![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
85 Cards in this Set
- Front
- Back
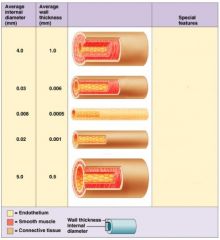
arteries
|
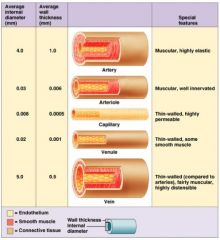
conducting vessels
∙ high pressure ∙ thick-walled, muscular & elastic ("pressure reservoir") |
|
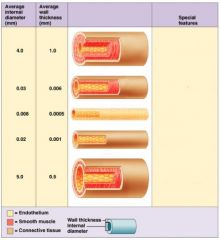
arterioles
|
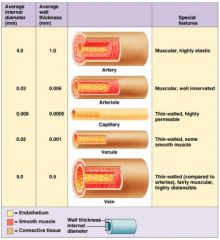
resistance vessels
∙ supply capillary beds ∙ smooth muscle in walls → vasoconstriction/vasodilation ∙ regulate local blood flow |
|
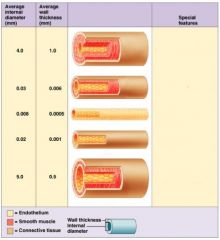
capillaries
|
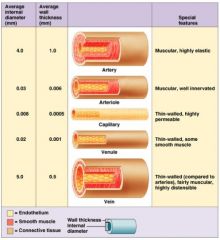
exchange vessels
∙ microscopic, very thin walls (endothelium) ∙ permeability of capillary walls: continuous < fenestrated < sinusoid |
|
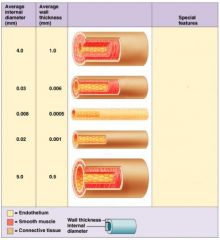
venules
|
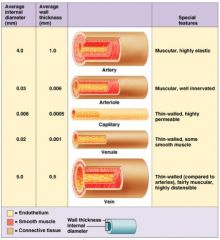
small, thin walled
∙ drain capillaries |
|
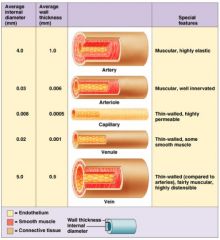
veins
|
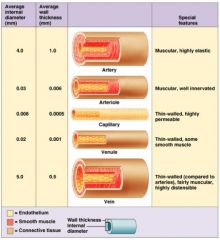
low pressure conducting vessels
∙ relatively thin-walled, high compliance/flexibility (:"volume reservoir") ∙ valves assist in one-way flow back to heart |
|
Physiology of Circulation:
Blood Pressure |
∙ Force exerted by blood on the walls of the blood vessels
∙ Expressed I'm millimeters of mercury (mm Hg) ∙ e.g. BP of 120 mm Hg = pressure exerted by column of mercury 120 mm high ∙ All vessels have an associated pressure, however blood pressure typically refers to arterial pressures |
|
As we saw with the heart → it is the _____ in BP (__________) that drives blood flow
|
difference: pressure gradient
|
|
|
What are the four main factors that affect blood pressure:
|
1) resistance
2) cardiac output 3) vessel elasticity 4) blood volume resistance and cardiac output are the most important |
|
|
resistance
|
• opposition to flow of blood in vessels
∙ measure of the amount of friction blood encounters ∙ most friction encountered in the systemic circulation is far from heart ∙ therefore referred to as peripheral resistance (PR) |
|
|
Three important sources of resistance are:
|
1) blood viscosity
2) total blood vessel length 3) blood vessel diameter (**most important & changes most frequently) |
|
|
blood viscosity
|
blood thickness of "stickiness"
∙ Viscosity and resistance are directly proportional ∙ ↑ viscosity ↑ resistance ∙ Viscosity does not change often in a healthy person |
|
|
Causes of viscosity
|
∙ dehydration
∙ ↑ EPO production (↑ RBC formation) |
|
|
blood vessel length
|
blood vessel length and resistance are directly proportional
∙ ↑ length ↑ resistance ∙ BV length does not change often in a healthy person |
|
|
Causes of an ↑ length
|
growth of adipose tissue → results in new blood vessel formation and thus an ↑ in total vessel length
|
|
|
blood vessel diameter
|
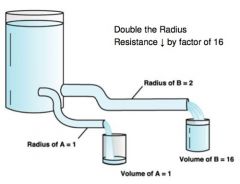
most important
∙ resistance is inversely proportional to BV radius by the 4th power (1/r⁴) ∙ ↓ BV radius ↑↑↑↑↑ resistance ∙ BV diameter does change often in a healthy person |
|
|
causes of an ↓ BV diameter
|
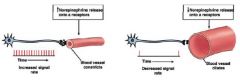
∙ vasoconstriction of vessels
∙ SNS vasomotor fibers release NE ∙ Vasoconstriction hormones Epinephrine, Angiotensin II, ADH |
|
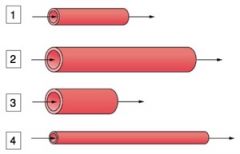
Which tube has the LEAST resistance?
