![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
73 Cards in this Set
- Front
- Back
|
Stages of wound healing
|
• Regeneration
o Restoring the tissue - new tissue is identical in structure and function to original tissue • Repair o Fibrous scar formation; normal structure and function is altered • Combined Mechanisms o Combining the two; MOST healing occurs with combined |
|
|
Four key successive phases
|
o Hemostasis
o Blood clots possible; hematoma 1. Vascular spasm (vasoconstriction) 2. Platelet plug formation 3. Blood coagulation o Inflammatory • Acute vs. Chronic o Proliferative • New tissues being formed • Fibroplasia – formation of fibrous scar tissue • Angiogenesis –formation of new blood vessels • Nerve growth o Remodeling/Maturation • Fibers becoming aligned, strengthening |
|
|
Bradykinin
|
• Stimulated by factor XII
• Promotes vasodilation and exudation |
|
|
o Prostaglandin
|
• Promotes vasodilation and edema
|
|
|
Nitric Oxide
|
-relaxes smooth muscle
vasodilation |
|
|
Edema Formation
|
• Exudate seeps into tissue spaces
• Has both positive and negative consequences |
|
|
Acute inflammation
|
Acute presents with:
1. Rubor (redness) 2. Tumor (swelling) 3. Calor (heat) 4. Dalor (pain) |
|
|
Chronic inflammation
|
Chronic Pain: may be associated with repetitive microtrauma, autoimmune responses, chronic conditions; does not have the cardinal signs of inflammation
|
|
|
Cryotherapy
|
o Primary goals of cryotherapy
• Limit edema • Reduce pain • Muscle relaxation/ contraction • Limit secondary hypoxic tissue injury |
|
|
• Thermotherapy
|
o Promote relaxation
o Pain relief o Increase blood flow o Facilitate tissue healing o Decrease muscle spasm o Prepare stiff joints for exercise |
|
|
• Ultrasound
|
o As deep heat:
• Joint contracture and scar tissue • Pain and muscle spasm • Subacute or chronic soft tissue inflammation • Requiring increased temperature or blood flow o Facilitate healing • Acute injury/inflammation of soft tissue or peripheral nerve • Open wounds • Fractures |
|
|
• Therapeutic levels of Heat
|
– Tissue must be increased to between 40°C and 45°C (104°F-113°F)
• This level is point of increased blood flow • Above this – potential to cause damage • Below this – sub-therapeutic |
|
|
Indications for Ice Massage
|
• Muscle belly, tendon, bursa, trigger points
|
|
|
Axon reflex
|
• Cutaneous thermoreceptors stimulated
• Impulse sent to spinal cord from cutaneous receptors – They also send signals toward skin blood vessels – A vasoactive mediator is released causing vasodilation and release of heat |
|
|
Release of chemical mediators
|
• Heat produces mild inflammation
• Chemical mediators released – Histamine and prostaglandins – Temperature elevation causes sweat secretion – Capillary permeability increases – Mild inflammation then occurs |
|
|
Local spinal cord reflex
|
• Cutaneous nerves send signal to spine
• Spinal cord sends signal to decrease sympathetic activity • Not relegated only to local region of treatment • Decrease in sympathetic activity allows vessels to vasodilate at the area (skin) where heat is applied so that the heat can then be dispersed. |
|
|
Stages of Repair Phase
|
- granulation
- fibroplasia - angiogenesis - re-epithelialization |
|
|
granulation
|
• Named for its cobbled appearance
• The fibrin matrix formed by platelets changes into granulation • Granulation presence indicates normal healing |
|
|
fibroplasia
|
• Fibroblasts drawn to wound from dermis by cytokines
• Fibroblasts then change into myofibroblasts • Caused by chemical mediators and low oxygen tension and oxygen pressure in the area • As new blood vessels are produced myofibroblast production slows • Collagen (Type III) is present in wound as soon as 2 days • Ground substance • Gelled material that forms the extracellular matrix • Facilitates fibroblast production and absorbs large amounts of water • Add flexibility and integrity to new tissue |
|
|
o Angiogenesis
|
• Occurs in various ways
• Sprouting of new pathway • Anastomosis with new and existing vascular paths • A response to: • Hypoxic environment • Free edge effect – no longer in contact • Cytokines |
|
|
o Re-epithelialization
|
• Cellular production and migration
• Important for providing barriers to infection and to decrease fluid loss • Concurrent with the formation of granulation tissue • Cellular Production • Contact inhibition is mediated by cytokines known as chalones o Chalones – inhibit mitosis; are not formed if there is damage to the cell (so mitosis can occur) • Migration • Process of cell movement from periphery to center • Occurs over granulation tissue |
|
|
acute pain
|
o Sharp
o Localized o Rapid onset o Short duration (usually) o Warning of tissue damage (actual or potential) |
|
|
Referred pain
|
o Pain at a site remote from the source of pathology
o It is believed that this pain occurs do to convergence o Brain unable to decipher or determine where pain is coming from |
|
|
• Persistent Pain
|
o Pain that is recurrent or episodic
o May accompany a re-injury o May be associated with chronic condition |
|
|
• Allodynia
|
pain is provoked by a stimulus that does not normally cause pain
|
|
|
• Hyperalgesia
|
heightened response to a painful stimulus
|
|
|
• Neuropathic
|
Complex Regional Pain Syndromes Types I & II
|
|
|
• Chronic Pain
|
pain lasting longer than 6 months
|
|
|
Reasons why someone may be in chronic pain
|
• Who goes into chronic pain state?
