![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
54 Cards in this Set
- Front
- Back
|
What two organisms account for 80% of perinatal infections (labor/birth) ?
a. E.Coli and Bacteroides b. E.Coli and Group B strep c. E.Coli and Staph aures d. E.Coli and Neisseria gonorrhea |
E. coli and GBS, while 30% of infected infants either die or have sequale
|
|
|
If mother makes specific antibody and passe it to the fetus in sufficient quantity, infant will still manifest infection.
a. true b. false |
false: the antibodies from the mother are protective (or vaccination)
|
|
|
What is the major source of neonatal infections?
a. intrauterine b. post partum c. vaginal colonization d. congenital |
vaginal colonization of E.Coli and GBS, while intrauterine infections are less pathogenic organisms causing CNS damage manifested later
remember decreased antibodies against bug also predisposes neonates |
|
|
Why are premature infants at risk for infection?
a. due to lack of enough antibodies transferred for protection b. increased contact to blood borne bugs c. lack of surfactant leading to less protection d. weak membranes that act as barriers |
lack of enough antibodies transferred for protection
|
|
|
These bacteria are associated with early spontaneous delivery, EXCEPT:
a. ureaplamsa urelyticum b. mycoplasm hominis c. treponema pallidum d. gardnerelia vaginalis |
terponema pallidum (syphillis) is not associated with early spontaneous delivery
|
|
|
What is a physical protective barrier for neonates in utero?
a. antibodies circulating in blood b amnionic membrane c. amnionic fluid |
amnionic membrane -- impermeable to bacteria; if membranes rupture early and subsequent labor is long or delayed, the baby becomes susceptible to peripheral infection
|
|
|
What is the most common cause of spsis and meningitis in neonates?
a. GBS b. E.Coli c. S. aures d. N.gonorrhea |
GBS (50% of pregnant women infected)
|
|
|
When is the best time to screen pregnant mother for GBS?
a. 20-24 wks b. 34-37 wks c. 37-40 wks |
34-37 wks via vaginal and rectal culture
|
|
|
Who should be treated for GBS?
a. maternal carriers b. GBS UTI c. unscreened mothers |
all of the above should start prophylactic treatment of IV ampicillin 4 hours before labor according to studies this action make a big difference in outcomes of bacterial infection with GBS
|
|
|
What are some risk factors of GBS infection in pregnant women?
a. preterm labor b. fever during labor c. multiple births d. prolonged rupture of membrane |
all of the above
a. preterm labor (less antibiotic in system) b. fever during labor c. multiple births d. prolonged rupture of membrane (lack of protection from membrane) |
|
|
What are 3 vital actions in treating GBS?
a. act quickly b. spinal tap c. IV ampicillin and gentamycin d. IV acyclovir |
act quickly, spinal tap (CSF), and IV amicillin and gentamycin (synergistic); IV acyclovir is useful only with viruses
|
|
|
Pregnant women are considered immunocompromised, what opportunistic organism, intarcellular, is often pathogenic as it colonizes teh GI and GU, but it is not as explosive as GBS and E.coli
a. Staph aures b. Chlamydia c. listeria monocytogenes d. terponema pallidum |
listeria monocytogenes intarcellular often associated with soil and certain cheeses
|
|
|
What is the recommended treatment duration of GBS infection leading to sepsis?
a. 5-7 day b. 7-14 days c. 14-21 days d. 1 months |
7-14 days
|
|
|
What is the recommended treatment duration of GBS infection leading to meningitis?
a. 5-7 day b. 7-14 days c. 14-21 days d. 6 months |
14-21 days
|
|
|
The difference between infection and colonization is that
a. infection results in no systemic immune response b. infection results in organism invasion resulting in an immune response c. colonization results from organism invasion with an immune response d. colonization results in organism causing harm |
infection results in organism invasion resulting in an immune response
affliction: organism resulting in harm colonization: organism on surface/mucus does not lead to systemic immune response |
|
|
What three neonatal infections can be treated with medication in pregnant women?
