![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
120 Cards in this Set
- Front
- Back
|
Juvenile Idiopathic Arthritis (JIA) - Definition
|
- occurring before the age of 16
- with persistent synovitis in one or more joints for at least 6 weeks (many prefer 3months) - all other diagnoses excluded |
|
|
JIA - 3 subtypes
|
Subtype varies according to how it presents in the 1st 6 months:
1) Oligoarticular (4 or fewer joints) 2) Polyarticular (>4 joints) 3) Systemic (spiking fevers) |
|
|
Outcome in JIA is most closely related to....
|
course after the first 6 months
|
|
|
JIA - etiology
|
- unclear
- thought to be autoimmune - some HLA alleles are important - some microbial Ag's may be important |
|
|
JIA - how is it initiated?
|
--> initiated by T-cell activation: presentation of antigens to T lymphocytes by APCs (macs, b-lymphs, fibroblasts)
--> T cell activation causes T and B lymphocyte production. --> cytokines are released including TNF-alpha, IL-1, and IL-6, which cause release of other mediators, such as prostaglandins, neutrophils, complement, proteases |
|
|
How is - SYSTEMIC JIA - activated?
|
mediated by IL-6 (and likely IL-1), which causes further migration of inflammatory cells into the synovia, which then damage synovial tissue, cartilage, and bone.
|
|
|
Characteristics of Synovium in JIA
|
- The inflamed synovia has lymphocytic and plasma cell infiltration (just like adult RA)
- WBC counts in synovial fluid are between 2,000 - 3,000/mL but can be as high as 100,000/mL - Panus formation occurs, which is growth of the synovium into the articular cartilage |
|
|
JIA Clues for Diagnosis:
|
- Morning stiffness that improves with movement later in the morning
- changes in walking, running, climbing, or willingness to play, esp in the morning hours - leg length discrepancies - return of need for assistance with dressing, eating, bathing, and toileting - enuresis may recur - developmental milestones may be lost |
|
|
Radiologic studies in JIA
|
non-specific early in the course, but...
- if fingers involved, look for widening of the mid-portion of the affected phalanges from periosteal new borne formation (takes months to years of active inflammation) |
|
|
OLIGOARTICULAR onset
(aka: pauciarticular) |
- 4 or fewer joints involved during the first 6 months of illness.
- 40-60% of JIA |
|
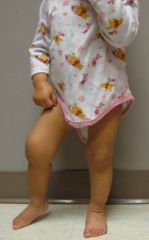
What is the cause of the Right Knee Joint swelling?
|
Oligoarticular JIA
|
|
|
OLIGOARTICULAR - demographic
|
- presents b/w 1-7yo, avg age is 5yo
- F:M 3:1 (overall) - F:M 6.5:1 (+uveitis) |
|
|
OLIGOARTICULAR - presenting symptoms
|
- slow onset
- usually present without many symptoms - ~25% are without any pain, showing up with incidental joint swelling |
|
|
OLIGOARTICULAR - joints most commonly involved
|
Most frequent to least:
knee --> ankle --> elbows --> wrists --> small joints of hands (10-15% of time) |
|
|
OLIGOARTICULAR - other findings
|
- rare to have findings other than arthritis in oligo (fever, rash, night pain are NOT seen)
- EXCEPT asymptomatic uveitis (occurs in ~30%) |
|
|
OLIGOARTICULAR - most important prognostic factor in developing uveitis
|
ANA(+) - predicts higher risk of developing uveitis
|
|
|
OLIGOARTICULAR - when does uveitis usually present?