– Kids that play contact sports early are less likely to experience chronic pain • Predictors of chronic pain? – Happiness at work – Happiness at home • Dorsal Root Ganglion – If injured – 7 to 8x more likely to go into chronic pain, but don’t produce pain for 2-3 weeks |
|
|
How US works
|
• Reverse Piezoelectric Effect - voltage is applied, the crystal can compress or expand. The polarity of the voltage depends on whether a crystal is compressed or expanded.
|
|
|
What is BNR? (Ultrasound)
|
• Beam-Non-Uniformity Ratio
o Ratio between spatial peak intensity and spatial average intensity o Determined by quality of the crystal and construction of transducer o Required to be labeled on all machines and is usually listed on coaxial cable of the applicator o Ratios that are less than or equal to 6:1 are considered acceptable for clinical use |
|
|
Temperatures in which modalities become a threat
|
Heat above 113 F.
|
|
|
Neuropraxias
|
– nerve conduction is being blocked; no structural damage to nerve; temporary condition; brought on by use of cold therapy for as little as 1 hour (continous); will not reverse for 6-8 weeks
|
|
|
axonotomesis
|
discontinuity of axons; endo-, peri-, and epineurium are intact; brought on by continuous use of cold therapy for around 2 hours; is not reversible
|
|
|
• PRECAUTIONS with Cryotherapy
|
o Hypertension
o Over a superficial peripheral nerve o Over an open wound o Poor sensation o Poor cognition – poor understanding o Very young or very old o Aversion to cold – possible cold intolerance |
|
|
• PRECAUTIONS with Ultrasound
|
o Sensation of area being treated
o Communication or cognitive deficits o Poor circulation or vascularity o Treatment over plastic or metal implants o Bone cement is highly absorptive o Metal is highly reflective – increase risk of standing waves and increased heat or unstable cavitation. |
|
|
Chronic inflammation
|
• Histamine
o Itching, allergies • Kinin (bradykinin etc.) o Vasodilation o Pain-causing • Prostaglandin o Sensitize blood vessels to inflammatory mediators o Sensitize nociceptors – danger signal! • Complement o Enhance defenses |
|
|
Effective Radiating Area of US
|
• Actual cross-sectional area of the ultrasound beam exiting metal end plate
• Determined by size and vibrational properties of crystal • Always smaller than area of metal end plate • Expressed in square centimeters (cm²) |
|
|
• Thermal conductivity
|
o Efficiency of a material or tissue to conduct heat
o Metals more efficient than non-metals – artificial joint, body piercings, shrapnel, etc. o Materials with a higher water content usually have higher thermal conductivity o Muscles have a higher water content than fat. |
|
|
• Stereoaugnosis
|
o Placing a familiar object in the hand; patient identifies object
|
|
|
• Tactile location
|
o Where the pressure is being placed
|
|
|
• Barioaugnosis
|
o Two objects of different weights being placed in the hands; patient identifies which is heavier
|
|
|
• Graphesthesia
|
o Recognize a letter or design drawn on a body part (with eyes closed)
o Usually on the hand |
|
|
Expected cold sensations
|
Cold: Cold – Burn – Ache – Numb
|
|
|
• Contraindications for Cryotherapy
|
o Uticaria
o Cold Intolerance o Cryoglobulinemia • Abnormal blood proteins with exposure to cold • Can cause ischemia and gangrene o Raynaud’s Disease o Vasospastic disorder o Over a regenerating peripheral nerve • Do not want to slow down regeneration o Over an area of circulatory compromise o Over an area of peripheral vascular disease |
|
|
• Contraindications for Heat
|
