![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
68 Cards in this Set
- Front
- Back
|
What are three types of vaginitis?
|
Trichomoniasis
Vulvovaginal Candidiasis (VVC) Bacterial Vaginosis (BV) |
|
|
This is a dynamic ecosystem that contains approximately 10 to the ninth powe bacterial colony-forming units.
|
The vagina
|
|
|
Normal vaginal discharge is?
|
clear to white, odorless, and of high viscosity.
|
|
|
Normal bacterial flora in the vagina is?
|
Normal bacterial flora is dominated by lactobacilli – other potential pathogens present.
|
|
|
The vagina is a what environment that prevents?
|
Acidic environment (pH 3.8-4.2) inhibits the overgrowth of bacteria
Some lactobacilli also produce H2O2, a potential microbicide |
|
|
Vaginitis is usually characterized by?
|
Vaginal discharge
Vulvar itching Irritation Odor |
|
|
What are the common types of vaginitis?
|
Trichomoniasis (15%-20%)
Bacterial vaginosis (40%-45%) Vulvovaginal candidiasis (20%-25%) |
|
|
What are other causes of vaginitis?
|
Mucopurulent cervicitis
Herpes simplex virus Atrophic vaginitis Allergic reactions Vulvar vestibulitis Foreign bodies |
|
|
How do you diagnose vaginitis?
|
Patient history
Visual inspection of internal/external genitalia Appearance of discharge Collection of specimen Preparation and examination of specimen slide |
|
|
Apart from the typical diagnostics, what are more specialized diagnostics for vaginitis?
|
DNA probes
Cultures Fem Examine Test Card™ PIP Activity Test Card™ |
|
|
The Fem Examine Test Card™ tests for?
|
card test for detection of pH and trimethylamine
|
|
|
The PIP Activity Test Card™ tests for?
|
detects enzyme breakdown from G. vaginalis
|
|
|
Symptom presentation Itch, discharge, 50% asymptomatic
Vaginal discharge Frothy, gray or yellow-green; malodorous Clinical findings Cervical petechiae “strawberry cervix” Vaginal pH > 4.5 KOH “whiff” test Often positive NaCl wet mount Motile flagellated protozoa, many WBCs |
Trichomoniasis
|
|
|
Symptom presentation Itch, discomfort, dysuria, thick discharge
Vaginal discharge Thick, clumpy, white “cottage cheese” Clinical findings Inflammation and erythema Vaginal pH Usually < 4.5 KOH “whiff” test Negative NaCl wet mount Few WBCs KOH wet mount Pseudohyphae or spores if non-albicans species |
Candidiasis
|
|
|
Symptom presentation Odor, discharge, itch
Vaginal discharge Homogenous, adherent, thin, milky white; malodorous “foul fishy” Vaginal pH > 4.5 KOH “whiff” test Positive NaCl wet mount Clue cells (> 20%), no/few WBCs |
Bacterial Vaginosis
|
|
|
Most common treatable STD
Estimated 7.4 million cases annually in the U.S. at a medical cost of $375 million Estimated prevalence: 2%-3% in the general female population 50%-60% in female prison inmates and commercial sex workers 18%-50% in females with vaginal complaints |
Trichomonas vaginalis
|
|
|
What are the risk factors for trichomonas vaginalis?
|
Multiple sexual partners
Lower socioeconomic status History of STDs Lack of condom use |
|
|
What is the transmission of trichomonas vaginalis?
|
Almost always sexually transmitted
T. vaginalis may persist for months to years in epithelial crypts and periglandular areas Transmission between female sex partners has been documented |
|
|
What is the microbiology behind trichomonas vaginalis?
|
Etiologic agent:
Trichomonas vaginalis - flagellated anaerobic protozoa Only protozoan that infects the genital tract |
|
|
Trichomonas vaginalis has a possible association with?
|
Pre-term rupture of membranes and pre-term delivery
Increased risk of HIV acquisition |
|
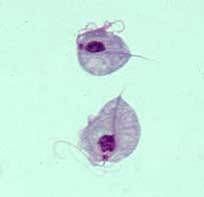
What is this?
|
Trichomonas vaginalis
|
|
|
What is the clinical presentation of trichomonas vaginalis in women?
