![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
152 Cards in this Set
- Front
- Back
|
Which type of cardiac hypertrophy is this? pressure- or volume-overload?
- concentric hypertrophy - increase in myocyte width - increase wall thickness - decrease in left ventricle cavity |
pressure-overload hypertrophy
|
|
|
Which type of cardiac hypertrophy is this?
- eccentric hypertrophy - increase in myocyte width - increase in myocyte length - increase in left ventricle cavity |
volume-overload hypertrophy
|
|
|
What is the cause of pressure-overload hypertrophy?
|
- HTN
- aortic stenosis |
|
|
What is the cause of volume-overload hypertrophy?
|
- chronic ischemia
- mitral insufficiency |
|
|
What is an independent risk factor for sudden death?
|
left ventricular hypertrophy
|
|
|
What usually precedes heart failure?
|
- hypertrophy
- increase preload - NE activation |
|
|
Which side of the heart is failing?
- dyspnea - orthopnea - paroxysmal nocturnal dyspnea - siderophages - pre-renal azotemia - hypoxic encephalopathy |
left-sided heart failure
- caused by HTN, ischemia, aortic, mitral diseases - cause pulmonary congestion, edema |
|
|
Which side of the heart is failing?
- hepatosplenomegaly - pleuroeffusion - dependent peripheral edema |
right-sided heart failure
- caused by left-sided heart failure, chronic pulmonary HTN(cor pulmonade) |
|
|
What can cause right-sided heart failure?
|
- left-sided heart failure
- chronic pulmonary HTN(cor pulmonade) |
|
|
What can cause left-sided heart failure?
|
- HTN
- ischemia - aortic, mitral diseases |
|
|
What %stenosis is assiciated with coronary ischemia with exertion?
|
75%
|
|
|
What %stenosis is assiciated with coronary ischemia at rest?
|
90%
|
|
|
Pathogenesis of ischemic heart disease.
|
- coronary artery lesion: atherosclerosis
- acute plaque changes - coronary artery thrombus - vasoconstriction |
|
|
Where do you usually find atheroslerotic plaque in coronary arteries?
|
- proximal LAD
- left circumflex - entire RCA |
|
|
List some acute plaque changes associated with ischemic heart diseases.
|
- hemorrhage
- ulceration - rupture - adrenergic stimulation - soft atheroma - fibrous cap-artery junction fissure - stenosis (mild vs severe) |
|
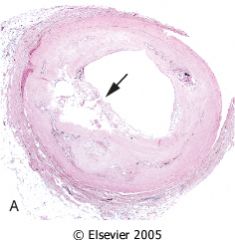
What kind of acute plaque change is this?
|
Plaque rupture
|
|
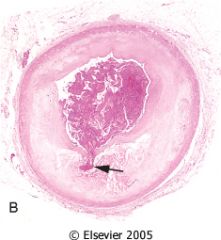
What kind of acute plaque change is this?
|
Plaque rupture with occlusive thrombus -> transmural infarction or sudden death
|
|
|
What acute plaque change is this?
- foam cells, lipids - thin fibrous cap, little smooth muscle - inflammatory cell clusters |
soft atheroma (vulnerable plaque)
|
|
|
These can cause what kind of acute plaque change?
- HTN - vasospasm - stress - circadian periodicity |
adrenergic stimulation
|
|
|
T/F: Slow progressive atherosclerosis in coronary arteries would increase collateral blood to the heart.
|
T.
|
|
|
T/F: Repetitive ischemia is protective against MI.
|
T.
|
|
|
Occlusive vs. non-occlusive thrombus?
- mural thrombus |
non-occlusive
|
|
|
Occlusive vs. non-occlusive thrombus?
- transmural thrombus |
occlusive
|
|
|
Occlusive vs. non-occlusive thrombus?
- unstable angina - subendothelial infarction - distant embolization with miroinfarct |
non-occlusive
|
|
|
4 pathogenetic mechanisms of ischemic heart disease.
|
- coronary artery lesion (atherosclerosis)
- acute plaque change - coronary artery thombus - vasoconstriction |
|
|
What is an independent preditor of coronary heart disease?
|
CRP: serum acute phase reactant
- inflammation -> endothelial cell release chemokines and adhesion molecules -> T cell and macrophage activation -> metalloproteinase digest collagen -> plaque rupture |
|
|
How does inflammation lead to ischemic heart disease?
|
- inflammation -> endothelial cell release chemokines and adhesion molecules -> T cell and macrophage activation -> metalloproteinase digest collagen -> plaque rupture -> exposed thrombogenic content -> thrombosis -> occlusion -> ischemia
|
|
|
Name the 4 syndromes of ischemic heart diseases.
