![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
153 Cards in this Set
- Front
- Back
|
What structures must light pass through before reaching the retina? |
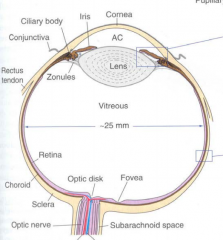
- Transparent cornea
- Anterior chamber - Lens - Vitreous body |
|
|
What happens at the fovea?
|
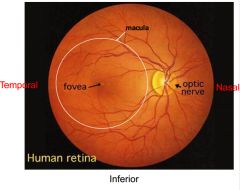
Where 99% of the vision occurs
|
|
|
What are the other names for the part of the optic nerve that can be seen in the retina?
|
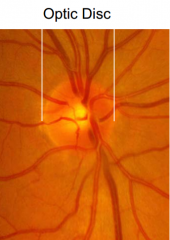
- Optic disk
- Optic nerve head - Disk - Papilla |
|
|
What does the term peripapillary mean?
|
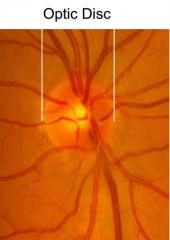
Near or around the nerve head
|
|
|
What does papilledema mean?
|
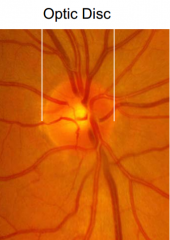
Swollen nerve head
|
|
|
What are the functions of the cornea?
|
- Helps to shield the rest of the eye from germs, dust, and other harmful matter
- Outermost lens - controls and focuses entry of light into eye |
|
|
Which eye structures contribute to protection of the eye?
|
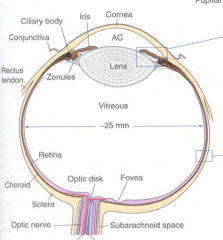
- Cornea
- Eyelids - Eye socket - Tears - Sclera (white part) |
|
|
What percentage of the eye's total focusing power is from the cornea?
|
65-75%
|
|
|
How does the cornea receive nourishment?
|
- NOT from blood vessels
- Rather from tears and aqueous humor that fills chamber behind it |
|
|
Why is it important that the cornea not contain blood vessels?
|
It needs to be transparent to refract light properly (blood vessels would interfere with this process
|
|
|
What are the layers of the cornea, outermost to innermost?
|
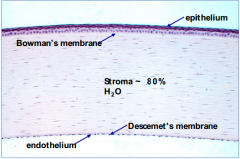
- Epithelium
- Bowman's membrane - Stroma - Descemet's membrane - Endothelium |
|
|
How much of the thickness does the epithelium contribute to the cornea?
|
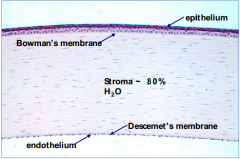
10%
|
|
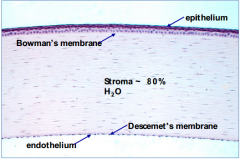
What are the functions of the corneal epithelium (outermost layer)?
|
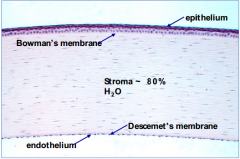
- Block passage of foreign material, such as dust, water, and bacteria, into the eye and other layers of the cornea
- Provides smooth surface that absorbs oxygen and cell nutrients from tears, then distributes them to the rest of the cornea |
|
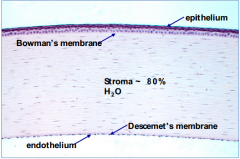
Why is the cornea so sensitive to touch?
|
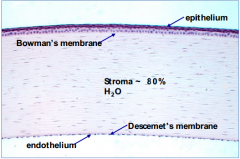
The epithelium is filled with thousands of tiny nerve endings that make the cornea extremely sensitive to pain when rubbed or scratched
|
|
|
Which layer of the cornea has a high regenerative capacity?
|
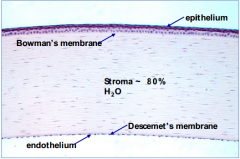
Epithelium
|
|
|
What kind of cells are in the epithelium of the cornea?
|
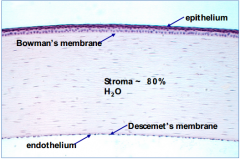
Stratified squamous cells
|
|
|
What part of the cornea provides a foundation on which the epithelial cells anchor and organize themselves?
