![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
139 Cards in this Set
- Front
- Back
|
Prevent initial creation of the hazard |
1
|
|
|
reduce account of energy contained in the hazard
|
2
|
|
|
Prevent release of a hazard that already exist
|
3
|
|
|
modify rate or spatial distribution of the hazard
|
4
|
|
|
separate time in or space the hazard from that which is to be protected
|
5
|
|
|
separate the hazard from that which is to be protected by a material barrier
|
6
|
|
|
modify basic nature of the hazard
|
7
|
|
|
make what is to be protected more resistant to the hazard
|
8
|
|
|
begin to counter the damage already done by the hazard
|
9
|
|
|
Stabilize, repair, and rehabilitate the object of the damage
|
10
|
|
|
prehospital systems have tragically limited their community involvement to the
|
postevent phase
|
|
|
seeks to tap the persuasive power of the law to compel adherance to simple but effective prevention strategies.
|
ENFORCEMENT
|
|
|
One of the most effective means of injury prevention are
|
those in which destructive energy release is permenantly sperarated from the host.
|
|
|
four step process for combating a community based disease.
|
1.SURVEILLANCE 2. RISK FACTOR IDENTIFICATION 3. INTERVENTION 4. IMPLEMENTATION
|
|
|
3 questions that may help determine the success of a community-based coalition to combat a community based disease
|
1. Have attitudes, skills, and judgement changed?
2. Has behavior changed? 3. Does behavioral change lead to a favorable outcome? |
|
|
The most valuable service an EMT can provide.
|
SELF-INJURY PREVENTION
|
|
|
_____ in medicine is process in which the medical care provider assesses the situation, the patient, and all of the resources that are available.
|
CRITICAL THINKING
|
|
|
Steps in Critical Thinking
|
Assessment, Analysis, Construction of a Plan, Action, Reassessment, Changes Along The Way
|
|
|
A strong fund of knowledge possessed by the provider and the ability to communicate these judgements with strength and conviction to all involved in the response to the patient are the ____
|
foundation for critical thinking
|
|
|
Three E's of Injury Prevention
|
Education, Enforcement, Engineering
|
|
|
There are essentially four steps in the process of caring for patients with acute injuries:
|
1) the prehospital phase |
|
|
The management of any patient begins with the________.
|
history of the patient's injury
|
|
|
_________address the interaction of the human body with components of the crash for blunt trauma , penetrating trauma, and blasts.
|
Mechanical principles
|
|
|
To understand the effects of the forces that produce bodily injury, the prehospital care provider needs first to understand two components--______________
|
energy exchange and human anatomy
|
|
|
Increasing _______ increases the kinetic energy.
|
VELOCITY
|
|
|
Drivers should always be at least ____ from the air bag cover, and front seat passengers should be at least ______ away. |
10in. & 18in. |
|
|
In motorcycle crashes failure to use helmets has be shown to increase head injuries by more than _________. |
300% |
|
|
_________ is a protective used by bikers to slow the rider more than the motorcycle so that the motorcycle will move out from under the rider in a motorcycle crash. |
"Laying the bike down" |
|
|
The victim on a rotational-impact crash first moves_____ and _____ as the vehicle pivots around the impact point. |
forward and then laterally
|
|
|
The NHTSA reports that in crashes involving fatalities in the year 2008, ____ of occupants who were totally ejected from a vehicle were killed.
|
77%
|
|
|
In a lateral impact between two cars that lack airbags
|
the occupants of the car struck on its lateral aspect are 5.6 times more likely to die than the occupants in the vehicle striking that car.
|
|
|
In lateral-impact collision between a van and a car
|
the occupants of the car struck broadside are 13 times more likely to die than those on the van.
|
|
|
What are the three phases of pedestrian collisions with MVC's? |
1)The initial impact is to the legs and sometimes the hips.
2)The torso rolls onto the hood of the vehicle.
3) The victim falls off the vehicle and onto the ground, usually headfirst, with possible cervical spine trauma. |
|
|
The injuries produced in pedestrian crashes vary according _______. |
the height of the victim and the height of the vehicle. |
|
|
Falls from greater than ______ the height of the victim are frequently severe.
