![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
123 Cards in this Set
- Front
- Back
|
Gravida
|
A woman who is or has been pregnant irrespective of pregnancy outcome.
|
|
|
Primigravida
|
the first pregnancy
|
|
|
Multigravida
|
subsequent pregnancies
|
|
|
Nulligravida
|
a woman who is not and has never been pregnant
|
|
|
Nullipara
|
a woman who has never completed a pregnancy to the stage of viability, she may or may not have aborted previously
|
|
|
Primipara
|
A woman who has been delivered oonce of a fetus or fetuses (multiple gestation) who reached the stage of viability
|
|
|
Multipara
|
A woman who has completed two or more pregnancies to stage of viability
|
|
|
Grand multipara
|
A woman who has completed 5 or more pregnancies to stage of viability
|
|
|
GTPAL
|
Gravity (G) – total # of pregnancies
Term (T) - Total # of deliveries after 37 weeks. Parity (P)– total # of deliveries Live (L) Abortions (SA, LA, ectopic) |
|
|
Premature delivery
|
delivery of an infant weighing between 500 and 2500 gm, after 20 weeks and prior to 37 weeks.
|
|
|
Term delivery
|
between 37 and 42 weeks
|
|
|
Posterm delivery
|
after 42 weeks
|
|
|
Fetal Death (Stillbirth)
|
death occurring in utero after 20 wks gestation
|
|
|
Perinatal Death
|
fetal or infant death occurring after 20 wks gestation and before 29 neonatal days.
|
|
|
Fetal Death Rate
|
the number of fetal deaths per 1000 births
|
|
|
Secondary Amenorrhea
|
Lack of menstrual bleeding for 3 or more months in women with past menses.
|
|
|
Primary Amenorrhea
|
absence of menarche by age 16
|
|
|
Oligomenorrhea
|
uterine bleeding that occurs at intervals more than 35 days
|
|
|
Polymenorrhea
|
uterine bleeding that occurs at regular intervals less than 21 days
|
|
|
Hypermenorrhea
|
excessive menstrual bleeding occurring during a regular menstruation
|
|
|
Hypomenorrhea
|
decrease in the amount of menstrual flow, often with a decrease in duration
|
|
|
Menorrhagia
|
Prolongation of menstrual flow, often associated with and increase of flow
|
|
|
Metrorrhagia
|
Bleeding occurring irregularly between menstrual cycles
|
|
|
Menometrorrhagia
|
Prolongation of the menstrual flow associated with irregular intermenstrual bleeding
|
|
|
Premenstrual spotting
|
variant of metrorrhagia occurring frequently and limited to the few days immediately preceding the menstrual flow.
|
|
|
Climacteric
|
transition from the reproductive phase to menopause
|
|
|
Dysmenorrhea
|
painful menses
|
|
|
Dysparunia
|
painful intercourse
|
|
|
Leukorrhea
|
vaginal discharge
|
|
|
Menarche
|
age at which menstruation begins
|
|
|
Premature menopause
|
Menopause before 35
|
|
|
Procidentia
|
full uterine prolapse
|
|
|
Classification of Abortion
|
Threatened
Inevitable Complete Incomplete Missed Septic Habitual |
|
|
Threatened Abortion
|
vaginal bleeding with or without uterine cramps, closed cx
|
|
|
Inevitable
|
vaginal bleeding with or without uterine cramps; fetoplacental tissue within the dilated cervix
|
|
|
Complete
|
embryo if present and entire placenta expelled
|
|
|
Incomplete
|
some products of conception remaining in the uterus: persistence of cramps, bleeding, or dilatation of the cervix
|
|
|
Missed
|
retention of products of conception before 20th week of pregnancy, failure of uterus to grow under observation or regression in size.
|
|
|
Septic
|
any abortion complicated by signs of infection
|
|
|
Habitual
|
three or more successive pregnancies terminating in spontaneous abortion.
