![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
50 Cards in this Set
- Front
- Back
|
growth fraction is...
|
cell proliferation/cell loss
|
|
|
What determines whether a tumor will have a fibrous capsule?
|
rate of growth. Slower growing malignant tumors and benign tumors generally have fibrous capsule.
|
|
|
Routes of metastases
|
direct seeding of body cavities - peritoneal implants of ovarian carcinoma
via lymphatics - carcinoma > sarcoma, follows pattern of lymph drainage via blood vessels carcinoma < sarcoma, follows pattern of venous drainage and frequently hits liver or lung because veins are easier to travel through |
|
|
Describe dominant/recessive in targets of genetic damage
|
protooncogenes are dominant
tumor suppressors are recessive apoptotic regulators can be either DNA repair are usually recessive Note: recessive genes can display dominance on pedigree. |
|
|
What is RAS?
|
It is an oncogenic g-protein. When the GTPase activity that inactivates the G protein dysfunctions and no longer occurs thereby constitutively stimulating cell division. Important for NF-1
|
|
|
What is ABL?
|
a gene important for Chronic Myelogenous Leukemia(CML)
a gene commonly mutated by 9:22 translocation that causes a hybrid gene to make a protein with a potent tyrosine kinase that sends growth promoting signals to nucleus |
|
|
What is Myc?
|
oncogene at nuclear transcription level. MYC protein binds DNA and activates transcription of growth related genes.
When Myc gene is translocated it gets overexpressed which causes overgrowth. |
|
|
Oncogenes at cell cycle level?
|
cyclin overexpression which allows easier traversal of checkpoints. CDKs can also be overexpressed to cause the same thing
|
|
|
What is the mechanism of RB?
|
It is a tumor suppressor gene that when dephosphorylated it binds to a transcription factor and inhibiting transcription(active). When it is phosphorylated, it releases E2F and allows it to promote transcription(inactive).
|
|
|
What is the mechanism of p53
|
p53 is a TSG.
p53 levels increase in response to DNA damage and induce p21 which encodes CDK inhibitor thereby halting G1 to S. P53 also induces GADD45 which is a DNA repair enzyme and if repair is successful MDM2 is expressed and degrades P53. If not, p53 engages apoptosis. Most common target for genetic aberrations in neoplasms. |
|
|
Apoptotic genes
|
frequently 3 letters starting with B.
BCL 2 is anti-apoptotic. Translocation from 18 to 14 causes overexpression which promotes cell proliferation. Pathway involves MYC and p53 genes. |
|
|
DNA repair genes
|
HNPCC is poster child for mismatch repair gene dysfunction and has genetic heterogeneity. Also one of the few autosomal dominant pre-cancerous conditions.
|
|
|
What does microsatellite instability indicate?
|
a dysfunction in a mismatch repair gene
|
|
|
Xeroderma Pigmentosum
|
Nucleotide Excision repair dysfunction that has genetic heterogeity.
|
|
|
Dysplasia encompasses what features...?
|
this is a characteristic of neoplasia.
pleomorphism(irregular cell shapes), nuclear abnormalities(high nuclear/cytoplasm ratio, nucleoli), mitotic figures, loss of polarity |
|
|
anaplasia
|
characteristic of neoplasia...
tumor giant cells and necrosis. severe form of dysplasia. |
|
|
What new characteristics can neoplastic cells attain?
|
neoantigens, oncofetal antigens, ectopic hormone production
|
|
|
Discuss tumor growth.
|
After 20 doublings, it is at 1 mg and needs new blood supply. At 30 doublings it is at 1 gram and is the limit of clinical detection. At 40 doublings, it is at 1 kg and you are dead.
|
|
|
Tumor growth generalization
|
malignant growth faster than benign growth. Poorly differentiated growth faster that well differentiated growth. Growth rate not constant and influences by many factors.
|
|
|
Development of sustained angiogenesis
|
needed at 1 mg or more. Balance of activators and inhibitors of angiogenesis. Vessels have abnormal pattern of growth and are leakier
|
|
|
Invasion
|
detach from neighbors, penetrate basement membrane and stimulate movement through membrane. Before penetration of basement membrane, it is called carcinoma in situ. After it is carcinoma.
|
|
|
Common metastatic sites
|
lymph node, liver, lung, bone, brain
uncommon: spleen, heart, striated muscle |
|
|
What translocation is in Burkitt lymphoma?
|
t(8:P14). This changes the regulatory mechanism for the MYC gene causing it to be overexpressed. (doesn't change actual protein like in CML)
|
|
|
What methods usually turn protooncogene to oncogene
|
translocation and gene amplification(homogenous staining regions or double minutes)
|
|
|
What are common mechanisms to inactivate TSG?
|
deletions and epigenetic changes.
Epigenetic changes are when you alter methylation of promotor sequences(not actual mutation) |
|
|
miRNAs and cancer
|
miRNAs do not code protein. primary mRNA is cleaved to make pre-mRNA where it interacts with a protein in cytoplasm called dicer that makes it into miRNA. miRNA interacts with RISC to silence a gene.
|
|
|
Chemical carcinogens
|
Initiators cause mutation. There are direct(carcinogens) and indirect(procarcinogens). Direct causes mutation, but indirect does not but your body turns it into something that does.