a. toxoplasma gondii b. rubella virus c. treponema pallidum d. HIV |
toxoplasma gondii (protozoan), treponema pallidum (syphillis), and HIV
all have treatment for pregnant infected women |
|
|
THese three neonatal afflictions have preventable vaccines?
a. rubella virus b. cytomegalovirus c. varicella zoster virus d. HBV |
rubella virus, varicella zoster virus (VZV),and HBV all have vaccines (preventable disease)
|
|
|
These three neonatal infections have neither vaccination or treatment in pregnant women?
a. CMV b. HSV c. VZV d. parvovirus |
CMV, HSV, and parovirus (neither vaccine or treatment)
|
|
|
What is a good measure reflecting pregnant women's hx of previous infection?
a. IgM b. IgG c. IgE |
IgG (is positive for agents that have previously infected mother (even prior to gestation)
|
|
|
temporary clinical manifestations of TORCHES include, EXCEPT?
a. microcephaly b. jaundice c. hepatosplenomegaly d. bone lesions |
jaundice, hepatosplenomegaly, and bone lesions are all temporary clinical manifestations of TORCHES
|
|
|
What two viruses can cause deafness in neonates?
a. HIV and CMV b. HSV and CMV c. rubella and CMV d. HSV and rubella B. |
rubella and CMV
|
|
|
neonate is presented to you with microcephaly, opthalmologic abnormalities, and risk for mental retardation. What can be suspected?
a. HIV infection b. premature delivery c. lack of surfactant d. TORCHES syndrome |
TORCHES syndrome (Toxoplasmosa, Rubella, CMV, HSV, VSV, Syphillis
|
|
|
congenital afflictions via primary infection are often more dangerous than reactive (recurrent) infection, caused by all EXCEPT:
a. toxoplasma b. rubella c. CMV d. HSV |
toxoplasma, rubella, HSV, VZV, and parovirus (NOT CMV, treponema pallidum, HBV, and HIV)
|
|
|
Pregnant female has a diagnosis of HSV, what can be done to prevent neonatal spread?
a. vaccination b. C-section c. treat w/acyclovir d. normal delivery will not harm neonate |
C-section, since there is no vaccine or treatment for HSV it is better if neonate is delivered via C-section to avoid perinatal affliction
|
|
|
What has the highest congenital risk affliction if neonate or mom are not treated?
a. HBV b. treponema pallidum c. rubella d. CMV |
HBV (90%) congenital risk of affliction (harm) associated with primary maternal infection
|
|
|
Why is it important to save the PLACENTA of women infected with toxoplasmosis.
a. biopsy required b. difficult to culture c. detection of IgG |
difficult to culture (need placenta) IgG from the mother turns OFF neonates own IgG synthesis for 4 months and maternal IgG disappears after 6 months
remember for the firs 4 months IgG may appear to be decreasing, but neonate may still be infected (physiological response due to maternal antibodies) |
|
|
What treatment is indicated for neonate afflicted with toxoplasmosis (protozoan)
a. pyrimethamine/sulfadiazine with folic acid b. acyclovir c. PCN d. ganciclovir |
pyrimethamine/sulfadiazine with folic acid (prevents adolescent blindness)
|
|
|
What can decrease congenital affliction with toxoplasmosis?
a. vaccination b. maternal treatment at 16wk gestation c. maternal treatment immediately d. administer IgG |
maternal treatment at 16wk gestation
|
|
|
What is significant about toxoplasmosis acquired during the 1st, 2nd, or 3rd trimester?