|
|
|
Tylenol (acetaminophen) plain
|
325 mg i-ii tabs po q3-4h prn
|
|
|
Tylenol extra strength
|
500 mg. tab i-ii tabs po q 3-4h prn
|
|
|
Tylenol #1
|
325 mg acetaminophen + 8 mg codeine. i-ii tabs po q 3-4h prn
|
|
|
Tylenol #2
|
325 mg acetaminophen + 15 mg codeine. i-ii tabs po q 3-4h prn
|
|
|
Tylenol #3
|
325 mg acetaminophen + 30 mg codeine. i-ii tabs po q 3-4h prn
|
|
|
Talwin (pentazosine)
|
50 mg. tab. po q 3-4h prn.
|
|
|
Percocet
|
(oxycodone 2.5 mg+ acetaminophen 325 mg)
i-ii tabs po q 3-4h prn. |
|
|
Percodan
|
(oxycodone 2.5 mg + ASA 325 mg) i-ii tabs po q3-4 h prn.
|
|
|
5. Demerol (meperidine)
|
50 mg po q 3-4h prn
|
|
|
6. Toradol (ketorolac) -NSAID
|
10 mg po q 6h prn
|
|
|
Demerol (meperidine)
|
10mg/kg IM Q3-4H for post-op/severe pain prn (always add antiemetic)
|
|
|
Morphine
|
1mg.kg IM Q3-4H prn for post op/severe pain prn (always add antiemetic)
|
|
|
Gravol (dimenhydrinate)
|
50 mg po/IM/IV/PR Q4H prn (for nausea)
|
|
|
Stemitil (prochlorperazine)
|
10 mg po/iv/im Q4H prn (for nausea)
|
|
|
Odansetron (Zofran)
|
0.15 mg/kg iv Q3-4H prn
|
|
|
Ativan (lorazepam)
|
1-2 mg SL/PO QHS prn
|
|
|
Seconal
|
100 mg po QHS prn
|
|
|
Bulk forming laxatives
|
Bran
Psyllium (metamucil 1-2 tbs po bid) |
|
|
Osmotic Laxatives
|
lactulose
MgSO4 Citromag fleet enema (sodium phosphate) PMS-Phosphates Glycerin supplements MOM (milk of magnesia) |
|
|
Stool Softeners
|
Docusate (colace - 100mg po BID)
Mineral oil |
|
|
Non-specific stimulant/irritant laxatives
|
Castor oil
Senna alkaloids (Senekot) Cascara ("brown bomb: 5cc cascara + 15cc MOM) Bisacodyl (dulcolax supp) |
|
|
Blood vessels of the umbilical cord
|
2 arteries, 1 vein.
|
|
|
Signs of Placental detachment
|
Gush of blood
Cord Lengthening Uterus becomes globular Fundus rises |
|
|
Four muscles of the perenium
|
bulbar cavernosus
Superficial Transverse Perenial Levator Ani Sphincter |
|
|
Active labour
|
Contractions causing cervical dilation (>3cm) and effacement.
|
|
|
4 types of tears
|
1st Degree - Vaginal mucosa
2nd Degree - Mucosa + underlying muscle 3rd Degree - Mucosa + muscle + partial anal sphincter 4th degree - complete tear into rectum. |
|
|
4 T's of postpartum hemorrhage
|
Tone (enlarged uterus - multiples, polyhydramnious, macrosomia; infection; distended bladder; prolonged PIT; prolonged induction)
Tissue )Retained products, clots, fibroids) Trauma (Rupture, inversion, operative vaginal delivery, tears) Thrombin (VWD, LMWH, DIC) |
|
|
BPP
|
Breathing movements - 1 of <20s w/in 30 mins
Body movements - 2 or more movements w/in 30 mins Fetal tone - 1 or more active extension with return to flextion AVF - 1 or more pockets of fluid > 2cm in vertical axis. +/- Reactive FHR |
|
|
Interpretation of FHR
|
Baseline - 110-160
Variability - 6-25 bpm, < 5 bpm for <40 min. Decelerations - early decels, occasional uncomplicated variable decels. Accelerations - >32 wks, >15 bpm lasting > 15 seconds - < 32 wks, >10 bpm lasting >10 seconds. - accels w/ fetal scalp stim. |
|
|
FHR Complicated Decels
|
- < 70 bpm for >60 sec
- Loss of variability in trough or BL - biphasic decels - overshoots - slow return to baseline - decreased baseline post decel - Baseline tachy or brady Late Decels w/ > 50% of contractions. Single prolonged decel of >3min |
|
|
Causes of decels
|
Early decel - head compression
Variable decel - cord compression Late decel - uteroplacental insufficiency |
|
|
4 stages of labour
|
1) Contractions and cervical dilation
2) Full dilation to delivery of baby 3) separation and expulsions of placenta 4) First postpartum hour |
|
|
IUGR
|
Symmetric
- early insult - head circ percentile = abd circ percentile Asymmetric - late insult - Head circ preserved, <abd circ. |
|
|
#1 cause of PPH
|
Uterine Atony
|
|
|
4 factors of abnormal progression of labour
|
Power
Passage Passenger Psyche |
|
|
Painless third Tri bleeding
|
Placenta previa until proven otherwise.
