![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
85 Cards in this Set
- Front
- Back
|
Calcium fractions in serum/plasma
|
-fCa2+ (free Calcium)
-Ca2+/Pr- (Protein Bound Calcium) -Ca2+/A- (Calcium bound to Ions other than proteins) |
|
|
What regulates each calcium fraction in the blood?
|
-fCa2+ = hormones
-Ca2+/Pr- = protein conc. -Ca2+/A- = anion conc. |
|
|
What is filterable Ca2+?
|
=fCa2+ + Ca2+/A-
-protein bound calcium should not pass through glomeruli |
|
|
Vitamin D Production
-describe process |
-hepatocytes or diet provide cholesterol which is converted by sunlight to cholecalciferol (Vit. D3)
-Cholecalciferol can also be provided by the consumption of plants -Cholecalciferol moves to hepatocytes where hydroxylase converts it to 25-HCCC (calcidiol) -25-HCC circulates in the blood and eventully passes through the glomerular filtration barrier -25-HCC is converted to calcitriol by hydroxylase in renal tubular cells |
|
|
Which is more active calcidiol or calcitriol?
|
-calcitriol by 25x
|
|
|
Animal that cannot form calcitriol in its kidneys?
|
-horse
-lacks 1a-hydroxylase |
|
|
PTH production in the parathyroid glands
-stimulated by |
-dec. [fCa2+]
-dec. [1,25-DHCC] (calcitriol) |
|
|
Activity of 1a-hydroxylase in the kidneys
-promoted by -inhibited by |
Promoted by:
-dec. [fCa2+] -inc. PTH Inhibited by: -inc [fCa2+] -inc. [PO4] |
|
|
Calcium mobilization from bone
-promoted by |
-inc. PTH
-inc. [1,25-DHCC] |
|
|
Calcium absorption in intestine
-promoted by |
-inc. PTH
-inc. [1,25-DHCC] |
|
|
Urinary excretion of calcium
-enhanced by -reduced by |
enhanced by:
-inc [fCa2+] reduced by: -dec. [fCa2+] -inc. PTH -inc 1,25-DHCC |
|
|
What processes increase [fCa2+]?
|
-inc. mobilization of Ca2+ from bone
-inc. absorption of Ca2+ by intestine -dec. excretion of Ca2+ by kidneys |
|
|
How is regulation of [fCa2+] different in horses?
|
-no production of 1,25-DHCC in the kidneys
-absorption of dietary calcium from the intestine is not tightly regulated -excess dietary Ca2+ is excreted by the kidneys |
|
|
What does a change in [tCa2+] represent?
|
-change in one or more of the calcium fraction concentrations
|
|
|
Samples that can be used for measuring fCa2+
|
-serum
-heparinized blood -heparinized plasma -DO NOT USE EDTA or Citrate!!! |
|
|
Hypercalcemia
-causes |
-primary hyperparathyroidism
-Humoral hypercalcemia of malignancy (HHM) -Hypervitaminosis D -dec. Urinary excretion |
|
|
Primary hyperparathyroidism
-caused by |
-parathyroid adenoma or adenocarcinoma
|
|
|
Primary hyperparathyroidism
-pathogenesis to hypercalcemia |
-inc. production of PTH
-inc. [PTH] --inc. mobilization of Ca from bone --inc. absorption of Ca from intestine --dec. renal secretion of Ca ---increases [fCa2+] ----inc. [tCa2+] |
|
|
Humoral Hypercalcemia of Malignancy
-aka -causes |
-aka: pseudohyperparathyroidism
causes: -Neoplasms (canine lymphoma, apocrine gland carcinoma) -PTH-rp |
|
|
HHM
-pathogenesis to hypercalcemia |
-Neoplastic cells
-inc. production and release of PTH-rp --inc. [PTH-rp] ---inc. mobilization of Ca from bone ---inc. absorption of Ca from intestine ---dec. renal secretion of Ca ----inc. [fCa2+] -----inc. [tCa2+] |
|
|
Hypervitaminosis D
-causes |
-rodenticides with cholecalciferol
-granulomatous inflammation (relatively uncommon) |
|
|
Hypervitaminosis D
-pathogenesis to hypercalcemia |
-Excess Vit. D intake/production
--inc. [1,25-DHCC] ---inc. mobilization of Ca from bone ---inc. absorption of Ca from intestine ---dec. renal secretion of Ca ----inc. [fCa2+] -----inc. [tCa2+] |
