![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
44 Cards in this Set
- Front
- Back
|
What are the pitfalls of CT/MRI in staging Wilms’ tumor? What is the purpose of thin slice CT/MRI in the setting of Wilms’ tumor?
|
Regional adenopathy may indicate nodal involvement or normal benign enlargement common in children; detection of extension into perirenal fat and adjacent structures is difficult to analyze because it is usually the result of compression, not frank invasion
Thin slice imaging can define extent of lesion including nodal involvement, can assess the contralateral kidney for evidence of Wilms’, can rule out pulmonary metastasis (most common site; if these are present, one would consider chemotherapy before surgery) |
|
|
Describe the staging of Wilms’ tumor.
|
Stage I: Tumor limited to kidney and completely excised. Nonruptured.
Stage II: Tumor beyond kidney but completely resected. Extrarenal vessels may contain tumor thrombus or be infiltrated by tumor. Stage III: Residual nonhematogenous tumor confined to abdomen, any LN involvement, any tumor spillage, rupture or biopsy, peritoneal implants, tumor beyond surgical margin (gross or microscopic) or tumor not completely removed Stage IV: Hematogenous mets to lung, liver, bone, brain Stage V: Bilateral renal involvement at diagnosis At the board review course the staging that we were given is a little different and gave me the following mnemonic. (1) W - within the kidney completely resected (2) I - into the peri-renal fat, inquiry (biopsy) (3) L - lymph nodes, loser b/c u couldn't resect it, leak or spill (4) M - metastatic disease (5) S - seperate or bilateral disease |
|
|
Name 4 biologic markers which aid in predicting prognosis.
|
LOH of chromosome 16
Telomerase (high activity associated with poor prognosis) Aneuploidy (poor prognosis) VEGF (more likely metastases) |
|
|
What is the initial therapy for most Wilms’ tumor?
|
Radical nephrectomy via transperitoneal approach. It is up to the SURGEON to determine tumor extent
|
|
|
Discuss the postop treatment modalities for each stage/histology of Wilms’.
|
Stage I or II FH and Stage I anaplastic: 18-week AMD + VCR
Stage III FH or II/III focal anaplastic: XRT, AMD,VCR, DOX x 24wk Stage IV FH: abdominal radiation and b/L lung radiation Stage II-IV diffuse anaplasia: XRT, AMD, VCR, DOX, CPM and etoposide |
|
|
What are the 3 main indications for preoperative chemotherapy versus immediate nephrectomy for Wilm's Tumor?
|
1.) Bilateral tumors
2.) Inoperative tumors at time of surgical exploration 3.) Tumor extension into vena cava above hepatic veins |
|
|
What is the treatment protocol for bilateral Wilms’ tumors?
|
1.) Biopsy first
2.) Preoperative chemotherapy x 4-6 weeks, because if a tumor is unresectable, bilateral, major vascular involvement, or solitary kidney that one should give neo-adjuvant chemotherapy to shrink the tumor before surgery. 3.) Re-exploration with partial nephrectomies |
|
|
What is the usual cause of preoperative chemo failure with Wilms’ tumors?
|
Tumor differentiation
|
|
|
Name the various long-term effects of anti-cancer treatment of Wilms’
|
Scoliosis from XRT
Hypogonadism and temporary azoospermia Ovarian failure (12% receiving XRT) &pregnancy complications (low BW) Cancer: HCC (from flank irradiation), Secondary AML CHF from anthracyclines (DOX) |
|
|
What are the predictors of survival of Clear cell sarcoma of the kidney (CCSK)?
|
Lower stage
Younger age at diagnosis Treatment with DOX Absence of tumor necrosis |
|
|
What is the most aggressive and lethal childhood renal tumor?
|
Rhabdoid tumor of the kidney (2% of renal tumors). Malignant rhabdoid tumor demonstrates extremely aggressive biologic behavior that is uniformly associated with poor prognosis and an 18-month survival rate of approximately 20%.
|
|
|
What gene/chromosome is involved with rhabdoid tumor of the kidney?
|
Chromosome 22 (INI1 gene)
|
|
|
What are the typical clinical features of Rhabdoid Tumor of the Kidney?
|
Early age at diagnosis (<16 months)
R = resistant to chemo A = advanced stage at diagnosis B = brain mets Doid sounds like dead, and there is a high mortality. |
|
|
What is the most common renal tumor in infants?
|
Congenital mesoblastic nephroma (CMN)
|
|
|
What is the defining feature of CMN?
|
Excellent outcome with radical surgery alone
|
|
|
What is solitary multilocular cyst or multilocular cystic nephroma and what ages are associated with diagnosis?
|
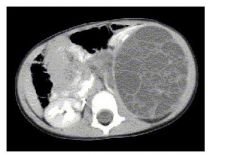
Benign renal tumor
50% in young children (usually boys) and 50% in young adult women, which I saw as a 5 as a resident in the psych patient with the large renal tumor that turned out to be this |
|
|
What is the treatment for multilocular cystic nephroma?
|
Usually radical nephrectomy or partial nephrectomy (if one uses intraoperative frozen sections to ensure resectability)
|
|
|
Of the RCC subtypes which are more common in children? What about other pediatric populations that get kidney cancer, such as sickle cell kids?
