![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
51 Cards in this Set
- Front
- Back
|
Penicillin G and Gram negative bugs
|
Gram-negatives are resistant to benzyl penicillin G. The gram-negative outer membrane layer inhibits entry of penicillin G and vancomycin. May be susceptible to penicillin derivatives such as ampicillin.
|
|
|
What bacteria genus can live in neutrophils?
|
Neisseria
|
|
|
How are neisseria characterized?
|
Gram-negative cocci that resemble paired coffee beans
|
|
|
Gonococcus and meningococcus: Polysaccharide capsule
|
G: No, M: Yes
|
|
|
Gonococcus and meningococcus: Maltose fermentation
|
G: No (Gonococcus ferments Glucose), M: Yes (MeninGococcus ferments Maltose and Glucose)
|
|
|
Gonococcus and meningococcus: Vaccine availability
|
G: No, M: Yes
|
|
|
What disease states does Gonococcus cause?
|
Gonorrhea, septic arthritis, neonatal conjunctivitis, PID
|
|
|
What disease states does Meningococcus cause?
|
Meningococcemia, Meningitis, Waterhouse-Friderichsen syndrome
|
|
|
What is Waterhouse-Friderichsen syndrome?
|
massive, usually bilateral, hemorrhage into the adrenal glands caused by fulminant meningococcemia. Characterised by overwhelming bacterial infection, rapidly progressive hypotension leading to shock, disseminated intravascular coagulation (DIC) with widespread purpura, particularly of the skin, and rapidly developing adrenocortical insufficiency associated with massive bilateral adrenal hemorrhage.
|
|
|
What disease states does Haemophilus Influenzae cause?
|
HaEMOPhilus causes: Epiglottitis, Meningitis, Otitis media, Pneumonia - Does not cause flu (that's a virus)!
|
|
|
How is Haemophilus Influenzae characterized?
|
Small gram-negative coccoid rod.
|
|
|
How is Haemophilus Influenzae transmitted?
|
Aerosol
|
|
|
Which type of Haemophilus Influenzae is most pathogenic?
|
capsular type B
|
|
|
Treatment for Haemophilus Influenzae meningitis
|
Ceftriaxone
|
|
|
Prophylaxis for Hemophilus Influenzae
|
Vaccine: Type B polysaccharide conjugated to diphtheria toxoid or other protein. Given between 2 and 18 months of age. Close contacts of infected person: Rifampin
|
|
|
How are enterobacteriaceae characterized?
|
Gram negative diverse group - Capsule (K [kapsular] antigen related to virulence of the bug), O antigen (somatic antigen which is the polysaccharide of endotoxin), Flagella (H antigen found in motile species), Ferment glucose, Enterobacteriaceae (woo!) (Mnemonic: COFFEe)
|
|
|
Enterobacteriaceae list
|
1. Escherichia coli, 2. Klebsiella pneumoniae, 3. Proteus mirablis, 4. Enterobacter sp., 5. Serratia, 6. Shigella, 7. Salmonella, 8. Yersinia enterocolitica
|
|
|
What disease states does Klebsiella cause?
|
1. Pneumonia in alcoholics and diabetics (In the name: Klebsiella pneumoniae), 2. Nosocomial UTIs (large mucoid capsule and viscous colonies), Mnemonic: AAA (Aspiration pneumonia, Abscess in lungs, Alcoholics)
|
|
|
Signs and symptoms of Klebsiella infection
|
1. Red currant jelly sputum 2. Abscess in lungs
|
|
|
Orange sputum: What bugs?
|
1. Pneumococcus 2. Klebsiella (or described as "red currant jelly sputum")
|
|
|
Red currant jelly sputum: What bug?
|
Klebsiella
|
|
|
Lactose-fermenting enteric bacteria
|
Mnemonic: Test lactose with MacConKEE'S - 1. Citrobacter 2. Klebsiella 3. E. coli 4. Enterobacter 5. Serratia
|
|
|
Salmonella vs. Shigella: Lactose fermenter?
|
Neither
|
|
|
Salmonella vs. Shigella: Motile
|
Both (Though, the evidence that shigella is motile is recent.) Can invade and disseminate hematogenously.
|
|
|
Salmonella vs. Shigella: Animal reservoir
|
Salmonella: Yes Shigella: No
|
|
|
Shigella transmission
|
4 Fs: 1. Food 2. Fingers 3. Feces 4. Flies
|
|
|
Salmonella vs. Shigella: Virulence
|
Salmonella: 100,000 organisms - Shigella: 10 organisms
|
|
|
True or False: Salmonellosis symptoms may be prolonged with antibiotic treatments
|
TRUE
|
|
|
What type of inflammatory response is seen in Salmonellosis?
