![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
54 Cards in this Set
- Front
- Back
|
defiene hypertension |
elevated systemic blood pressure |
|
|
what is normotension |
normal blood pressure range |
|
|
what is the range for systolic and diastolic blood pressure for a normotensive person |
systolic < 130 diastolic < 85 |
|
|
define hypertension |
abnormally high chronic blood pressure |
|
|
what is the range for systolic and diastolic blood pressure in mild hypertension |
systolic --> 140-159mmHg diastolic --> 90-99 |
|
|
what is the range for systolic and diastolic blood pressure in very severe hypertension |
systolic = >210 diastolic= >120 |
|
|
what proportion of hypertensive cases are primary |
90% |
|
|
what are the causes of primary hypertension |
smoking diet (esp. salt) obesity and lack of exercise genetic factor |
|
|
what proportion of hypertensive cases are secondary |
<10% |
|
|
what are the causes of secondary hypertension |
renal hypertension pheochromocytoma |
|
|
what is pheochromocytoma |
a small vascular tumor of the adrenal medulla, causing irregular secretion of epinephrine and norepinephrine, leading to attacks of raised blood pressure, palpitations, and headache |
|
|
what are the further conditions which can be caused as a result of hypertension |
atherosclerosis stroke heart failure renal failure retinopathy (disease of the retina which results in impairment or loss of vision) |
|
|
statistically what is the benefit of reducing blood pressure |
40% reduction of stroke >50% reduction in heart failure |
|
|
what is the formula for blood pressure |
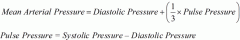
there are 2 btw: BP = CO X SVR |
|
|
what is the equation for Cardiac Output |
HR x SV |
|
|
what are the 3 different ways that the sympathetic nervous system can be targeted to lower blood pressure |
can target heart can target blood vessels can reduce renin release from kidney |
|
|
what type of receptors are targeted to reduce the effects on the heart and reduce renin release from the kidney? |
Beta-1 |
|
|
what type of receptors are targeted to reduce the effect on blood vessels |
alpha-1 |
|
|
how can the kidney be targeted to lower blood pressure and through what kind of drug can this effect be achieved |
kidney can reduce blood volume this can be achieved through the use of diuretics (helps you pee) |
|
|
which hormones can be inhibited to lower blood pressure |
RAA (renin-angiotensin-aldosterone) system can be inhibited: 1) inhibit ACE (Angiotensin converting enzyme) 2) angiotensin receptor blockers |
|
|
how can arterioles be targeted to lower blood pressure |
Vasodilatation of peripheral resistance arterioles through Ca2+ channel blockers |
|
|
give 2 examples of adrenoceptor blockers and give their type of beta blocker (1 or 2) |
propanolol --> B1 and B2 atenolol --> B1
|
|
|
what action do b-adrenoceptor blockers have and are they reversible |
they are competitive reversible antagonists |
|
|
how do b-adrenoceptor blockers work to decrease blood pressure |
decrease in blood pressure via blockade of b1 sympathetic tone on heart and reduction in renin release from kidney also decrease in HR SV and CO (all 3 form equation pretty much) |
|
|
what are the adverse side effects to B-adrenoceptor blockers |
(a) Exacerbate asthma (block of B2–absolute contraindication) (b) Intolerance to exercise (c) Hypoglycaemia |
|
|
give 2 examples of adrenoceptor blockers and give their type of alpha blocker (1 or 2) |
phentolamine (a1 and a2) doxazosin (a1 selective) |
|
|
what action do a-adrenoceptor blockers have and are they reversible |
same as beta, they are competitive reversible antagonists |
|
|
how do alpha adrenoceptors work to decrease blood pressure |
they decrease bp by: -decreasing sympathetic tone in arterioles (a1) -decreasing peripheral resistance |
|
|
what are the adverse effects of alpha-adrenoceptor blockers |
(a) Postural hypotension (loss of sympathetic venoconstriction) (b) Reflex tachycardia (via baroreceptors)
(reflex tachycardia is when the blood pressure falls and the heart beats faster to try and "fix it") |
|
|
give 2 examples of ACE inhibitors |
captopril and enalapril |
|
|
where is ACE found and what is its function |
it is found on the vascular endothelial surface it converts angiotensin I to active II |
|
|
what is the main characteristic of angiotensin II |
it is a vasoconstrictor |
|
|
what is the mechanism through which ACE work |
