![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
150 Cards in this Set
- Front
- Back
|
what is the accuracy of unenhanced CT to diagnose appendicitis |
94% |
|
|
what is the nl bowel wall thickness distended and contracted?
|
1-2 mm, 3-4 mm
|
|
|
at the GE junction the stomach may measure up to?
|
2 cm
|
|
|
benign pathologic small bowel thickening usually does not exceed what length?
|
1 cm
|
|
|
benign wall thickening is caused by?
|
ibd, ischemia,inramural hemorrhage
|
|
|
neoplastic wall thickening is caused by?
|
adenocarcinoma,lymphoma,leiomyosarcoma
|
|
|
when distended the wall of the esophagus should not exceed?
|
3 mm
|
|
|
what is the most common benign tumor of the esophagus?
|
leiomyoma
|
|
|
what are the 3 general causes of esophagitis?
|
gerd,radiation,infection
|
|
|
what is the main ct finding in esophagitis?
|
long segment of circumferential wall thickening >5mm
|
|
|
what is Boerhaave's Syndrome?
|
spontaneous rupture of the esophagus associated with violent vomiting
|
|
|
the gastric wall should not exceed ___ when distended?
|
5 mm
|
|
|
what is the best CT scan finding for gastritis
|
thickened gastric folds, MC in the antrum
|
|
|
what is Scirrhous Carcinoma (Linitis Plastica)
|
diffuse wall thickening with luminal narrowung seen in gastric carcinoma
|
|
|
What is the MC site for GI Lymphoma?
|
stomach NHL B-cell type
|
|
|
What is a Cajal Cell?
|
The common precursor cells for GIST (stromal tumors) arise
|
|
|
Where do most GIST arise from?
|
the Muscularis Propria in the stomach
|
|
|
What differentiates a GIST from a leiomyosarcoma?
|
presence of KIT CD117 protein- tyrosine kinase growth receptor factor
|
|
|
What are the 2 MC causes for gastric varices?
|
portal htn, spenic vein thrombosis
|
|
|
What is the hallmark finding for splenic vein thrombosis?
|
gastric varices without esophageal varicies
|
|
|
What are the anatomic ends of the duodenum?
|
pylorus and ligament of Treitz
|
|
|
What Ligament divides the right and left lobes of the liver?
|
Falciform
|
|
|
What vessels supply the liver?
|
portal vein 75%, Hepatic artery 25%
|
|
|
What medication stops peristalsis and dilates bowel wall?
|
Glucagon
|
|
|
Small bowel lumen and wall thickness should not exceed?
|
2.5 cm, 3 mm
|
|
|
Wall thickening greater than 1.5 cm is c/w?
|
mesenteric mass
|
|
|
What is visually different from THe jejunum compared to the ileum?
|
jejunal loops are feathery with distinct folds. ileum loops are featherless with thin walls
|
|
|
Where do Carcinoid tumors MC occur?
|
Appendix 50% and Small Bowel 20%
|
|
|
Intussusception is associated with what metastatic tunor to the bowel?
|
Melanoma, fibrosing CT characteristic
|
|
|
What is the hallmark finding in Crohn's Disease?
|
Circumferential thickening of the bowel wall maybe as thick as 3 cm. esp the terminal ileum
|
|
|
What is the Comb Sign?
|
produced by hyperemic thickening of the vasa recta is a sign of active disease
|
|
|
What is a paralytic ileus?
|
dilitationof proximal and distal small bowel without a transition zone.
|
|
|
What is a complete SBO?
|
dilitation of proximal small bowel with a distinct transition zone to collapsd distal bowel
|
|
|
What is a partial SBO?
|
falls between sbo and ileus. the proximal bowel is less dilated and the transition zone is less distinct
|
|
|
What causes most SBO?
|
adhesions
|
|
|
What is the MC malignancy seen in the Mesentery?
|
Lymphoma
|
|
|
The normal appendix does not exceed what dimension?
|
6 mm
|
|
|
What is Gardner's Syndrome?