|
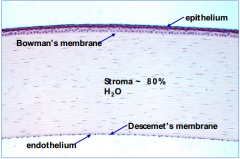
Bowman's Membrane
|
|
|
Bowman's layer of the cornea is composed of what?
|
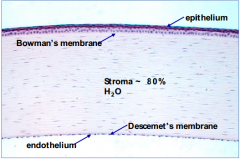
- Strong layered protein fibers - collagen
- Acellular |
|
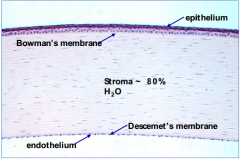
What happens if Bowman's layer of the cornea is injured?
|
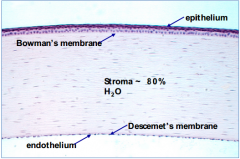
Can form a scar as it heals - this can impact vision if they are large and centrally located
|
|
|
What is the function of Bowman's membrane of the cornea?
|
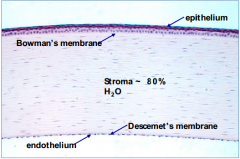
Barrier to infection
|
|
|
What layer of the cornea is beneath Bowman's membrane? What percentage of the eye thickness does it contribute?
|
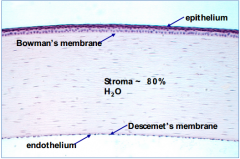
Stroma - 90% of cornea's thickness
|
|
|
What are the contents of the stroma of the cornea?
|
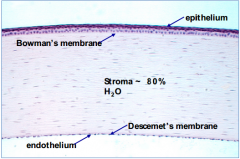
- 78% water
- 16% collagen - No blood vessels |
|
|
What is the function of the collagen in the stroma of the cornea?
|
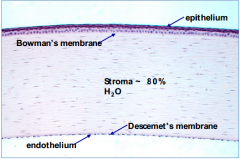
- Gives cornea strength, elasticity, and form
- Unique shape, arrangement, and spacing are essential to produce the cornea's light-conducting transparency |
|
|
What layer of the cornea is under the Stroma?
|
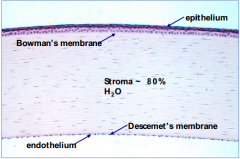
Descemet's Membrane (D=deep)
|
|
|
What is the structure of Descemet's membrane in the cornea?
|
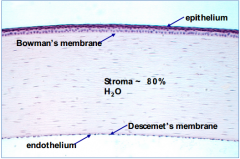
- Collagen fibers (different from those of stroma)
- Endothelial cells |
|
|
What happens to the thickness of Descemet's membrane in the cornea?
|
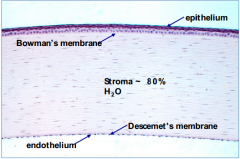
- Thin sheet originally
- Increases in thickness with age |
|
|
What are the functions of Descemet's membrane in the cornea?
|
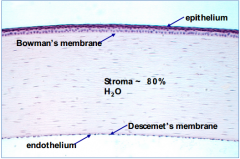
Protective barrier against infection and injuries
|
|
|
What happens to Descemet's membrane after injury?
|
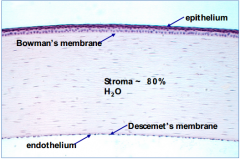
Regenerates
|
|
|
What is the thin, innermost layer of the cornea?
|
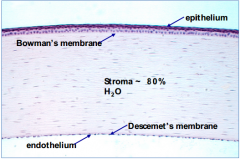
Endothelium
|
|
|
What is the function of the endothelial cells of the cornea?
|
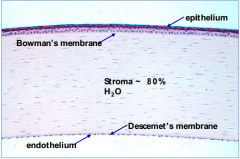
- Keeps the cornea clear
- Pumps excess fluid out of the stroma |
|
|
What would happen if the endothelial layer of the cornea didn't pump water out of the stroma?
|
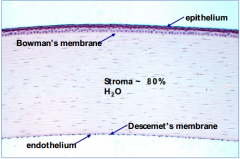
- Stroma would swell with water, become hazy, and ultimately opaque
- Cause loss of vision |
|
|
What happens to endothelial cells of the cornea after injury? The eye?
|
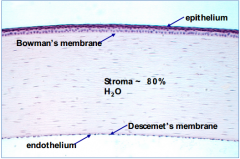
- Destroyed forever
- Can lead to corneal edema and blindness - Only therapy is for a corneal transplant |
|
|
What is the term for nearsightedness? Where does the image focus? What kind of lens is used to treat this?
