![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
77 Cards in this Set
- Front
- Back
|
Diabetes Mellitus
-definition |
-relative or absolute absence of insulin production or action
-metabolic disease characterized by abnormal CHO and lipid metabolism |
|
|
Ketoacidosis
-definition |
-metabolic acidosis caused by the accumulation of ketoacids
-can occur without acidosis |
|
|
3 Main ketone bodies
|
-acetoacetic acid
-beta-hydroxybutyrate -acetone* *not a metabolic acid |
|
|
Gucosuria
-define |
-glucose in the urine
-always abnormal |
|
|
Ketoacidosis
-mainly due to |
-diabetes
|
|
|
Main hormones produced in the islet of langerhans
|
-glucagon
-somatostatin -insulin |
|
|
Cells producing:
-glucagon -insulin -somatostatin |
-glucagon = alpha-cells
-insulin = beta-cells -somatostatin = delta-cells |
|
|
Majority of the Islet of Langerhans made up of
|
-Beta-cells
|
|
|
Islet of Langerhans
-function influenced by |
-circulating hormones
-gut hormones -autonomic nerves -nutrients |
|
|
Why is there generally a higher response to oral glucose than IV glucose?
|
-gut hormones
|
|
|
Actions stimulated by insulin
|
*blocks catabolism
Glucose uptake: -muscle -adipose -liver Amino acid uptake: -muscle Free fatty acid uptake: -adipose Glucose conversion to glycogen in liver |
|
|
Actions inhibited by insulin
|
-muscle breakdown to amino acids
-adipose tissue breakdown to free fatty acids |
|
|
Actions stimulated by glucagon
|
-glycogenolysis & gluconeogenesis in liver
-glucose release from liver -adipose tissue conversion to ketone bodies |
|
|
Major pathology of diabetes
|
Islet defect
-impaired insulin secretion (Dog = beta cell loss, Cat = impaired cell function) Peripheral defect -impaired insulin action (cat = insulin resistance) |
|
|
Where is impaired insulin action a main concern?
|
-muscle
|
|
|
Diabetes classifications
|
-Type 1 = insulin dependent (islets targeted)
-Type 2 = non-insulin dependent -Transient DM = variable need for insulin; glucose toxicity -Type 3 (Secondary) DM = physiologic/pathologic factors causing insulin resistance |
|
|
Type 1 diabetes
-most common in |
-Dog
|
|
|
Type 2 diabetes
-most common in |
-cats
|
|
|
Transient diabetes
-most common in |
-cats
|
|
|
Type 3 (secondary) DM
-example |
-gestational diabetes in dogs (resolution after birth)
|
|
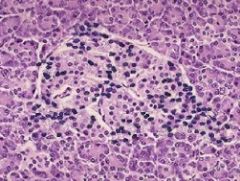
-Pathology
-effect |
-Lymphocytic insulinitis
-targets beta-cells |
|
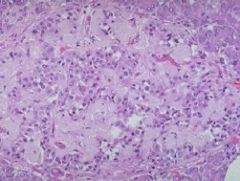
-pathology
-effect |
-Amylin deposition
--production by beta-cells -possible etiology in cats |
|
|
Relationship between obesity and insulin resistance
|
-cost to maintain normoglycemia is higher
-insulin is not as effective in the obese patient |
|
|
Insulin resistant
-aka |
-glucose intolerant
|
|
|
Relationship between body condition score and glucose tolerance
-why? |
-higher BCS = more glucose intolerant
-elongation of glucose tolerance curve -insulin is not activated as quickly and is not as effective in patients with a higher BCS |
|
|
Animals that typically have a longer glucose tolerance curve
|
-carnivores
*reason why different normal are needed b/n species |
|
|
Islet pathology and/or peripheral insulin defect promotes _____.
|
-glucose intolerance
|
|
|
What is a definite that will be needed at the time of diagnosis for DM?
|
-insulin
|
|
|
Renal threshold for glucose absorption in:
-dog -cat |
-dog = 180 mg/dl
-cat = 200+ mg/dl *above these values in circulating blood, we can call diabetic |
|
|
Pre-diabetic
-circulating glucose values |
150-220 mg/dL
|
|
|
Diabetes Mellitus
-signalment generalizations (gender, age, breed) |
Gender
-Dogs: female -Cats: male Age -middle aged and older Breed -Dogs: Cairn terriers, poodles, dachshunds, min schnauzer -Cats: Burmese (Australia), Siamese |
|
|
Diabetes Mellitus
-clinical signs |
-classical triad (Polydipsia, Polyphagia, Polyuria)
-weight loss -obesity -occasional cataracts (dogs), neuropathy (cats), asymptomatic hyperglycemia |
|
|
Diabetes Mellitus
-minimum data base |
-CBC
-Serum biochem (w/ T4 in cats) -Urinalysis -Urine culture -Serum fructosamine (optional) |
|
|
Diabetes mellitus
-CBC results |
-usually normal
|
|
|
Diabetes Mellitus
-Biochemistry panel results |
-hyperglycemia
-elevated ALP & ALT ("noisy") -Inc. serum triglycerides |
|
|
Approx. normal blood glucose level across most species
|
-100 mg/dl
|
|
|
Diabetes mellitus
-urinalysis & urine culture results |
-glucosuria
-ketonuria -proteinuria -pyuria -bacteria |
|
|
What does finding of glucosuria mean?
|
-Blood glucose has been above threshold for a period of time
|
|
|
Diabetes mellitus
-reason for increased serum triglycerides in biochem panel |
-insulin deficiency
--lipoprotein lipase becomes inactive ---inc. in circulating VLDLs and chylomicrons |
|
|
Diabetes mellitus
-distinguishing from stress hyperglycemia |
-glucosuria rarely present
-ketonuria never present -recheck urine glucose at home in 48-72 hrs -serum fructosamine test (will only be high if stress hyperglycemia is aroung for more the 3-4 days) |
|
|
Serum fructosamine test
-shows a representation of what? |
-average. glucose levels in the 2 wk period before the test
|
|
|
Diabetes mellitus
-actions in starting treatment |
-client education/training (syringe handling, hypoglycemia awareness, etc.)