|
AD assoc with multiple adenomatous polyps, osteomas,sebaceous cysts and desmoid tumors
|
|
|
Appendicoliths are seen in what percentage of pts with appendicitis?
|
28%
|
|
|
What is the name of the classification system for colon cancer?
|
Dukes
|
|
|
Where does colon ca metastisize to?
|
liver, lung, and adrenal
|
|
|
What %age of pts who have undergone bowel resection for ca will have recurrent disease?
|
70-80% within 2 years
|
|
|
Describe the difference in bowel wall thickening beween Crohns, UC, and Pseudomembranous colitis?
|
UC 7-8 mm
Crohns 10-20 mm Pseud. Colitis up to 30 mm |
|
|
What is Typhilitis?
|
infection of the cecum and ascending colon. classically in pts who have leukemia undergoing chemo
|
|
|
What are the MC areas of the colon affected by Ischemic Colitis?
|
watershed areas, splenic flecture and recto sigmoid
|
|
|
What are the CT hallmarks of Toxic Megacolon?
|
dilitation of the colon > 5 cm, thinning of wall, pneumatosis, and perforation
|
|
|
What are the 4 categories of Pneumatosis Intestinalis?
|
Bowel Necrosis, Mucosal Disruption, Increased mucosal permeability, and Pulmonary conditions
|
|
|
What is the MC type of volvulus?
|
Sigmoid
|
|
|
Where does the apex o the twisted bowel point to in Sigmoaid and Cecal Volvulus?
|
Sigmoid: LLQ
Cecal:RLQ |
|
|
What is a Cecal Bascule?
|
Folding of the Cecum rather than a twisting. it gets displaced into the central abdomen
|
|
|
What is the significance of the Marginal Artery of Drummond?
|
anastomoses the (IMA) with the (SMA). It is sometimes absent, as an anatomical variant.
|
|
|
What is the Median Arcuate Ligament Syndrome?
|
the ligament inserts low and thus crosses the proximal portion of the celiac axis, causing compression and sometimes resulting in abdominal pain usually in women worse during expiration
|
|
|
What is a Nutcracker Esophagus?
|
finding of increased pressures during peristalsis, diagnosis made when pressures exceed 180 mmHg; this has been likened to the pressure of a mechanical nutcracker
|
|
|
What does the CREST Syndrome stand for? What disease is it associated with?
|
Scleroderma ;
Calcinosis Raynaud's syndrome Esophageal dysmotility Sclerodactyly Telangiectasia |
|
|
What is Plummer Vinson Syndrome?
|
aka Paterson-Brown-Kelly syndrome or sideropenic dysphagia is a disorder linked to severe, long-term iron deficiency anemia, which causes (dysphagia) due to (esophageal webs)
|
|
|
What is the luminal diameter for Shatzki's ring and symptoms?
|
<12mm 100% symptomatic
13-20 mm 50% >20 assymptomatic |
|
|
How many sec does it take the food to traverse the esophagus?
|
8 to 10 sec
|
|
|
What is Passavant's Cushion?
|
A prominence on the posterior wall of the nasal pharynx formed by contraction of the superior constrictor of the pharynx during swallowing.
|
|
|
Name the 2 lateral Diverticulum?
|
Lateral and Killian-Jamieson
|
|
|
Where is a Zenkers Diverticulum always located?
|
posterior and superior or through the Cricopharyngeus muscle. never below
|
|
|
What is Rigler's Sign?
|
double wall sign, is seen on an x-ray of the abdomen when air is present on both sides of the intestine; a Rigler's sign is present when air is present on the inside (lumenal side) and the outside (peritoneal side
|
|
|
Caroli disease?
|
communicating, cavernous ectasia of the intrahepatic bile ducts
rare, autosomal recessive usually detected in childhood or early adulthood no cirrhosis or portal HTN predisposed to calculus formation recurrent cholangitis ==> liver abscesses ==> death increased risk of cholangiocarcinoma a/w medullary sponge kidney (renal tubular ectasia) in 80% |
|
|
primary sclerosing cholangitis?