|
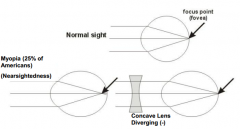
Myopia - light from far away focuses in front of the fovea (eye is too long or cornea too strong)
- Use concave lens (diverging -) |
|
|
What is the term for farsightedness? Where does the light focus? What kind of lens is used to treat this?
|
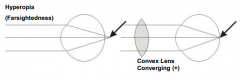
- Hyperopia - light from close up focuses behind fovea (eye is too short or cornea too weak)
- Use convex lens (converging +) |
|
|
What are the most common vision problems in the U.S.? How many?
|
- Myopia (25%)
- Hyperopia - Astigmatism - Approx. 120 million people in U.S. wear glasses or contact lens to fix these conditions |
|
|
What are wave aberrations?
|

Refractive errors that cause diffraction and scattering of light
|
|
|
What are the components of the uvea? Which is the largest component?
|
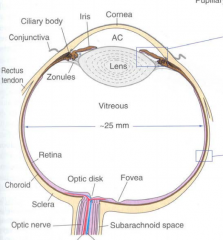
- Choroid - largest component
- Ciliary Body - Iris |
|
|
What are the three layers of the choroid (from out to in)?
|
- Vessel layer
- Chorocapillary layer - Bruch's membrane |
|
|
What are the contents of the vessel layer of the choroid? Is it the most outermost, middle, or innermost layer of the choroid?
|
- Contains medium sized arteries and veins, loose CT and melanocytes
- Outermost layer |
|
|
What are the contents of the choriocapillary layer of the choroid? Is it the most outermost, middle, or innermost layer of the choroid?
|
- Capillaries arrange in one plane, fenestrated type
- Middle layer of choroid |
|
|
What are the contents of the Bruch's membrane of the choroid? Is it the most outermost, middle, or innermost layer of the choroid?
|
- Amorophous hyaline membrane (only 3-4 microns thick)
- Innermost layer |
|
|
What rests upon the Bruch's membrane of the choroid?
|
Retinal pigmented epithelia
|
|
|
What is the ciliary body an expansion of?
|
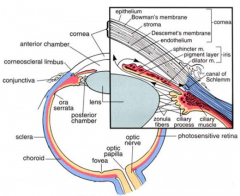
Expansion of the stroma of choroid near the lens
|
|
|
What three regions does the ciliary body contact?
|
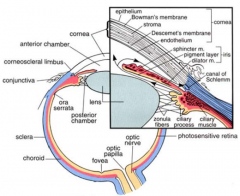
- Vitreous body
- Sclera - Posterior chamber/lens |
|
|
What are the projections from the ciliary body? Where do they project to?
|
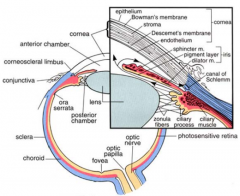
- Ciliary processes
- Project toward lens |
|
|
What meshwork is found within the ciliary body?
|
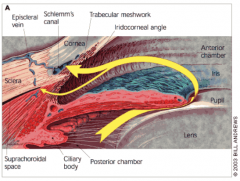
Trabecular meshwork within ciliary body near limbus
|
|
|
How does aqueous humor drain from the anterior chamber?
|
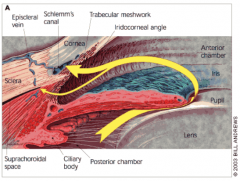
Via the trabecular meshwork in the ciliary body
|
|
|
What structure covers the lens?
|
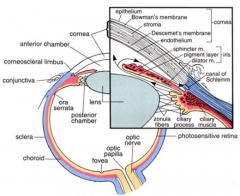
Iris (part of uvea)
|
|
|
What does the iris regulate?
|
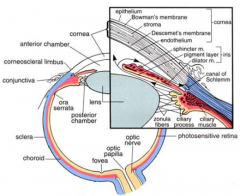
Amount of light reaching the retina
|
|
|
What are the components of the iris?
|
- Vascular, loose CT
- Interspersed with melanocytes |
|
|
What determines eye color?
|
- Number and type of melanocytes in the iris
- Eumelanin - brown/black melanins - brown eyes - Pheomelanin - red/yellow melanins - blue/green eyes |
|
|
What side of the iris is lined? With what?
|
Posterior surface lined with a double layer of pigmented epithelium
|
|
|
What part of the iris absorbs light?