1) they prevent the formation of Angiotensin II, which is a vasoconstrictor, this means the peripheral resistance falls and bp lowers too
2) Reduced blood volume (loss of angiotensin II- stimulated release of aldosterone, thus reduction of renal reabsorption of Na+ and water) |
|
|
what are the adverse effects of ACE inhibitors |
Generally very well tolerated but: (a) Sudden fall in BP on 1st dose (b) Persistent irritant cough – due to reduced breakdown of bradykinin, a peptide that activates sensory nerves in lung tissue |
|
|
what are the 2 receptor sub-types of angiotensin II receptor blockers |
AT1 and AT2 |
|
|
what do the AT1 Angiotensin II receptor blockers do |
AT1 receptor mediates vasoconstrictor and aldosterone-releasing actions of angiotensin II |
|
|
give 2 examples of AT1 blockers and what type of agents are these drugs |
Losartan and candesartan antihypertensive agents |
|
|
do angiotensin II receptor blockers have any side effects |
no apparent ones nah |
|
|
give an example of a diuretic |
bendroflumethiazide |
|
|
how do diuretics lower blood pressure |
they reduce the blood volume they do this by reduced renal absorption of Na+ and water (it also has a vasodilator action which may contribute since it lowers peripheral resistance) |
|
|
what are the adverse effects of diuretics |
they cause a decrease in plasma K+ |
|
|
give 3 examples of Calcium channel blockers |
verapamil, diltiazem and nifedipine |
|
|
when do L-type voltage operated Calcium channels open, and where does this Calcium then enter into following this |
upon membrane depolarisation enters into cardiac and vascular smooth muscle |
|
|
what are the different methods of blocking L-type voltage operated Calcium channels |
1. Open channel block (cork in a bottle!) 2. Allosteric modulation |
|
|
what drugs work by the open channel block mechanism in the L-type voltage operated Calcium Channels |
verapamil and diltiazem |
|
|
what is the method of action for allosteric modulation in L-type voltage operated Calcium channel blocking what type of drugs work in this way? |
bind at allosteric site and reduce channel opening nifedipine works this way |
|
|
what is the order of tissue selectivity in terms of the drugs nifedipine, dilitiazem and verapamil in relation to smooth and cardiac muscle |
Smooth muscle: nifedipine > diltiazem > verapamil Cardiac muscle: verapamil > diltiazem > nifedipine |
|
|
how do Calcium channel blockers lower blood pressure |
Reducing peripheral resistance (block of Ca2+ entry into vascular smooth muscle --> vasodilatation) Reducing cardiac output (block of Ca2+ entry into cardiac muscle - heart rate (HR) and stroke volume (SV) both reduced) |
|
|
what are the potential adverse effects of calcium channel blockers |
(a) Headache (c) Cardiac dysrhythmias (negative chronotropic effect and slowed conduction) |
|
|
if a person is aged 55 or under, what is the first drug to put them on |
ACE inhibitor or low cost angiotensin II receptor blocker |
|
|
if a person is aged 55 or older or they are of african or Caribbean origin, what is the first drug they should be put on according to SIGN guidelines |
Calcium channel blocker |
|
|
As part of "step 1" a patient should be put on ACE/ angiotensin II receptor blocker if they are under the age of 55, and on a Calcium channel blocker if they are over the age of 55 or of African/Caribbean origin, what is step 2 |
they should be put on ACE/angiotensin II receptor blocker as well as a calcium channel blocker |
|
|
As part of "step 1" a patient should be put on ACE/ angiotensin II receptor blocker if they are under the age of 55, and on a Calcium channel blocker if they are over the age of 55 or of African/Caribbean origin. In step 2 they would be put on both of these, what is step 3? |
they should be put on ACE/angiotensin II receptor blocker as well as a calcium channel blocker and also a thiazide-like diuretic |
|
|
As part of "step 1" a patient should be put on ACE/ angiotensin II receptor blocker if they are under the age of 55, and on a Calcium channel blocker if they are over the age of 55 or of African/Caribbean origin. In step 2 they would be put on both of these, in step 3 they are put on both of these as well as a thiazide-like diuretic, what is step 4 known as and what are the steps undertaken in step 4? |
they should be put on ACE/angiotensin II receptor blocker as well as a calcium channel blocker and also a thiazide-like diuretic. Lastly they should also consider an alpha or beta blocker
they should also consider seeking expert advice |

