![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
118 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Do all arteries carry only oxygenated blood? |
Nope |
|
|
|
What is autonomic neuropathy associated with? |
Silent (painless) myocardial ischemia |
|
|
|
T\F a widened pulse pressure is found in shock and congestive heart failure |
False |
|
|
|
Does skeletal muscle or cardiac muscle have a higher oxygen demand? |
Cardiac muscle is higher |
|
|
|
What does cessation of blood flow to the myocardium produce? |
Immediate ischemia |
|
|
|
Does unstable atherosclerotic plaques compared to stable plaques have |
Blah |
|
|
|
Risk factors for atherosclerotic heart disease |
Obesity Male Inflammation Sedentary lifestyle High LDL Low HDL |
|
|
|
Does cocaine promote thrombosis by activating platelets? |
Yes |
|
|
|
Is cocaine a vasodilator? |
No it's a vasoconstrictor |
|
|
|
Does cocaine decrease heart rate? |
No it increases it |
|
|
|
Neutral pH |
7.0 |
|
|
|
In humans normal arterial blood pH |
7.4 (7.35-7.45) Slightly alkalotic, slight base excess, slight HCO3- excess |
|
|
|
Acid = |
H+ which = protons |
Charge |
|
|
Increase H+ does what to pH |
Decreases pH so it's more acidic/ less base |
|
|
|
Decrease H+ does what to pH |
Higher pH so less acid and more base |
|
|
|
pH equations |
pH=-log[H+] Or pH= [HCO3] / [paCO2] |
|
|
|
Metabolic and respiratory parts that make up pH |
Metabolic = HCO3 levels Resp = paCO2 levels |
|
|
|
How does the body deal w acid? |
By using HCO3 buffers protons, takes away acid but leaves conjugate base - that has negative charge (aka an anion) |
|
|
|
Kidney and HCO3 |
It is made by kidney but takes few days to make significant level, kidney also saves/re absorbs HCO3 to elevate levels |
|
|
|
H2O and CO2- what happens to them in the body |
Water/co2 are exhaled by lungs, some h2o is used by body, h2co3 (carbonic acid) an intermediate metabolite is present in very small concentrations, H+ is buffered (removed by proteins) |
|
|
|
H2o + co2 <-> ______ <-> ______ |
H2co3 H+ + hco3 |
|
|
|
Normal arterial paco2 |
35-45 |
|
|
|
Arterial bicarbonate normal levels |
Hco3: 24-31 Kidney related |
|
|
|
Normal levels of pH, Paco2 and hco3 in arterial blood |
PH: 7.35-7.45 Paco2: 35-45 Bicarbonate: 24-31 |
|
|
|
Respiratory alkalosis blood levels |
PH= greater than 7.45 PCo2 = less than 35 |
|
|
|
Etiology of resp alkalosis |
Hyperventilation, anxiety, stress Drugs. Aspirin/caffeine intoxication High fever |
|
|
|
Metabolic acidosis blood levels |
PH less than 7.35 Hco3 less than 22 |
|
|
|
Metabolic acidosis etiology |
Diarrhea, renal tubular acidosis, lactic acidosis, ketoacidosis, shock, cardiac arrest, toxins ethanol, methanol, ethylene glycol |
|
|
|
Respiratory acidosis blood leveks |
Ph less than 7.35 Paco2 greater than 45 |
|
|
|
Respiratory acidosis etiology |
Narcotic overdose, severe CNS injury Airway obstruction Severe asthma pneumonia copd |
|
|
|
Metabolic alkalosis |
Ph higher than 7.35 Hco3 greater than 31 |
|
|
|
Metabolic alkalosis etiology |
Vomiting Gastric drainage Loop diuretics Too much antacid |
|
|
|
If bicarbonate level goes down you can become... |
Acidodic |
|
|
|
Major buffer for H+ in the body |
Hemoglobin / proteins in general |
|
|
|
Arterial vs Venous blood |
arterial: higher O2 levels, standard for blood gases Venous: lower O2, higher co2, more acidodic |
|
|
|
2 types of immunity |
Innate (natural/native) Adaptive (acquired, specific) |
|
|
|
List innate immunity traits |
Physical/molecular/cellular defenseman place before infection Low levels, always ready Always present Antigen nonspecific Respond immediate No immunologic memory Attacks nonself Doesn't distinguish between different microbes |
|
|
|
What does innate immunity recognize |
General classes of molecules shared by related groups of microbes that are essential to their survival Does not recognize specific antigens |
|
|
|
Examples of innate immunity |
Epithelial barrier (skin, cilia, mucus, stomach acid, saliva, tears) Macrophages, neutrophils, eosinophils, nk cells, dendritic cells Plasma proteins Lysosomes |
|
|
|
Immune system that doesn't distinguish between different mucrobes |
Innate |
|
|
|
Physical/molecular/cellular defenseman place before infection Low levels, always ready Always present Antigen nonspecific Respond immediate No immunologic memory Attacks nonself Doesn't distinguish between different microbes |