|
Posterior surface which is lined w/ a double layer of pigmented epithelium
|
|
|
How are the fibers of the dilator pupillae arranged? What kind of cells? What layers is it between?
|
- Radially arranged myoepithelial cells
- Between vascular and pigment layers |
|
|
What controls the dilator pupillae? What happens when it contracts?
|
- Sympathetic innervation - superior cervical ganglion
- Contracts = dilates |
|
|
How are the fibers of the sphincter pupillae arranged? Where?
|
- Concentric smooth muscle bundles
- At pupil margin (inner aspect of iris) |
|
|
What controls the sphincter pupillae? What happens when it contracts?
|
- Parasympathetic innervation - CN III from Edinger-Westphal nucleus
- Contracts --> constricts |
|
|
What does the anterior chamber contain? Function?
|
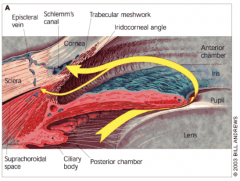
- Contains aqueous humor
- Avascular (so no blood vessels) - Involved in maintaining intraocular pressure |
|
|
Where is aqueous humor produced? Where does it move?
|
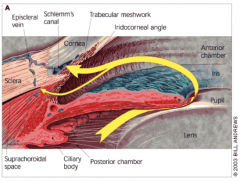
- Produced in ciliary processes in the posterior chamber
- Passes from posterior chamber into anterior chamber (between iris and lens) - Drained from anterior chamber via trabecular meshwork - Humor passes into canal of Schlemm that drains into venous system |
|
|
What is the leading cause of blindness and vision impairment? How common is it?
|
Glaucoma - 2.5 million people in U.S. (3% of people older than 55 years; although 1/2 are unaware they have it)
|
|
|
What are the types of glaucoma?
|
- Primary Open Angle Glaucoma (POAG)
- Angle Closure Glaucoma (also normal tension glaucoma, but the first two listed are the main types) |
|
|
What are the symptoms of glaucoma?
|
- Increase in intraocular pressure (IOP)
- Can damage CN II (Optic N.) - Visual field defect (perimeter) |
|
|
What happens in normal tension glaucoma?
|
Optic nerve damage despite normal IOP (intraocular pressure)
|
|
|
What is secondary glaucoma?
|
When another disease causes or contributes to increased eye pressure, resulting in optic nerve damage and vision loss (as a result of ganglion cell death)
|
|
|
What is Open-Angle, or Chronic Glaucoma? Frequency?
|
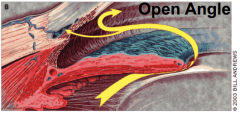
- Obstruction in drainage system of eye
- When fluid reaches angle, it passes too slowly through meshwork - Fluid builds up, pressure rises, and damage to optic nerve and vision loss may occur - 80-85% of all glaucoma cases |
|
|
What is Angle-Closure Glaucoma? Frequency? Severity?
|
- Poor access to drainage system in eye
- Angle between iris and cornea narrows, blocking drainage of aqueous humor - Acute, sudden increase in pressure in eye causes intense pain and blurred vision - Very rare - Very severe, can cause blindness in 24-48 hours if not treated |
|
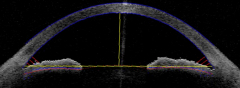
Is there anything wrong with this eye?
|
No - normal
|
|
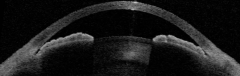
Is there anything wrong with this eye?
|
Yes - Angle-Closed Glaucoma
|
|
|
What are the clinical signs of glaucoma?
|
- Elevated pressure (tonometry) - normal pressure is 12-22 mm Hg
- Visual field defect will reveal a selective peripheral loss of sensitivity - Increased cupping of Optic Nerve |
|
|
How do you assess the cupping of the optic nerve?
|
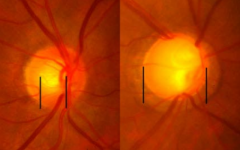
Cup to disk ratio: 0-1, higher is worse
(Left is better) |
|
|
At what percent loss of peripheral vision does a patient usually come in?
|
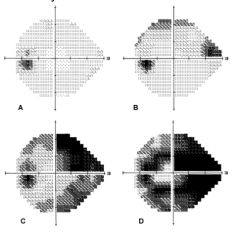
Not until 75% loss!!
