagocytic or degradative function of macrophages |
|
|
what is characteristic of inverted urothelial papiloma
|
grows downward into the mucosa
benign |
|
|
what is the are the risk factors for bladder carcinoma
|
men>women
industrialized> developing country age 50-80 cigarette smoking, arylamine exposrue, schistosoma haematrobium infectinos(SCC) radiation exposure, long tern antibiotic use |
|
|
what is the genetic compentent of bladder cancer
|
chromosome 9 typically papillary noninvasive lesions
chromosome 17,13 invasive lesions |
|
|
what is the presentation of urothelial tumors
|
painless hematuria
all types tend to recur |
|
|
what is schistosoma haematobium associated with
|
Sqamous cell carcinoma of the bladder
bad prognosis |