|
- within the first 5-6 years of initial presentation
- screen more frequently in the early years, but continue annually in later years dt continued increased risk |
|
|
OLIGOARTICULAR - ophtho screening if ANA(+)
|
- within first 4-7 years and ANA(+) --> you need to perform ophthalmologic screening by SLIT-LAMP EXAM
- perform q3 months in the first 4 years of diagnosis - perform q6 months b/w 4-7 years of diagnosis |
|
|
OLIGOARTICULAR - uveitis or iridocyclitis
|
- inflmmation of the anterior uveal tract and the adjacent ciliary body
- most serious and most common complication - occurs in 20-25% - greatest risk: ANA+ and <6 yo - Uveitis is often silent, by time child complains of eye pain permanent damage has occurred. - COMPLETE slit lamp exam is necessary - complications: cataracts, synechiae, glaucoma, band keratopathy, macular edema - chronic uveitis results in permanent visual damage in >15% of affected pts despite Rx |
|
|
OLIGOARTICULAR - screening if ANA(-) and diagnosis is >7 years
|
- screen every 12 months
|
|
|
OLIGOARTICULAR - limb length discrepancy
|
- inflammation brings increased blood flow and nutrients
- results in boney overgrowth in length and width - knee and ankle joint injection with glucocorticoids early in the course may prevent leg length discrepancies |
|
|
OLIGOARTICULAR - labs
|
- NONspecific
- ANA(+) at least in low titer (< or = 1:320) in ~70% - RF and Hg are usually normal - ESR, CRP may be normal! |
|
|
OLIGOARTICULAR - long term articular outcome
|
- good, although some patients may develop limb-length discrepancy
- 25-30% will eventually develop a polyarticular course |
|
|
POLYARTICULAR - definition
|
- 30-40% of JIA
- 5 or more joints during the first 6 months |
|
|
POLYARTICULAR - demographic
|
- F:M ratio is 3:1
RF(+) mc older, usually adolescent RF(-) usually younger, with a peak incidence in the toddler age group |
|
|
POLYARTICULAR - joints affected
|
affects large and small joints and typically involves the cervical spine, hips, shoulders, and TMJ.
**symmetric joint involvement may be seen (similar to adult RA) - spine |
|
|
POLYARTICULAR - late findings
|
- cervical spine fusion
- micrognathia (**also represent late findings in SYSTEMIC) |
|
|
POLYARTICULAR - presenting symptoms
|
-fatigue (mc)
- also fever, weightloss, and rheumatoid nodules |
|
|
POLYARTICULAR - prognostic factors
|
RF(+) Polyarticular JIA: occurs in 10%, usu signifies a disease more similar to adult RA. Poor prognostic factor, signifies need for aggressive mgt
(anti-CCP antibody relevance has not been found) ANA(+) Polyarticular JIA: (occurs in 30%). Uveitis is less common, affecting only 10-15% with +ANA which is ~half of occurance in oligoarticular ANA+, <7 years old and polyarticular JIA: have intermediate risk of uveitis and should be monitored closely |
|
|
SYSTEMIC JIA - definition
|
requires occurrence of fever and other systemic findings
10-20% with JIA |
|
|
SYSTEMIC JIA - demographic
|
F:M 1:1, with peak age of 5-10 years.
|
|
|
SYSTEMIC JIA - key findings when febrile
|
1 or 2 fevers spikes to 103 degrees on a DAILY basis, which will return to normal without any antipyretics (quotidian or diquotidian fever pattern).
- Usually the fever is in the evening and can be associated with SEVERE MYALGIA and ARTHRALGIA. |
|
|
SYSTEMIC JIA - when Afebrile
|
when the fever is gone, the child appears better and may have no significant symptoms
|
|
|
SYSTEMIC JIA - things to look for, RASH
|
- usually associated with the fever
- migratory in appearance - macular - pink-to-salmon coloring - discrete borders - with or without central clearing - occurs on the TRUNK, THIGHS, and AXILLAE - KOEBNER phenomenon - mild irritation such as rubbing or scratching may cause the rash to appear - may be very pruritic or not - biopsy will show only nonspecific lymphocytic infiltration |
|
|
SYSTEMIC JIA - things to look for, Synovitis/Arthritis
|
- may or may not appear initially, but no dx until joint involvement presents
- Arthritis may occur as oligoarticular (~25-30%) or polyarticular (70-75%) involvement. |
|
|
SYSTEMIC JIA - worst prognostic indicators
|
- active disease 1 year after onset and diagnosis before 4 years of age
- also the amount of arthritis predicts long-term outcome - high aldolase, high ferritin in severe systemic illness |
|
|
SYSTEMIC JIA - signs/symptoms
|
- sick appearing with constitutional symptoms, FTT
