![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
67 Cards in this Set
- Front
- Back
|
Where in the lymph nodes are B-cells found?
|
Germinal follicles
|
|
|
Where in the body are T-cells found (2)?
|
1) Paracortex of lymph nodes
2) Thymus |
|
|
Where in the body are histiocytes found (2)?
|
1) Subcapsular sinus of lymph nodes
2) Skin |
|
|
What is another name for histiocytes?
|
Langerhans cells
|
|
|
At what age range is lymphadenopathy usually benign? Malignant?
|
Benign <30 y/o
Malignant >30 y/o |
|
|
What does painful lymphadenopathy usually indicate (2)?
|
1) Infection
2) Autoimmune disease |
|
|
What does painless lymphadenopathy usually indicate (2)?
|
1) Metastasis
2) Primary malignant lymphoma |
|
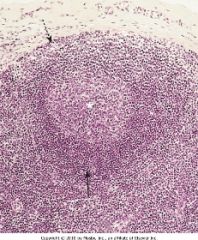
White asterisk: what region?
Solid arrow: what region? Dotted arrow: what region? |
White asterisk: germinal follicle
Solid arrow: paracortex Dotted arrow: subcapsular sinus |
|
|
Metastasis to left supraclavicular lymph node. From where (2)?
|
1) Stomach
2) Pancreatic carcinoma |
|
|
Metastasis to hilar lymph nodes. From where (1)?
|
1) Lung cancer
|
|
|
Metastasis to para-aortic lymph node. From where (1)?
|
1) Testicular cancer
|
|
|
Follicular hyperplasia. Histologic appearance?
|
Prominent germinal follicles
|
|
|
Dermatopathic lymphadenitis such as in psoriasis. Histological appearance.
|
Melanin pigmentation
|
|
|
Cat-scratch disease. Cause?
|
Bartonella henselae
|
|
|
Toxoplasmosis. Cause? Clinical features?
|
Toxoplasma gondii
Mononucleosis-like syndrome with painful cervical lymphadenopathy |
|
|
Tularemia. Cause? Reservoir? Clinical feature?
|
Francisella tularensis
Rabbits (zoonosis) Ulceroglandular lesions |
|
|
Sinus histiocytosis in axillary lymph nodes of breast cancer patient. Good or bad?
|
Good
|
|
|
Non-Hodkin's lymphoma. Cell of origin?
|
B-cell (>80%)
|
|
|
What extranodal sites may non-Hodgkin's lymphoma arise from (3)?
|
1) Stomach
2) CNS 3) Peyer's patch |
|
|
Are non-Hodgkin's lymphoma common in children and adults?
|
Most common malignant lymphoma in adults and children (~60%).
|
|
|
What types of non-Hodgkin's lymphoma may EBV cause (2)?
|
1) Burkitt's lymphoma
2) CNS lymphoma |
|
|
What type of non-Hodgkin's lymphoma may H. pylori cause (1)?
|
Malignant lymphoma of stomach
|
|
|
Which autoimmune disorders are associated with non-Hodgkin lymphoma (2)?
|
1) Sjogren's syndrome
2) Hashimoto's thyroiditis |
|
|
Mycosis fungoides. What cell type is involved? What tissue is involved?
|
CD4 Th cells
Skin |
|
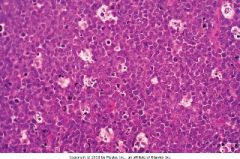
Lymph node section. What pattern is present? Diagnosis?
|
Starry sky pattern with reactive histiocytes.
Burkitt's lymphoma |
|
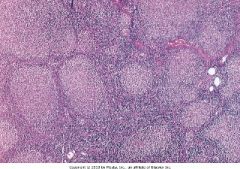
Diagnosis?
|
Follicular lymphoma
|
|
|
Sézary syndrome. What?
|
Mycosis fungoides in leukemic phase.
|
|
|
Nodular sclerosing Hodgkin Lymphoma. More common in men or women?
|
Women
|
|
|
What type of Hodgkin Lymphoma is EBV associated with?
|
Mixed cellularity type.
|
|
|
What is the classic neoplastic cell of Hodgkin Lymphoma? Immunophenotype?
|
Reed-sternberg cell. CD15+, CD30+
|
|
|
What is required for diagnosis of Hodgkin Lymphoma?
|
Reed-sternberg cell
|
|
|
What uncommon fever variant is associated with Hodgkin Lymphoma? Characteristics?
|
Pel-Ebstein fever. Recurring bouts of fever followed by remissions.
|
|
|
What is more important for the prognosis of Hodgkin Lymphoma, stage or type?
|
Stage
|
|
|
What lymph nodes are involved in nodular sclerosing Hodgkin Lymphoma (2).
|
1) Mediastinal nodes
2) Either cervical or supraclavicular nodes |
|
|
What secondary malignancies are patients with Hodgkin Lymphoma at increased risk for?
|
Acute myelogenous leukemia (AML) or non-Hodgkin lymphoma (NHL)
|
|
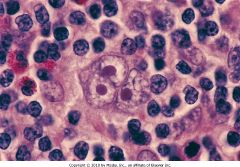
Diagnosis. (include type)
|
Mixed-cellularity Hodgkin Lymphoma.