|
|
Decreased Urinary Excretion of Ca2+
-causes |
-Equine renal failure
-Canine renal failure -Canine Addison's Disease |
|
|
Equine renal failure
-pathogenesis to hypercalcemia |
Renal disease destroys most equine nephrons
-dec. GFR --dec. clearance of Ca & Ca/A- ---inc. [fCa2+] & [Ca2+/A-] ----increase [tCa2+] dietary calcium excess is normally excreted by horse kidneys |
|
|
Canine Renal Failure
-pathogenesis to hypercalcemia |
Renal disease destroys most of the nephrons
-dec. GFR --dec. clearance of A- (PO4, SO4, citrate) ---increased formation of Ca2+/A- complexes in plasma & complexes are not cleared ----inc. [Ca2+/A-] -----inc. [tCa2+] |
|
|
Canine Addison's Disease (hypoadrenocorticism)
-pathogenesis to hypercalcemia |
Hypoadrenocorticism --> hypovolemia
-inc. activation of RAS --inc. angiotensin ---inc. proximal tubular reabsorption of Na+ and Ca2+ ----inc. [fCa2+] -----inc. [tCa2+] |
|
|
Hypocalcemia
-causes |
-Hypoalbuminemia
-Primary hypoparathyroidism -Hypovitaminosis D -inc. urinary excretion -Pregnancy, Parturient, Lactational |
|
|
Primary hypoparathyroidism
-causes |
Parathyroid gland destruction
-surgery -others (uncommon) |
|
|
Primary hypoparathyroidism
-pathogenesis to hypocalcemia |
-dec. production & release of PTH
-dec. [PTH] ---dec.mobilization of Ca from bone ---dec. absorption of Ca from intestine ---inc. renal secretion of Ca ----dec. [fCa2+] -----dec. [tCa2+] |
|
|
Disorder seen with a decrease in Vitamin D, Phosphate, or Calcium
|
-Rickets
|
|
|
Hypovitaminosis D
-causes |
-chronic renal disease --> secondary renal hyperparathyroidism
-Pseudohypovitaminosis D (vitamin D dependent Rickets) -dietary deficiency |
|
|
Chronic renal disease leading to hypovitaminosis D is most commonly seen in:
|
-dogs
-cats -cattle |
|
|
Pseudohypovitaminosis D
-Types |
-Type 1: defect in 1a-hydroxylase gene --> dec. Calcitriol formation
-Type 2: defect in the vitamin D receptor gene --> dec. cell response to calcitriol |
|
|
Describe how chronic renal disease causes secondary renal hyperparathyroidism
|
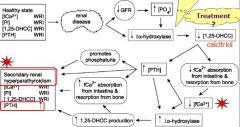
|
|
|
Effects noted with secondary renal hyperparathyroidism
|
-inc. [PTH]
-dec. WRI [tCa2+] -inc. WRI [Pi] -possible azotemia |
|
|
Hypocalcemia due to Pregnancy, Parturition, or Lactation
-aka |
-milk fever
-puerperal tetany |
|
|
Pregnancy, Parturition, Lactation
-pathogenesis to hypocalcemia |
-Parturition --> lactation
--Rapid inc. in Ca loss in milk ---not mobilizing Ca from bones fast enough ----dec. [fCa2+] -----dec. [tCa2+] |
|
|
Inc. urinary excretion of calcium
-causes |
-inc. urinary excretion of anions
-Furosemide (Lasix) treatment |
|
|
Increased urinary excretion of anions
-pathogenesis to hypocalcemia |
-Inc. anion loss in urine (AcAc, lactate, HCO3-)
--obligate loss of cations in urine (Ca, Na, K) ---hypocalcemia |
|
|
Furosemide Treatment
-pathogenesis to hypocalcemia |
-Inhibition of Cl- resorption in the ascending loop of henle
--reduced electrical gradient for Ca2+ resorption ---hypocalcemia |
|
|
Describe how inc. PO4 results in hypocalcemia
|
-PO4/Ca2+ complexes form and are engulfed by macrophages --> dec. PO4 and Ca2+ conc.
-tissue becomes calcified after damage by primary disease |
|
|
[fCa2+]
-regulated by |
-body
|
|
|
[fCa2+] sample collection
-preferred sample -tubes used |
-serum (anaerobic)
-red top |
|
|
Why is handling of a sample for fCa2+ critical?