Innate immunity |
|
|
|
Epithelial barrier (skin, cilia, mucus, stomach acid, saliva, tears) Macrophages, neutrophils, eosinophils, nk cells, dendritic cells Plasma proteins Lysosomes |
Innate immunity |
|
|
|
Natural killer cells are part of__ immunuty |
Innate |
|
|
|
Less rapid but more effective immunity |
Adaptive |
|
|
|
Initially naive but then develops memory, 1st must recognize foreign agen then process then produce amplified response |
Adaptive immunity |
|
|
|
Antigen specific immunity |
Adaptive |
|
|
|
Immunity that attacks specific microbes at specific antigens |
Adaptive |
|
|
|
2 types adaptive immunity |
Humoral (antibody proteins in blood) Cell mediated (phagocytic cells) |
|
|
|
Humoral immunity |
B cell Antibody proteins in blood |
|
|
|
Cell mediated immunity |
T cells Phagocytic cells |
|
|
|
Immunity that recognizes general class of lipopysaccharide molecules in gram- bacterial walls |
Innate |
|
|
|
Immunity recognizes antibody specific to endotoxins o antigen of e.coli in cell wall |
Adaptive |
|
|
|
T cells come fron |
Thymus |
|
|
|
B cells come from |
Liver, then thymus, then bone marrow, then blood |
|
|
|
Immunity you need to be exposed a second time for response |
Adaptive |
|
|
|
More specific immunity |
Adaptive |
|
|
|
First identified as antigens that evoke rejection of transplanted organs |
Mhc ( majorhistocompatabity complex) |
|
|
|
Aka HLA (human leukocyte antigen) in humans |
Mhc |
|
|
|
Mhc |
Major histocompatibility complex Important in organ transplant The better the match of similar antigens between recipient and donor, the less rejection of organ by recipient |
|
|
|
Where are different lymphocytes generated and where do they mature |
Generated from stem cells in bone marrow or fetal liver B cells mature in bone marrow T cells mature in thymus then go to lymph nodes to wait to be activated by antigen presenting cells |
|
|
|
T lymphocyte functuon |
Functions in cell mediated immunity - virus -rejection of tissue grafts -delayed hypersensitivity reactions (ex. Tb skin test) -intracellular microbes (ex. Legionella pneumonophila) -graft vs host - contact sensitivity |
|
|
|
CD4+ |
Type of t lymphocyte Master regulator for the immune system Important in aids |
|
|
|
Types of t lymphocytes |
Memory cells Cd4+ Cd8 (become cytotoxic T cells) Regulatory T cells (suppress immune response) |
|
|
|
Cytokines |
Small cell signaling proteins Act through cell surface receptors After releasing cells itself, immediate adjacent cells, distant cells Specific kinds released by different types of cells |
|
|
|
Cytokines difference from hormones |
-Higher initial concentration - much greater increase 1000 fold trauma and infection -made by different types of cells - erythropoietin is a cytokine hormone |
|
|
|
Erythropoietin |
Cytokine hormone made by fibroblasts in kidney and CNS neurons and astroglia for memory Tells precursor to Rbcs to start making rbcs |
|
|
|
Are cytokines hirmones |
No |
|
|
|
Def of hormones |
Secreted by discrete glands (ie B cells in pancreas) and affect distant cells and tissues |
|
|
|
Effect of low concentration of cytokines |
Local effects |
|
|
|
Effects of high concentrations of cytokines |
Systemic effects |
|
|
|
1918 flu pandemic |
Relatively more deaths in young people Healthy immune system liability (produce stronger immune response, greater cytokine response, caused cytokine storm) |
Cytokines |
|
|
Cytokine storm |
Cause of 1918 flu pandemic deaths Fever, erythema, swelling, cachexia, fatigue, lack of cytokine regulation, loss of feedback loop Implicated in sirs (systemic inflammatory respond syndrome) So many cytokines killed virus but good cells too |
|
|
|
What does cytokine storm cause |
Inflammation, organ failure, infection |
|
|
|
Plasma cells |
Typically not in peripheral blood- found in lymph nodes Part of B cell humoral adaptive immunity Short lived, needs continuous colony stimulator factor Produces antibody against antigen |
|
|
|
Typically not in peripheral blood- found in lymph nodes Part of B cell humoral adaptive immunity Short lived, needs continuous colony stimulator factor Produces antibody against antigen |
Plasma cells |
|
|
|
Immuniglobulins secreted by plasma cells |
Igg Igm Iga Ige |
|
|
|
IGG |
Immunoglobulin secreted by plasma cells 75% of all antibodies in normal individual Crosses placenta, protects fetus |
|
|
|
Igm |