|
|
|
GDM Screening
|
24-28 weeks - 1 hr OGCT
- PG <7.8mmol/L = no GDM - PG 7.9-10.2 - do 2hr 75gm OGTT - PG >10.2 = GDM |
|
|
GBS Screen
|
34 - 36 weeks, rectovaginal swab.
At time of delivery - 5 million units of Pen G to start, then 2.5 million units IV Q4H until delivery. |
|
|
When Rhogam in Rh neg women?
|
- Routinely at 28 wks
- w/in 72 hours of birth of Rh +ve fetus - w/ +ve Kleihauer-Betke test - w/ any invasive procedure during pregnancy - |
|
|
Hormones of the menstrual cycle
|
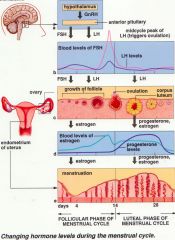
|
|
|
Folic Acid Requirements
|
- 3 months prior to conception reduces risk of ONTD by 70%
- 0.4 mg daily for 3 months prior and 3 months after conception. - 5 mg if diabetes, epilepsy, FHx of NTD or prev child with NTD. |
|
|
If 3+ early losses or midtrimester losses?
|
Consider:
- Thrombophilia testing - Hysterosonogram for uterine cavity abnormalities - Progesterone supplementation? - Genetic counseling & karyotyping - Cervical cerclage (for cervical insufficiency) - Low dose ASA, heparin |
|
|
Cervical Cancer Risk Factors
|
1) HPV infection, esp subtype 16 &18.
18 is responsible for adenocarcinoma. 2) Smoking 3) immunosuppression 4) ? HSV, ?BCP |
|
|
Pap smear screening
|
1) Begin within three years of the onset of vaginal sexual activity
2) Annual screening at first, Q 2-3 years after three consecutive normal paps. 3) No appropriate time to stop screening in women who still have a cervix. |
|
|
Limitations of pap smears
|
1) False-positive ASCUS & LSIL
2) False negative rate of a single screening test up to 50% (hence the need for regular serial screening) 3) Visible cervical lesion needs a biopsy, cytology is not adequate for a visible lesion. |
|
|
Women at greatest risk for developing cervical cancer in Ontario
|
Women who have a lack of regular screening.
- native - Low socioeconomic status - sex-trade workers - Northern Ontario - Immigrant women |
|
|
Bethesda Classification of abnormal cervical cytology
|
1) Satisfactory vs. Unsatisfactory cytologic sample.
- lack of sampling entire transformation zone - low celularity - inflammatory cells/blood 2) Epithelial cell abnormality detected vs. no abn. detected i) Squamous cell abnormality detected - Atypical squamous cells of undetermined signicicance (ASC-US) - Atypical squamous cells - Can't rule out hight grade squamous intraepithelial lesion (ASC-H) - Low grade squamous intraepithelial lesion (LSIL) - High grade squamous intraepithelial lesion (HSIL) - Squamous cell carcinoma ii) Glandular abnormality detected (endocervical, endometrial, NOS) - Atupical glandular cells (AGS) - Atypical clandular cells -favour neoplastic - Adenocarcinoma in-situ - Adenocarcinoma |
|
|
Management of abnormal cervical cytology report
|
ASC-US - Reflex HPV testing vs. repeat cytology vs. colposcopy
ASC - H - Colposcopy LSIL - Colposcopy HSIL - Colposcopy AGC - Colposcopy, ECC, endometrial biopsy AGC - favour neoplasia -Colposcopy, ECC, endometrial biopsy, cone biopsy Adenocarcinoma-in-situ -Colposcopy, ECC, endometrial biopsy, cone biopsy Squamous cell carcinoma or Adenocarcinoma - URGENT colposcopy |
|
|
What is Colposcopy?
|
- Examination of the cervix under magnification using a colposcope.