- Rash - Synovitis/Arthritis - Severe myalgias (CPK usually normal, but ALDOLASE usually quite elevated in severe systemic illness) - pericarditis and myocarditis - pleuritis - lymphadenitis - hepatosplenomegaly (in 70%) - abdominal pain - weight loss and fatigue - Uveitis is rare! (<5%) |
|
|
SYSTEMIC JIA - labs
|
- occasional leukemoid reaction >40,000
- thrombocytosis (occasionally >1million) - high CRP and ESR - Anemia is common (microcytic anemia of chronic disease due to inability to utilize iron stores) - low albumin - Ferritin levels >4000 (nl <200) correspond to more severe systemic disease - RF always negative! - ANA is rarely positive |
|
|
JIA age of onset in various types
|
OLIGO - pk (2-3 yo), rare >10 yo
POLY - pk (2-5yo), 2pk (10-24 yo) SYST - no peak |
|
|
JIA and MAS
|
severely affected kids with JIA develop MAS - cytokine dysfunction resulting in uncontrolled accumulation of activated T cells and Macs in many organs
- elevated transaminases - coagulopathy with +DD, prolonged PTT - drop in plts, ESR - bone marrow with hemophagocytosis - may be triggered by viral infxn: EBV, CMV, HSV, VZV, parvo B19 - may be triggered by drugs: Sulfa drugs and NSAIDs - Monitor with labs 1-2x/wk and clnical (every 1-2 wks) - prompt tx with CORTICOSTEROIDS and CYCLOSPORINE if needed to prevent life-threatening complications - METHOTREXATE and SULFASALAZINE are contraindicated !!! |
|
|
DDx JIA
|
pain WITHOUT joint swelling - think of ortho problems like AVN, SCFE, OS, growing pains, benign hypermobility, psychogenic pain syndrome
DDx Systemic JIA - malignancies, SLE, acute rheumatic fever, serum sickness, Kawasakis |
|
|
Treatment for JIA - NSAIDs
|
- may be used initially, either with or without DMARDs
- duration of use should NOT be longer than a couple months if the pt has not reached complete remission - may be used in conjunction with other meds for symptom control |
|
|
Treatment for JIA - Intraarticular injection of Triamcinolone
|
- used if only a few joints involved (ie: oligo)
- shown to decrease occurrence of leg-length discrepancies (affected leg is longer due to extra bone deposition) |
|
|
Treatment for JIA - DMARDs (FDA-approved)
|
- FDA-approved: Methotrexate, sulfasalazine, leflunomide, TNF-inhibitors (eternercept and adalimumab), and T-cell modulators (abatacept)
|
|
|
Treatment for JIA - DMARDs (NOT FDA-approved)
|
- FDA - NON-approved = hydroxychloroquine, azathioprine, cyclophosphamide, infliximab (TNFinhibitor), anakinra (an IL-1 blocker).
|
|
|
Treatment for JIA - DMARDs (FDA-approved, examples)
|
- Methotrexate: usually the first DMARD to be used, given 1x/wk as pills or injected subQ
- Sulfasalazine and hydroxychloroquine: used less often bc there's less data - Cyclosporine: also used occasionally in polyarticular JIA along with MTX - Azathioprine, cyclophosphamide, and leflunomide: occasionally given for severe, resistent cases - Eternercept and adalimumab: appear to work well for polyarticular JIA but LESS well for systemic onset. - Abatacept, a soluble fusion protein that inhibits costimulation of T cells is also approved for polyarticular. - Anakinra: helpful for systemic |
|
|
Treatment for JIA - Intraarticular injection of Triamcinolone
|
- used if only a few joints involved (ie: oligo)
- shown to decrease occurrence of leg-length discrepancies (affected leg is longer due to extra bone deposition) |
|
|
Treatment for JIA - corticosteroids?
|
- not used unless periods of VERY severe disease, flares, or systemic manifestations
- try to use the lowest doses possible to minimize side effects (<0.25mg/kg/day or <10 mg/day) |
|
|
Treatment for JIA - DMARDs (FDA-approved)
|
- FDA-approved: Methotrexate, sulfasalazine, leflunomide, TNF-inhibitors (eternercept and adalimumab), and T-cell modulators (abatacept)
|
|
|
Outcomes of JIA
|
- follow q1-3months, but may be years before remission occurs
- 25-50% have functional limitations, but improved capacity over last 40yrs with better meds and joint replacement - 30-40% may have active synovitis as adults - mortality is rare <0.5% with systemic JIA died from amyloidosis in the past, now rarely seen due to better meds. - major causes of death: infections dt immunosuppression and MAS |
|
|
Treatment for JIA - DMARDs (NOT FDA-approved)
|
- FDA - NON-approved = hydroxychloroquine, azathioprine, cyclophosphamide, infliximab (TNFinhibitor), anakinra (an IL-1 blocker).