|
-if aerobic, there is a binding of H+ and HCO3- leasind to a loss of CO2
-the decrease H+ bindingn to protein allows more Ca to bind to protein, causein a decrease in [fCa2+] |
|
|
Excpetions for when disorders of [tCa2+] are not typically disorders of [fCa2+]
|
-dec. [tCa2+] due tp hypoalbuminemia ([fCa2+] not affected)
-binding of Ca2+ to anions ([fCa2+] not directly affected) |
|
|
Different forms of Pi depending on pH
|
-H3PO4
-H2PO4- -HPO42- -PO43- |
|
|
Major factors that determine serum [Pi]
|
-intestinal absorption
-renal excretion -shifting between ICF and ECF -animal age |
|
|
Pi
-sample to collect |
-non-hemolyzed serum or plasma
|
|
|
Most common forms of Pi due to normal pH
-ratio |
-H2PO4- : HPO42-
-1:4 ration |
|
|
Hyperphosphatemia
-causes |
-dec. urinary PO4 excretion
-inc. PO4 absorption from intestine -shift of PO4 from ICF to ECF -Age -others |
|
|
Dec. urinary excretion of PO4
-reasons |
-Prerenal, Renal, Postrenal disorder
-Primary hypoparathyroidism |
|
|
Prerenal, Renal, Postrenal disorder
-pathogenesis of hyperphosphatemia |
-dec. GFR
--dec. clearance of PO4 ---inc. [PO4] --> inc. [Pi] |
|
|
Primary hypoparathyroidism
-pathogenesis of hyperphosphatemia |
-dec. production and release of PTH
--dec. [PTH] ---inc. tubular resorption of PO4 ----inc. [PO4] --> inc. [Pi] |
|
|
Hemolysis/Delayed harvesting of Serum or Plasma
-pathogenesis of hyperphosphatemia |
-Prolonged in vitro storage of RBCs or in vitro hemolysis
--PO4 leaks out of RBCs ---inc. [PO4] --> [Pi] |
|
|
Shift of PO4 from ICF to ECF
-causes |
-Myopathies
-Acute tumor lysis syndrome |
|
|
Rhabdomyolysis
-types |
-exertional
-malignant hyperthermia |
|
|
Acute-tumor lysis syndrome
-define |
-rapid death of neoplastic cells
-lymphoma |
|
|
Inc PO4 absorption from the intestine
-causes |
-phosphate enema
-hypervitaminosis D |
|
|
Phosphate enema
-pathogenesis of hyperphosphatemia |
Phosphate enema (Na & PO4)
-inc. intestinal absorption of Na --> inc. [Na] -increase intestinal absorption of PO4 --inc. [PO4] = inc. [Pi] ---inc. formation of Ca & PO4 colloid in plasma ----Ca & PO4 colloid enters macrophages ----- dec. [fCa2+] ------ dec. [tCa2+] |
|
|
Hypervitaminosis D
-pathogenesis to hyperphosphatemia |
-inc. intestinal absorption of PO4
-inc. mobilization of PO4 from bone --inc. [PO4] = inc. [Pi] |
|
|
Difference between hypervitaminosis D and inc. PTH on phosphate
|
-inc. PTH will also inc. PO4 renal excretion
|
|
|
Affect of GH on Pi levels
|
-GH will cause an increase in tubular PO4 absorption
|
|
|
Hypophosphatemia
-causes |
-dec. PO4 absorption from intestine
-inc. urinary PO4 excretion -shift in PO4 from ECF to ICF -Defective mobilization of PO4 from bone (vs loss in milk) -Equine renal disease (failure) |
|
|
Dec. PO4 absorption from the intestine
-cause |
-prolonged anorexia
|
|
|
Inc. Urinary PO4 excretion
-cause |
-inc. PTH or PTHrp activity
|
|
|
Magnesium
-most is found where |
-bones
-tissues |
|
|
In what animal is the amount of Mg in RBC not greater than the amount of Mg in plasma
|
-Cattle
|
|
|
How is Mg regulated
|
-hormones
|
|
|
Mg2+ assay
-samples to collect |
-serum or heparinized plasma
|
|
|
Hypermagnesemia
-causes |
-Renal failure and causes of decreased GFR
-pseudohypermagnesemia from in vitro hemolysis or delayed removal of RBCs from serum (not cattle) |
|
|
Hypomagnesemia
-causes |
-Hypoproteinemia (prolonged anorexia, grass tetany)
-Osmotic diuresis -ketonuria |
|
|
Grass tetany
-due to |
-cattle eating lush, green grass
|
|
|
iPTH
-define |
-immunoreactive parathyroid hormone
|
|
|
PTH
-secretion is stimulated by |
-dec. fCa2+
-dec. vitamin D |
|
|
Effect of inc. PTH on calcium and phosphorus
|
-inc. Ca mobilization and resorbtion
-dec. phosphorus retention (promotes phosphaturia) |
|
|
PTH analysis
-sample collection |
-add protease inhibitor or freeze because susceptible to proteolysis
|
|
|
PTH and fCa2+ relationship
|
-inc. [fCa2+] expect dec. [PTH]
-and vice versa |
|
|
Inc. Serum PTH
-causes |
-neoplasm of the parathyroid gland
-hyperplastic parathyroid glands |
|
|
Hyperplastic parathyroid glands due to
|
-chronic renal disease
dec. [fCa2+]: -secondary renal hyperparathyroidism -secondary nutritional hyperparathyroidism -Vit. D dependent rickets |
|
|
Dec. Serum PTH
-causes |
-damaged parathyroid glands
-inhibited parathyroid glands |
|
|
Parathyroid gland inhibition
-due to |
-hypervitaminosis D
-hypercalcemic disorders |
|
|
PTH-rp
-normal physiological processes |
-promotes Ca2+ balance in the fetus
-produced by many cells -low blood concentrations in healthy adults |
|
|
Human PTH-rp assays
-can be used for |
-dogs
-cats |
|
|
Inc. serum [PTH-rp] due to:
|
-humoral hypercalcemia of malignancy
|
|
|
HHM causes in
-dogs -cats -horses |
-dogs: lymphoma, apocrine gland carcinoma
-cats: carcinoma of the lung, kidney, bronchi -horse: carcinoma |