(dark = decreased sensitivity) |
|
|
What is the lamina cribrosa?
|
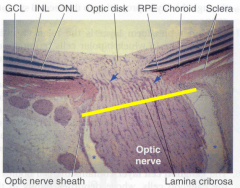
Network of collagen fibers through which the fibers of the optic nerve exit the eye - may be altered in glaucoma
|
|
|
What percent of the refractive power of the eye is contributed by the lens?
|
Only 20% (~10D vs. ~50D for cornea)
|
|
|
What are the structural components of the lens?
|
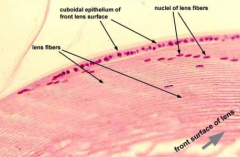
- Capsule - ECM surrounding lens
- Epithelium - anterior surface of lens - Lens fibers - body of lens (no organelles) |
|
|
What are the functions of the lens?
|
- Refraction
- Accommodation |
|
|
What supports the lens?
|
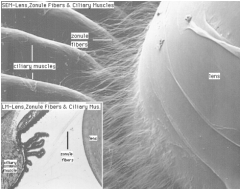
Fibers (suspensory ligaments or zonules) attached to ciliary body
|
|
|
How does the thickness of the lens change with accommodation?
|
- Thinner when focused on distant objects (relaxed ciliary muscles)
- Thicker walls when focusing on near objects (contracting ciliary muscles) |
|
|
What is a cataract?
|
Opacification of the lens
|
|
|
By 80 years old, what percent of Americans have or have had cataracts?
|
50%
|
|
|
How are cataracts described?
|
Based on location within lens
- Nuclear cataracts - center of lens - Cortical cataracts - layer surrounding lens - Posterior capsular cataracts - back outer layer of lens (more rapid progression) |
|
|
Which type of cataracts develop more rapidly?
|
Posterior Capsular Cataracts
|
|
|
How are cataracts removed?
|
Removal of the lens (phacoemulsification or extracapsular surgery) and implantation of an IOL (intraocular lens)
|
|
|
What are the structural components of the vitreous body?
|
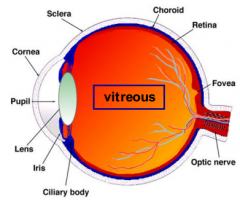
- Nearly acellular
- Major macromolecules: Type II collagen and hyaluronic acid - 99% water |
|
|
What is the function of the vitreous body?
|
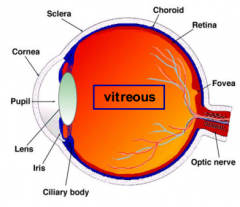
- Transparent structure
- Nutrition |
|
|
What are the two main layers of the retina?
|
1. Neural (sensory) retina
2. Retinal pigment epithelium (RPE) |
|
|
What is the location of the fovea relative to CN II?
|
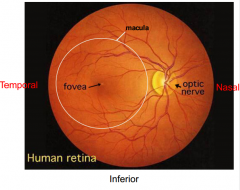
Fovea is temporal to CN II
|
|
|
What is the fovea?
|
Latin for small pit; region used for high acuity vision
|
|
|
What are the regional specializations of the neural (sensory) retina?
|
- Fovea
- Anteriorly, number of neural elements in retina declines, becoming a single layer of epithelium (unpigmented) that covers the ciliary body |
|
|
What are the layers of the neural retina (from external to internal - following path of light stimulus)?
|
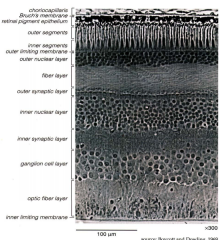
- Photoreceptor (rod and cone) outer and inner segments
- Outer nuclear layer (ONL) - Outer plexiform layer (OPL) - Inner nuclear layer (INL) - Inner plexiform layer (IPL) - Ganglion cell layer (GCL) - Nerve fiber layer (NFL) - Inner limiting lamina |
|
|
What is the most posterior (external) layer of the neural retina?
|
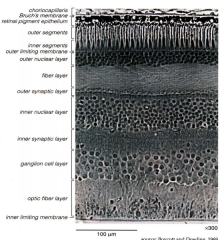
Photoreceptor (rod and cone) outer and inner segments
|
|
|
What is in the ONL?
|
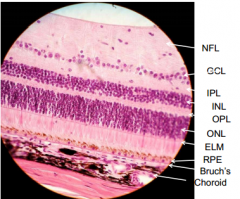
Outer nuclear layer - contains nuclei of rods and cones
|
|
|
What is in the OPL?
|
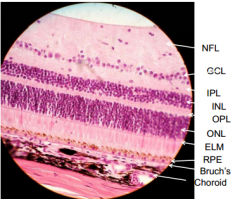
Outer plexiform layer - synapses of rod and cone axons w/ bipolar neurons
|
|
|
What is in the INL?