(PTQ) |
3 times |
|
|
Bilateral fractures of the calcaneus, compression or shear fractures of the ankles and distal tibial or fibular fractures are often associated with _______. |
Don Juan Syndrome |
|
|
______ can result in an unstable spine.
|
angulation and inline compression.
|
|
|
The effect produced by the compression of the lung against a closed glottis, by impact on either anterior or lateral chest wall. |
paper-bag-effect |
|
|
________ Occurs when the heart pressed between the sternum and the spine. |
cardiac contusion |
|
|
A more frequent compression injury in the thorax is compression of the lungs which leads to _______. |
pulmonary contusion |
|
|
80% of patients who suffer _________ die on scene at the time of initial impact. |
traumatic aneurysm |
|
|
The _______ is the weakest of all the walls and structures surrounding the abdominal cavity. |
diaphragm |
|
|
The torn or ruptured diaphragm has four common consequences. |
1. The "bellows" effect that is usually created by the diaphragm is lost and ventilation is affected.
2. The abdominal organs can enter the thoracic cavity and reduce space available for lung expansion.
3. The displaced organs can become ischemic from compression of their blood supply.
4. If intra abdominal hemorrhage is present, the blood can also cause a hemothorax. |
|
|
3 factors that influence the size of the frontal surface area of a projectile are: |
Profile, tumble, and fragmentation |
|
|
Tumble motion of a missile maximizes its damage at _______ |
90 Degrees |
|
|
Gender of an attacker often determines the trajectory of the wound in stabbing incidents. ________ attackers tend to stab _______ whereas ________ attackers tend to stab _______. |
Male/Upwards and Female/Downwards |
|
|
Medium-energy weapons include handguns and some rifles whose muzzle velocity is ________. |
1000 ft/sec.
|
|
|
The temporary cavity created by a medium-energy weapon is _____ to _____ times the caliber of the bullet. |
three/five |
|
|
High energy weapons have a muzzle velocity in excess of _______. |
2000 ft/sec. |
|
|
High energy weapons create a temporary cavity _________ times or greater than the caliber of the bullet. |
25 |
|
|
The average birdshot shell may contain _______ pellets. |
200 to 2000 |
|
|
The average buckshot shell may contain only _______ pellets. |
6 to 20 |
|
|
The ________ provides the most important variable when evaluating the shotgun injury victim. |
range(distance) |
|
|
The four major categories of shotgun wounds: |
1) Contact wound 2) Close range wound 3) Intermediate range wound 4) Long range wound |
|
|
_________ occur when the muzzle is touching the victim at the time the weapon is discharged. |
contact wound |
|
|
__________ is characterized by circular entrance wounds with more evidence of soot, gunpowder, or filler stippling around the wound margins. |
close-range wound |
|
|
_________ are characterized by the appearance of satellite pellet holes emerging from the border around a central entrance wound. |
intermediate-range |
|
|
This pattern is a result of individual pellets spreading from the main column of shot and generally occurs at a range of 6 to 18 ft. |
intermediate-range |
|
|
These wounds are typically characterized by the classic spread of scattered pellet wounds and result from a range greater than 18 ft. |
Long-range wounds |
|
|
________ is essential when examining all patients involved in trauma. |
adequate exposure |
|
|
The greatest challenges for clinicians at all levels of care in the aftermath of an explosion are_____. |
the large number of casualties and multiple, penetrating injuries. |
|
|
Blast waves can travel at greater than _______ and are composed of ______ and ______ components. |
16,400 ft/sec./static and dynamic |
|
|
3 types of energy associated with an explosion: |
1) Kinetic and heat energy in the blast wave
2) Kinetic energy of fragments formed by the breakup of the weapon casing and surrounding debris.
