![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
13 Cards in this Set
- Front
- Back
|
Purpose of acute inflammation: |
Sentinel cells found microbial insult and/or tissue damage, and need reinforcement
1. Delivery of leukocytes and plasma proteins to site of injury - vasodilation - vascular permeability - emigration, activation and chemotaxis of leukocytes (leave blood and go into tissues) 2. Elimination of agent (effector processes) 3. Trigger acquired immunity 4. Initiate tissue repair 5. Systemic responses - fever, leukocytosis etc. |
|
|
5 signs of acute inflammation |
1. Rubor (redness) 2. Tumor (swelling) 3. Calor (heat) 4. Dolor (pain) 5. Functio Laesa (loss of function)
*mainly consequences of local vascular changes |
|
|
Initiators of acute inflammation: |
Infections: - bacteria - viruses - parasites - microbial toxins Trauma Physical and Chemical injury: - cold (frostbite) - burns - irradiation Tissue Necrosis Foreign body: - dirt - suture Immune Reactions: - hypersensitivities - autoimmune diseases |
|
|
What happens when sentinel cells detect microbial or parasitic products in the host tissues? |
Sentinel cells such as macrophages express PRRs so they can monitor tissues for PAMPS/DAMPS
When they find a PAMP, it leads to signaling cascades within the macrophage, which activates it
The macrophage then synthesizes and releases proinflammatory cytokines (ILs, TNF) or chemokines that act as signals for other inflammatory cells (to release even more) and blood vessels in the area
These chemokines/cytokines set up a concentration gradient as they move away from the macrophage and that helps to direct other luekocytes like neutrophils to the site of insult = chemokine-directed chemotaxis |
|
|
How are mast cells involved in acute inflammation? |
Cytokines produced by macrophages activate the mast cell to rapidly amplify proinflammatory signals
Mast cells sit near blood vessels and nerves and contain granules with histamine and serotonin (vasoactive compounds), associated with type 1 hypersensitivities (allergies)
the degranulation of mast cells (ie. release of serotonin and histamine) causes changes to local vasculature |
|
|
How are eicosanoids and cytokines different? |
Cytokines are proteins, can travel further distances
Eicosanoids (leukotrienes and prostaglandins) are oxidized derivatives of fatty acids - short half life and act locally on vasculature and endothelium |
|
|
What are the vascular changes that occur in acute inflammation? |
1. Vasodilation and local stasis of blood flow 2. Increased vascular permeability 3. Expression of cell-adhesion molecules on vascular endothelium |
|
|
What are the mediators of local vascular changes? |
1. Histamine, serotonin 2. Nitric Oxide 3. Prostaglandins and leukotrienes |
|
|
Histamine: |
Mast cell degranulation adjacent to blood cells
Induced by: - trauma/cold/heat - immune reactions (IgE) - C3a and C5a (from complement activation pathway) - Histamine releasing proteins from leukocytes - Neuropeptides (substance P) - Cytokines (IL-1 and IL-8)
Binds to H1 receptors on endothelial cells
Dilation of arterioles and increased permeability of venules |
|
|
Nitric Oxide: |
- Released from endothelial cells and macrophages - Induces relaxation of vascular smooth muscle - Also anti-inflammatory role (reduces leukocyte recruitment) - NO is microbicidal |
|
|
Prostaglandins and leukotrienes |
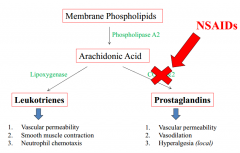
|
|
|
Why is vasodilation and stasis of blood flow important in acute inflammation? |
- Increased blood to area - Expansion of capillary beds - Decreased velocity of flow - Increased permeability (fluid loss)
All allow more leukocytes to travel to site of injury/infection, blood slows down enough so that the leukocytes can exit the blood into the tissues |
|
|
What mediators influence vasodilation/stasis of blood flow? |
Histamine NO Prostaglandins |