|
|
|
Treatment for JIA - DMARDs (FDA-approved, examples)
|
- Methotrexate: usually the first DMARD to be used, given 1x/wk as pills or injected subQ
- Sulfasalazine and hydroxychloroquine: used less often bc there's less data - Cyclosporine: also used occasionally in polyarticular JIA along with MTX - Azathioprine, cyclophosphamide, and leflunomide: occasionally given for severe, resistent cases - Eternercept and adalimumab: appear to work well for polyarticular JIA but LESS well for systemic onset. - Abatacept, a soluble fusion protein that inhibits costimulation of T cells is also approved for polyarticular. - Anakinra: helpful for systemic |
|
|
Treatment for JIA - corticosteroids?
|
- not used unless periods of VERY severe disease, flares, or systemic manifestations
- try to use the lowest doses possible to minimize side effects (<0.25mg/kg/day or <10 mg/day) |
|
|
Outcomes of JIA
|
- follow q1-3months, but may be years before remission occurs
- 25-50% have functional limitations, but improved capacity over last 40yrs with better meds and joint replacement - 30-40% may have active synovitis as adults - mortality is rare <0.5% with systemic JIA died from amyloidosis in the past, now rarely seen due to better meds. - major causes of death: infections dt immunosuppression and MAS |
|
|
Juvenile Spondyloarthropathy includes...
|
1) juvenile ankylosing spondylitis
2) post-infectious reactive arthritis (Reiter's) 3) inflammatory bowel disease (and its associated arthropathy) 4) juvenile psoriatic arthritis |
|
|
Juvenile Spondyloarthropathy - Enthesitis
|
means inflammation of the enthesis (which is where tendons, ligaments, or fasia attach to bone)
|
|
|
Enthesitis-related Arthropathies (as part of new classification schema for JIA)
|
1) juvenile spondyloarthropathy
2) SEA (syndrome of seronegativity, enthesopathy, and arthropathy) 3) HLA-B27-associated arthropathy and enthesopathy syndrome - oligoarticular onset JIA "type II" 4) juvenile ankylosing spondylitis |
|
|
Enthesitis-Related Arthropathies (ERA) - incidence
|
half as common as JIA, occuring in ~20/100,000
|
|
|
How are ERAs different compared to other childhood inflammatory arthritides?
|
- HLA-B27 association is variable (can range from 50% in psoriatic arthritis to 90% in ankylosing spondylitis)
- older children are affected - it is familial 10-20% of the time - arthritis is usually peripheral, with lower limb involvement in an asymmetric manner (except in psoriatic arthritis) |
|
|
You make the diagnosis of ERA in a child with chronic arthritis by these criteria:
|
1) The child has both ARTHRITIS + ENTHESITIS or...
2) ARTHRITIS or ENTHESITIS + at least 2 of: - Sacroiliac joint tenderness and/or inflammatory spinal pain - HLA-B27(+) - FHx of 1st or 2nd degree relative with HLA-B27(+) dz - Anterior Uveitis - Onset of arthritis in a boy after age 8 yo |
|
|
How do ERAs present clinically?
|
- usually boys
- morning pain and stiffness - pain relieved by playing or other activity - pain predominantly in the joints of the LOWER extremities (often in low back/buttocks) - pain at the entheses of the heels, feet, knees - the oligoarthritis is usually asymmetrical - the entheses that are affected may be exquisitely painful to palpation - can elicit sacroiliac pain to direct palpation or pelvic manipulation |
|
|
How common are constitutional symptoms in ERAs?
|
- less common; fever and weight loss occurring in fever than 10% of children with ERA.