|
May be asymptomatic in women
Vaginitis Frothy gray or yellow-green vaginal discharge Pruritus Cervical petechiae ("strawberry cervix") - classic presentation, occurs in minority of cases May also infect Skene's glands and urethra, where the organisms may not be susceptible to topical therapy |
|
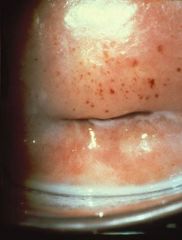
What is this and what is it associated with?
|
Strawberry cervix due to T. vaginalis
|
|
|
May cause up to 11%-13% of nongonococcal urethritis in males
Urethral trichomoniasis has been associated with increased shedding of HIV in HIV-infected men Frequently asymptomatic |
Trichomonas vaginalis in men
|
|
|
How do you diagnose T. vaginalis?
|
Motile trichomonads seen on saline wet mount
Vaginal pH >4.5 often present Positive amine test Culture is the “gold standard” DNA probes |
|
|
How do you diagnose T. vaginalis in men?
|
Male diagnosis - Culture
First void urine concentrated - at least an hour after not voiding Urethral swab |
|
|
This has limited sensitivity and low specificity for detecting T. vaginalis in women.
|
Pap smear
|
|
|
What is TX for T. Vaginalis?
|
CDC-recommended regimen
Metronidazole 2 g orally in a single dose CDC-recommended alternative regimen Metronidazole 500 mg twice a day for 7 days No follow-up necessary |
|
|
How do you TX T. Vaginalis in pregnant women?
|
CDC-recommended regimen
Metronidazole 2 g orally in a single dose No evidence of teratogenicity |
|
|
What do you do if there is TX failure in T. vaginalis?
|
If treatment failure occurs after 1 treatment attempt with both regimens, the patient should be retreated with metronidazole 2 g orally once a day for 3-5 days
Assure treatment of sex partners If repeated treatment failures occur, contact the Division of STD Prevention, CDC, for metronidazole-susceptibility testing 404-639-8363 www.cdc.gov/std |
|
|
What two things are important with patient partner management?
|
Sex partners should be treated
Patients should be instructed to avoid sex until they and their sex partners are cured (when therapy has been completed and patient and partner(s) are asymptomatic) |
|
|
What is involved with patient education and counseling in T. vaginalis?
|
Nature of the disease
May be symptomatic or asymptomatic, douching may worsen vaginal discharge, untreated trichomoniasis associated with adverse pregnancy outcomes Transmission issues Almost always sexually transmitted, fomite transmission rare, may persist for months to years, associated with increased susceptibility to HIV acquisition |
|
|
With risk reduction, the clinician should?
|
Assess patient’s potential for behavior change
Discuss individualized risk-reduction plans with the patient Discuss prevention strategies such as abstinence, monogamy, use of condoms, and limiting the number of sex partners Latex condoms, when used consistently and correctly, can reduce the risk of transmission of T. vaginalis |
|
|
Affects most females during lifetime
Most cases caused by C. albicans (85%-90%) Second most common cause of vaginitis Estimated cost: $1 billion annually in the U.S. |
Vulvovaginal Candidiasis (VVC)
|
|
|
These are normal flora of skin and vagina and are not considered to be sexually transmitted pathogens
|
Candida species
|
|
|
What is the microbiology of Candidiasis?
|
Candida species are normal flora of the skin and vagina
VVC is caused by overgrowth of C. albicans and other non-albicans species Yeast grows as oval budding yeast cells or as a chain of cells (pseudohyphae) Symptomatic clinical infection occurs with excessive growth of yeast Disruption of normal vaginal ecology or host immunity can predispose to vaginal yeast infections |
|
|
Vulvar pruritis is most common symptom
Thick, white, curdy vaginal discharge ("cottage cheese-like") Erythema, irritation, occasional erythematous "satellite" lesion - like a diaper rash External dysuria and dyspareunia |
Candidiasis
|
|
|
Candidiasis can be a sign of what underlying disease?
|
Diabetes
|
|
|
How do you diagnose candidiasis?