3)Electromagnetic energy |
|
|
The most common form of primary blast injury is ________. |
tympanic membrane rupture |
|
|
When the blast wind of an explosion propels fragments to create multiple penetrating injuries, these injuries are termed __________. |
secondary injuries
|
|
|
_________ are usually the predominant wound agent in an explosion. |
secondary injuries |
|
|
This category of injury includes crush injuries caused by structural collapse, large objects propelled into people, people propelled onto hard surfaces. |
tertiary injuries |
|
|
Heat, flames, gas, and smoke generated during explosions cause __________ that includes burns, inhalation injury, and asphyxiation. |
quaternary injuries |
|
|
_________ are produced when bacteria, chemicals, or radioactive materials are added to the explosive device and released upon detonation. |
quinary injuries |
|
|
Typical primary blast injuries
PTQ |
Tympanic membrane rupture Blast lung Eye injuries Concussion
|
|
|
Typical Secondary blast injuries |
Penetrating injuries Traumatic amputations Lacerations |
|
|
Typical tertiary blast injuries |
Blunt injuries Crush syndrome Compartment syndrome |
|
|
Typical quaternary blast injuries |
Burns Toxic gas and other inhalation injuries Injury from environmental contamination |
|
|
______________ will significantly influence whether a patient lives or dies. |
Early identification, adequate understanding, and appropriate treatment of underlying injury |
|
|
Stab wounds are most likely to injure the
|
liver (40%)
small bowel (30%) diaphragm (20%) Colon (15%) |
|
|
Gunshot wounds commonly damage the
|
small bowel(50%)
Colon(40%) liver(30%) abdominal vessels(25%) |
|
|
The most reliable indicator if intra-abdominal bleeding is the presence of________ from an unexplained source.
|
hypovelimic shock
|
|
|
The approximate internal blood loss associated with rib fractures is______.
|
125ml
|
|
|
The approximate internal blood loss associated with radius and ulna fractures is________.
|
250-500 ml
|
|
|
The approximate internal blood loss associated with humerus fractures is _____.
|
500-750 ml
|
|
|
The approximate internal blood loss associated with tibia or fibula fractures is ________.
|
500-1000 ml
|
|
|
The approximate internal blood loss associated with femur fractures is _______.
|
1000-2000 ml
|
|
|
The approximate internal blood loss associated with pelvis fractures is _______.
|
1000-massive
|
|
|
The 5 classic symptoms of compartment syndrome:
|
1) pain
2) paresthesia 3) pulselessness 4) pallor 5) paralysis |
|
|
A mangled extremity refers to a complex injury resulting from high energy transfer in which significant injury occurs to two or more of the following:
|
1) skin and muscle
2) tendons 3) bone 4) blood vessels 5) nerves |
|
|
The elements of smoke inhalation:
|
thermal injury, asphyxiation, delayed toxin induced lung injury
|
|
|
When hated dry air at ______ is inhaled, the air is cooled to______by the time out is at the level of the trachea.
|
300°C/50°C
|
|
|
The severity of toxin induced lung injury is largely dependant on two factors:
|
the composition of the smoke and the duration of exposure
|
|
|
the initial and most important element of caring for a patient with smoke exposure is________.
|
determining the need for orotracheal intubation.
|
|
|
The severity of Chemical injury is determined by for factors:
|
nature of the chemical, concentration of the chemical, duration of contact, mechanism of action of the chemical
|
|
|
The incidence of blunt trauma is highest in the______ population.
|
pediatric
|
|
|
Children are more susceptible than adults to ________.
|
acute cardiovascular collapse from tension pneumothorax.
|
|
|
_________Is the most common cause of death in the pediatric population.
|
traumatic brain injury
|
|
|
Trauma is the sixth leading cause of death in persons_______.
|
Age 55-64
|
|
|
The Cardiac output diminishes by approximately_______from 20-80 years of age.
|
50%
|
|
|
_______are the leading cause of trauma death and disability in those over 75 years of age.
|
Falls
|
|
|
_______are the leading cause of trauma death in the geriatric population between 65 and 74 years of age.
|
Motor Vehicle Crashes
|
|
|
_______and _______ are the most common causes of death from burns in elderly patients.
|
vascular collapse/infection
|
|
|
Golden Principle 1
|
Ensure the safety of the prehospital care providers and the patient.
|
|
|
Golden Principle 2
|
Assess the seen situation to determine the need for additional resources.
|
|
|
Golden Principle 3
|
Recognize the kinematics that produced the injuries.
|
|
|
Golden Principle 4
|
Use the primary survey approach to identify life threatening conditions
|
|
|
Golden Principle 5
|
Provide airway management While maintaining cervical spine stabilization.