- Acetic acid is used to highlight dysplastic cells (turn acetowhite) - Lugol's iodine may be used which stains normal epithelium, NOT dysplastic cells - Highlighting dysplastic cells facilitates colposcopic-directed biopsy to confirm histology and guide treatment. |
|
|
Treatment modalities for cervical dysplasia
|
1) Destructive/Ablative (destroys tissue containing dysplastic cells)
- laser ablation (CO2 laser) - cryotherapy (freeze-thaw-freeze technique w/ nitrous oxide) - electrocoagulation (pt needs to be grounded) *** Must rule out cervical cancer first *** - May seriously under-treat with destruction alone. 2) Excisional - Loop electroexcision procedure (LEEP) - Cone Biopsy(cold knife cone vs. laser cone) - Hysterectomy *** Definitive pathology specimen is obtained*** |
|
|
When should the excisional technique be used?
|
- positive endocervical curettage
- suspected glandular abnormality - histology confirmed microinvasive cervical cancer - Significant discrepancy between cytology, colposcopy, and histologic findings |
|
|
Prevention of Cervical Neoplasia
|
Primary Prevention
i) prevention of HPV infection - Abstinence - Condom use - HPV Immunization (gardasil - 6, 11, 16, 18) ii) Prevention of cervical dysplasia in HPV +ve women - Avoidance of co-factors (smoking, HIV) Secondary Prevention - Cytologic screening ("pap smear") - ?HPV screening? |
|
|
HPV Vaccine
|
- Immunization against subtypes 6, 11, 16, 18 (covers 70% of burden of disease)
- Recommended for all women aged 9 - 26, regardless of previous exposure to HPV or previous development of cervical neoplasia. - 3 injections over 6 months |
|
|
Cervical cancer histologic subtypes
|
- Caused 420 deaths in 2003
Histologic subtypes - Squamous cell *** - Adenocarcinoma - Adenosquamous - Clear cell - Small Cell - Sarcoma - Melanoma - Secondary spread |
|
|
Cervical cancer Symptoms
|
- Asymptomatic discovered on routine pap
- Abnormal vaginal bleeding (classically post-coital bleed) - Malodorous vaginal discharge - weight loss - Pelvic pain - Sciatica - Obstructive uropathy - GI symptoms |
|
|
Spread of cervical cancer
|
1) local invasion of cervix, uterine corpus, vagina, parametrium
2) Lymphatic spread to pelvic and para-aortic lymph nodes 3) Hematologic spread to liver, lung 4) Intraperitoneal implantation (seeding) |
|
|
Cervical Cancer Staging
|
FIGO staging system incorporates:
- Vaginal speculum - Bimanual - Pelvirectal - CXR - Cystoscopy - Proctoscopy - IVP |
|
|
Treatment of Cervical Cancer
|
1) Surgery
- Very early stage - simple hysterectomy vs. cone biopsy - Traditional early stage - Radical hysterectomy ( uterus, cervic, 1-2cm cuff of cagina, parametria, and pelvic lymphadenectomy. Ovaries may be left in situ for fertility/avoiding early menopause - Small invasive cancer w/ desire for fertility - radical trachelectomy (removes cervix, parametrium, vaginal cuff - fundus is surrounded with cerclage to prevent incompetence during pregnancy and reconnected to the vagina. - 60% pregnancy rate) 2) Radiation - Early stage non-surgical candidates or adjunct to surgery if needed (+ve lymph node, +ve margin etc..) - Mainstay for advanced stage as curative or palliative - External beam RT daily over 5 weeks, followed by brachytherapy (continuous radiation) over a few days. 3) Chemotherapy - Cisplatin given concomitantly with external beam on a weekly basis. - Can also be used palliatively. |
|
|
Dystocia
|
Abnormal labour or difficult childbirth
Def'n: The abnormal progression of cervical dilation and/or fetal descent during labour. Active phase of 1st stage: >4 hours of <0.5 cm/hr cervical dilation 2nd stage: > 1 hour with no fetal descent during active pushing aka: Cephalopelvic disproportion aka: Failure to Progress *** Do not make a diagnosis of dystocia when cervical dilation is less than 4 cm.*** |