|
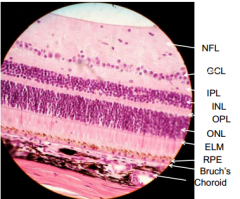
Inner Nuclear Layer - nuclei of bipolar neurons (also nuclei of horizontal and amacrine neurons and Muller glia)
|
|
|
What is in the IPL?
|
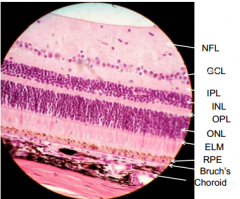
Inner Plexiform Layer - synapses of bipolar axons w/ ganglion cells
|
|
|
What is in the GCL?
|
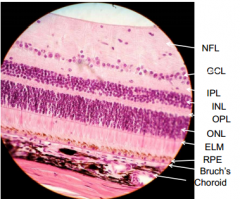
Ganglion Cell layer - nuclei of ganglion cells
|
|
|
What is in the NFL?
|
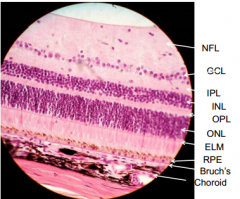
Nerve Fiber Layer - axons of ganglion cells that converge to form optic nerve
|
|
|
What is in the inner limiting lamina?
|
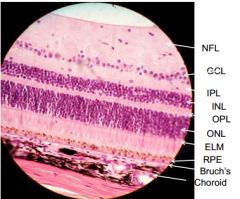
Basement membrane of Muller glial cells
|
|
|
What are the structural features of photoreceptors?
|
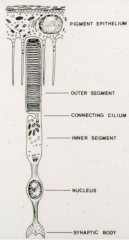
- Inner segments
- Outer segments - Connecting cilium |
|
|
What is in the outer segments of photoreceptors?
|
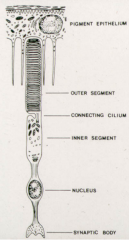
- Flattened membrane discs
- Photosensitive visual pigments (opsin) |
|
|
What structures are in the inner segment of a photoreceptor?
|
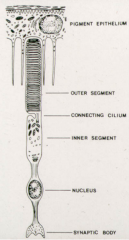
Organelles for protein synthesis and energy production
|
|
|
What happens in the connecting cilium of a photoreceptor?
|
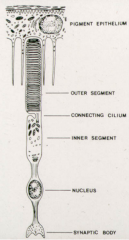
- Transport of proteins to outer segment from inner segment
- 10 billion opsin molecules / sec. |
|
|
What are the two types of photoreceptors?
|
- Rods
- Cones |
|
|
What are the features of a rod photoreceptor?
|
- Long, slender outer segments
- Numerous except at fovea - Very light-sensitive |
|
|
What are the features of a cone photoreceptor?
|
- Conical outer segments w/ membrane discs
- Less sensitive than rods - Responsible for high acuity and color vision |
|
|
Which photoreceptor is more sensitive?
|
Rods
|
|
|
Which photoreceptor has higher acuity?
|
Cones
|
|
|
How do the structures of the outer segments of photoreceptors differ?
|
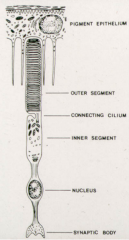
- Rods - long and slender; free floating discs
- Cones - conical w/ membrane discs; discs persist as folds |
|
|
When are rods active?
|
Active at night; inactive in light
|
|
|
How are the outer segments of photoreceptors formed?
|
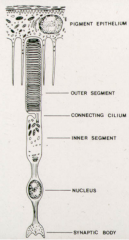
In folding of the plasma membrane:
- In rods the folds pinch off so the discs become free-floating - In cones the discs persist as folds and are in contact w/ extracellular space |
|
|
Where is the densest distribution of cones?
|
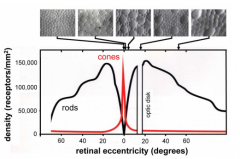
At 0 degrees (at fovea); basically none anywhere else
|
|
|
Where is the distribution of rods on the retina?
|
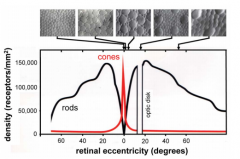
- Peaks about 20 degrees from fovea (around optic disk)
- None at fovea - Declines at increasing angles from 20 degrees |
|
|
The location of cone centers at the fovea forms what arrangment?