-determining the insulin type to be used -assessing other factors (diet, meds, supplements, etc.) -follow-up plan (rechecks, callbacks, progress reports) |
|
|
Diabetes mellitus
-goals of treatment |
-eliminate clinical signs
-address contributing factors -control hyperglycemia -avoid hypoglycemia -make treatment convenient |
|
|
Diabetes mellitus
-ways to control hyperglycemia |
-insulin
-exercise/diet (rare efficacy when used alone) -oral hypoglycemic drugs |
|
|
Diabetes mellitus
-treatment of choice |
-insulin
|
|
|
What would ideal insulin therapy accomplish?
|
-it would replicate the physiological insulin profile
|
|
|
Normal insulin profile
-describe |
-normal basal level (never 0)
-spikes (regular with meals) |
|
|
Short acting Insulins
-primary use |
-CRI for emergency treatment
|
|
|
Intermediate Acting Insulin
-primary use |
-dogs
-occasional cats |
|
|
Long-Acting Insulin
-primary use |
-Cats
-occasional dogs -Basal insulin |
|
|
Short acting insulins
|
-Regular insulin (human rDNA insulin)
-Insulin lispro (analogue insuling) |
|
|
Intermediate acting insulins
|
-NPH insulin*** dogs
-Humulin (human rDNA) -Vetsulin (porcine) dogs & cats |
|
|
Long acting insulins
|
-Glargine (analogue)
-Detemir (analogue) -ProZinc (human rDNA)*** Cats |
|
|
Insulin
-"U" |
-unit
-insulin conc. in units/mL |
|
|
U100 insulin
-insulins |
-all human insulins
-NPH -HumulinR -Lantus |
|
|
U40 insulin
-insulins |
-only vet products
-ProZinc -Vetsulin |
|
|
Converting factor for U100 to U40
|
U100 is 2.5x more concentrated than U40
|
|
|
Initial insulin dosing
-guidelines |
-0.25-0.5 units/kg
-same for dogs and cats -same for most at-home insulins -most insulins dosed BID |
|
|
Initial insulin dosing
-what is the usual dose range -why would you want to possibly start dosing at the lower end of the range |
-0.25-0.5 units/kg
Start at the lower end if: -concern of hypoglycemic -mild hyperglycemia -very thin patient |
|
|
Initial dose
-rare to start cats above what dose |
-3.0 units/dose
|
|
|
Changing insulin dose/type
-guidelines |
-think small & slow
-10-25% change with 1 week adjustment -Cat doses change by 0.5-1 U increments -switching from once to twice daily reduce AM dose by 25% -change type, start over with 0.5-1.0 U/kg |
|
|
Reason to alter diet in an animal with Diabetes Mellitus
|
-trouble regulating with insulin
|
|
|
Diabetes mellitus
-possible diet changes (reasons) |
-low fat (alleviate lipid abnormalities)
-high fiber (smooth glucose absorption) -high protein/low CHO (cat) |
|
|
Diabetes mellitus
-optimal dog feeding |
-2x/day on schedule
|
|
|
Diabetes mellitus
-optimal cat feeding |
-free choice feeding
-diet if obese |
|
|
Why is exercise important in diabetic animals?
|
-alteration of insulin needs
|
|
|
Diabetes mellitus
-how is monitoring clinical signs helpful/not helpful |
Helpful
-lacking clinical signs usually means serum glucose is below renal threshold (250 mg/dl) Not helpful -insensitive indicator of physiologic control |
|
|
Diabetes mellitus
-how is monitoring urine for glucose and ketones helpful/not helpful? |
Helpful
-parallels clinical signs -even controlled diabetics have glucosuria -sudden changes in glucose/ketones may indicate pre-clinical problems Not helpful -lacking glucosuria doesn't distinguish excellent diabetic control from hypoglycemia |
|
|
Diabetes mellitus
-how is monitoring serum glycated proteins helpful/not helpful? |
Helpful
-provide info when history not available -idea of avg. glucose over preceding 2 wks Now helpful -large "normal" range -affected by many variables |
|
|
Diabetes mellitus
-how is monitoring the glucose curve helpful/not helpful? |
Helpful
-can optimize insulin treatment -can be taught to clients to help provide superior results -good for detecting hypoglycemia Not helpful -hardly helpful especially in cats due to high level of day-to-day variability |
|
|
Diabetes mellitus
-alternative therapies occasionally used |
-acarbose
-sulfonylurea drugs -metformin -thiazolidinediones |
|
|
Acarbose
-function in DM treatment |
-inhibits glucosidase reducing intestinal starch absorption
|
|
|
Sulfonylurea drugs
-function in treatment of DM |
-enhances beta cell insulin release
-only Cats |
|
|
Metformin
-function in DM treatment |
-dec. hepatic glucose production
|
|
|
Diabetes mellitus
-new therapies |
-Incretin mimetics
-Dipeptidyl peptidase inhibitors |
|
|
Incretion mimetics
-function in DM treatment |
-hormone that is a GLP-1 agonist, boosting the effects of insulin
|
|
|
Dipeptidyl Peptidase Inhibitors
-function in DM treatment |
-enzyme inhibitor that decreases degredation of GLP-1
|