a. infection during the 1st trimester results in less congenital infections and more subclinical infections b. infection during the 2nd trimester results in more congenital infections and more subclinical infections c. infection during the 3rd trimester results in less congenital afflictions and more subclinical afflictions d. the first 4 wks of gestation results in 100% congenital affliction |
a. false: infection during the 1st trimester results in more congenital disease (7% severe) and less subclinical (most are seen in 3rd trimester)
b. false: infection during the 2nd trimester results in more congenital afflictions and less subclincal c. true: infections during the 3rd trimester results in less congenital afflictions and more subclinical afflictions (amnionic barrier) d. false: first 4 weeks of 1st trimester results in spontaneous abortions Why? because after 3 rd trimester amnionic membrane protects fetus from infection (barrier is built) |
|
|
What is the most common cause of congenital blindness, often preventable?
a. rubella b. HSV c. CMV d. toxoplasmosis |
Preventable because there is treatment for toxoplasmosis--> pyrimethamine/sulfadiazine with folic acid
|
|
|
Although genetic/metabolic conditions are the most common cause of cataracts, what neonatal affliction can also cause cataracts?
a. rubella b. toxoplasmosis c. CMV d. HBV |
rubella
|
|
|
3month old neonate recently moved from Costa Rica, presents with low birth weight, purpura, hepatitis/jaundice, and bony abnormalities. You determine that this condition is preventable, as it can lead to hearing loss, cataracts, heart disease and mental retardation. what diagnostic tool is appropriate?
a. viral culture b. serology IgM c. PNA PCR d. antigen detection/PCR |
viral culture is the best: Rubella (mother was probably not vaccinated or did not vaccinate child)
|
|
|
pregnant female comes in with her 5 y/o boy, stating that she is not feeling well with flu-like symptoms (fever, adenopathy, hepatitis, pneumonia). Because her child is in daycare you want to r/o what viral infection in the pregnant mother often caused via sexual, hematogonous transmission, and oral secretions. You are concered about TOrCHES infections causing developmental delays and deafness. How can she be tested?
a. viral culture of amnionic fluid b. serology IgM c. PNA PCR d. antigen detection PCR |
testing for CMV often spread in daycares (41% infection rate) and she has a 25% risk of congenital affliction to neonate:
viral culture of amnionic fluid, urine, or respiratory secretions, BUFFY coat cells, PCR on amnionic fluid, blood, or saliva you can treat mother with hyperimmuneIgG or antiviral remnants (although inadequately studied) |
|
|
Why is it vital to perform an EEG on a neonate infected with congenital CMV?
a. risk of epilepsy b. silent seizures interfere with brain development c. silent seizures can result in hearing loss d. silent seizures interfere with ocular development |
this is a preventable cause of poor brain mental development, when you can control the silent seizures
|
|
|
What is an optimal treatment for CMV?
a. acyclovir b. ganciclovir or valganciclovir c. hyper ImmuneIgG d. benzathine PCN G |
ganciclovir or valganciclovir
|
|
|
This virus has a 50% risk of neonatal infeciton (perinatal) with 25% sever affliction --> death, while there is a 1% severe affliction and 5% miscarriage if there is a primary maternal infection (congenital risk). Meaning there is a high change of transmission during labor. It is a common infeciton often aysmptomatic. What can be done to decrease the incidence of infection.
a. vaginal delivery b. C-section > 4hr post ROM c. early C-section d. C-section on target of delivery date |
early C-section decreases the incidence of infection dramatically from 54% (vaginal) > 94% C-section after 4 hr ROM to > 7% early C-section
this can save lives and remember HSV II (70%), while HSVI (30%) |
|
|
What is the MAjOR reason there is less of a risk of congenital HSVII spread when compared to perinatal HSVII.
a. increase maternal antibody levels b. placenta and amnionic membrane protection c. increase in cell mediated immunity |
placenta and amnionic membrane protection -- against congenital spread, but the neonate is still at risk of perinatal spread due to delivery through birth canal and antibodies do not protect neonate through birth canal; cell mediated immunity is not present until later months in neonate
|
|
|
What is an easily obtained and rapid test to diagnose HSV in neonates, for quick diagnosis and early treatment of acyclovir?