|
idiopathic
a/w IBD (50%), usually UC M > F peak age 20-30 y/o chronic inflammation + fibrosis of all bile ducts stricture, obstruction, abscess ("string of beads") intramural pseudo-diverticula cholangioCa (10%!!) dilatation proximal to stricture may signal Ca DDx: cholangioCa (diffuse form) primary biliary cirrhosis (PBC) AIDS-related cholangitis (? d/t CMV) |
|
|
medullary sponge kidney?
|
"renal tubular ectasia"
dilatation & cyst formation of collecting tubules in renal pyramids Ca2+ ==> medullary nephrocalcinosis not hereditary; males (2:1) usually bilateral a/w renal tubular acidosis (RTA) Caroli disease parathyroid adenoma hypertrophic pyloric stenosis Ehlers-Danlos syndrome ipsilateral hemihypertrophy |
|
|
Gardner syndrome?
|
autosomal dominant
adenomas --> colon Ca (tx: colectomy) periampullary Ca soft-tissue lesions sebaceous cysts subQ fibromas, leiomyomas, lipomas bony lesions osteomas (esp. in sinuses) exostoses cortical thickening dental abnormalities (caries, extra teeth, odontomas) |
|
|
intussusception?
|
75% in kids <2 y/o
ileocolic (75%), ileo-ileocolic (15%) 90% idiopathic leading point: lymphoid tissue (possibly increased 2' to enteritis) in older kids + adults (ileo- or colocolic) Meckel diverticulum Peyer's patches lymphoma large mesenteric nodes duplications polyps "currant jelly" stools "coiled spring" on BE ** transient intussusception: a/w spruePseudokidney sign |
|
|
SPEN?
|
Solid and Papillary Endothelial Neoplasm
|
|
|
pancreas divisum?
|
unfused ducts of Wirsung and Santorini
incidence: 5-11% 21-45% get pancreatitis, possibly due to stenosis of the minor ampulla |
|
|
Boerhaave syndrome?
|
complete, transmural laceration of esophagus
etiology: spontaneous (retching, EtOH) 2' to endoscopy, trauma, vagotomy, FB sx: chest pain, shock, dyspnea, cyanosis grave prognosis M > F usually on LEFT uncommonly sub-diaphragmatic see also: esophageal trauma V sign of Naclerio |
|
|
V sign of Naclerio?
|
V-shaped collection of air
in mediastinum + along diaphragm indicates pneumomediastinum + pneumothorax seen in Boerhaave syndrome |
|
|
Mallory-Weiss syndrome?
|
mucosal gastric tear
only 10% are purely esophageal: most are at GE junction or proximal stomach M > F, associated with retching, EtOH massive hematemesis, abd pain Dx: endoscopy Rx: IA vasopressin |
|
|
Normal extrinsic impressions on the esophagus are made by what 3 structures?
|
Aorta
Left Mainstem Bronchus Left atrium |
|
|
Name the 3 compartments of pharynx and their anatomic landmarks
|
Nasopharynx: base of skull to soft palate
Oropharynx: Soft palate to the Hyoid bone Hypopharynx: Hyoid bone to the cricopharyngeus muscle |
|
|
At what level do you find the cricopharyngeus muscle?
|
C5-C6
|
|
|
Hamartomatous polyps accur in what syndrome? Are they malignant?
|
Peutz-Jeghers, no
|
|
|
Where is a Meckel's located?
|
antimesenteric border of the ileum, up to 2m from the ileocecal valve. 2 to 8 cm in length
|
|
|
What is the vascular hallmark of splenic vein thrombosis?
|
gastric varices without esophageal varices
|
|
|
What distinguishes GIST's from leiomyomas/sarcomas?
|
Tyroaine kinase growth factor (CD117)
|
|
|
desmoplastic (fibrotic) tumors
|
carcinoid of SB or colon
Hodgkin's lymphoma scirrhous gastric Ca |
|
|
What is the tx for GIST?