Promoters (cocarcinogens) simulate cell proliferation |
|
|
Carcinogenesis requires...
|
initiator and then a promoter
|
|
|
Ames test
|
tells you if a chemical is a mutagen(not carcinogen). Tests for both direct and indirect because it has added mammalian metabolic activating system(p450)
|
|
|
Ionizing radiation causes damage by....
|
NOT by affecting DNA. Rather it turns water into free radicals which then go on to damage DNA.
|
|
|
HPV mechanism of carcinogenesis
|
inhibits p53 function which inhibits growth arrest and apoptosis
|
|
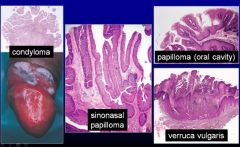
What causes this?
|
These are benign HPV neoplasms.
|
|
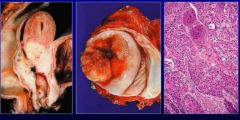
What are these?
|
These are uterine-cervix, recto-anal squamous cell carcinoma. These are malignant neoplasms of HPV.
Histologically there is the classic keratin pearls on the right. Reserved for well differentiated squamous cell carcinoma. |
|
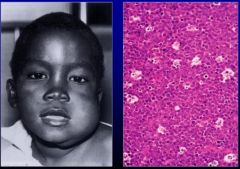
What is this a classic example of?
|
Burkitt Lymphoma(malignant neoplasm) caused by EBV. Note morphology is "starry sky". The sky is malignant lymphocytes. The stars are tingible body macrophages which is a macrophage that has apoptotic debris in cytoplasm.
|
|
|
What neoplasms associated with EBV?
|
Burkitt Lymphoma, B-cell lymphoma, hodgkin disease, nasopharyngeal carcinoma
|
|
|
What is the mechanism by which EBV causes cancer?
|
It enters via CD21, viral LMP-1 mimics CD-40 which stimulates proliferation/survival.
|
|
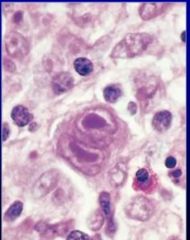
What is this?
|
A slide showing hodgkin disease you have a malignant cell called a reed-sternburg cell with very prominent nucleoli that is binucleated. This is a diagnostic cell for Hodkins disease usually caused by EBV. Sometimes can overlap with CMV.
|
|
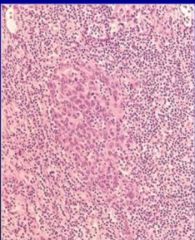
What is this?
|
Nasopharyngeal carcinoma caused by EBV. Note how cells are bigger in the middle? Those are cancer cells mixed with lymphocytes.
|
|
|
Hepatitis B Virus
|
Probably promotor effect for hepatocellular carcinoma through indirect effect(cell death, increased cell division).
|
|
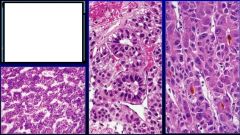
What is this caused by? What is it?
|
it is hepatocellular carcinoma.
caused by Hepatitis B Virus(DNA) or Hepatitis C Virus(RNA) |
|
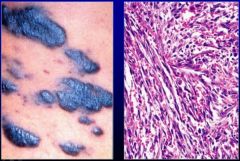
What is this? What causes it?
|
Kaposi Sarcoma. Unclear mechanism of cancer causing. Malignant cells defining slit like spaces containing red blood cells.
|
|
|
Human T-Cell leukemia Virus Type 1(HTLV-1)
|
RNA virus(retrovirus). likes CD4 positive T cells that causes leukemia/lymphoma 40-60 years AFTER infection most likely with a promotor effect.
|
|
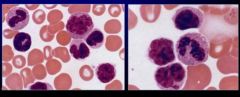
What is this caused by?
|
Human T-Cell leukemia Virus Type 1(HTLV-1)
|
|
|
Helicobacter pylori
|
gram negative bacillus that can cause gastric lymphoma/carcinoma via promotor effect.
|
|
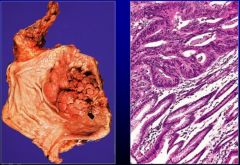
What is this caused by? WHat is it?
|
Helicobacter Pylori. It is Gastric Carcinoma.
|
|
|
Tumor immunity cells
|
NK cells, CTL, activated macrophages, B cells
|
|
|
Common neoplasms in immunocompromised patients
|
lymphoma(EBV), Kaposi Sarcoma(KSHV), uterine cervical carcinoma(HPV), gastric carcinoma(Helicobacter pylori)
|
|
|
breast cancer arises from....
|
adenocarcinoma arises from ductal glandular epithelium
|
|
|
Adenocarcinomas can generally be described as....
|
scirrhous
|
|
|
What is desmoplasia caused by in adenocarcinoma of the breast?
|
the cancer cells stimulating the surround stroma to produce collagen.
|