|
- angina pectoris
- MI - sudden death - chronic ischemic heart disease |
|
|
Three types of angina pectoris.
|
- stable: chronic severe coronary artery stenosis
- prinzmetal variant: coronary artery spasm - unstable: crescendo angina |
|
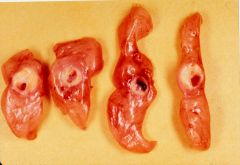
What is this?
|
acute thrombus in coronary artery
|
|
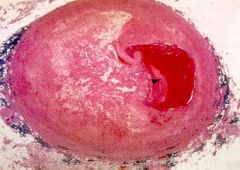
What is this?
|
stenotic plaque with occlusive thrombi
|
|
|
What type of angina pectoris is this?
- chronic severe coronary artery stenosis -> transient myocardial ischemia |
stable
|
|
|
What type of angina pectoris is this?
- coronary artery spasm -> transient myocardial ischemia |
Prinzmetal variant
|
|
|
What type of angina pectoris is this?
- plaque rupture with mural thrombus -> transient myocardial ischemia |
unstable (eg crescendo angina)
|
|
|
Occlusion of which coronary artery can cause ischemia of this region?
- anterior LV, apex - anterior interventricular septum |
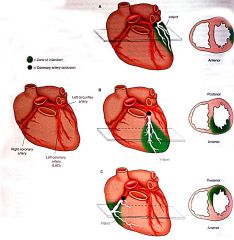
LAD
|
|
|
Occlusion of which coronary artery can cause ischemia of this region?
- inferior/posterior ventricles - posterior interventricular septum |
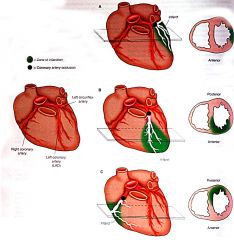
RCA
|
|
|
Occlusion of which coronary artery can cause ischemia of this region?
- lateral LV |
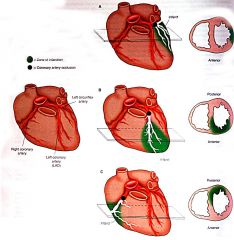
left circumflex coronary artery
|
|
|
Response of heart to ischemia.
- within seconds |
anaerobic glycolysis
|
|
|
Response of heart to ischemia.
- in 1 min |
loose contractility
|
|
|
Response of heart to ischemia.
- in 20-40 min |
irreversible cell injury
|
|
|
Response of heart to ischemia.
- in 1 hour |
microvascular injury
|
|
|
Response of heart to ischemia.
- in 2 hours |
necrosis
|
|
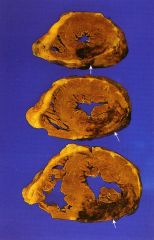
Which type of myocardial infarction is this?
|
transmural
- full thickness - caused by thrombotic occlusion of single coronary artery |
|
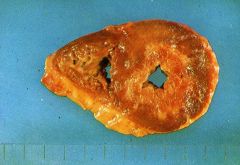
Which type of myocardial infarction is this?
|
subendothelial
- can be circumferential - caused by diffuse stenosing atherosclerosis |
|
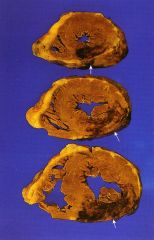
What time frame is this in?
|
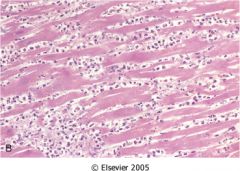
1-3 days after ischemic attack
- mottling - neutrophilic infiltrate - eosinophila in cytoplasm - no striation |
|
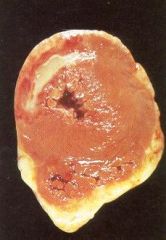
What time frame is this in?
|
3-7 days after ischemic attack.
- soft yellow center with hyperemic border - phagocytosis and granulation tissue |
|
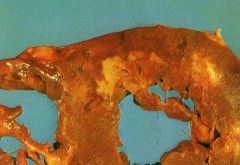
What time frame is this in?
|
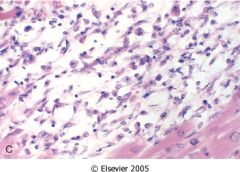
7-10 days after ischemic attack
- max yellow softening with depressed red margin - max macrophage phagocytosis and early granulation tissue at border |
|
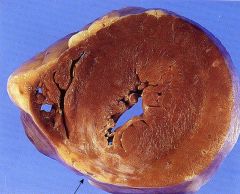
What time frame is this in?