- if growth delay is present, SUSPECT IBD !! - acute symptomatic iritis (ie: acutely painful, red eye) in ~ 5-10% |
|
|
Labs in ERAs?
|
ESR is normal in 50%
HLA-B27(+) in 50-90% IgA may be elevated |
|
|
ERAs - first line treatment
|
Begin treatment with NSAIDs; use for at least 1 month to see effect
- also orthotics made to redistribute weight away from the painful enthesis |
|
|
ERAs - second line treatment
|
- if NSAIDs not effective: 2nd line is Joint injection with triamcinolone, or sulfasalazine and methotrexate, especially for peripheral joint disease.
- these are not as effective for axial disease |
|
|
ERAs - best treatment for psoriatic arthritis or ankylosing spondylitis
|
- Etanercept
- Infliximab, adalimumab, and other anti-TNF therapies (also for IBD-associated arthropathy) |
|
|
ERAs - outcomes
|
- some have disease for only 3-6 months before it resolves
- those with chronic course are more likely to have complications |
|
|
ERAs - outcomes of chronic course
|
- sacroiliitis with spondylitis
- progress into adulthood with ankylosing disease of the back and sacroiliac joints - 80% of adult AS patients do fairly well |
|
|
Arthritis with IBD: incidence
|
occurs in ~25% of pts with IBD
|
|
|
Arthritis with IBD: characteristics of peripheral arthritis dz
|
Peripheral joints more commonly affected
- F=M - NOT associated with HLA-B27 - Arthritis flares with gut flares |
|
|
Arthritis with IBD: characteristics of axial arthritis dz
|
If axial arthritis occurs:
- Incidence in M>>F - ASSOCIATED with HLA-B27 - NOT dependent on gut flares |
|
|
Arthritis with IBD: symptoms and signs
|
constitutional symptoms: fatigue, weight loss, growth delay, fever, oral ulcers, abdominal pain/tenderness, diarrhea, erythema nodosum, pyoderma gangrenosum, clubbing
|
|
|
Arthritis with IBD: treatment Peripheral Arthritis
|
Peripheral Arthritis with a gut flare - will usually respond to appropriate therapy for the gut disease. So try corticosteroids and/or sulfasalazine.
|
|
|
Arthritis with IBD: treatment Axial Arthritis
|
Spine Disease - may need tx when gut inactive. Try Sulfasalazine, MTX, etanercept, Infliximab, Adalimumab.
**anti-TNF >> sulfasalazine and MTX for spine dz |
|
|
Juvenile Psoriatic Arthritis - diagnostic criteria
|
Clinical:
1) ARTHRITIS + PSORIASIS or... 2) ARTHRITIS + at least 2 of: - dactylitis - nail findings (pitting, oil spots, onycholysis) - FHx of psoriasis in 1st degree |
|
|
Juvenile Psoriatic Arthritis - distribution and clinical course of arthritis
|
- arthritis can precede the psoriasis by many years
- initially, the arthritis is an ASYMMETRIC, OLIGOARTHRITIS of SMALL and LARGE joints with DACTYLITIS. - DIP joint arthritis is common - eventually, the arthritis may become POLYARTHRITIS - some have chronic OLIGOARTHRITIS or DIP arthritis and NEVER progress to polyarthritis. |
|
|
Juvenile Psoriatic Arthritis - incidence of arthritis in cutaneous vs. nail psoriasis
|
- arthritis develops in ~7% patients with CUTANEOUS psoriasis
- arthritis develops in ~30% with psoriatic NAIL involvement |
|
|
Juvenile Psoriatic Arthritis - other complications
|
UVEITIS - is common
|
|
|
Juvenile Psoriatic Arthritis - labs
|
ANA positivity is common (30-50% of pts)
|
|
|
Juvenile Psoriatic Arthritis - gender distribution depends on age at presentation
|
- younger pts usu girls
- adolescents usu boys |
|
|
Reactive Arthritis - timing of onset
|
1-4 weeks after a GI infection
|
|
|
Reactive Arthritis - name infectious organisms responsible for triggering
|
- GI infection: Yersinia, Shigella, Salmonella, or Campylobacter, C. diff, Giardia
- GU infection: Chlamydia or Mycoplasma |
|
|
Reiter's Syndrome - diagnostic critera
|
Triad: Reactive Arthritis, conjunctivitis, Urethritis. (Urethritis occurs even if the infectious trigger was GI in origin)
|
|
|
Reactive Arthritis - Mucocutaneous Features
|
oral ulcers, genital ulcers, papular skin lesions
|
|
|
Reactive Arthritis - features of arthritis
|
- (enthesitis and dactylitis) that affects the LARGE, weight-bearing joints.
