![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
76 Cards in this Set
- Front
- Back
|
Cytokine |
Communication molecule |
|
|
Macrophages engulf and destroy by |
Phagocytosis |
|
|
Types of leukocytes |
Lymphocyte, monocyte, eosinophil, basophil, neutrophil |
|
|
Intracellular signaling leads to |
1. Upregulation and/or down regulation of genes, transcription factors; 2. Production of other cytokines; 3. Increase in # of surface receptors for other molecules; 4. Suppression of their own effect by feedback inhibition |
|
|
Cells that release inflammatory mediators |
Basophils, eosinophils |
|
|
Phagocytic cell types |
Macrophages, neutrophils, monocytes |
|
|
Main function of dendritic cells |
"Gather up" antigens, bring them to T-cells, and initiate response from those T-cells |
|
|
Antigen |
Anything that initiates an adaptive immune response |
|
|
Where do B-lymphocytes develop? |
Bone marrow |
|
|
Where do T-lymphocytes develop? |
Thymus |
|
|
T-helper lymphocyte function |
Help B-lymphocytes and macrophages |
|
|
T-cytotoxic lymphocyte function |
Kill virus-infected cells; kill some tumor cells |
|
|
B-lymphocytes and antigens |
Interact directly |
|
|
T-lymphocytes and antigens |
Antigens are "presented" to T-helper cells by virus-infected cells that need to be "killed" |
|
|
Each B-lymphocyte has a very specific surface receptor that... |
Binds to only one; can respond to any type of biomolecule; may require "help" from T-helper lymphocytes |
|
|
T-cells only respond to: |
Short peptides |
|
|
MHC |
Major Histocompatibility Complex |
|
|
Normal role of MHCs |
Present peptides to T-lymphocytes |
|
|
MHC Class I |
Present peptides to T-cytotoxic cells |
|
|
MHC Class II |
Present peptides to T-helper cells |
|
|
CD8 |
Cell surface molecule presented on T-cytotoxic cells; looking for peptides presented only by MHC Class I |
|
|
CD4 |
Cell surface molecule presented on T-helper cells; looking for peptides presented only by MHC Class II |
|
|
Specificity for presented peptide is determined by: |
Peptide-specific receptor |
|
|
Function of responding cell is selected by: |
Type of MHC presenting peptide |
|
|
Antigen vaccine |
From killed or weakened organism. Will not cause infection or disease |
|
|
Attenuated vaccines |
Weakened version of organism |
|
|
Inactivated vaccines |
Dead form of organism. (Inactivated toxin -toxoid) |
|
|
Current vaccines |
Protective |
|
|
Recent vaccines |
Therapeutic |
|
|
Future vaccines |
Immunogenic and Tolerogenic |
|
|
Immunogenic |
Produces immune response |
|
|
Tolerogenic |
Produces immunological tolerance; induces immune state of unresponsiveness to foreign antigen |
|
|
Adjuvant |
Substance that enhances body's immune response |
|
|
Therapeutic |
Raise immune response during ongoing disease |
|
|
Prophylactic |
Trigger immunological memory |
|
|
Practical introduction to immune system |
Course goal |
|
|
Stimulate critical thinking about design and application of biomaterials |
Course goal |
|
|
Connect cellular and molecular biology concepts and apply to immune system |
Course goal |
|
|
Showcase clinical problems in immunology and biomaterial science |
Course goal |
|
|
Introduce interaction of various immune system components with engineered biological devices; implants; cells and tissues |
Course goal |
|
|
Explore strategies and solutions for maximizing biocompatibility of engineered biomaterials with immune system |
Course goal |
|
|
Immune system is collectively all of the cells/tissues and chemicals in body that are dedicated to: |
Defend it from invasion by pathogens |
|
|
All of the cells of the immune system originate in the: |
Bone marrow |
|
|
White blood cell location |
Blood and lymphatic system |
|
|
Neutrophils - found in ___, function is:____ |
Blood; attracted to and release cytokines |
|
|
Human immune system's natural goal of homeostasis involves destroying any "foreign" (non-self) material using immune responses. What response does not involve foreign material? |
Autoimmune response |
|
|