Which tube has the GREATEST resistance? |
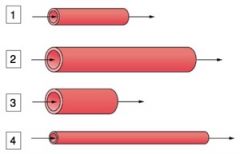
LEAST RESISTANCE - 3
GREATEST RESISTANCE - 4 |
|
|
Blood encounters resistance when is contacts blood vessel walls
If resistance ↑ blood pressure must ↑ to keep blood moving |
↑ Viscosity ↑ BV Length and ↓ BV Diameter →→ ↑ Blood Pressure
↓ Viscosity ↓ BV Length and ↑ BV Diameter →→ ↓ Blood Pressure |
|
|
Blood Pressure and Vessel Elasticity
Healthy arteries are elastic (stretch and recoil) as blood moves through them |
serves as "shock absorbers" to reduce sudden ↑ in BP as blood is forcefully pumped in "waves" from heart to arteries
|
|
|
Blood Pressure and Vessel Elasticity
Unhealthy (non-elastic or occluded) arteries cannot expand |
artery walls therefore experience higher blood pressure & can become damaged
|
|

Blood Pressure and Blood Volume (BV)
As BV ↑ in vessel, more fluid presses against vessel walls → |

causing a ↑ BP
|
|

Blood Pressure and Blood Volume (BV)
As BV ↓, less fluid presses against vessel walls → |

causing a ↓ BP
|
|
|
Blood Pressure and Blood Volume (BV)
Causes of ↑ blood volume |

↑ salt intake ("H₂O follows salt" into ECF (blood)), overhydration
|
|
|
Blood Pressure and Blood Volume (BV)
Causes of ↓ blood volume |
dehydration, excessive sweating, hemorrhaging
|
|
|
Blood Pressure and Cardiac Output
Increasing CO will cause an increase in BP because more pressure is being exerted against vessel walls |
Cardiac Output = Heart Rate x Stroke Volume
|
|
|
Increasing HR or SV will _________ CO and therefore BP
|
increase
|
|
|
Decreasing HR or SV will _________ CO and therefore BP
|
decrease
|
|
|
Blood Flow
|
volume (not speed) of blood flowing through a vessel, organ, or entire circulation in a given period of time:
∙ measured in ml per minute ∙ equivalent to cardiac output (CO) when considering entire CV system ∙ relatively constant when at rest ∙ varies widely through individual organs |
|
Blood Flow (F) is:
|
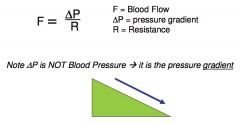
∙ directly proportionally to the difference in blood pressure (△P) between two points in the circulation
∙ inversely proportional to the resistance of the vessel connecting those 2 points |
|
|
Relationship between blood flow and the pressure gradient (△P)
|
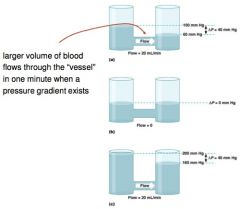
larger volume of the blood flows through the "vessel" in one minute when a pressure gradient exists
|
|
|
High Blood Flow (F) vs Low Blood Flow (F)
|
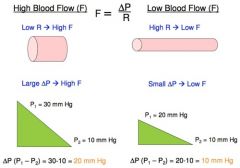
|
|
|
systemic blood pressure
|
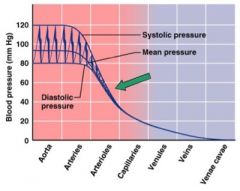
pumping action of heart generates blood flow through vessels along a pressure gradient (always moving from higher to lower pressure areas)
• pressure = highest in aorta (100mm Hg) • declines throughout length of pathway • pressure = 0 mm Hg in right atrium Steepest change in blood pressure occurs in arterioles |