|
Papillary RCC is the most common, usually chromosomal translocation involving TFE gene at the X chromosome
Renal medullary carcinoma more common in sickle cell kids |
|
|
What renal lesions are involved in the tuberous sclerosis complex?
|
Angiomyolipoma
Simple cysts PCKD RCC |
|
|
What chromosomes are involved in the TSC?
|
Chromosomes 9 (TSC1) and 16 (TSC2)
|
|
|
What percent of primary testicular tumors in prepubertal children are benign?
|
74%
|
|
|
Name the 3 main types of germ cell tumors in order of decreasing incidence in children.
|
Immature & mature teratomas
Yolk sac tumor Epidermoid cyst |
|
|
Name the 3 main types of gonadal stromal tumors in order of decreasing incidence.
|
Leydig cell tumor
Sertoli cell tumor Gonadoblastoma |
|
|
True/False: Patients with intersex disorders have an increased incidence of gonadal tumors.
|
True. These include androgen insensitivity syndrome and gonadal dysgenesis (the latter with a risk that is increased in the presence of a Y chromosome- 10% incidence of tumor development by 20yo)
|
|
|
What is the characteristic histopathology associated with yolk sac tumor?
|
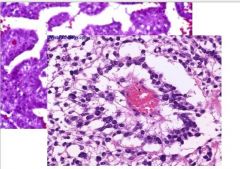
Schiller-Duval bodies
AFP present via staining Mixture of epithelial and mesenchymal cells in organoid pattern |
|
|
What is the pathognomonic histologic feature of Leydig cell tumor?
|
Reinke’s crystals (present in only 40% of these tumors)
|
|
|
Is there an association between cryptorchidism and development of CIS?
|
Yes- CIS incidence is 1.7% in adults who previously underwent orchiopexy
|
|
|
What sonographic features distinguish benign and malignant testicular tumors in children?
|
None really but anechoic cystic lesions can suggest a benign lesion.
|
|
|
What are the unique sonographic findings of an epidermoid cyst?
|
Heterogenous intratesticular mass with concentric rings of alternating hypoechoic and hyperechoic layers (“onion skin” appearance)
|
|
|
What lab test may help identify tumors amenable to testis-sparing procedure in children?
|
AFP (YSTs always produce AFP and all AFP+ tumors have yolk sac components
|
|
|
What is the ½ life of AFP? Of beta-HCG?
|
5 days
24 hours |
|
|
When do AFP levels reach adult levels?
|
At 8 months of age. Until then, AFP levels may be normally elevated in infant boys and do not necessarily indicate malignant disease
|
|
|
What is the most common prepubertal testis tumor in children? How does this differ from adults?
|
Teratoma, immature has much more benign course than those in adults
|
|
|
How are testicular teratomas managed in children?
|
Testis-sparing procedure via inguinal incision (no radical orchiectomy)
|
|
|
What is the initial treatment for YST? What is the most common site of distant metastasis in YSTs?
|
Radical inguinal orchiectomy (routine RPLND and chemo NOT indicated)
Follow with chest xray/CT/MRI monthly x 3 months, q3mos, then q6mo for 36 months Lung and retroperiteonal LN |
|
|
What stage is most common at diagnosis with Yolk Sac Tumors?
|
90% present as Stage I disease
|
|
|
What is the most common sex cord tumor in children and what is the peak age incidence?
|
Leydig cell tumor (4-5 yo)
Sertoli cell tumors occur earlier in age |
|
|
What substances are produced by Leydig cell tumors?
|
Testosterone (causing precocious puberty), corticosteroids, progesterone, estrogens
|
|
|
What is the differential diagnosis of precocious puberty?
|
Leydig cell tumors
Pituitary lesions Large cell Sertoli cell tumors Hyperplastic testicular nodules from CAH |
|
|
What is the treatment for Leydig cell and Sertoli cell tumors?
|
Inguinal orchiectomy although testis-sparing surgery now reported
|
|
|
What is a good mnemonic for Wilm's Tumor Staging?
|
*Remember that in the US it is Surgical Staging.
W - within kidney I - into perirenal fat (outside capsule) or spillage during surgery or a surgical inquiry (biopsy automatically upstages to II) L - lymph nodes +, or you are a loser and couldn't resect it all, or massive leak. M - mets S - seperate sides, tumor on both sides. |
|
|
In the US we stage Wilm's Tumor with surgery, is there ever a role for chemo first?
|
*Well if a patient needs chemo first that is a BUST!
B - bilateral, U - unresectable, S - single kidney, or T - tremendous vascular involvement. This makes sense right you are trying to get this primary out. |
|
|
What is the treatment for congenital mesoblastic nephroma?
|
Congenital mesoblastic nephroma is the most common renal neoplasm in infants <3months and almost universally is associated with a benign course.
So this helps you to think of the fact that in the US surgical staging is the way to go. |
|
|
What is the difference in children that present with Wilm's Tumor versus those children that present with neuroblastoma?
|
*In contrast to children with Wilm's Tumor is that children with Neuroblastoma present with masses that cross the midline and they appear sick.
Since VMA is the metabolite of both neuroblastoma & pheochromocytoma, it serves as the primary tumor marker. It is easily measured in the urine. |