- arthritis may last 3-6 weeks, but can last for a few months |
|
|
Reactive Arthritis vs. Septic Arthritis
|
both p/w fever, systemic symptoms; may need to aspirate joint fluid and do gut, urethra, or conjunctiva cultures for study to prove otherwise
|
|
|
Reactive Arthritis - Treatment
|
Treat with NSAIDs.
- more severe cases may require - Abx therapy, such as doxycycline in children over age 7 yo. Abx is used as a remittive agent, although PCR can identify bacterial peptides in synovial tissue long after routine culture techniques are negative. - Resistant cases may require sulfasalazine, MTX, and/or anti-TNF agents |
|
|
Vasculitides - 3 classes (depending on size of the vessel)
|
Small-vessel: caused by immune complexes, p/w purpura and includes (drug rxns, Wegener's Granulomatosis, Serum Sickness, HSP)
Medium-vessel: causes organ system damage and incudes (polyarteritis nodosa (PAN) and Kawasakis) Large-vessel: may cause claudication symptoms; includes (Takayasu's arteritis) |
|
|
Henoch-Schonlein Purpura (aka Anaphylactoid Purpura) - incidence/demographic
|
the mc vasculitide in childhood
- mean age at diagnosis is 4 yo - >75% are under age 7 - age range 3-15, but can be seen in older adolescents and adults - M:F 2:1 |
|
|
HSP - seasonality
|
most cases in winter and spring
|
|
|
HSP - mechanism
|
IgA-mediated; it's a leukocytoclastic vasculitis with neutrophil infiltration in the vessel walls of arterioles, capillaries, and postcapillary venules. IgA and small amts of IgG and C3 are deposited
|
|
|
HSP - underlying cause
|
- in ~50% cases a URI infection precedes the disease
Triggers: **Bacterial (GAS pyogenes, Legionella, Mycoplasma, Yersinia); **Viruses (EBV, Varicella, CMV, parvovirus, hepatitis B); **Drugs (penicillin, cephalosporins, thiazide diuretics), vaccines (measles, yellow fever) **Food additives **Insect bites |
|
|
HSP - mc manifestation
|
RASH!
seen in ALL patients, and is the presenting finding in ~50% patients |
|
|
HSP - description of skin lesions
|
- begins as small wheels or red maculopapules --> progress to petechial and purpuric lesions
- found on LE and in dependent pressure-bearing areas (BUTTOCKS). - also, face, ears in younger children - rash lasts 4 days to 4 weeks **ANGIOEDEMA may precede the rash **ORCHITIS may be a hallmark of HSP !! |
|
|
HSP - arthritis outcome
|
NO associated chronic arthritis
|
|
|
HSP - second mc manifestation?
|
- Joint Involvement in ~25% pts
- arthritis/arthralgia can be the initial HSP symp (complicates dx until rash appears) - Usu. arthritis of LARGE joints (knee, ankles). - No joint effusions - PERIARTHRITIS with edema around joints and inflammation of tendon sheaths is the mc joint manifestation!! |
|
|
HSP - 3rd mc manifestation?
|
GI symptoms, occur in 65% pts: colicky abdominal pain, +/- vomiting. Pain can precede rash and other classic symptoms (dx more difficult until rash appears, may be confused with appendicitis)
|
|
|
HSP and GI bleeding
|
occult bleeding accompanies abdominal pain; 33% with MELENA; hematemesis rare; only 5% have major GI bleeding episode;
|
|
|
HSP - next step if abd pain is severe or persistent?
|
perform ULTRASOUND to r/o intussusception, which is NOT rare - especially ileoileal intussusception (2-14% of pts)
|
|
|
HSP and Abdominal US findings
|
AUS shows increased echogenicity and THICKENING of the wall of the 2nd portion of the DUODENUM and GB HYDROPS; occur ONLY if pt has GI symptoms
|
|
|
HSP - Renal Manifestations - Incidence
|
10-50% of those affected, usually mild and transient.
|
|
|
HSP - Renal Manifestations
|
Look for ISOLATED microscopic hematuria, or hematuria and proteinuria; mechanism: IgA deposition just like Berger Dz.