|
Imatinib (Gleevec), tyrosine kinase inhibitor
|
|
|
typhlitis
|
necrotizing inflammation of the colon in neutropenic patients
* cecum ("typhlon" in Greek) most frequent site * patients with leukemia, terminal lymphoma, aplastic anemia, cyclic neutropenia * symptoms: abdominal pain, diarrhea xray findings: * SBO * soft-tissue mass in right lower quadrant * thumbprinting due to bowel wall edema * intramural gas * bowel wall thickening ultrasound findings: * thickening of bowel mucosa * intraluminal fluid * pericecal fluid * abdominal abscess |
|
|
dromedary hump
|
extra mass of normal tissue found only on the lateral portion of the left kidney
* normal variant * "It's not a tumor." - Arnold Schwartzenegger in Kindergarten Cop |
|
|
Monckeberg's Medial Calcific Sclerosis
|
form of arteriosclerosis is characterized by calcific deposits in the media of small to medium-sized muscular arteries. Because the intima is not involved, the lumen is not compromised, and there is little clinical consequence to the pure form of this abnormality. However, some patients also have atherosclerosis affecting the same vessel.
|
|
|
GI-tract target lesion
|
* metastatic melanoma
* 1' neoplasm o spindle cell tumor (benign or malignant) o lymphoma o carcinoid o carcinoma * metastasis o breast Ca o lung Ca o renal Ca o Kaposi's sarcoma * eosinophilic granuloma * ectopic pancreas |
|
|
target lesions of liver/spleen
|
* lymphosarcoma (incl. Kaposi sarcoma)
* melanoma |
|
|
gastroschisis
|
Gastroschisis represents a herniation of abdominal contents through a paramedian full-thickness abdominal fusion defect. The abdominal herniation is usually to the right of the umbilical cord. No genetic association exists. A gastroschisis usually contains small bowel and has no surrounding membrane. The herniated bowel is not rotated and is devoid of secondary fixation to the posterior abdominal wall.
Gastroschisis usually is detected in the second trimester using antenatal sonography. The maternal serum alpha-fetoprotein (AFP) level is elevated in 77-100% of mothers. The mortality rate is approximately 17%. Surgical repair should be offered within the first day after delivery to avoid infection. The outcome is no different in infants delivered in tertiary obstetric centers than in infants delivered in smaller peripheral hospitals, although delivery within easy access of a neonatal surgical unit is advised. Cesarean delivery is performed in many mothers of fetuses with gastroschisis, although this does not convey any advantage over vaginal delivery. |
|
|
Omphalocele
|
mphalocele is an anterior abdominal wall defect at the base of the umbilical cord, with herniation of the abdominal contents. The herniated organs are covered by the parietal peritoneum. After 10 weeks' gestation the amnion and Wharton jelly also cover the herniated mass.
Omphaloceles are associated with other anomalies in more than 70% of the cases. Most associated anomalies are chromosomal. The anomaly is detected during routine ultrasonographic examination of the fetus or during an investigation of an increased alpha-fetoprotein (AFP) level. |
|
|
asplenia / polysplenia syndromes
|
probably different degrees of the same disorder
* asplenia (Ivemark syndrome, bilateral right sidedness) o more severe o right lung lobar anatomy bilaterally, bilateral eparterial bronchi o associated with cardiac, GI/GU and situs anomalies + TAPVR(~100%),ECD(85%)and many others o Howell-Jolly bodies - RBC inclusions * polysplenia (bilateral left-sidedness) o left lung lobar anatomy bilaterally, bilateral hyparterial bronchi o multiple spleens/splenules o bilateral SVCs, azygos continuation of IVC o associated with cardiac(less common than in asplenia), GI/GU and situs anomalies |
|
|
adenomyomatosis of gallbladder
|
type of hyperplastic cholecystosis
* increase in number and height of mucosal folds * secondary to hyperplasia of mucosal and muscular elements * Rokitansky-Aschoff sinuses (intramural diverticula) * 5% of all cholecystecomies * > 35 years; M:F = 1:3 associated with: * gallstones in 25-75% * cholesterolosis in 33% findings: * "comet-tail" artifact seen by US - cholesterol crystals in RA sinses * may have smooth sessile fundal mass in GB * may have an "hourglass" configuration with transverse septum * "pearl necklace gallbladder" on OCG |
|
|
Rokitansky-Aschoff sinuses
|
small outpouchings of gallbladder mucosa that extend through the muscularis layer
* may be congenital * a/w adenomyomatosis of gallbladder |
|
|
most common cause of mechanical SBO in patients who have had previous abdominal surgery
|
Adhesions
|
|
|
carcinoid syndrome
|
vasodilation 2' to serotonin elaboration
bronchial carcinoid SB carcinoid indicates liver mets (liver would otherwise break down serotonin secreted by 1' lesion) |
|
|
carcinoid tumor
|
"rule of one-third"
1/3 of GI carcinoid in SB 1/3 ==> mets 1/3 have 2nd malignancy 1/3 multiple 90% from distal ileum or appendix 90% of appendicial tumors desmoplastic reaction ==> kinking + angulation of SB angio: intensely vascular lesions arise from seratonin producing intraepithelial endocrine cells, namely the Kulchitsky’s cells of the crypts of Lieberkuhn |
|
|
What %age of pts with carcinoid tumor have carcinoid syndrome?