Immunoglobulin secreted by plasma cells 1st antibody to respond to antigen Does not cross placenta |
|
|
|
IGA |
Immunoglobulin secreted by plasma cells Mucosal production Tears, gut, milk, saliva |
|
|
|
IGE |
Immunoglobulin secreted by plasma cells Lowest concentration of any immunoglobulin Parasites, allergy, hypersensitivity (anaphylaxis) |
|
|
|
Immunoglobulin of highest concentration |
IGG |
|
|
|
First antibody to respond to antigen |
IGM |
|
|
|
Immunoglobulin in mucosal |
(Tears, saliva, milk, gut) IGA |
|
|
|
Lowest concentrated immunoglobulin |
IGE |
|
|
|
Immunoglobulin associated with parasites and allergy |
IGE |
|
|
|
Immunoglobulin that c tosses placenta |
IGG |
|
|
|
Immunoglobulin levels at birth |
Newborn has high IGM and no IGG, if elevated IGG it is from mom so the baby had an infection in utero |
|
|
|
At birth origin of IGG is... |
Maternal |
|
|
|
If elevated IGG at birth... |
Baby got infection from mom in utero |
|
|
|
Primary immune response |
Macrophages phagocytize antigen, present to t helper cell that processes it, TH then activate B cells that produce antibodies Takes 2-3 weeks |
|
|
|
How long does primary immune response process take |
2-3 weeks |
|
|
|
What kind of response to vaccines produce |
Primary immune response |
|
|
|
Secondary immune response |
B memory cells respond to antigen immediately Plasma antibody levels rise w/in days |
|
|
|
Boost shot produces what type of immune response |
Secondary |
|
|
|
IGG in response to antigen exposure (describe graph) |
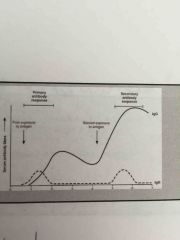
Primary antibody response levels go up then start to decline but in response to 2nd exposure go way up even higher |
|
|
|
IGM in response to multiple exposures to antigen (graph) |
Levels go up in each response but quickly got back to zero after each response so each response is the same level as before |
|
|
|
What is Passive immunity |
ATB pass directly into body from external source instead of body making them |
|
|
|
Artificial examples of passive immunity |
Diphtheria antitoxin Antivenom IV immunoglobulin Rabies vaccine |
|
|
|
Examples natural passive immunity |
IGG through the placenta IGA through breast milk |
|
|
|
Natural active immunity |
Exposed to antigen, develop disease and acquire immunity |
|
|
|
Artificial active immunity |
Vaccine exposed to antigen but no symptoms or very mild |
|
|
|
Vaccination |
Substance that produces immunity |
|
|
|
Immunization |
Process by which person becomes protected from disease By vaccines or being exposed to the disease |
|
|
|
Vaccination vs immunization |
Vaccination: substance that produces immunity Imm: process by which person becomes protected from the disease |
|
|
|
Active immunity produces _____ so if re exposed, b and T cell response if _____ |
Immunologic memory Rapidly mobilized |
|
|
|
Types of vaccines |
Inactivated or dead Part of microbe Attenuated live or viable |
|
|
|
Inactivated or dead vaccines typically.. |
Need a booster |
|
|
|
Live or viable vaccines |
Less need for boosters Can be excreted and inoculate others Cannot be used in immunoconpromised (ex. Polio persists in intestines) Do better job at stimulating cell mediated immunity |
|
|
|
Do most vaccines do a good job of stimulating cell mediated immunity |
No they do a poor job But live attenuated do it better |
|
|
|
Do vaccines stimulate innate immunity |
None do currently |
|
|
|
Immunoconpromised people and vaccines |
May not develop immunologic response to vaccine antigen Can develop vaccine associated disease from live attenuated virus |
|
|
|
Can host develop disease from vaccine? |
Very rarely and typically milder Immunosuppressed can from live vaccines |
|
|
|
Very rare things vaccines can cause |
The illness itself Act as super antigen and overstimulate immune system Cause allergic reaction to egg protein because it is produced in embryonic chicken eggs |
|
|
|
Vaccine autism myth |
Thine risk (ethyl Hg) does not cause autism, it is almost never used anymore but autism is increasing |
|
|
|
Adjuvant |
Added to vaccine to stimulate immune response to target antigen |
|
|
|
Hapten |
Small molecule that can elicit immune response when attached to lrg protein carrier cannot elicit response by itself |
|
|
|
Hapten is associated with... |
Type IV cell mediated immunity |
|
|
|
Immunosnescense |
Deterioration of immune system w/ age Decreased response to infection Decreased immunologic memory especially to vaccination |
|