|
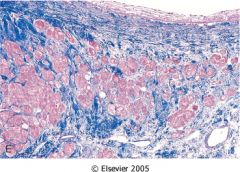
2 months after ischemic attack
- scarring complete - dense collagen |
|
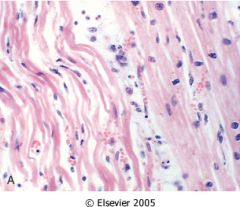
What time frame is this in?
|
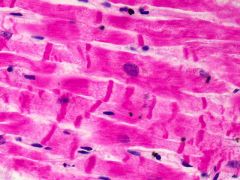
4-12 hrs after ischemic attack
- wavy fibers - neutrophils - coagulative necrosis - contraction bands |
|
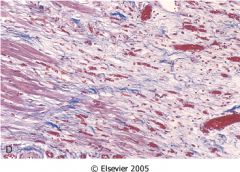
What time frame is this in?
|
2-8 wks after ischemic attack
- increased collagen - decreased cellularity |
|
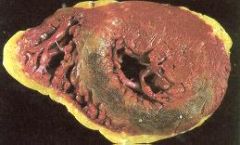
What is the cause of this?
|
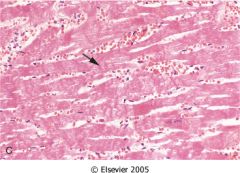
myocardial reperfusion
- hemorrhagic infarction - see contraction bands |
|
|
What are some complications of myocardial infarction?
|
- contractile dysfunction
- arrhythmia - myocardial rupture: 3-7 days after - pericarditis - RV infarction - extension/ expansion of infarct - mural thromboembolus - ventricular aneurysm: all layers - papillary muscle dysfunction with mitral valve regurgitation |
|
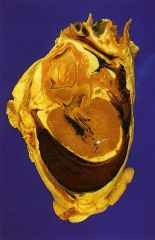
What is this complication of MI?
|
myocardial rupture with temponade
- most commonly occurs after infarction |
|
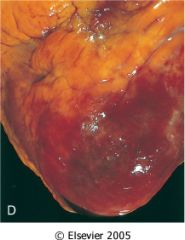
What complication of MI is this?
|
fibrinous pericarditis
|
|
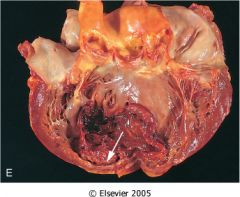
What is this complication of MI?
|
mural thrombus
|
|
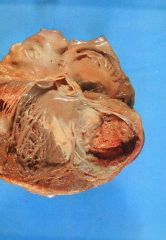
What is this complication of MI?
|
ventricular aneurysm: all layers affected
|
|
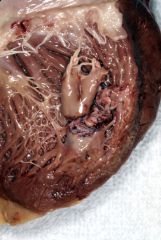
What is this complication of MI?
|
papillary muscle rupture
|
|
|
CK-MB level peaks ___ hrs after MI.
|
24 hrs
normalize 3 days after |
|
|
TroponinI level peaks ___ hrs after MI.
|
48 hrs
normalize 7-10 days after |
|
|
Mechanism of sudden death in MI.
|
lethal arrhythmia -> myocardial electrical irritability -> ventricular fibrillation, asystole
|
|
|
Features of chronic ischemic heart disease.
|
- progressive
- prior infarcts common - LV volume overload hypertrophy |
|
|
Systemic or pulmonary HTN?
HTN causes - atrial fibrillation - renal failure - progressive ischemic heart disease - heart failure |
systemic HTN
|
|
|
Systemic or pulmonary HTN?
HTN causes - right ventricular hypertrophy with dilation - acute cor pulmonade - chronic cor pulmonade |
pulmonary HTN
|
|
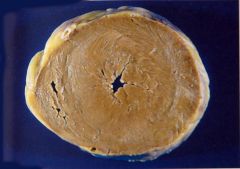
Systemic or pulmonary HTN?
|
systemic HTN
- concentric LVH (pressure overload) |
|
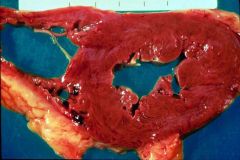
Systemic or pulmonary HTN?
|
systemic HTN
- superimposed volume overload dilation on decompensated HTN heart disease |
|
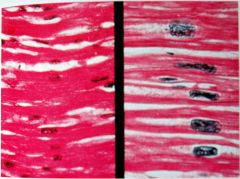
Systemic or pulomary HTN?