|
Triangular array
|
|
|
What happens during development of the fovea?
|
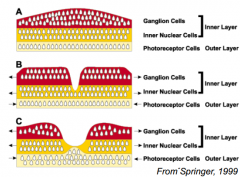
- Cone packing increases (increases visual acuity)
- Foveal pit develops after thickening of the retina - Site of incipient fovea is avascular all along |
|
|
What kind of cells are int he retinal pigment epithelium (RPE)?
|
Simple, cuboidal melanin-containing epithelial cells
|
|
|
What is the location of the retinal pigment epithelium (RPE)?
|
Between neural retina and Bruch's membrane (BM)
|
|
|
What are the function of the retinal pigment epithelium (RPE)?
|
- Provides outer blood-retinal barrier
- Absorbs scattered light (melanin) - Transports nutrients and ions between photoreceptors and choriocapillaries - Spatial buffering of ions in subretinal space - Reisomerization of all trans retinal - Outer segment renewal - Secretion of growth factors for maintenance and structural integrity of retina |
|
|
What does the retinal pigment epithelium (RPE) do for scattered light?
|
Absorbs it with melanin
|
|
|
The retinal pigment epithelium (RPE) transports nutrients and ions between what?
|
Photoreceptors and choriocapillaries
|
|
|
What does the retinal pigment epithelium (RPE) buffer?
|
Spatial buffering of ions in the subretinal space
|
|
|
What does the retinal pigment epithelium (RPE) do to retinal molecules?
|
Reisomerizes all trans retinal
|
|
|
What does the retinal pigment epithelium (RPE) do to the outer segments of photoreceptors?
|
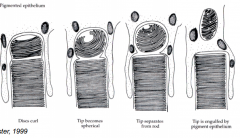
- RPE engulfs, digests, and recycles approx. 10% of mass of each photoreceptor outer segment per day
- Occurs on a diurnal schedule w/ peak of rod outer segment disc shedding occurring at dawn and peak of cone outer segment disc shedding occurring at dusk |
|
|
What does the retinal pigment epithelium (RPE) secrete?
|
Growth factors for maintenance and structural integrity of retina
|
|
|
How many photoreceptors are there per RPE cell?
|
~40 photoreceptors / RPE cell
|
|
|
When does outer segment phagocytosis happen for rods and cones?
|
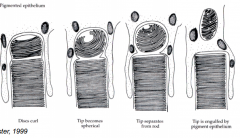
- Rods - at dawn
- Cones - at dusk |
|
|
Approximately every how many days is there a completely new outer segment on a photoreceptor?
|
Approximately every 10 days - because 10% is recycled per day
|
|
|
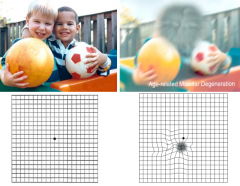
What is the leading cause of blindness in elderly in developed countries?
|
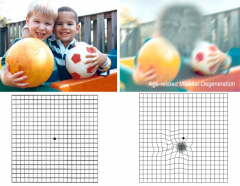
Age-related Macular Degeneration (AMD)
|
|
|
What happens in age-related macular degeneration (AMD)?
|

- Drusen develop within Bruch's membrane
- Vision loss is slow and deteriorates central vision first |
|
|
Which disease affects central vision first? Peripheral vision first?
|
Central vision - Age-Related Macular Degeneration (AMD)
Peripheral vision - Glaucoma |
|
|
What are the risk factors for AMD?
|
Family hx of AMD, smoking, blue eyes, CFH mutation
|
|
|
How do you treat macular degeneration?
|

Try to halt progression to "wet" with Anti-VEGF
|
|
|
What is in the center of the macula?
|
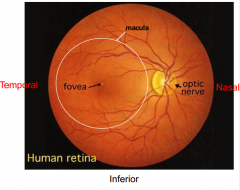
Fovea
|
|
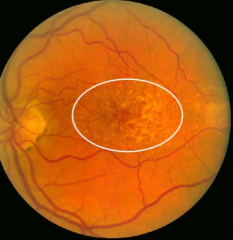
What is this a picture of?
|
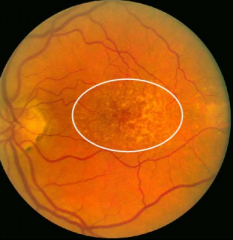
Are-related Macular Degeneration (AMD)
|
|
|
What arteries supply blood to the retina? Percent contribution?
|
ICA --> Ophthalmic Artery -->
- Retinal artery system (Central Retinal A.) ~30% - Ciliary artery system (Anterior and Posterior Ciliary aa.) ~70% |
|
|
What artery supplies the inner retina?
|
Central Retinal Artery
|
|
|
What artery supplies the cornea?
|
Anterior Ciliary Artery
|
|
|
Which arteries supplies the ciliary body?
|
- Anterior Ciliary A.