Notes: Reed-Sternberg cells, eosinophils, plasma cells |
|
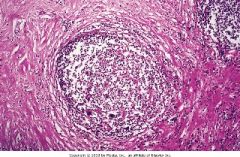
Diagnosis? (include type)
|
Nodular-sclerosing Hodgkin's lymphoma
|
|
|
Langerhans histiocytes. Distinguishing immunophenotype? Pathognomonic intracellular structure?
|
CD1+
Birbeck granules |
|
|
Malignant histiocytosis. What tissues commonly involved (2)?
|
1) Skin
2) Lytic bone lesions |
|
|
Hand-Schuller-Christian disease is a type of malignant histiocytosis. What is the classic triad?
|
1) Lytic skull lesions
2) Diabetes insipidus 3) Exophthalmos |
|
|
Eosinophilic granuloma. What? Clinical finding (1)?
|
Benign histiocytosis
Unifocal lytic lesions in bone |
|
|
Mast cell disease. Clinical signs and symptoms (3)?
|
1) Pruritis
2) Swelling 3) Hyperpigmentation |
|
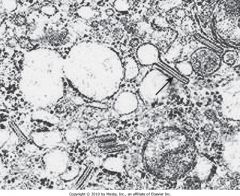
What cell is this? Why?
|
Histiocyte
Birbeck granules |
|
|
Urticaria pigmentosum. Clinical findings (2)?
|
1) Dermatographism
2) Regressed lesions remain hyperpigmented |
|
|
Histology of Urticaria Pigmentosum?
|
Mast cells containing metachromatic granules that stain positive with toluidine blue and Giemsa stain.
|
|
|
Plasma cell dyscrasia. Finding on serum protein electrophoresis?
|
Monoclonal spike, usually IgG.
|
|
|
Bence Jones protein. What?
|
Light chains (κ or λ) in urine.
|
|
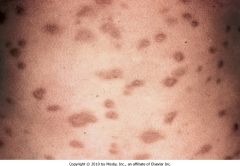
Biopsy revealed Giemsa positive cells. Diagnosis?
|
Urticaria Pigmentosum
|
|
|
What age group does multiple myeloma typically involve?
|
>40 y/o
|
|
|
What is the typical cellular progression of multiple myeloma?
|
Normal plasma cell → monoclonal gammopathy of undetermined significance (MGUS) → myeloma
|
|
|
Multiple myeloma. Classical bone findings (3)?
|
1) Lytic lesions
2) Pathologic fractures 3) Hypercalcemia |
|
|
Multiple myeloma. Classical renal findings include proteinaceous casts composed of what (2)?
|
1) Bence Jones protein
2) Intratubular multinucleated giant cell reaction |
|
|
Multiple myeloma. Common causes of death (2)?
|
1) Renal failure
2) Sepsis |
|
|
What is the most common monoclonal glomerulopathy?
|
MGUS
|
|
|
What cell type is present in the red pulp of the spleen (1)?
|
Macrophages
|
|
|
What cell types are present in the white pulp of the spleen (2)?
|
1) B-cells
2) T-cells |
|
|
What is the most common cause of splenomegaly in developing countries?
|
Malaria
|
|
|
Gaucher's disease. What is deficient and what is elevated?
|
↓ glucocerebrosidase
↑ glucocerebroside |
|
|
Niemann-Pick. What is deficient and what is elevated?
|
↓ sphingomyelinase
↑ sphingomyelin |
|
|
Massive splenomegaly. Common complications (4)?
|
1) LUQ pain
2) Splenic infarctions 3) Friction rub 4) Left-sided pleural effusion |
|
|
Splenomegaly in cirrhosis. Morphology?
|
Thickened "sugar-coated" spleen
|
|
|
Hypersplenism. Causes what?
|
Destruction of hematopoietic cells causing peripheral blood cytopenia.
|
|
|
Splenic dysfunction. Increased risk for what?
|
Streptococcus pneumoniae sepsis
|
|
|
Mechanisms for septicemia seen in splenic dysfunction (3)?
|
1) ↓ IgM
2) ↓ tuftsin (increases macrophage phagocytic receptors) 3) ↓ splenic macrophages |
|
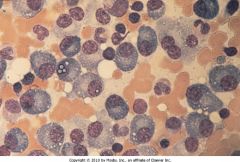
This patient presented with proteinaceous tubular casts and lytic bone lesions. What malignant cell types are shown in this slide?
|
Plasma cells.
|
|
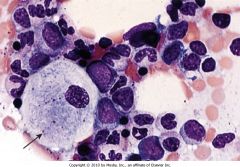
This patient presented with splenomegaly. This is a bone marrow biopsy. What is the diagnosis?
|
Gaucher's disease
Notes: macrophage with fibrillary appearnae of cytoplasm |
|
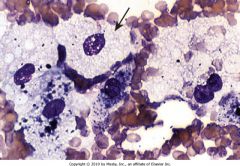
This patient presented with splenomegaly and a bone marrow biopsy was taken. What is the diagnosis?
|
Niemann-Pick Disease
Notes: Soap bubble appearance of macrophage cytoplasm. |

