![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
39 Cards in this Set
- Front
- Back
|
Transmisison routes for A. caninum
|
Infective L3 can be acquired by:
1. Skin penetration 2. Ingestion - food/water, arrasted larvae in paratenic hosts, lactogenic transmission (major source of infection of puppies) Transplacental route = unimportant |
|
|
Pathogenesis of Hookworms
|
Blood sucking activity
1. Attach to mucosa and pull a plug of intestinal mucosa into the buccal capsule 2. Use teeth to lacerate mucosa 3. Secrete proteolytic enzymes and anticoagulant 4. Change sites frequently so old sites continue to bleed Anemia develops 1. Initially normocytic, normochromic 2. Becomes microcytic, hypochromic with time |
|
|
Variable Clinical Signs of Canine Hookworm Disease
|
Severity depends upon:
1. Dosage 2. Age resistance, acquired immunity and premunition 3. Iron reserves (low in puppies) 4. Nutritional status 5. Other stress factors, infections |
|
|
Clinical Signs of Canine Hookworm Disease: Anemia
|
1. Pale mucous membranes
2. Decreased stamina, weakness 3. Melena or possible bloody feces 4. Unthrifty appearance (thin, rough hair coat) |
|
|
Clinical Syndromes of Canine Hookworm Disease
|
1. Peracute neonatal ancylostomiasis
2. Acute ancylostomiasis 3. Chronic (compensated) Ancylostomiasis 4. Secondary (decompensated) Ancylostomiasis |
|
|
Description of Peracute Neonatal Canine Ancylostomiasis
|
1. Result of lactogenic transmission from dam
2. Onset of signs a. Often appear healthy 1st week then crash 2nd week b. Signs can develop as early as 4 days of age c. Often fatal by 10-24 days of age even with treatment 3. Pups: extremely pale with blood in feces, +/- diarrhea; weak 4. NO eggs in feces (yet) 5. Necropsy findings = blood and immature worms in intestinal tract |
|
|
Description of Acute Canine Ancylostomiasis
|
1. Results from acquisition of large numbers of L3 over short period of time
a. Usually seen in older pups b. Pallor due to normocytic, normochromic anemia c. Melena d. Weakness e. Often die unless treated promptly f. STRONGYLE TYPE EGGS PRESENT IN FECES g. Adult worms and blood in SI at necropsy |
|
|
Description of Chronic (Compensated) Canine Ancylostomiasis
|
Common in mature dogs with low number of hookworms
Dogs asymptomatic unless stressed Feces are normal in appearance and have low to moderate numbers of strongyle type eggs |
|
|
Description of Secondary (Decompentsated) Canine Ancylostomiasis
|
Mature, usually malnourised dogs
a. Moderate number of worms + many eggs b. Microcytic, hypochromic anemia (pale, melena: may develop bloody diarrhea) c. Thin, rough hair coat, lethargic d. Can be fatal |
|
|
Treatment of Peracute Neonatal Canine Ancylostomiasis
|
Anthelmintic
Supportive care including blood transfusion, O2 Poor prognosis |
|
|
Treatment of Acute and Chronic Compensated Canine Ancylostomiasis
|
Anthelmintic
|
|
|
Treatment of Secondary Canine Ancylostomiasis
|
Anthelmintic plus nutritional support
|
|
|
Prevention and Control of Canine Ancylostomiasis for adults
|
1. Decrease number of L3 in environment
2. Identify and treat infected dogs 3. Sanitation: remove feces daily + cleaning 4. Impervious flooring 5. Kill larvae in environment |
|
|
Prevention and Control of Ancylostomiasis for puppies
|
1. Prevent transmammary transmission
2. Treat high risk puppies 3. |
|
|
Anthelmintics for Prevention of Canine Ancylostomiasis
|
1. Heartworm/hookworm
a. Ivermectin/pyrantel - Heartgard Plus for adults b. Milbemycin - Interceptor for adults + larvae |
|
|
Describe Ancylostoma tubaeforme
|
1. Fairly host specific for cats
2. Structure and life cycle similar to A. caninum = infection by skin penetration or ingestion and paratenic hosts with hypobiotic larvae |
|
|
Clincial Feline Ancylostomiasis
|
1. Uncommon
2. Clinical signs: weight loss, regenerative anemia 3. Heavy infection can be fatal 4. Diganosis a. Strongylid eggs in feces b. Cannot distinguis different Ancylostoma spp. eggs |
|
|
Describe Uncinaria stenocephala
|
1. More prevalent in northern US
2. Structure a. Adults with cutting plates instead of teeth 3. Lactogenic transmission important 4. No prenatal transmission |
|
|
Describe Bunostomum spp
|
1. Ruminant hookworms
a. B. phlebotomum in cattle b. B. trigonocephalum in sheep and goats 2. More prevalent in warmer climates 3. Survive best in warm and wet areas 4. Percutaneous infection most common |
|
|
Life cycle of Bunostomum
|
Adults in small intestine produce eggs and suck blood
Larvae develop in environment to infective L3 stage Infection by skin penetration or ingestion a. Enter blood and undergo "tracheal migration" to reach SI b. Prepaten period = 4-8 weeks |
|
|
Clinical signs of Bunostomum
|
Similar in all ruminant hosts: pruritus, alopecia of lower legs (L3 skin penetration)
Then progressive iron deficiency anemia --> hypoproteinemia --> dependent edema Anorexia, weight loss or poor growth, diarrhea: fetid, possibly with blood Infection can be severe-fatal (50 worms can cause severe anemia in a calf and 200-300 worms will kill a sheep) |
|
|
Treatment of Bunostomum
|
Most broad-spectrum anthelmintics effective
|
|

Identify
|
Ancylostoma caninum egg
|
|
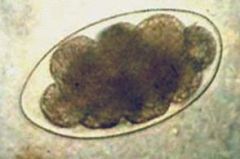
Identify.
