![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
26 Cards in this Set
- Front
- Back
|
List concerns surrounding vaginal breech delivery.
|
Increased perinatal morbidity and mortality
Increased maternal morbidity (genital tract lesions) Reason for breech (e.g. ?fetal anomaly) |
|
|
Specifically what are the main causes of fetal mortality with vaginal breech delivery?
|
Cord prolapse (1% Frank, 10% Footling)
Birth asphyxia Brain injury and hemorrhage Head entrapment (Williams OB) |
|
|
According to SOGC guildelines, with careful case selection and management, for term singleton vaginal breech delivery, what is the:
a) perinatal mortality? b) serious short-term neonatal morbidity? |
a) 2/1000
b) 2% (Level IIa evidence) |
|
|
According to SOGC guidelines, do long-term neurological infant outcomes differ by planned mode of delivery, even in the presence of serious short-term outcomes?
|
No
(Level I evidence) |
|
|
If pre- or early-labour ultrasound is not available, what is recommended regarding mode of delivery?
|
Cesarean Section
|
|
|
What features should be assessed on pre- or early-labour ultrasound when considering a patient for potential breech delivery?
|
Type of Breech
Frank or Complete (Footling = C/S) Fetal growth EFW: 2500-4000g Fetal head attitude Flexed or Neutral |
|
|
According to SOGC guidelines, list contraindications to offering vaginal breech delivery (9)
|
Contraindication to any Vaginal Delivery
Patient refusal Requirement for Labour Induction Lack of pre- or early-labour U/S Macrosomia FGR Non- Frank or Complete breech Fetal head/neck extension Fetal anomaly incompatible with breech delivery Cord presentation Inadequate maternal pelvis |
|
|
When membranes rupture what must immediately be done?
|
Vaginal exam to rule out cord presentation.
|
|
|
According to SOGC guidelines, is continuous FHR monitoring recommended or required in:
A) 1st stage of labour B) 2nd stage of labour |
A) recommended
B) required |
|
|
According to SOGC guidelines, what is the best indicator of an adequate maternal pelvis?
|
Adequate progress in labour.
SOGC seems to define this as "failure to progress over 2h in the presence of adequate uterine contractions". |
|
|
According to SOGC guidelines, is induction of labour for a breech fetus recommended?
Is oxytocin for labour augmentation an option? |
No.
Yes. if dystocia is felt secondary to inadequate contractions. The guidelines suggest that oxytocin is used only with epidural analgesia (?) |
|
|
What is recommended if adequate progress in labour cannot be achieved?
|
Cesarean section
|
|
|
According to SOGC guidelines, what are recommendations regarding the second stage of labour and delivery?
|
1) Continuous FH monitoring
2) Delivery in or near and OR capable of C/S w/i 30min 3) <=90min passive 2nd stage 4) <=60min active 2nd stage 5) if fetus not delivered in this time frame --> C/S 6) Presence of skilled resus team |
|
|
What percentage of fetuses are breech at
a) <=28wks b) >=32wks c) >=37wks What percentage of fetuses will spontaneously convert to cephalic presentation after 36wks? |
a) 25%
b) 7-15% c) 3-4% d) 25% (chances lowered by: extended fetal legs, oligohydramnios, short umbilical cord, primiparity, and fetal/uterine abnormalities) |
|
|
List the types of breech presentation.
|
Frank (50-70%)
bilateral hip flexion and knee extension Complete (5-10%) bilateral hip flexion +/- knee flexion Incomplete (10-30%) Uni/bilateral hip extension, foot or knee lead breech Footling uni/bilateral feet lead breech Kneeling breech (RARE) |
|
|
List risk/associated factors for a term fetus in breech presentation?
|
Preterm fetus
Fetal abnormality Uterine abnormality fibroid, bicornuate, septum Placenta position fundal, previa Previous breech fetus Multiple gestation Polyhydramnios Increasing parity |
|
|
1) What is the 'star-gazer fetus'?
2) What percentage of breech fetuses will be affected? 3) What is the management? 4) Why is this management recommended? |
1) Extended neck/head
2) 5% 3) Cesarean Section 4) Risk of injury to fetal spinal cord, difficulty with head entrapment |
|
|
During vaginal examination for fetal position, what reference point is used? (e.g. occiput for cephalic presentations)
|
Sacrum
|
|
|
When the breech reaches the perineum, stimulation (touching) may prompt what reflex and result in what outcome?
|
Moro reflex
Head extension |
|
|
When are breech extraction maneuvers permitted?
|
After delivery to the umbilicus and if deemed necessary (non-reassuring fetal status)
|
|
|
List key elements to partial breech extraction.
|
Spontaneous delivery to umbilicus
(unless sacrum posterior, then gently rotate) Gentle, constant downward rotation with maternal effort, grasping ASIS/sacrum Never elevate fetal legs above horizontal (45 degrees maximum) Supra-pubic pressure from assistant to keep fetal head flexed |
|
|
Describe strategies to manage nuchal arms
|
Downward, rotational movement through 180 degrees to spontaneously reduce
Loveset manuever when scapula seen ??Bickenbach (Consider episiotomy for working room) |
|
|
What is the Duhrssen incision?
|
Incision made to cervix in the 10, 2, and sometimes 6 o'clock positions
|
|
|
Describe strategies to manage an entrapped head?
|
Suprapubic pressure (Bracht maneuver)
Maternal expulsive effort Episiotomy Mariceau/Prague maneuver Forceps (Piper, etc.) Nitroglycerin (50-200ug IV Zavanelli & Cesarean delivery Symphysiotomy |
|
|
What is the modified Prague manuever?
|
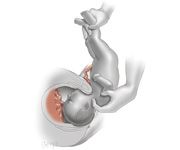
If the fetus delivers sacrum posterior, the legs are grasped and the abdomen is flexed onto the maternal abdomen - a finger is hooked over the bilateral shoulders and suprapubic pressure is used for delivery of the head
|
|
|
Describe a symphysiotomy
|
Foley w/ introducer in urethra/bladder
Deviate foley left/right Incision through skin and symphysis pubis Maternal rest 2 days then weightbearing |