|
|
Steepest change in blood pressure occurs in ________
|
arterioles
|
|
|
systolic pressure
|
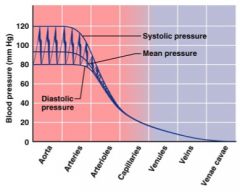
pressure exerted on arterial walls during ventricular contraction
|
|
|
diastolic pressure
|
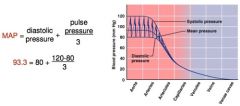
lowest level of arterial pressure during a ventricular cycle
|
|
|
pulse pressure
|
the difference between systolic and diastolic pressure
|
|
|
mean arterial pressure (MAP)
|
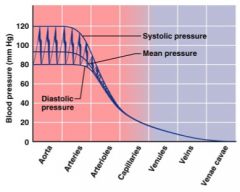
pressure that propels blood to tissues
|
|
|
pulse pressure
|
the difference between systolic and diastolic pressure
|
|
|
MAP =
|
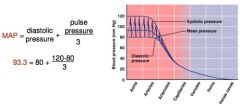
diastolic pressure + 1/3 pulse pressure
Since diastole lasts longer than systole, MAP is not simply the average of systolic and diastolic pressure |
|
|
Blood Pressure (MAP Regulation)
Maintaining blood flow is vital for proper organ function tissue perfusion - |
blood flow through tissues
|
|
|
To ensure blood flow to all tissues, body regulates/maintains homeostasis of:
|
cardiac output, resistance, and blood volume
|
|
|
What are the two types of MAP regulation?
|
short term controls and long term controls
|
|
|
MAP Regulation
short term controls |
mediated by:
a) nervous system b) hormones • counteract moment-to-moment fluctuations in blood pressure by altering Resistance • can also affect Cardiac Output |
|
|
MAP Regulation
long term controls |
mediated by:
a) renal mechanisms regulate Blood Volume b) additional hormonal mechanisms • regulate Blood Volume |
|
|
Brain Centers (Medulla Oblongata) for ____ term control of MAP
|
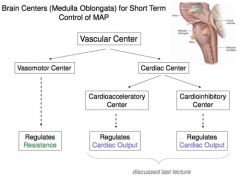
short
|
|
|
Vasomotor center
|
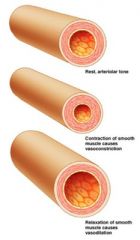
in medulla oblongata regulates diameter of blood vessels (resistance)
• transmits impulses via SNS fibers that innervate smooth muscle (tunica media) of arteries (esp. arterioles) |
|
|
Vasomotor tone
|
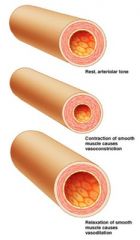
arterioles are almost always in state of moderate constriction; varies by location/organ
|
|
|
↑ SNS activity =
|
vasoconstriction
|
|
|
↓ SNS activity =
|
vasodilation
|
|
|
Baroreceptors
|
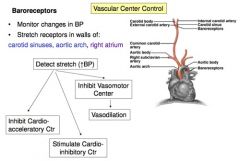
• monitors changes in BP
• stretch receptors in walls of: carotid sinuses, aortic arch, right atrium |
|
|
Baroreceptor Reflexes
|
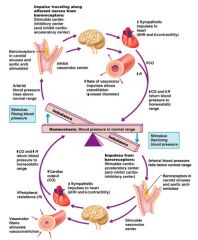
Vascular Center Control
|
|
|
Baroreceptor Reflexes
When blood pressure rises, Vascular centers: |
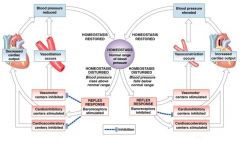
decrease cardiac output
cause peripheral vasodilation |
|
|
Baroreceptor Reflexes
When blood pressure falls, Vascular centers: |
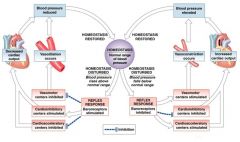
increase cardiac output
cause peripheral vasoconstriction |
|
|
What hormones increase MAP?