|
systemic HTN
- myocyte hypertrophy - myocyte irregularity and variability - increased interstitial fibrosis |
|
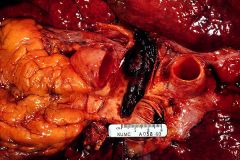
Systemic or pulmonary HTN?
|
pulmonary HTN
- acute cor pulmonade: saddle pulmonary thromboembolus - acute dilation of right ventricle |
|
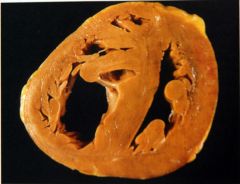
Systemic or pulmonary HTN?
|
pulmonary HTN
- chronic pulmonade - right ventricular hypertrophy with dilation |
|
|
What is the most common valvular disease?
|
senile calcific aortic stenosis
|
|
|
Possible causes of aortic stenosis.
|
- senile calcific cortic stenosis
- calcified congenital bicuspid aortic valve - rheumatic heart disease |
|
|
Possible causes of aortic insufficiency.
|
- HTN,aging -> aortic root dilation
- infective endocarditis - myxomatous valvular degeneration - rheumatic heart disease |
|
|
Possible causes of mitral insufficiency.
|
- myxomatous valvular degeneration
- infective endocarditis - rheumatic heart disease - fen-phen valvular fibrosis |
|
|
Possible causes of mitral stenosis.
|
- rheumatic heart disease
|
|
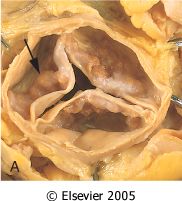
What is valvular disease?
|
senile calcific aortic stenosis
- concentric LVH: angina, syncope - no commissure fissure - base calcification > edge |
|
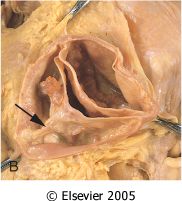
What is this valvular disease?
|
calcified congenital bicuspid aortic valve
- no commissure fissure - midline raphe - high risk for infective endocarditis |
|
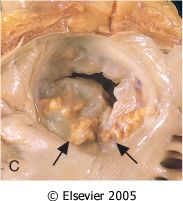
What is this valvular disease?
|
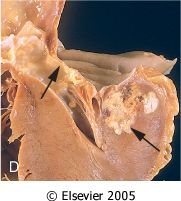
mitral annular calcification
- degenerative calcification - hear mid systolic murmur - can thromboembolize - risk for infective endocarditis |
|
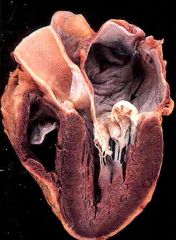
What is this valvular disease?
|
myxomatous degeneration of mitral valve
- mitral valve prolapse - thick rubbery valve leaflets ballooning into atrium: fibrosa thinned - thin elongated chordae - secondary atrial and ventricular thickening - thrombi on superior valve surface |
|
|
What is this valvular disease?
- thick rubbery mitral valve leaflets ballooning into atrium: fibrosa thinned - thin elongated chordae - secondary atrial and ventricular thickening - thrombi on superior valve surface |
myxomatous degeneration of mitral valve
|
|
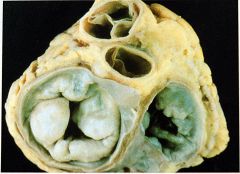
What is this valvular disease?
|
myxomatous degeneration of mitral and tricuspid valve
- connective tissue disorder - associated with marfan syndrome |
|
|
What is this vavular disease?
- connective tissue disorder - associated with marfan syndrome |
myxomatous degeneration of mitral and tricuspid valve
|
|
|
What is this disease?
- migratory painful polyarthritis - acute pancarditis - painless subcutaneous nodules - truncal rash (erythema marginatum) - syndenham's chorea |
acute rheumatic fever -> pancarditis
- acute valvulitis - fibrinous pericarditis - myocarditis: aschoff bodies |
|
|
What is this valvular disease?
- verrucae on mitral valve closure line |
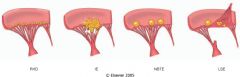
acute rheumatic valvulitis
|
|
|
What is this valvular disease?
- ring abscess - large destructive vegetation |
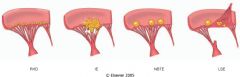
acute infective endocarditis
|
|
|
What is this valvular disease?
- large non-destructive vegetation |
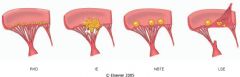
subacute infective endocarditis
|
|
|
What is this valvular disease?
- small-medium vegetation along closure lines |
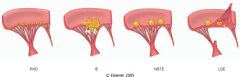
non-bacterial thrombotic endocarditis
|
|
|
What is this valvular disease?