|
|
Abnormal labour patterns
|
1) Primary abnormal progression in labour - protraction
2) Secondary Arrest - Adequate progress of labour followed by an arrest of dilatation in the first stage of labour (Assoc. w/ occiput posterior) - Secondary Arrest - Second stage of labour as fetus fails to descend particularly with maternal expulsive effort. |
|
|
Etiology of Dystocia
|
Power
- Contractions may be hypotonic or in-coordinate - Maternal expulsive efforts may be inadequate Passenger - Fetal position - Fetal size - Fetal anomalies (ie hydrocephalus) - Fetal attitude? Passage - Pelvic structure - Soft tissue obstruction (Tumor, full bladder/full rectum, vaginal septum) Psyche - Anxiety - Stress - Pain |
|
|
Prevention of Dystocia
|
- Pt eductation about labour
- Only admit in active labour - Pain management in prolonged latent phase - Supportive companion and one to one nursing care in active labour. - Maintain ambulation and upright position in labour as much as possible. - Maintain adequate hydration - Do not delay - manage non-progressive active labour with ROM and Oxytocin. |
|
|
Evaluation of abnormal labour
|
- Assess maternal status
* Vitals *Pain * Ctx pattern * Membranes * Cervical dilation/Effacement * Pelvic architecture - Assess fetal status * FHR * Fetal station * Fetal presentation and position |
|
|
Oxytocin
|
Initial dose: 1-2 mU/min
Increase interval: q30min Dosage increment: 1-2 mU Maximum dose: 40 mU |
|
|
Indication for Induction
|
Maternal
- Post-dates - Preeclampsia - Any maternal medical problem Fetal - IUGR - Hemorhage - PROM - Chorioamnionitis - GDM - Fetal compromise - Iso-Immune disease |
|
|
Contraindications to Oxytocin
|
- Severe vaginal bleeding
- Placenta previa - Hypotension - Abnormal fetal lie (transverse, footling breech) - Prior classical or inverted-T uterine incision. - Pelvic structural deformities |
|
|
Adverse Effects of Oxytocin
|
- Fetal compromise (hyperstimulation)
- Uterine rupture (hyperstimulation) - Water Intoxication (ADH effect) - Hypotension (Vasodilation) |
|
|
VBAC risks and successes
|
Risk of rupture - 1.5%
Chance of successful vaginal delivery post C/S: - 50% - 85% - 50% if previous C/S was for dystocia - 85% if previous C/S was due to any non-reoccurring issue, ie * previa * breech * triplets * non-reassuring fetal HR |
|
|
Indications for assisted vaginal birth (operative delivery)
|
Fetal
- Evidence of fetal compromise requiring immediate delivery Maternal - Failure to deliver spontaneously in the second stage - Conditions which require a shortened second stage - Inefficient maternal effort |
|
|
Contra-indications for Operative delivery
|
- Non-cephalic presentation, face or brow
- Unengaged head - Incompletely dilated cervix - Low probability of success Specific to vacuum - <34 weeks gestation - deflexed attitude of fetal head - need for rotation - fetal conditions (bleeding disorder, demineralization disorder) |
|
|
Prerequisites for operative delivery
|
- Informed concent
- Vertex presentation - Vertex engaged - Term or near term - cervix fully dilated - Membranes ruptured - Adequate maternal pelvis - Adequate anaesthesia - Maternal bladder empty - backup plan - Ongoing assessment |
|
|
Risks of assisted vaginal birth
|
- Maternal soft tissue trauma
- Fetal scalp trauma (Laceration, hemorrhage) - Fetal subgleal/subaponeurotic hemorrhage (not limited by suture lines like a cephalohematoma, therefore +++ blood loss can be fatal.) |
|
|
Indications for C/S
|
Most Common
