![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
13 Cards in this Set
- Front
- Back
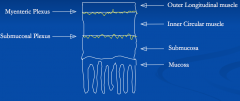
GI structure |
From the oesophagus to the anal canal, it has a similar basic structure - Primed by pacemaker cells (interstitial cells of Cajal) = initiate a spreading basal electrical rhythm (BER) - Spike potentials occur when the threshold is crossed. Causes muscle contraction Sensitive to stretch = stimulation of gut activity directly or via local neural reflexes. Co-ordination by the myenteric plexus |
|

|
Chyme activates mechanoreceptors → engage with myenteric plexus - Upstream = contraction of muscle - Downstream, release of vasoactive intestinal polypeptide (VIP) = relaxation of muscle Direction of propulsive movements downstream |
|
|
Gut activity - Modified by extrinsic autonomic nerves - Also modified by locally produced chemicals & hormones |
Modified by extrinsic autonomic nerves - PNS- ↑ motility via ACh on mAChR's, or indirectly by modifying activity of interstitial cells of Cajal - SNS- ↓ motility: - Directly via NA on β-adrenoceptors - Indirectly via NA on α₂-adrenoceptors, presynaptically on parasympathetic nerve terminals = ↓ ACh release from parasympathetic nerves |
|
|
Stages of GI motility |
1. Mastication 2. Deglutition- 2 stages of swalling, oropharyngeal & oesophageal The oesophagus is a hollow tube separated at each end by sphincters - Zone of elevated pressure prevents transit from 1 region to another & separates oesophagus from stomach Swallowed food is pushed one 1 end by peristalsis (wave-like contraction) |
|
|
Oesophageal peristalsis |
Mechanoreceptors in pharynx detect bolus, initiate 1⁰ peristaltic wave - Controlled by vagal nerve, speed is 5cm/s, lats 7-10s, gravity assisted, rate of movement is proportional to viscosity of bolus If food is not projected to stomach, a 2nd wave is initiated by local vago-vagal reflexes Empty oesophagus- small intermittent waves, salivary swallowing (7-70/hr) |
|
|
Gastric motility |
Primed by pacemaker cells, initiate BER (every 3-5min) - Not always associated with peristaltic wave, just when underlying tissue is at its more excitable Smooth muscle excitability is controlled by: - Myogenic properties of sm cells - Intrinsic & extrinsic nerve activity - Hormones or locally produced chemicals |
|
|
Gastric motility |
Empty stomach = feeble contractions Full stomach= 1st hr peristaltic waves weak as pyloric sphincter is closed, later waves more powerful - Associated with mixing of gastric content & emptying into duodenum |
|
|
Control of gastric motility |
Neural control- vagal relaxatory fibres = relaxation in corpus & fundus, mediated by VIP. Stimulated by oesophageal & gastric distention - SNS via NA inhibitis, via inhibition of PNS ganglionic transmission. Stimulated via distention of small intestines Vagal fibres release ACh to stimulate gastric motility Hormones: - Stimulatory- gastrin (antrum), motillin (from small intestine) - Inhibitory- gastrin (proximal stomach), secretin, CCK |
|
|
Rate of movement of contents - Meal composition |
Rate at which gastric contents pass into duodenum depends on motility & meal composition - Standard meal is fastest, protein is medium, lipids are slow - Volume- greater the volume of contents, the faster the rate of emptying - Fragment size- solid fragments <1mm only pass into duodenum suspended in liquid phase - Osmolarity- osmolarities > & <200mOsm slow emptying - Acid- excess acid in small intestine slows gastric emptying - Fat- fat in upper small intestine slows gastrin emptying |
|
|
Small intestine motility |
In the small intestine, intestinal contents are mixed with secretions of mucosal cells & with pancreatic juice & bile 2 types of muscular contraction: - Segementing - mixing. Occurs in circular muscle, moves chyme to & fro, increases exposure to mucosal surface. BER duodenum 12/min, terminal ileum 9/min = allows movement down the tract - Peristaltic- more longitudinal over short distance. After a meal, occasional long distance wave (migrating motility complex) |
|
|
Control of small muscle motility |
1. Myogenic mechanisms- stretch 2. Myenteric plexus (local regulation). Stimulatory = ACh, gastrin, CCK. Inhibitory = VIP, opiods, NO 3. Extrinsic nerves- some vagus, sympathetic (presynaptic inhibition), direct 4. Local chemicals- fat slows transit time |
|
|
Large intestinal motility |
Food takes ∼12 hours to reach terminal ileum - Ileal-caecal sphincter prevents retrograde movement of bacteria from colon Large intestine reabsorbs water & stores faeces. Movement slow & non-propulsive. Haustral contractions kneads content. 2/hr - 3-4 per day powerful contractions drive contents to distal large intestine prior to defecation, initiated by food in stomach (gastro-colic reflex) |
|
|
Defecation |
Rectum is usually empty - Arrival of faecal material = desire to defecate via sensory nerves = peristaltic wave in colon & internal anal sphincter relaxes Anus- tonically contracted ring of smooth muscle with voluntary control of external anal sphincter Defecation reflex: Myenteric plexus is weak, PS spinal reflex present, voluntary effect |