- Long Posterior Ciliary A. |
|
|
Which arteries supplies the iris?
|
- Anterior Ciliary A.
- Long Posterior Ciliary A. |
|
|
What artery supplies the choroid (outer retina)?
|
Short Posterior Ciliary A.
Choriocapillaries |
|
|
Which part of the eye receives the greatest blood flow? Why is this important?
|
Choroid (65-85%) - vital for maintenance of outer retina (photoreceptors in particular)
|
|
|
Where does the remaining blood that doesn't go to the choroid go?
|
Retina through the central retinal artery from the optic nerve head
|
|
|
The central retina artery is a branch from what? Begins where relative to the optic nerve head?
|
- Branch of ophthalmic artery
- Begins about 4 mm posterior to optic nerve head |
|
|
Does the central retinal artery branch?
|
- Divides into 2 main branches in the optic nerve
- Further divides to supply each quadrant of eye w/ an artery and vein |
|
|
The macular vessels arise from branches of what?
|
Superior Temporal and Inferotemporal arteries
|
|
|
What specializations happen at the fovea?
|
- Avascular zone
- Excavation of inner retinal neurons, foveal pit - High cone density - Absence of rods |
|
|
If there is impaired foveal specialization, what happens?
|
- Aniridia - absence of an iris
- Albinism - absence of pigment (melanin) |
|
|
What is albinism?
|
Inherited disorder of melanin biosynthesis - associated w/ absent or reduced melanin pigment in the eye, and often the skin and hair
|
|
|
How common is albinism?
|
1:17,000
|
|
|
What are the two principle types of albinism? Genetic linkage? Symptoms?
|
- Oculocutaneous albinism (OCA) - autosomal recessive; OCA1A-no pigment anywhere; OCA1B-some pigment due to leaky mutation allowing residual enzyme (tyrosinase)
- Ocular albinism (OA) - X-linked, typically normal skin and hair |
|
|
What are the universal albinism visual symptoms?
|
- Nystagmus - involuntary eye movement
- Refractive errors - Photophobia - Reduced acuity - Macular translucency - Iris transillumination - Altered retinostriate projections - Foveal hypoplasia (arrested foveal development) |
|
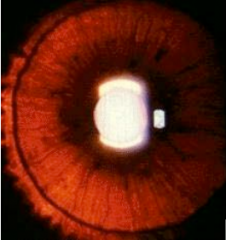
What is this? What is it a sign of?
|
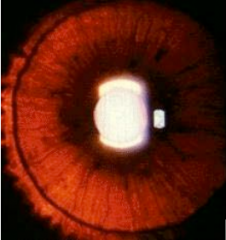
Iris transillumination - clinical sign of albinism
|
|
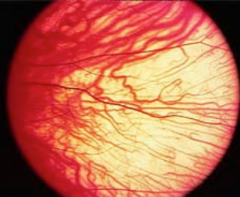
What is this? What is it a sign of?
|
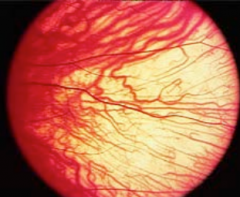
Macular Translucency - clinical sign of albinism
|
|
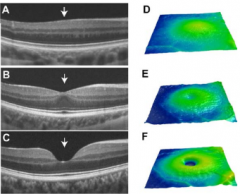
What is this? What is it a sign of?
|
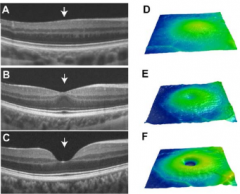
Foveal Hypoplasia (top) - clinical sign of albinism
(bottom two are normal) |
|
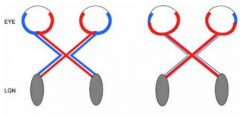
What is this? What is it a sign of?
|
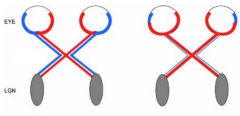
Altered Ipsi/Contra impairs stereo vision - clinical sign of albinism
(left is normal, right is albino) |