- small vegetations not confined to closure lines |
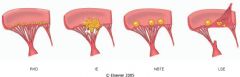
SLE
|
|
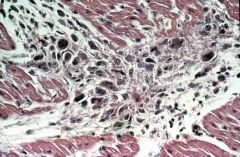
What disease does this suggest?
|
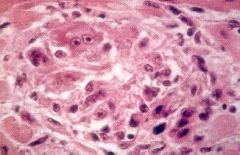
acute rheumatic fever
- Aschoff bodies - lymphocytes - necrotic collagen |
|
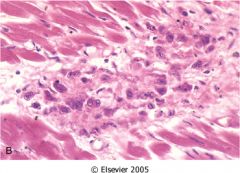
What disease does this suggest?
|
acute rheumatic fever
- aschoff bodies - lymphocytes - necrotic collagen |
|
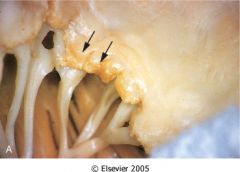
What is this valvular(mitral) disease?
|
acute rheumatic vavulitis
- verrucae on closure line |
|
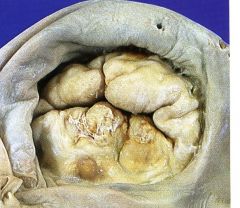
What is this valvular disease?
|
chronic rheumatic heart disease
- fibrotic mitral valve - fused commissure (fish mouth) |
|
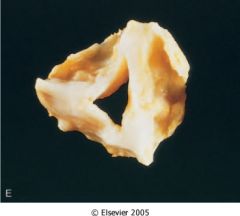
What is this vlavular disease?
|
Chronic rheumatic heart disease
- fibrotidc aortic valve - fused commissures |
|
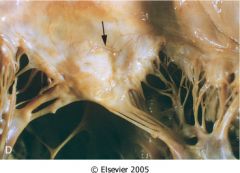
What is this valvular disease?
|
Chronic rheumatic heart disease
- fibrotic mitral valve - thick and fused chordae |
|
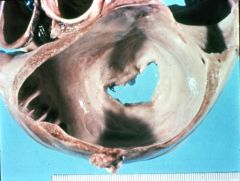
What is this valvular disease?
|
chronic rheumatic heart disease
- fibrotic mitral valve - fused commissures - stenosis - left atrial enlargement |
|
|
List the 4 types of endocarditis.
|
- infective
- non-bacterial - SLE (Libman-Sack disease) - carcinoid heart disease |
|
|
Name some microbes that can cause acute infective endocarditis.
|
- s. aureus
- s. pneumoniae - gram- enterics - fungi |
|
|
Name some microbes that can cause subacute infective endocarditis.
|
- s. viridian
- s. fecaelis - s. bovis |
|
|
Name some microbes that can cause infective endocarditis on prothetic valves.
|
- coagulase- staph: eg staph epidermidis
|
|
|
What is this heart disease?
- spiking fever, chills, petechiae - rapidly progressive, destructive - ring abscess - large destructive vegetations on heart valves |
acute infective endocarditis
|
|
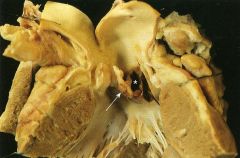
What is this disease?
|
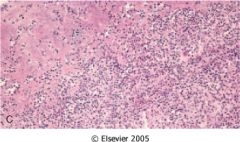
acute infective endocarditis
- ring abscess - large destructive vegetations - see neutrophils and fibrin |
|
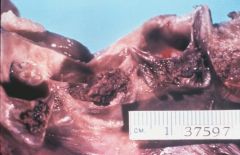
What is this disease?
|
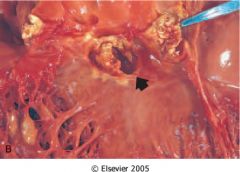
acute infective endocarditis
- large destructive vegetation - also see ring abscesses(see figure) |
|
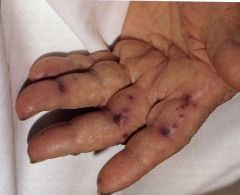
This is a minor injury in what disease?
|
acute infective endocarditis
- janeway lesion: non-painful infarcted macules and papules |
|
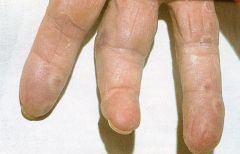
This is a minor injury in what disease?
|
acute infective endocarditis
- osler nodes |
|
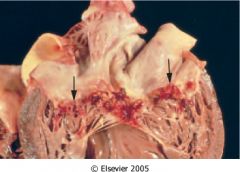
What is this valvular disease?