|
|
|
Golden Principle 6
|
support ventilation and deliver deliver oxygen to maintain an SpO2 greater than 95%'
|
|
|
Golden Principle 7
|
Control any significant external hemorrhage
|
|
|
Golden Principle 8
|
Provide basic shock therapy, including appropriately splinting musculoskeletal injuries and restoring and maintaining normal body temperature.
|
|
|
Golden Principle 9
|
Maintain manual spinal stabilization until the patient is immobilized on a long backboard.
|
|
|
Golden Principle 10
|
For the critically injured trauma patients, initiate transport to the closest appropriate facility within 10 minutes of arrival on scene.
|
|
|
Golden Principle 11
|
Initiate warmed intravenous fluid replacement en route to the receiving facility.
|
|
|
Golden Principle 12
|
Ascertain the patients medical history and perform a secondary survey when life threatening problems have been satisfactorily managed or have been ruled out.
|
|
|
Golden Principle 13
|
Provide thorough and accurate communication regarding the patient and the circumstances of the injury to the receiving facility.
|
|
|
Golden rule 14
|
Above all, Do no further harm.
|
|
|
The normal ventilatory rate in the adult patient is______.
|
12-20 ventilation per minute
|
|
|
To do the greatest good for the greatest number of patients with the resources available is the________.
|
key principle of disaster medical care
|
|
|
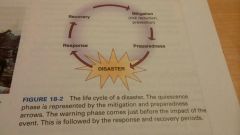
______is the preparation level of the disaster cycle.
|
quiescence
|
|
|
________is the mitigation phase of the disaster cycle.
|
prodome phase
|
|
|
_______ is the disaster phase of the disaster cycle.
|
impact phase
|
|
|
_______the response phase is the response phase of the disaster cycle.
|
rescue phase
|
|
|
_______is a setting in which resources, supplies, equipment, personnel, transportation, and other aspects of the physical, political, social, and economic environments are limited.
|
austere environment
|
|
|
Medical concerns related to Mass Casualty Incidents include these four elements.
|
1)Search and Rescue
2)Triage and initial stabilization 3) Definitive medical care 4) Evacuation |
|
|
S.T.A.R.T
|
Simple Triage And Rapid Treatment
|
|
|
M.A.S.S.
|
Move, Assess, Sort, Send
|
|
|
S.A.L.T.
|
Sorting the patient based on their ability to move
Assessing the patient for the need for Life-saving interventions Treatment and Transport |
|
|
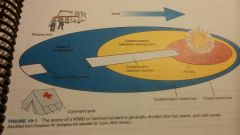
These are important features of the casualty collection point:
|
-Proximity to the disaster site
-Safety from hazards and uphill and upwind from contaminated environments -Protection from climatic conditions -Easy visibility for disaster victims and assigned personnel -Convenient exit routes for air and land evacuation |
|
|
Treatment on the scene is generally limited to the following:
|
-Manually opening the airway
-Correction of tension pneumothorax -External hemmorage control -Administration of chemical agent antidote |
|
|
When responding to a disaster involving hazmat and WMDs, it is critical that the triage and treatment areas be at least ________ upwind and uphill of the contaminated area.
|
300 yards
|
|
|
__________ is the foundation of foster preparedness.
|
independent learning
|
|
|
As it pertains to principles of decontamination, the simple act of removing clothing achieves removal of __________of contamination.
|
70% to 90%
|
|
|
Symptoms associated with the muscarinic effects of nerve agent toxicity is D.U.M.B.E.L.S.
|
Diearreah
Urination Miosis Bradycardia, Bronchospasm Emesis Lacrimation Salivation, Sweating |
|
|
MTWHF is the mnemonic that represents the constellation of symptoms associated with stimulation of nicotinic receptors.
|
Mydriasis
Tachycardia Weakness Hypertension Hyperglycemia Fasciculations |
|
|
Sequence for Donning Personal Protective Equipment
|
Gown
Mask or Respirator Goggles or Face Shield Gloves |
|
|
____________is the most poisinous substance known. It ________ times more toxic than the nerve agent VX and _________ times more toxic than sarin.
|
Botulinum Toxin/15,000/100,000
|
|
|
H.E.L.P.
|
Heat
Escape Lessening Posture |
|

3
|
3
|
|
433
|
433
|
|

438
|
438
|
|

438
|
438
|
|
449
|
449
|
|

461
|
461
|