|
10%, if the syndrome is occuring there must be mets to the liver
|
|
|
Hypertrophic Pyloric Stenosis
|
Not usually seen until 3 weeks
projectile vomiting olive sign tx:pyloromyotomy wall > 3mm elongated >18 mm |
|
|
liver tumors are primarily supplied by which vessel?
|
hepatic artery
|
|
|
The liver gets it's primary blood supply from?
|
Portal Vein
|
|
|
retroperitoneal liposarcoma
|
most common primary retroperitoneal tumor
rarely arises from lipoma 95% of all fatty retroperitoneal tumors 40-60 years; M>F most radiosensitive sarcoma (32% 5-year survival) findings CT contrast enhancement mixed density (fat and soft tissue elements) pseudocystic pattern: water density secondary to volume averaging angio: hypovascular; no vessel dilation, capillary staining, laking sites for liposarcoma: lower extremity 45% abdominal cavity and retroperitoneum 14% trunk 14% upper extremity 8% head and neck 7% |
|
|
What vessel primarily supplies liver tumors?
|
Hepatic Artery
|
|
|
diaphragmatic eventration
|
upward displacement of abdominal contents secondary to a congenitally thin hypoplastic diaphragm
* location: o anteromedial on right o total involvement on the left o R:L = 5:1 * findings: o small diaphragmatic excursions o often lobulated contour see: elevated hemidiaphragm |
|
|
elevated hemidiaphragm
|
* phrenic nerve paralysis: invasive Ca, trauma, aneurysm
* idiopathic: right-sided in males, poss. viral * subphrenic disease: abscess, peritonitis; pancreas, GB * neurological disease: polio, peripheral neuritis, zoster * splinting: chest wall injury * myotonia congenita * pulmonary infarct * eventration * gaseous distension of stomach or colon * DDxChest fluoro may be helpful to rule out paralysis. * Basal ("subpulmonic") effusion may mimic elevation. |
|
|
What %age of gallstones are radiopaque?
|
15%
|
|
|
peliosis hepatis
|
* benign, intrahepatic vascular disorder
o a/w benign + malignant liver tumors o possible vasodilatory response to sex hormones o (?) clinical significance * multiple endothelium-lined, blood-filled spaces * communicate with sinusoids * angio (parenchymal phase): o multiple round collections of contrast in liver (3 - 15 mm) * DDx: o focal nodular hyperplasia o hypervascular mets o cavernous hemangiomata |
|
|
3 normal extrinsic impressins on the esophagus
|
aortic arch
left main bronchus left atrium |
|
|
intussusception adults vs peds
|
adults ileal-ileal
peds ileal-colic |
|
|
Most frequent congenital anomaly of GI tract
|
Meckel Diverticulum
|
|
|
Treatment of midgut volvulus
|
Ladd procedure: Reduction of volvulus, division of mesenteric bands, placement of small bowel on right and large bowel on left and appendectomy.