|
Uncinaria stenocephala egg
|
|
|
Describe Order Strongylida - Superfamily Ancylostomatoidea
|
1. The hookworms
2. Hooked anterior end 3. Highly cuticularized buccal capsule 4. Equipped with teeth or cutting plates 5. Attach to host intestinal mucosa and suck blood 6. Bursate males |
|
|
Describe the basic hookworm life cycle
|
Direct:
1. Adults in small intestine of host 2. Egg to L3 in environment 3. Routes of infection = skin penetration and ingestion 4. Migrate through host to reach intestine 5. Larval arrest or HYPOBIOSIS can occur |
|
|
Define Hypobiosis
|
A state of arrested or delayed larval development in the host.
|
|
|
Hookworms of dogs and cats.
|
1. Ancylostoma caninum - common dog hookworm but rare in cats (most pathogenic species)
2. A. tubaeforme - common hookworm in cats 3. A. braziliense - both dogs and cats 4. Uncinaria stenocephala - mainly dogs |
|
|
Describe Ancylostoma caninum
|
1. Robust worms = 1/2 inch long; fresh worms are red or gray
2. Anterior end bent dorsally ("hooked") Large buccal capsule with mouth, 3 pairs teeth Usually firmly attached to mucosa of SI 3. Males - large copulatory bursa with long, thin, flexible spicules 4. Very common in dogs of all ages in MW 5. L3 survive best in moist, sandy-loam soils at moderate temperatures Do NOT survive freezing or temps greater than 37 degrees C |
|
|
Life cycle of A. caninum and Fate of L3
|
1. Adults in small intestine: females are oviparous
2. In environment: a. Within egg: morula --> L1 --> hatches from egg b. L1 develops and molts --> L2 develops (no molt) --> sheathed, infective L3 in environment Egg --> L3 takes 2-8 days 3. Pre-patent period ~ 16 days 4. L3 ingested or penetrate skin of new host a. If acquired by skin penetration undergo blood-lung migration i. Decision time 1. Undergo Tracheal migration (trachea - SI) 2. Undergo Somatic migration (muscles - hypobiotic) 3. Mucosal migration (gastric glands or SI mucosa) |
|
|
Definition of Premunition.
|
A state of resistance to infection which is established after an acute infection has become chronic and which persists as long as the infecting organisms remain in the body.
|
|
|
Hypobiotic larvae of A. caninum in a pregnant bitch
|
1. Larvae are "activated"
a. Occur in milk up to 20 days post-whelping b. Undergo LACTOGENIC TRANSMISSION to nursing pups c. Develop directly to adults in puppy SI |
|
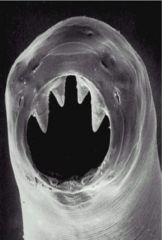
Identify
|
Order Strongylida - Family Ancylostomatoidea (Hookworm)
|
|
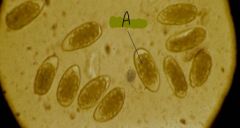
Identify
|
Strongyle-type eggs
|
|
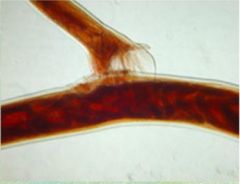
Identify.
|
Copulating hookworms: males have a copulatory bursa with bursal rays.
|
|
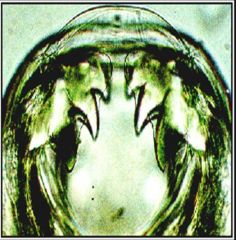
Identify.
|
Ancylostoma caninum because buccal cavity has 3 pairs of teeth.
|
|
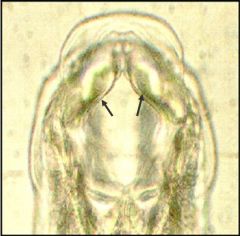
Identify.
|
Cutting plates of Uncinaria stenocephala
|
|
|
Describe cutaneous larva migrans
|
Hookworm L3 that penetrates human skin. It tries to complete the life cycle but is unable to penetrate deeper skin layers. Larval migration tunnels appear as ridges on skin.
|
|
|
Describe cutaneous larva migran lesions
|
1. Intensely pruritic
2. Persistent 3. Self-limiting 4. Second degree bacterial infection common 5. More severe and persistent if person hyper-sensitized by prior exposure |