a. viral culture b. IgM sepcific serology c. HSV specific antigen d. PCR of CSF and blood |
best answer is PCR of CSF and blood
others are ok to use, remember HSV needs to be diagnosed early and treated early with acyclovir, so use appropriate diagnostic tool |
|
|
maternal HB surface antigen positivity MANDATES preventive treatment of infant
a. true b. false |
TRUE
1) HBIG at birth 2) 1st HB vaccine dose at birth 3) 2nd HB vaccine dose in 1 month 4) 3rd HB vaccine dose in 6 months |
|
|
All are helpful diagnostic tools for congenital HBV EXCEPT:
a. IgM specific serology of infant b. maternal HB surface antigen c. HBe antigen detection in infant d. viral culture |
a. IgM specific serology of infant
b. maternal HB surface antigen c. HBe antigen detection in infant all are useful in congenital HBV diagnosis |
|
|
Unlike HSV, HBV has a higher risk for congenital transmission (50% vs. 1%), and while early C-section can improve the rates of perinatal transmission in HSV, what can improve the rate of perinatal transmission in HBV?
a. also early C-section b. give HBV vaccine to infant c. treat with acyclovir d. give mother hyperIg and HBV vaccine to infant |
give mother hyperIg and HBV vaccine to infant
give HBV vaccine depending on the category: chronic carrier + untreated child (as you treat the child the risks decrease from 90% --> 5%) optimal is 1 dose of hyper Ig + 3 dose vaccine for infant 5% |
|
|
When trying to prevent HBV transmission in neonates, what is the difference if mohter is HBsAg positive or HBsAg negative. When in doubt treat as HBsAg positive and give:
a. no HBIG b. HBV vaccine w/in 2 months c. 2nd vaccine 1-2 months later and 3rd vaccine 6-18 months later d. give HBIG at birth |
steps for HBsAg positive mother:
a. HBIG at birth b. 1st HBV vaccine at birth c. 2nd HBV vaccine 1 month, 3rd at 6 months steps for a HBsAg negative mother: a. no HBIG b. HBV vaccine w/in 2 months c. 2nd vaccine 1-2 months later and 3rd vaccine 6-18 months later |
|
|
congenital VZV, similar to HSV is rare/infrequent due to 90% of adults protected from previous infection or vaccine, but perinatal spread is DANGEROUS if primary infection is manifested w/in 5 days before or after birth of baby. Varicella can disseminate to brain, lung, and liver. How can the neonate be treated in this case.
a. give acyclovir b. give VZIG c. give acyclovir and VZIG d. perinatal transmission can't be treated |
give VZIG first
if mother develops symptoms near time of delivery give neonate VZIG (varicella zoster hyperimmunoglobulin); if neonate develops symptoms then give acyclovir d. congenital varicella can't be treated |
|
|
What is not reliable when diagnosing HVZ (VZV)? remember clinical diagnosis of acute maternal varicella maybe lifesaving for the neonate!!
a. IgM specific antibody b. HVZ viral culture c. HVZ antigen detection d. HVZ specific PCR |
all are EXCEPT IgM specific antibody
|
|
|
Why is HSV and VZV so deadly in perinatal transmission?
a. decreased cell-mediated immunity in neonate b. decreased humoral mediated immunity in neonates c. poor functioning liver d. low macrophage count |
decreased cell mediated immunity which often combats these viruses easily
|
|
|
Syphillis, Rubella, and HIV often share similarities in that they all have high incidence of congenital transmission, while Rubella offers a vaccine for prevention what is significant about early diagnosis of syphillis:
a. it is not preventable often leading to abortion, stillbirth, or congenital affliction b. it is completely preventable with prenatal treatment of mother c. is is preventable with vaccination d. is preventable with early C-section |
b. completely preventable with prenatal treatment of mother prior to 16 weeks gestation with benzathine PCN G (IV), and if there is also HIV use a higher dose
although congenital syphillis still has a 50% mortality rate despite treatment if neonate is born w/disease |
|
|
What two test are useful in diagnosing syphillis?