- Repeat C/S - Dystocia - Breech presentation/other malpresentations - Non-reassuring fetal status Absolute Indications - Placenta Previa - Cord Prolapse - Previous uterine surgery - Previous classical c/s or inverted T incision - Previous uterine rupture - Malpresentation - Obstructed pelvis Relative Indications - Failed induction - Abnormal progression in labour - Pre-eclampsia/eclampsia - DIabetes - Cardiac Disease - Placental Abruption - Multiple Pregnancy |
|
|
Risks of C/S
|
- Infection (wound, sepsis, uterine, urinary
- Hemorrhage - Atelectasis - Injury to bowel or bladder or ureter - Deep venous Thrombosis - Pulmonary Embolus - Longer recovery time *** All risks are increased if the C/S follows and unsuccessful trial of labour *** |
|
|
Labour Pain relief
|
Non-pharmacologic
* Reduction of painful stimuli - maternal movement and position change - counter-pressure - abdominal decompression * Activation of peripheral sensory receptors - Superficial heat and cold - Immersion in water - touch and massage - acupuncture and acupressure - transcutaneous electrical nerve stimulation (TENS) - Intradermal injection of sterile water - Aromatheraphy * Enhancement of descending inhibitory pathways - attention focusing and distraction - hypnosis - music and audio analgesia - biofeedback Pharmacologic - Nitrous Oxide in latter part of 1st stage - Narcotics IV/PCA pump * Combined with anti-emetic * Decreased fetal heart rate variability * Causes neonatal respiratory depression (reverses with NALOXONE) - Peripheral nerve blocks - Perineal Infiltration - Epidural block |
|
|
Contraindications to VBAC
|
Absolute
- Previous classical, inverted-T, or unknown incision - Other uterine surgeries - Previous history of uterine rupture - Opinion of previous surgeon (weak or thin myometrium observed during previous c/s- get operative note) - Mother desires a repeat C/S Relative - If induction is required - two or more previous lLSCS scars - Multiple pregnancy - Breech presentation - Poor obstetrical history - Pt desires tubal ligation |
|
|
Risk of VBAC
|
- UTERINE RUPTURE
- Prolonged labour - maternal fever and infection - failed trial necessitating a repeat c/s (all c/s risk are higher after a trial of vag delivery) |
|
|
Why VBAC?
|
- Reduced intervention, and their risks
- faster recovery |
|
|
Risk of elective repeat C/S
|
All risks of C/S are increased with repeat c/s due to scarring, including injury to surrounding structures and hemorrhage.
|
|
|
Signs of Uterine Rupture
|
-UR occurs in 1-5/1000 VBACs
Signs - Profound fetal bradycardia - Constant lower abdominal pain (may be masked by epidural) - Cessation of uterine contractions - Vaginal bleeding - Recession of presenting part on vaginal exam - intra-abdominal hemorrhage - hypovolemic shock |
|
|
Causes of Uterine Rupture
|
- Uterine Scar (C/S, myomectomy, previous uterine perforation, salpingectomy with cornual resection.)
- Excessive uterine action (oxytocin, prostaglandins, neglected obstructed labour) - Trauma (Forceps, manual removal of placenta, assault/MVA) - Misc (multiparity, uterine anomalies, placenta accreta) |
|
|
Placental attachment
|
Placenta ACCRETA - invasion of the myometrium which does not penetrate the entire thickness of the muscle. (75-78%)
Placenta INCRETA - the placenta further extends into the myometrium (17%) Placenta PERCRETA - the placenta penetrates the entire myometrium to the uterine serosa (5-7%). The placenta can attach to other organs such as the rectum or bladder. |
|
|
Indications for Induction of Labour
|
Emergent
- Severe gestational hypertension - Suspected fetal compromise - Severe intrauterine growth restriction - maternal disease - significant antepartum haemorrhage - choreoamnionitis Urgent - PROM - IUGR w/ no acute compromise - Poorly controlled diabetes - Iso-immune disease Non-Urgent - prolonged pregnancy - well controlled diabetes - prior intrauterine death - logistical problems |