|
History, signs and symptoms
Visualization of pseudohyphae (mycelia) and/or budding yeast (conidia) on KOH or saline wet prep pH normal (4.0 to 4.5) If pH > 4.5, consider concurrent BV or trichomoniasis infection Cultures not useful for routine diagnosis |
|
|
Sporadic or infrequent vulvovaginal candidiasis
Or Mild-to-moderate vulvovaginal candidiasis Or Likely to be C. albicans Or Non-immunocompromised women |
Uncomplicated VVC (Vulvovaginal Candidiasis)
|
|
|
Recurrent vulvovaginal candidiasis (RVVC)
Or Severe vulvovaginal candidiasis Or Non-albicans candidiasis Or Women with uncontrolled diabetes, debilitation, or immunosuppression or those who are pregnant |
Complicated VVC (Vulvovaginal Candidiasis)
|
|
|
Mild to moderate signs and symptoms
Non-recurrent 75% of women have at least one episode Responds to short course regimen |
Uncomplicated VVC (Vulvovaginal Candidiasis)
|
|
|
What is CDC recommended TX for uncomplicated VVC vulvovaginal candidiasis?
|
Intravaginal agents:
Butoconazole 2% cream, 5 g intravaginally for 3 days† Butoconazole 2% sustained release cream, 5 g single intravaginally application Clotrimazole 1% cream 5 g intravaginally for 7-14 days† Clotrimazole 100 mg vaginal tablet for 7 days Clotrimazole 100 mg vaginal tablet, 2 tablets for 3 days Clotrimazole 500 mg vaginal tablet, 1 tablet in a single application Miconazole 2% cream 5 g intravaginally for 7 days† Miconazole 100 mg vaginal suppository, 1 suppository for 7 days† Miconazole 200 mg vaginal suppository, 1 suppository for 3 days† Nystatin 100,000-unit vaginal tablet, 1 tablet for 14 days Tioconazole 6.5% ointment 5 g intravaginally in a single application† Terconazole 0.4% cream 5 g intravaginally for 7 days Terconazole 0.8% cream 5 g intravaginally for 3 days Terconazole 80 mg vaginal suppository, 1 suppository for 3 days Oral agent: Fluconazole 150 mg oral tablet, 1 tablet in a single dose |
|
|
Recurrent (RVVC)
Four or more episodes in one year Severe Edema Excoriation/fissure formation Non-albicans candidiasis Compromised host Pregnancy |
COMPLICATED VVC
|
|
|
Complicated VVC: How do you treat
Recurrent VVC (RVVC)? |
7-14 days of topical therapy, or
150 mg oral dose of fluconozole repeated 3 days later Maintenance regimens (see CDC STD treatment guidelines) |
|
|
Complicated VVC: How do you treat Severe VVC?
|
7-14 days of topical therapy, or
150 mg oral dose of fluconozole repeated in 72 hours |
|
|
Complicated VVC: How do you TX non albicans?
|
Non-albicans
Optimal treatment unknown 7-14 days non-fluconozole therapy 600 mg boric acid in gelatin capsule vaginally once a day for 14 days |
|
|
Complicated VVC: How do you TX
Compromised host? |
7-14 days of topical therapy
|
|
|
How do you handle partner management with VVC?
|
VVC is not usually acquired through sexual intercourse.
Treatment of sex partners is not recommended but may be considered in women who have recurrent infection. A minority of male sex partners may have balanitis and may benefit from treatment with topical antifungal agents to relieve symptoms. |
|
|
What is involved with patient counseling and education regarding VVC?
|
Nature of the disease
Normal vs. abnormal vaginal discharge, signs and symptoms of candidiasis, maintain normal vaginal flora Transmission Issues Not sexually transmitted Risk reduction Avoid douching, avoid unnecessary antibiotic use, complete course of treatment |
|
|
Most common cause of vaginitis
Prevalence varies by population: 5%-25% among college students 12%-61% among STD patients Widely distributed Linked to premature rupture of membranes, premature delivery and low birth-weight delivery, acquisition of HIV, development of PID, and post-operative infections after gynecological procedures Organisms do not persist in the male urethra |
Bacterial Vaginosis (BV)
|
|
|
What are the risk factors for bacterial vaginitis?