a. RPR/VDRL (high sensitivity/low specificity) b. FTA-ABS or TPHA (measure IgG) (high specificity) c. IgM specific test |
a. RPR/VDRL (high sensitivity/low specificity)
b. FTA-ABS or TPHA (measure IgG) (high specificity) while IgM are not yet reliable |
|
|
What are important tools available to evaluate an infant for syphillis?
a. meticulous physical exam b. long bone X-ray c. serology d. LP with CSF analysis e. CXR for pneumonia |
all of the above are vital
a. meticulous physical exam b. long bone X-ray c. serology d. LP with CSF analysis e. CXR for pneumonia |
|
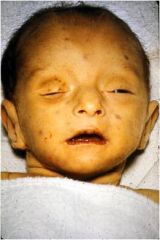
32y/o female recently immigrated from Africa, has not received MMR vaccine. Comes in with 2 month old boy, low birth weight, purpura, heptitis/jaundice, bony abnormalities, endocrine abnormalities What is the BEST tool to help you make the diagnosis:
a. viral culture b. IgM serology c. RNA PCR d. maternal surface antigen |
boy has congenital RUBeLLA
viral culture is the BEST IgM ~ 50% accurate and RNA PCR is not always available Rubella syndrome: low birth weight, purpura, heptitis/jaundice, bony abnormalities, endocrine abnormalities |
|
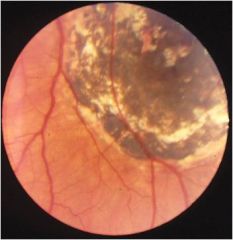
Neonates presents with hepatomegdaly, hypogonadism, and microcephaly. His condition is commonly associated with adolescent blindness. How can you diagnose this condition:
a. IgG b. IgM serology c. save placenta d. PCR on amniotic fluid |
save the placenta it is the best way for detection of Toxoplasmosis
treat neonate with pyrimethamine/sulfadiazine maternal treatment after 16 wk gestation reduces congenital affliction |
|
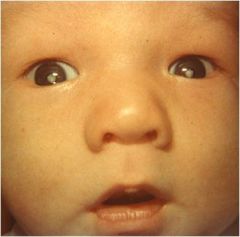
Often diagnosed with viral culture, preventable with vaccine, associated with syndrome resulting in low-birth weight, purpura, hepatitis/jaundice, bony abnormalities, and endocrine abnormalities
a. CMV b. rubella c. VZV d. HBV |
rubella
although all others also have a vaccine except CMV |
|
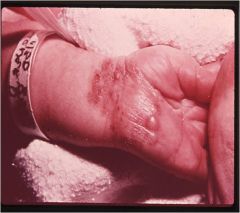
Early C-section is life saving ot avoid perinatal transmission. Diagnosed via viral culture, IgM (not reliable), viral specific antigen, and PCR of CSF and blood. Early diagnosis and early treatment are KEY.
a. CMV b. HSV c. rubella d. syphillis |
HSV treat with acyclovir
|
|
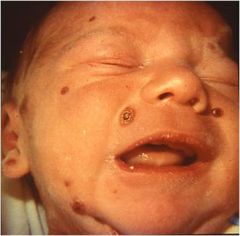
Congenital form has not treatment, but perinatal transmission is treated, otherwise it is quiet dangerous resulting in disseminated disease from skin to brain, lungs, and liver. Diagnosed with viral culture, antigen detection, and viral specific PCR.
a. rubella b. HSV c. Varicella d. syphillis |
Varicella
give hyperimmuneglobulin VZIg, if symptoms present give acyclovir |
|
|
Preventable disease if treat mother with benzathine PCN G (IV), screen with RPR/VDRL and FTA-ABS or TPHA. Evaluate neonate withe meticulous physical exam, long bone X-ray, serology, LP with CSF, and CXR for pneumonia
a. CMV b. HSV c. syphillis d. Rubella |
syphillis preventable with treatment of mother
|