|
vasopressin (ADH), Anglotensin II, and Adrenal medulla hormones
|
|
|
Vasopressin (ADH)
|
causes vasoconstriction in most tissues
|
|
|
Anglotensin III
|
causes vasoconstriction
|
|
|
Adrenal medulla hormones
|
epinephrine & norepinephrine cause vasoconstriction in most tissues and ↑ CO
|
|
|
What hormones decrease MAP?
|
Atrial natriuretic peptide (ANP) & Brain natriuretic peptide (BNP)
|
|
|
Atrial natriuretic peptide (ANP) & Brain natriuretic peptide (BNP)
|
cause vasodilation (and other LONG TERM mechanisms)
|
|
|
Long-Term Mechanisms: Renal Regulation
Kidneys act directly and indirectly to maintain long-term blood pressure by altering blood volume (rather than peripheral resistance): |
1) Direct renal mechanism
2) Indirect renal mechanism |
|
|
Long-Term Mechanisms: Renal Regulation
Direct renal mechanism |
alters BV by altering filtration rate
**without use of hormones BV or MAP rises ↓ rate that fluid from bloodstream is filtered at kidneys rises (= more urine production) BV or MAP falls ↓ rate that fluid from bloodstream is filtered at kidneys falls (= less urine production) |
|
|
Long-Term Mechanisms: Renal Regulation
Indirect renal mechanism |
involves renin-angiotensin mechanism
MAP falls ↓ Renin (enzyme) released from kidneys ↓ Triggers enzymatic cascade that produces angiotensin II ↓ Angiotensin II - vasoconstrictor & stimulates aldosterone & ADH release ↓ aldosterone enhances Na+ reabsorption at kidneys ("H₂O follows") & ADH ↑ H₂O reabsorption at kidneys (both decrease urine production) |
|
|
An _____ in BV raises MAP (because of a greater fluid load in the vascular system); _____ BV causes fall in MAP
|
increase: decrease
|
|
|
Long-Term Mechanisms: Additional Hormonal Mechanisms
Renal mechanism |
stimulates release of hormones to regulate blood volume
• angiotensin II, ADH, aldosterone |
|
|
Long-Term Mechanisms: Additional Hormonal Mechanisms
Additional hormones regulate blood volume: |
1) ANP/BNP
• Reduce Blood Volume ∙ increase Na+ excretion at kidneys ∙ block release of ADH, aldosterone, epinephrine, and norephinephrine ∙ reduce thirst ∙ promote water loss at kidneys (↑ urine production) 2) EPO • Increase Blood Volume ∙ stimulate RBC production → ↑ volume |
|
|
Capillary Exchange
|
• exchange occurs between blood plasma and interstitial fluid
• vital for maintaining homeostasis nutrients, wastes, signaling molecules are exchanged via diffusion |
|
|
diffusion
|
movement of ions or molecules from high to low concentration (down concentration gradient)
|
|
|
________ is also exchanged in slightly more complex manner
|
Fluid
|
|
|
Two forces at work during capillary exchange of fluids
|
Hydrostatic pressure & Osmotic Pressure
|
|
|
Hydrostatic Pressure
|