|
subacute infective endocarditis
- large non-destructive vegetation |
|
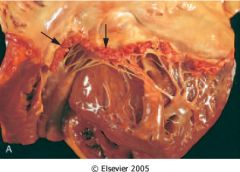
What is this valvular disease?
|
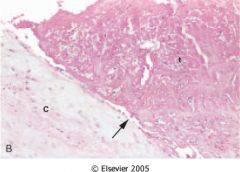
non-bacterial thrombotic endocarditis
- small-medium vegetation along closure lines - fibrin, no inflammatory cells |
|

What is this valvular disease?
|
SLE endocarditis
- small vegetations not confined to closure lines - can be on underside of valves - fibrinous hematoxylin bodies |
|
|
What valvular disease is this?
- affect right sided leaflet - mural intimal smooth muscle proliferation - collagenous proliferation - some associated with serotonin producing carcinoid tumors |
carcinoid heart disease
|
|
|
What valvular disease is this?
- anticoagulant related hemorrhage - thromboemboli - infective endocarditis |
complications associated with mechanical prosthetic valves
|
|
|
What valvular disease is this?
- degenerative changes with calcification - infective endocarditis |
complications associated with bioprosthetic valves
|
|
|
List the three types of cardiomyopathies.
|
- dilated cardiomyopathy
- hypertrophic cardiomyopathy - restrictive cardiomyopathy |
|
|
Some primary causes of dilated cardiomyopathy.
|
- x-linked muscular dystrophy
- mitochondrial disease in children |
|
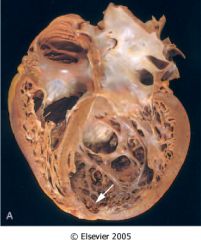
What is this heart disease?
- 4 chamber dilation - myocyte hypertrophy - systolic dysfunction - interstitial fibrosis |
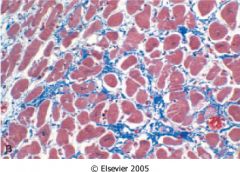
dilated myopathy
|
|
|
Some secondary causes of dilated cardiomyopathy.
|
- alcohol
- pregnancy - viral myocarditis: coxsakievirus B - hemochromatosis: iron overload - chronic anemia - doxorubicin/daunorubicin - sarcoidosis: numerous epicardial granuloma |
|
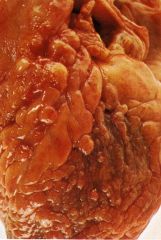
What is this disease?
|
Sarcoidosis -> dilated cardiomyioathy
- numerous epicardial granulomas |
|
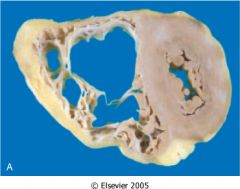
What is this disease?
|
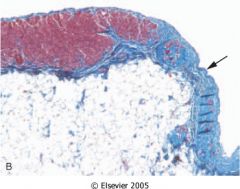
arrhythmic RV cadiomyopathy
- RV thinning - chromosome 14 - fatty infiltration and interstitial fibrosis |
|
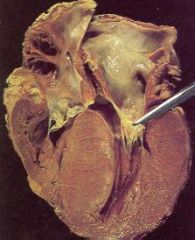
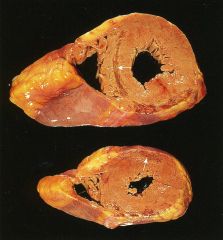
What is this heart disease?
|
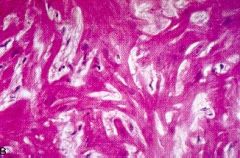
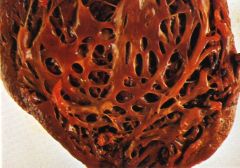
Hypertrophic cardiomyopathy
- LVH, diastolic dysfunction - septal thickening - "banana" ventricular cavity - myocyte hypertrophy with disarray - interstitial fibrosis |
|
|
What is the most common cause of sudden death in young atheletes?
|
hypertrophic cadiomyopathy
- AD: sarcomeric protein mutation (B-myosin heavy chain, myosin binding protein C, troponin-T) |
|
|
What are some treatment for hypertrophic cardiomyopathy?
|
- medications for ventricular relaxation
- excise LV outflow obstruction |
|
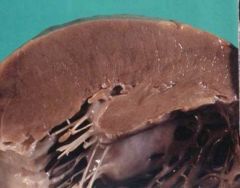
What is this heart disease?