|
|
|
"Moulage sign"
|
(cast) characteristic of sprue
|
|
|
Reversal of jejunoileal fold pattern
|
sprue
|
|
|
Thickened proximal small bowel folds with micronodularity (1-2 mm) & low density mesenteric adenopathy (near fat HU)
|
whipple's
|
|
|
buzz words for ulcerative colitis
|
lead pipe colon
collar button ulcers toxic megacolon backwash ilietis sclerosing cholangits |
|
|
buzz words for crohns
|
cobblestones
pseudosacculations apthous ulcers string sign creeping fat comb sign |
|
|
Treatment of Ulcerative colitis
|
Medical
Sulfasalazine, steroids, azathioprine Methotrexate, LTB4 inhibitors Surgical: Total or proctocolectomy, Brooke or continent ileostomy (Kock pouch) |
|
|
Treatment of Crohn's
|
Mucosal biopsy to diagnose
Medical Steroids, azathioprine, mesalamine Metronidazole, antibody treatment Surgical Resection of diseased bowel Strictureplasty, primary fistulotomy |
|
|
Extensive ahaustral colonic dilatation, air-fluid levels, mucosal islands or pseudopolyps
|
Toxic Megacolon
|
|
|
"Accordion sign":
|
Trapped enteric contrast between thickened colonic haustral folds. a/w pseudomembranous colitis
|
|
|
Treatment of pseudomembranous colitis
|
Mild cases: Discontinue offending antibiotic therapy
Severe cases Metronidazole (drug of choice) or oral vancomycin Fulminant & toxic megacolon: Colectomy |
|
|
Pneumatosis, mesenteric venous gas, symmetric bowel wall thickening or thumbprinting on CT
|
ischemic colitis
|
|
|
Watershed segments of colon
|
Splenic flexure: Junction of superior mesenteric artery (SMA) & inferior mesenteric artery (IMA) (Griffith point)
Rectosigmoid: Junction of IMA & hypogastric artery (Sudeck point) Left colon: Typical in elderly with decreased perfusion Right colon: Young patients due to decreased collateral blood supply; chronic renal failure patients |
|
|
cecal vs sigmoid volvulus
|
cecal points toward luq
sigmoid points toward ruq |
|
|
Treatment of cecal volvulus
|
Colonoscopy to reduce volvulus
Complicated cases: Surgery (cecopexy, cecostomy, resection) |
|
|
Treatment of sigmoid volvulus
|
Nonoperative
Proctoscopic/colonoscopic decompression of obstruction ± stabilization via rectal tube insertion 70-80% success rate Nonoperative + operative Decompression, mechanical cleansing & elective sigmoid resection Complicated cases Surgical emergency Follow-up Water-soluble contrast enema to rule out underlying colon cancer |
|
|
Congenital, multifocal, segmental, saccular dilatation of intrahepatic bile ducts.
Communicating cavernous biliary ectasia |
Caroli disease:
|
|
|
caroli's disease vs syndrome
|
syndrome includes hepatic fibrosis
|
|
|
"Central dot" sign:
|
Strong, enhancing, tiny dots (portal radicles) within dilated intrahepatic bile ducts on CECT.
seen in caroli's dz |
|
|
2 types of hyperplastic cholecystosis
|
Adenomyomatosis
Cholesterolosis |
|
|
Adenomyomatosis vs cholesterolosis
|
Adenomyomatosis: Fundal, diffuse or mid-body GB wall thickening with intramural high amplitude echoes & "comet tail" reverberation artifacts
Cholesterolosis: Multiple GB polyps CECT: Thickened GB wall (segmental or diffuse); often brisk enhancement of wall post-contrast; cystic nonenhancing spaces within GB wall corresponding to intramural diverticula |
|
|
DDX Fibrolamellar Carcinoma
|
conventional HCC, intrahepatic cholangiocarcinoma,
focal nodular hyperplasia (FNH), hepatocellular adenoma, cavernous hemangioma. |
|
|
what is a normal gastric band phi angle
|
A normal gastric band should have a phi angle (angle between the spinal column and the gastric band) of 4°-58°.
|
|
|
what are some complications to gastric banding?