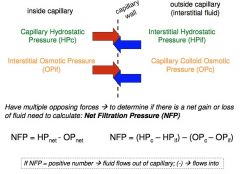
force exerted by fluid pressing against a wall
in capillaries = Capillary Hydrostatic Pressure (HPc) ~ capillary blood pressure (pressure of blood against wall) Force fluids OUT of capillary in interstitial fluid = Interstitial Hydrostatic Pressure (HPif) Force fluids INTO capillary |
|
|
Osmotic Pressure (OP)
|
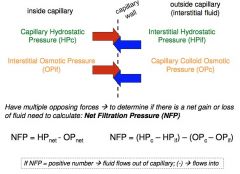
of a solution is force of osmotic water movement
in capillaries = Capillary Colloid Osmotic Pressure (OPc) abundant plasma proteins (albumins) create OPc Force fluids INTO capillary in interstitial fluid = Interstitial Osmotic Pressure (OPif) Force fluids OUT of capillary |
|
|
Colloid Osmotic Pressure
|
created by presence of large molecules (e.g. plasma proteins) that can't move across membrane
• protein molecules "pull" water toward them (encourage osmosis) |
|
|
At arterial end of capillary →
|
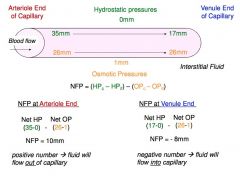
fluid moves out of capillary into interstitial fluid (filtration)
|
|
|
At venous end of capillary →
|
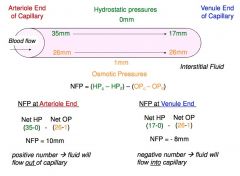
fluid moves into capillary out of interstitial fluid (reabsorption)
|
|
|
The Transition Point:
|
Between filtration and reabsorption
—closer to venous end than arterial end Therefore → capillaries filter more than reabsorb Excess fluid enter lymphatic vessels |
|
|
Fluid Recycling
|
Water continuously moves out of capillaries, and back into bloodstream via the lymphatic system
|
|
|
Fetal Circulation
|
• Embryonic lungs and digestive tract nonfunctional
• Respiratory functions and nutrition provided by placenta |
|
|
Fetal Circulation
Blood flows to the placenta: |
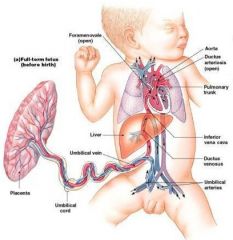
through pair of umbilical arteries
-arise from internal iliac arteries and enter umbilical cord |
|
|
Fetal Circulation
Blood returns from placenta: |
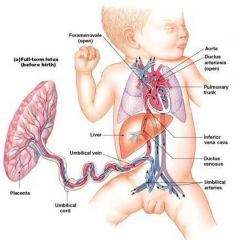
in a single umbilical vein
-drains into ductus venosus |
|
|
Fetal Circulation
Ductus venosus: |
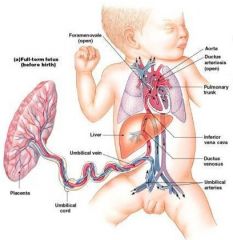
empties into inferior vena cava
|
|
|
What are the two fetal pulmonary circulation bypasses?
|
foramen ovale and ductus arteriosus
|
|
|
Foramen ovale
|
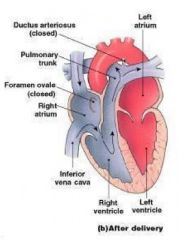
• interatrial opening
• covered by valve-like flap • directs blood from right to left atrium |
|
|
Ductus arteriosus
|
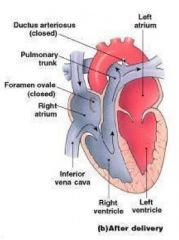
• short vessel
• connects pulmonary and aortic trunks |
|
|
Cardiovascular Changes at Birth
|
• Pulmonary vessels expand
• Reduced resistance allows blood flow • Rising O₂ causes ductus arteriosus constriction • Rising left atrium pressure closes foramen ovale |
|
|
NFP =
|
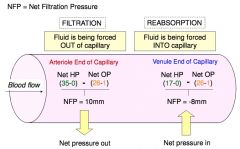
Net Filtration Pressure
|