- mild myocyte hypertrophy - diastolic dysfunction - bilateral dilation - "Wax drip" atrial endocardoial nodule - pale waxy myocardium - smooth firm rubbery endocardium |

restrictive cardiomyopathy (amyloidosis)
|
|
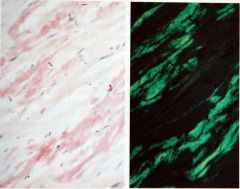
What is this heart disease?
- congo red stain - apple-green birefrigence |
cadiac amyloidosis -> restrictive cardiomyopathy
|
|
|
List some types of cardiac amyloidosis.
|
- senile cardiac amyloidosis: transthyrectin deposits
- isolated atrial amyloidosis: ANP deposits - systemic amyloidosis |
|
|
What type of cardiac amyloidosis?
- more in elderly black people - transthyrectin deposits |
senile cardiac amyloidosis
|
|
|
What type of cardiac amyloidosis?
- ANP deposits |
isolated atrial amyloidosis
|
|
|
What is this heart disease?
- caused by eosinophilic leukemia |
Leoffler's endomyocarditis
- fatal - treated by surgical endomyocardial stripping |
|
|
List come causes of infectious myocarditis.
|
- viral
- chlamydia - rickettiae - bacterial: c. diptheria, n. menigococcus, b. burgdorferi - protozoa: t. cruzi, t. gondi - helminth: t. spiralis |
|
|
List some causes non-infectious myocarditis.
|
- drug hypersensitivity: antibiotics, diuretics, anti-HTN
- immune related: SLE, rheumatic fever, transplant rejection - sarcoidosis - giant cell |
|
What is this heart disease?
|
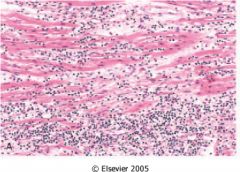
viral myocarditis
- flabby myocardium with hemorrhagic and pale areas. - chronic lymphocytic infiltrate with myocyte damage |
|
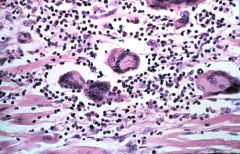
What is this heart disease?
|
giant cell myocarditis
- chronic infiltrate with giant cells - pale and hemorrhagic myocardium - bad prognosis |
|
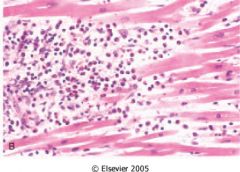
What is this heart disease?
|
hypersensitivity myocarditis
- chronic esodinophilic infiltrate |
|
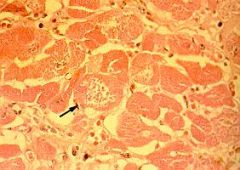
What is this heart disease?
|
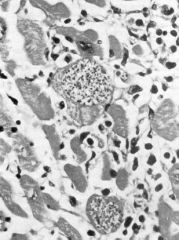
chagas disease
- trypanosomes in myocytes with mixed inflammation |
|
|
List some types of acute pericarditis.
|
- serous
- fibrinous/serofibrinous pericarditis - purulent/supperative - hemorrhagic caseous |
|
|
List some types of chronic pericarditis.
|
- adhesive pericarditis
- adhesive mediastnopericarditis pericarditis - constrictive pericarditis |
|
|
Diastolic or systolic problem?
- constricitive pericarditis (chronic) |
diastolic dysfunction: require pericardiectomy
|
|
|
Some causes of pericarditis.
|
- infections: viral, bacteria, fungal, parasites
- immune mediated: RF, SLE, scleroderma, post-cardiotomy, post-MI, drug hypersensitivity. - uremia - MI - cardiac surgery - neoplasms - trauma - radiation |
|
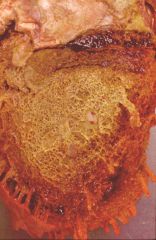
What type of heart disease is this?
- friction rub - yellow cloudy fluid with fibrin and scant inflammatory cells (see figure) |
fibrinous pericarditis (most common)
- MI - uremia - radiation - RF, SLE, RA - trauma |
|
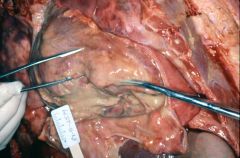
What heart disease is this?
- fever, chills - white exudates with abundant acute inflammation (see figure) |
purulent pericarditis
- infectious cause: via blood, lymphatics, empyema, pneumonia, mediastinitis, annular ring abscess, surgery |
|
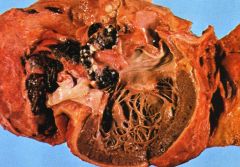
What heart disease is this?