|
African American
Two or more sex partners in previous six months/new sex partner Douching Absence of or decrease in lactobacilli Lack of H2O2-producing lactobacilli |
|
|
What is known about the transmission of bacterial vaginitis?
|
Currently not considered a sexually transmitted disease, but acquisition appears to be related to sexual activity
|
|
|
What is the microbiological basis of bacterial vaginitis?
|
Overgrowth of bacteria species normally present in vagina with anaerobic bacteria
BV correlates with a decrease or loss of protective lactobacilli |
|
|
Bacterial vaginitis correlates with a decrease or loss of?
|
protective lactobacilli
|
|
|
What is specifically associated with protective lactobacilli and its help in fighting off bacterial vaginitis?
|
Vaginal acid pH normally maintained by lactobacilli through metabolism of glucose/glycogen
Hydrogen peroxide (H2O2) is produced by some Lactobacilli,sp. H2O2 helps maintain a low pH, which inhibits bacteria overgrowth Loss of protective lactobacilli may lead to BV |
|
|
The following details correlate to what?
All lactobacilli produce lactic acid Some species also produce H2O2 H2O2 is a potent natural microbicide Present in 42%-74% of females Thought to be toxic to viruses like HIV |
H2O2 -PRODUCING LACTOBACILLI
|
|
|
50% asymptomatic
Signs/symptoms when present: 50% report malodorous (fishy smelling) vaginal discharge Reported more commonly after vaginal intercourse and after completion of menses |
Clinical presentation and symptoms of bacterial vaginitis
|
|
|
You obtain bacterial vaginitis diagnosis by using what?
|
AMSEL CRITERIA
|
|
|
Amsel Criteria:
Must have at least three of the following findings to diagnose bacterial vaginitis: |
Vaginal pH >4.5
Presence of >20% per HPF of "clue cells" on wet mount examination Positive amine or "whiff" test Homogeneous, non-viscous, milky-white discharge adherent to the vaginal walls |
|
|
Pregnant women with symptomatic bacterial vaginitis disease should be treated with?
|
Metronidazole 250 mg orally 3 times a day for 7 days, OR
Clindamycin 300 mg orally twice a day for 7 days |
|
|
TX for bacterial vaginitis, CDC-recommended regimens:
|
Metronidazole 500 mg orally twice a day for 7 days, OR
Metronidazole gel 0.75%, one full applicator (5 grams) intravaginally, once a day for 5 days, OR Clindamycin cream 2%, one full applicator (5 grams) intravaginally at bedtime for 7 days |
|
|
TX for bacterial vaginitis, Alternative regimens:
|
Metronidazole 2 g orally in a single dose, OR
Clindamycin 300 mg orally twice a day for 7 days, OR Clindamycin ovules 100 g intravaginally once at bedtime for 3 days |
|
|
Bacterial vaginitis Asymptomatic high-risk women (those who have previously delivered a premature infant) are handled how?
|
May be screened at first prenatal visit
Follow up 1 month after completion of therapy |
|
|
What are the four things to do in bacterial vaginitis screening and TX in asymptomatic patients?
|
Asymptomatic screening of low-risk pregnant women is not recommended.
Therapy is not recommended for male partners of women with BV. Female partners of women with BV should be examined and treated if BV is present. Screen and treat women prior to surgical abortion or hysterectomy. |
|
|
What is the recurrence of bacterial vaginitis?
|
20% recurrence rate after 1 month
Recurrence may be a result of persistence of BV-associated organisms and failure of lactobacillus flora to recolonize. Data do not support yogurt therapy or exogenous oral lactobacillus treatment. Under study: vaginal suppositories containing human lactobacillus strains |
|
|
Partner management in bacterial vaginitis.
|
After multiple occurrences, some consider empiric treatment of male sex partners to see if recurrence rate diminishes, but this approach has not been validated.
|
|
|
Three main things in patient counseling and education regarding bacterial vaginitis.
|
Nature of the Disease
Normal vs. abnormal discharge, malodor, BV signs and symptoms, sexually associated Transmission Issues Not sexually transmitted between heterosexuals, high association in female same-sex partnerships Risk Reduction Avoid douching Limit number of sex partners |