Define biocompatibility related to interaction of biomaterials with immune system |
State in which biomaterials are able to exist and function in human body without causing adverse immune response |
|
|
Prerequisite tests for evaluation of biocompatibility of materials: |
Performance standards under simulated conditions, end use applications, exposure (body temp, water, ions, pH, dissolved gases, electrolytes, cells, proteins), safety |
|
|
Biomaterials such as medical devices sold in USA must be registered through what agency? |
FDA |
|
|
Characteristics of innate immunity are variable or fixed? |
Variable |
|
|
Adaptive immunity increases or declines during response? |
Declines |
|
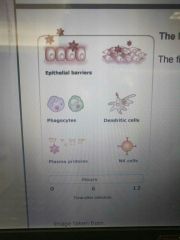
Innate or adaptive? |
Innate |
|
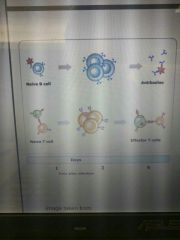
Innate or adaptive? |
Adaptive |
|
|
Challenges of ensuring biocompatibility of engineered materials/cells/tissue |
Foreign body response, chronic inflammation, no current vaccine available, safety, design challenges |
|
|
Biomaterials recognized as "non-self" by human immune system. In order to achieve biocompatibility they must be designed to: |
Resist body's natural goal of homeostasis |
|
|
Non-specific defenses of innate immunity |
Physical barriers, complement system, inflammatory mediators, phagocytic cells, cytokines |
|
|
Are antibodies part of innate immune system? |
No |
|
|
Main components of innate immune system |
Physical epithelial barriers, phagocytic leukocytes, circulating plasma proteins, natural killer cells |
|
|
Two distinct branches of adaptive immune system |
Humoral and cell mediated |
|
|
Biomaterials can initiate which three innate immune responses? |
Inflammation, phagocytosis, and cytokine signaling |
|
|
Biomaterials (not from living things) |
Metals, metal alloys, metal oxides, glass, synthetic polymers, adhesives |
|
|
Properties of biomaterials to consider |
Physicochemical properties, durability, desired functions, physiology and anatomy, effects of failure, cost, manufacturing, material strength, stiffness and flexibility, fatigue endurance, wear resistance, dimensional stability, dynamic loading conditions, electrical and thermal conductivity, light transmission, size, biodegradability, bioactivity, self-repair, metal corrosion |
|
|
The complement system is considered humoral immunity but is part of the innate immune system largely due to the fact that: |
It is not adaptable/does not change over course of an individual's lifetime |
|
|
Basic functions of complement system |
Optimization, cell lysis, apoptosis, agglutination |
|
|
How do biomaterials trigger the complement system specifically? |
Blood and plasma protein adhere to biomaterials |
|
|
Key roles of skin interface |
Protect against pathogens, protect against excessive water, insulation, temperature regulation, sensation, synthesis of vitamin D, protection of vitamin B folates |
|
|
Skin functions- protect deeper tissues from: |
Mechanical damage (bumps), chemical damage (acids and bases), bacterial damage, ultraviolet radiation (sunlight), thermal damage (heat or cold), dessication (drying out) |
|
|
3 main layers of skin |
Epidermis, dermis, subcutaneous tissue |
|
|
Parts of epidermis |
Stratum: dead layer of skin, melanin: skin pigmentation |
|
|
Parts of dermis |
Blood vessels, sweat glands, collagen fibers, nerves, smooth muscle fibers |
|
|
Responsibilities of dermis |
Structural integrity, elasticity, resiliency |
|
|
Subcutaneous tissue |
Fat (adipose) tissue - gives skin shape |
|
|
Subcutaneous tissue contains: |
Blood vessels, nerves, collagen fibers |
|
|
Laceration |
Wound produced by tearing of soft body tissue; irregular, jagged and often contaminated with bacteria and debris from whatever object caused it |
|
|
Puncture wound |
Usually caused by a sharp pointy object; usually does not bleed excessively; can appear to close up; prone to infection |
|
|
Four phases of wound healing |
1. Haemostasis 2. Inflammatory response 3. Proliferation 4. Remodelling |