- thick organizing visceral pericardium - black and white caseous mediastinal lymph nodes (see picture) |
caseous pericarditis
- TB - most frequent precursor of diabling constrictive pericarditis |
|
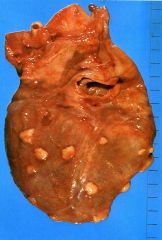
What is this disease?
|
carcinomatous pericarditis
- nodules of metastatic breast cancer |
|
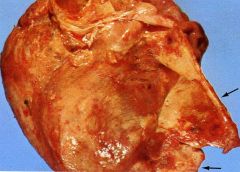
What is this heart disease?
- organization obliterates pericardial sac and forms thick dense fibrous or fibrocalcific scar - diastolic dysfunction - require pericardiectomy |
constricitive pericarditis
- fibrotic parietal peritoneum peeled off left ventricle |
|
|
What is the most frequent precursor of diabling constrictive pericarditis?
|
caseous pericarditis (TB)
|
|
|
What is this pericardial disease?
- clear fluid with scant chronic inflammatory cells - usually resolves without organization |
serous pericarditis
- usually non-infectious |
|
|
What is this pericardial disease?
- bloody with fibrinous or supprative fluid - most commonly caused by neoplasms |
hemorrhagic pericarditis
|
|
|
What is this pericardial disease?
- delicate stringy organization obliterates pericardial sac - rarely symptomatic |
adhesive pericarditis (chronic)
|
|
|
What is this pericardial disease?
- organization obliterates pericardial sac - external parietal pericardium adheres to mediastinal structures - cause cardiac hypertrophy and dilation |
adhesive mediastinopericarditis (chronic)
|
|
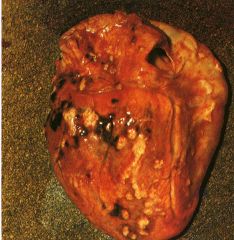
What is this heart disease?
- cause fibrinous pericaridits most often - aortic valvulitis |
rheumatoid heart disease
- no commissure fission - rheumatoid nodules of myocardium, endocardium, valves, aorta |
|
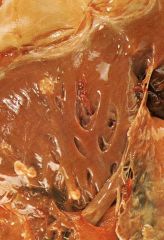
What is the most common heart tumor?
|

- metastatisis from other cancers: lung, breast, esophageal, melanoma, lymphoma/leukemia
- nodules of metastatic carcinoma to heart (see figure) |
|
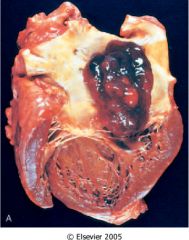
What is this heart disease?
- most common primary heart tumor - mojority in LA - sessule or pedunculated gelatinous or hard mass (see figure) |
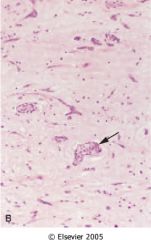
myxoma
- stellate myxoma cells - endothelial cells - smooth muscle cells - acid mucopolysaccharide matrix |
|

What is this heart disease?
- valvular neoplasm - hair-like projections on valvular surface (see figure) |
papillary fibroelastoma
- myxoid tissue with elastic fibers - can embolize |
|
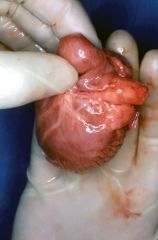
What is this heart disease?
- most common primary heart tumor in children - hemartoma: associated with tuberous sclerosis - gray myocardial mass protruding into ventricle (see figure) |
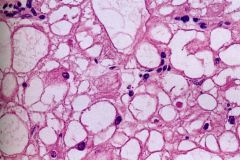
rhabdosarcoma
- spider cells: central nucleus with cytoplasmic glycogen vacules |
|

What is this heart disease?
- most common primary cadiac malignancy - poor prognosis |
angiosarcoma
|
|
|
What is this heart disease?
- poorly encapsulated tumor of mature adipose tissue - possible hamartoma |
lipoma
- common in LV, RA, atrial septum: subendocardium, supepicardium, myocardium |
|
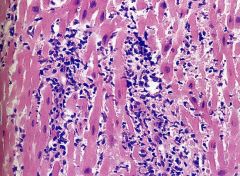
What type of graft rejection is this?
- intersitital lymphocytes - myocyte damage |
acute rejection
- requires immunosuppresion |
|
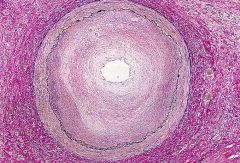
What type of graft rejection is this?
- diffuse stenosing intimal proliferation |
chronic (graft arteriopathy)
- silent infarction in denervated heart - CHF or sudden death - the cause is low level inflammation |

