![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
20 Cards in this Set
- Front
- Back
|
What are some characteristics of HSC (Hematopoietic Stem Cells)?
|
- capable of differentiating
- capable of self renewing (asymmetric replication) - mark for CD34+ (early progenitors) |
|
|
What is the difference between bone marrow and stem cell transplant?
What are 3 sources of HSC? |
Difference is WHERE the cells come from (BM- cells come from BM, SC- cells taken from peripheral blood).
Bone Marrow Peripheral Blood stem cells Umbilical cord cells |
|
|
Where is bone marrow harvested from?
What is the limitation to using umbilical cord blood? |
PSIC (Posterior superior iliac crest)
Umbilical cord blood is limited in number of cells (can only use what's in the cord) |
|
|
How do you prep someone for peripheral stem cell harvest?
How does "time to engraftment" compare to "degree of graft vs. host disease" |
Give them G-CSF--> take blood and plasmapherese to remove only CD34+ cells --> transplant to recipient
More days to engraft = typically less chronic graft vs. host disease (ex: cord blood = longest to engraft but has least GVHD). |
|
|
What is an Autologous transplant?
For what diseases is autologus transplant curative? for what diseases does it cause progression free survival? |
Autologous = patients given high dose chemo to remove bone marrow and use their own stem cells to repopulate.
Multiple Myeloma = progression free survival (but not cure) NHL, HD, Amyloidosis = Autologous transplant can be curative |
|
|
What is the major disadvantage to using Autologous transplant?
|
Concern for relapse (we are not sure if we are reinfusing patient with diseased marrow). However, low toxicity AND can lead to possible cure.
|
|
|
MHC Class I is found on what cells? What type of T cell is it targeted by?
MHC Class II is found on what cells? What type of T cell is it targeted by? |
MHC I --> expressed on almost all cells. Targeted by CD8.
MHC II --> on B-cells, Dendritic Cells, Monocytes. Targeted by CD4+. |
|
|
What is the difference between Full Allogeneic, Non-Myeloablative "mini" allogeneic, or Haplo allogeneic transplants?
|
Full allogeneic --> complete ablation of bone marrow
Mini --> chemo will not completely remove bone marrow, but rely on Graft vs. Leukemia to wipe out remaining leukemia. Haplo--> Use stem cells from a donor that's a half match (ex: parent). Immune reaction will hopefully put cancer cells into remission (but you're at increase risk of GVHD) |
|
|
How is HLA typing inherited? What is the chance of the identical HLA antigens as your sibling?
Does blood type need to be matched? |
HLA typing inherited by Mendelian Genetics (thus siblings have 1/4 chance of having identical HLA antigens).
Blood type does NOT need to be matched! |
|
|
Would a older patient be a better or worse donor? a better or worse recipient?
Why do men make better donors than women, in general? |
Older patient- higher risk as donor (more antigenic exposure), and as patient (higher risk of GVHD).
Men have less antigenic exposure (women have been pregnant!). |
|
|
What conditions are ideal for Allogeneic Bone Marrow Transplants?
|
AML, ALL, CML, CLL
Multiple Myeloma Sickle Cell, Thalassemia Myelodysplastic syndrome Aplastic Anemia (where BM has been completely wiped out) |
|
|
What is the major disadvantage of Allogeneic Transplant?
|
High mortality rate --> Graft vs. Host disease
There is a risk for graft rejection and you must have a match in order to undergo transplant |
|
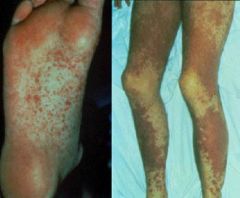
Describe the pathogenesis of how the condition above occurs (post-transplant).
What other body systems are affected |
Graft vs. Host disease- donor T-cells attack native organs on the recipient (recognizes them as foreign)
- Skin (rash) - Gut (diarrhea and gastric ulcerations) - Mouth ulcers - Eyes (sicca syndrome) |
|
|
In what type of transplant do we see Graft vs. Leukemia (GVL) effect?
|
Allogeneic transplant --> New T cells from donor will sruvey and attack malignant cell.
|
|
|
The staging of acute GVHD is based on what three findings?
What is "Acute GVHD" defined as? |
1) Area of skin damaged
2) volume of diarrhea 3) level of bilirubin Acute = <100 days post transplant Chronic = >100 days post transplant |
|
|
How do you treat GVHD?
What is the major difference between morbidities associated with Autologous transplant and morbidities associated with Allogeneic transplants? |
- Immunosuppression (Steroids - 1mg/kg prednisone).
- If that fails use others- cyclosporine, tacrolimus, etc. - Rituximab (unknown how it works) ONLY with Allogeneic do you get GvH and Acute Renal Failure / Veno-occlusive disease (much less sxs with Autologous transplant) |
|
|
What is it critical to workup on a patient undergoing Pre-transplant screening?
|
- HLA typing (if allogeneic)
- All organ system checks (Echo, EKG, PFTs) - Infectious Serologies (HIV, Hepatitis, CMV) - Detal screening |
|
|
What is the time course for a typical allogeneic transplant procedure?
|
7 days of conditioning (pts. get chemo to deplete BM counts)
Day 0: stem cells delivered from blood bags- monitor for anaphylaxis Day 1-28: monitor counts, on immunosuppresion (can get toxicity) |
|
|
What are complications of allogeneic grafting procedure?
What is Veno-occlusive disease? |
Immunosuppression: CMV, PCP, and VZV reactivation
Engraftment syndrome: From cytokine release after neutrophils engraft (fever, rash, pulmonary edema) VoD= inflammation/damage to hepatic sinusoids. Leads to clotting. Pts get weight gain, ascites, and increased bilirubin. |
|
|
When you think of lymphomas, should you recommend autologous or allogeneic transplant?
|
Autologous transplant 1st (if patient fails, then do allogeneic transplant).
|