|
Monocytes
|
|
|
Transmission of Yersinia enterocolitica
|
1. Pet feces (eg puppies) 2. Contaminated milk or pork
|
|
|
Yersinia enterocolitica infection: Clinical presentation
|
1. Outbreaks are common in day-care centers 2. Can mimic Crohn's or appendicitis
|
|
|
Disease states caused by Legionella (list only)
|
1. Asymptomatic infection, 2. Pontiac fever, 3. Legionnaires disease
|
|
|
Describe Pontiac fever
|
Caused by Legionella. Presents like influenza. Strikes suddenly and completely resolves in one week. Originally described in the Pontiac Michigan government AC.
|
|
|
Describe Legionnaires' disease
|
Very high fever with severe pneumonia
|
|
|
Treatment for Legionella
|
Has a beta-lacatamase (penicillin-resistant) - 1. Erythromycin, 2. Rifampin
|
|
|
Diagnosis: Pneumonia in a smoker >50 years of age. Gram stain of pus shows many neutrophils with few microbes.
|
Legionella
|
|
|
Special culture requirements for: Legionella
|
Grows on charcoal yeast extract culture with iron and cysteine Mnemonic: French legionnaire with silver helmet, sitting around a campfire (charcoal medium) with a canteen of water (water transmission) and his iron dagger-he is no sissy (cysteine).
|
|
|
Legionella: Gram stain
|
Gram negative. Gram stains poorly (use silver stain) Mnemonic: French legionnaire with silver helmet, sitting around a campfire (charcoal medium) with his iron dagger-he is no sissy (cysteine).
|
|
|
Legionella: How transmitted?
|
Aerosol transmission from environmental water sources (AC, Showers, whirlpools, cooling towers, supermarket produce mist) Mnemonic: French legionnaire with silver helmet, sitting around a campfire (charcoal medium) with a canteen of water (water transmission) and his iron dagger-he is no sissy (cysteine).
|
|
|
Pseudomonas: Disease states
|
PSEUDDOburnnas: 1. Pneumonia (especially in CF), 2. Sepsis (black lesions on skin), 3. External otitis (swimmer's ear), 4. UTI (nosocomial and drug-resistant), 5. Drug use, 6. Diabetic Osteomyelitis, 7. Burns and wound infections, 8. Hot tub folliculitis
|
|
|
Pseudomonas: Organism characterization
|
1. Gram-negative rod, 2. non-lactose fermenting, 3. Aerobic (think AERuginosa) and oxidase positive (cytochrome c oxidase for oxidative phosphorylation), 4. Produces pyocyanin (blue-green) pigment, 5. Fruity odor
|
|
|
What to know about exotoxins produced by: Pseudomonas aeruginosa
|
Exotoxin A is an ADP ribosylating A-B toxin (similar to Diphtheria toxin) - Mechanism: Inactivates elongation factor 2 (EF-2) - Also has endotoxin (as it is gram negative) which produces fever and shock.
|
|
|
Diagnosis: Sepsis in burn victim
|
Most likely Pseudomonas
|
|
|
Treatment for pseudomonas
|
Aminoglycoside plus Extended-spectrum penicillin (eg piperacillin, ticarcillin)
|
|
|
Helicobacter pylori: Disease states
|
Causes: 1. Gastritis 2. 90% of duodenal ulcers - Risk factor for: 1. Peptic ulcer 2. Gastric carcinoma
|
|
|
Helicobacter pylori: Characterization
|
1. Gram negative rod 2. Urease-positive 3. Creates alkaline environment
|
|
|
Treatment for Helicobacter Pylori
|
Triple treatment: 1. Metronidazole with one of the two combos: 2. Bismuth (eg Pepto-Bismol) 3. Either Tetracycline or Amoxicillin OR 2. Omeprazole 3. Clarithromycin
|
|
|
What bug?: Urease-positive gram-negative bacteria
|
Proteus and H. Pylori
|
|
|
Gardnerella: Characterization
|
Pleomorphic, gram-variable rod.
|
|
|
What disease states does Gardnernella cause?
|
Vaginosis: 1. Greenish vaginal discharge with fishy smell 2. Noninflammatory (nonpainful) 3. Mobiluncus (anaerobe) is also seen 4. Clue cells are visible (vaginal epithelium covered with bacteria) 5. Positive Whiff test
|
|
|
Clue cell, indicative of Gardnerella vaginosis
|
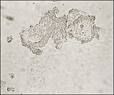
What is this?
|