o Over areas with lack of thermal sensation
o Vascular insufficiency or vascular disease o Over areas of recent hemorrhage or potential hemorrhage o Over areas of known malignancy o Over acute inflammation o Over infections or infected areas o Over areas where liniments or heat rubs have been applied |
|
|
• Contraindications for Ultrasound
|
o In the region of a cardiac pacemaker
o During pregnancy o Over abdominal, pelvic, or lumbar region o Over eyes and testes o In a region of active bleeding or infection o In a region of a tumor or malignancy o In a region of a DVT or thrombophlebitis o Over the heart, stellate or cervical ganglia o Over epiphyseal plates or growing bones o Over the spinal column o Cognition, language barriers, etc. |
|
|
-Spinothalamic tract
|
--Discrimitive pain
--Temperature --Crude touch --Pressure |
|
|
Spinomesencephalic tract
|
Pain modulation
Sensorimotor integration of pain Motor reflex to pain |
|
|
Spinoparabrachial tract
|
Affective component of pain
|
|
|
Spinoreticular tract
|
Modulation of pain
Motivational, emotional, unpleasant component of pain |
|
|
Spinohypothalamic-limbic tract
|
Autonomic adjustments to pain
|
|
|
take home from anterolateral system
|
The “Take-Home”
Multiple ascending pathways Ipsilateral, contralateral, bilateral Redundant system |
|
|
dull pain
|
bone
|
|
|
sharp pain
|
muscle, nerve
|
|
|
burning pain
|
nerve
|
|
|
tingling pain
|
nerve
|
|
|
What is pain?
|
Defined as
Unpleasant sensation Unpleasant emotional response Actual or potential tissue damage Warning signal so appropriate response evoked Has multiple components Integration of contextual and learned information |
|
|
A fibers
|
are fast and first of pain, myleinated, depending on source varies on conduction speed, but he faster of the 2
|
|
|
C fibers
|
are unmylienated, kick in after a month, respond to stimuli with stronger intensities, more associated w/ chronic pain
|
|
|
1 degrees c increase in US?
|
1°C to increase metabolic rate
|
|
|
2-3 C to increase in US
|
2°-3°C to reduce spasm and pain and to also increase blood flow
|
|
|
4 C increase in US
|
4°C to increase collagen extensibility and inhibit sympathetic activity
|
|
|
What 3 things does cryotherapy cause the body to do?
|
1.Decrease the bleeding and inflammation,2. decrease muscle spasm, allow for increase in the pain threshold
|
|
|
Convection cryotherapy in acute phase of healing
|
Not encouraged in acute phase of healing
Why????????????????? Can cause an increase in swelling and pooling in the dependent position |
|
|
Peripheral Nerve effects
|
Cooling to 56° F blocked conduction of A fibers
Lower than 56 to block C fibers. |
|
|
Cold transfers
|
• Occurs through conduction, convection, and evaporation
o Conduction – direct contact o Convection – through flow of air/liquid • Rarely used in therapy because body segment is usually placed in gravity-dependent position o Evaporation – cool liquid removes heat and is then evaporated (sweat) |
|
|
Heat transfer
|
Heat
• Conduction • Convection • Radiation o Conversion of heat energy to electromagnetic radiation o Rarely used (heat lamps) |
|
|
US Attenuation
|
• Measure of the decrease in sound energy as the US travels, either by absorption, reflection, or refraction.
|
|
|
Dermatome chart
|
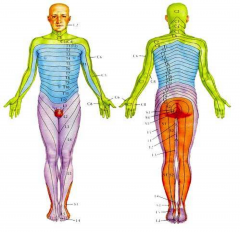
|
|
|
Phagocytosis photo
|
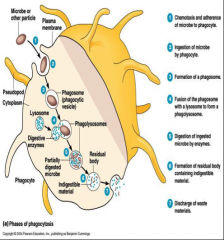
|
|
|
Gases and liquids- US
|
Longitudinal waves
Parallel to direction of energy flow |
|
|
Solids- US
|
Longitudinal and transverse waves
Perpendicular to direction of energy flow |