|
|
|
HSP - MC Renal Outcome
|
<1-2% have residual renal disease, and even fewer progress to end-stage renal disease.
|
|
|
HSP - RFs for permanent renal damage?
|
- > than 7 years old
- purpura lasting > 1 month - severe, persistent GI symp - decreased factor 13 |
|
|
HSP - other features
|
- orchitis
- pulmonary hemorrhage |
|
|
HSP - labs
|
clinical dx, no specific labs needed to confirm. Nonspecific findings include high WBC counts, elevated ESR (50% of pts), **elevated IgA**, NORMAL platelet and coag studies
|
|
|
HSP - studies
|
you can use ultrasound to look for inc. echogenicity and thickening of the wall in the 2nd portion of the duodenum and gallbladder, as well as for ileoileal intussusception
|
|
|
HSP - long term monitoring
|
Monitor closely for at least 3 months after dx for development of renal involvement
|
|
|
HSP - therapy
|
- no specific Rx;
- supportive outpt care sufficient. - no Rx for skin lesions unless severe and ulcerate, then use corticosteroids - non-steroidals for pain control, avoid if renal or GI dz - corticosteroids if severe abdominal pain or severe scrotal swelling/edema |
|
|
HSP nephritis - therapy?
|
- no therapy has shown benefit for HSP nephritis
- Most improve w/o specific therapy, although have been trials of IV methylprednisolone, cyclophosphamide, azathioprine |
|
|
HSP - outcome
|
- usu self-limited, lasting ~4wks in 65% children
- recurrences in up to 40% from 6 weeks to 2 years after initial presentation - prognosis is excellent with most problems stemming from acute GI bleeds early in illness or long term renal involvment |
|
|
MC Vasculitis of Childhood?
2nd MC Vasculitis? |
#1 - HSP
#2 - Kawasaki |
|
|
Leading cause of acquired heart disease in children in the US?
|
Kawasalki
|
|
|
Kawasaki - demographic and incidence
|
occurs in children under 5 years of age, affects boys more than girls (1.5:1), incidence highest in Asian children; Japan: incidence is 90/100,000 in kids <5 yo
|
|
|
Kawasaki - incidence of recurrence
|
nearly 1-3% have a recurrence, which is mc in boys > 6 yo or < 6 months
|
|
|
Kawasaki Disease - etiology
|
unknown, KD simulates an infectious disease but no organism can be identified. One theory - staphylococcal and streptococcal superantigen stimulation of the immune system
|
|
|
Kawasaki Disease - diagnostic criteria
|
FEVER for at least 5 days PLUS min. 4 of 5 of:
1) B/L conjunctival injection w/o exudate 2) Rash 3) MM changes (lips + oral cavity) - red pharynx, dry fissured lips, or injected, strawberry tongue 4) changes in peripheral extremities - edema or redness of the hands/feet --> later desquamation of fingers/toes 5) Cervical LAD - usu non fluctuant with at least 1 node of 1.5cm diameter (these 5 things occur with 80-90% frequency except for cervical LAD, which is 60-70%. **You can dx with <4 criteria if +coronary artery dz on echo |
|
|
Kawasaki Disease - describe the characteristic rash
|
usually macular, polymorphous with no vesicles, scaling, or crusting on the trunk AND frequently more prominent in the perineal area later in the course followed by desquamation of this area
|
|
|
3 stages of Kawasaki - Stage I
|
Stage 1 KD:
Acute phase: fever 1-2 weeks, 104 or >er, 4 of 5 major criteria. IRRITABILITY. Also: aseptic meningitis, acute uveitis, diarrhea, mild obstructive jaundice with elevated LFTs, GB hydrops, sterile pyuria. Polyarthritis or polyarthralgia (knees, ankles, hands) in 33%. Asprirated fluid with PMNs, Cx (-). |
|
|
3 stages of Kawasaki - Stage I cardiac manifestations
|
nearly 33% will have pericrdial effusions, and muocarditis. Coronary artery abnormalities can occur as early as day 3 of illness, buar are mc seen from 10 days to 4 weeeks after onset. Even with tx they are found in 5-9%. Increased risks in kids <1 yo, make, fever >16 days, cardiomegaly, arrhythmias other than Type I AV block, fever recurrence after 48 hrs of being afebrile.
|