|
gastric banding is associated with complications; the most common of which include band misplacement, band slippage, band herniation, perforation, pouch dilation, and erosion of the gastric wall.
|
|
|
what is the normal position of a gastric band in relationship to the diaphragm and what is a phi angle?
|
The gastric band should be 4–5 cm below the diaphragm with a phi angle of 4°–58°.
|
|
|
what should the stoma size be in gastric banding?
|
The stoma should be 3–4 mm in diameter.
|
|
|
Risk factors for the development of cholangiocarcinoma include?
|
clonorchiasis, primary sclerosing cholangitis, Caroli disease, intrahepatic stone disease, chronic liver disease/cirrhosis, Thorotrast exposure, and choledochal cysts.
|
|
|
What are the classic findings of gallstone ileus? What is the triad
|
Classic findings of gallstone ileus are pneumobilia, small bowel obstruction, and ectopic gallstone (Rigler triad).
|
|
|
mcc well-circumscribed heterogeneously enhancing mass arising from the abdominal wall.
|
Solitary fibrous tumor
|
|
|
paragangliomas in which locations are a/w parasympathetic or sympathetic system?
|
Paraganglia associated with the parasympathetic system are located in the head, neck, and anterior mediastinum. Paraganglia associated with the sympathetic system are located in the posterior mediastinum and retroperitoneum.
|
|
|
paragangliomas are a/w which diseases?
|
Paragangliomas can be sporadic or hereditary in association with multiple endocrine neoplasia type 2 A and B, tuberous sclerosis, neurofibromatosis, von Hippel-Lindau, and Carney’s triad.
|
|
|
What is Carneys triad?
|
Carney’s triad (malignant gastrointestinal stromal tumors, pulmonary chondroma, and extra-adrenal paragangliomas).
|
|
|
What make up the portal triad
|
portal vein
hepatic artery bile duct |
|
|
DDX Periportal Edema
|
Systemic hypervolemia or overhydration
Passive hepatic congestion Acute hepatitis Hepatic trauma Dilated intrahepatic ducts (Imaging findings can mimic periportal edema.) |
|
|
DDX Calcified splenic nodules
|
sarcoid,
histoplasmosis, tuberculosis, disseminated pneumocystis carinii infection. Clinical history can help narrow the differential diagnosis. Other findings of portal hypertension such as portosystemic collateral vessels favor GGB, Gamma Ganda Bodies |
|
|
mc congenital abnormality of the gi tract |
meckel's diverticulum
|
|
|
classic findings of Gardner syndrome
|
Colonic adenomatous polyps,
extracolonic adenomatosis, osteomas, and desmoid tumors |
|
|
MC liver tumor
|
hemangioma |
|
|
Fat-containing FNHs may demonstrate unusual features such as
|
larger size, |
|
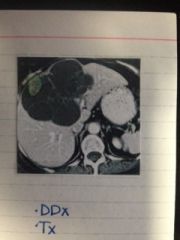
|
cystic mass with internal septations |
|
|
What is Blind Loop Syndrome? |
Blind-loop syndrome, a complication of small-bowel diverticulosis, occurs when food and waste are trapped within the diverticula, which promotes an overgrowth of bacteria that leads to malabsorption and diversion of nutrients to the bacteria. Patients often present with enteritis symptoms along with steatorrhea, malnutrition, anemia, and weight loss. |
|
|
Most adrenocortical carcinomas are functional, what hormone do they secrete? |
Cortisol |
|
|
The most specific findings for adrenal malignancy are? |
Irregular margins. Thick enhancing rim? |
|
|
What are the histological subtypes of an appendiceal Mucocele? |
four main histologic subtypes: retention cyst, mucosal hyperplasia, cystadenoma, or cystadenocarcinoma. The former two classifications are nonneoplastic entities with the latter representing neoplastic mucin-secreting tumors. The diagnosis in this case of “low-grade mucinous neoplasm” is an entity between cystadenoma and cystadenocarcinoma in which cells have penetrated the appendiceal wall. Low-grade mucinous neoplasms have the highest risk of developing into pseudomyxoma peritonei. |

