![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
31 Cards in this Set
- Front
- Back
|
standard definition of pathological healing
|
outcome of inflammation that is characterized by regeneration and/or scarring
|
|
|
standard definition of pathological regeneration
|
replacement of injured cells by healthy cells where full function is re-established
|
|
|
standard definition of pathological scarring (aka fibrosis)
|
occurs in tissue that cannot regenerate cells, so the cells used in replacement are connective tissue. full function not re-established
|
|
|
standard definition of pathological repair
|
healing through scarring, exclusively
|
|
|
in reference to the cell cycle, which cells in the body are examples of permanent nondividing cells?
|
neuron
cardiac muscle skeletal muscle |
|
|
what stage of the cell cycle do cells that are continuously dividing reside in even if they are not active in the cell cycle?
|
G0 = quiescent(stable) cells
|
|
|
labile tissue
|
tissue that is continually dividing, have a short G0 stage, contain stem cells.
ex. epithelium, mucosa, bone marrow |
|
|
stable/quiescent tissue
|
tissue that has a low level of replication, have a long G0 stage, reenter the cell cycle only under certain conditions
ex. liver, pancreas, kidney fibroblast, condrocyte, osteocyte, smooth muscle vascular endothelial leukocytes |
|
|
permanent/non-dividing tissue
|
left cell cycle forever, can no longer enter any part of the cell cycle including G0
ex. cardiac muscle skeletal muscle neuron |
|
|
stem cells
|
progenitor cells with unlimited proliferative capacity. replicates in an asymmetric way so that they can perpetually self-generate
|
|
|
adult stem cells
|
limited "niches" of stem cells that are much more limited than embryonic stem cells
|
|
|
what are the "niches" of adult stem cells?
|
isthmus of gastric glands
base of crypts of the colon bulge area of hair follicle limbus of cornea canals of Hering in the liver olfactory bulb dentate gyrus satellite cells in skeletal muscles |
|
|
what are the two main components of the extracellular matrix?
|
interstitial matrix
basement membrane |
|
|
collagen
|
one of the most important components of the extracellular matrix
|
|
|
What are the 4 most common types of collagen and where are they found?
|
Type I - skin, bone, tendons, organs
Type II - catrilage, vitreous humor Type III - ganulation tissue, keloids, uterus, embryonic tissue Type IV - basement membrane Type I, Type III are used most in healing |
|
|
What three conditions must be met for regeneration to be able to occur?
|
1) cells must be labile or stable cells
2) injurious area must have some surviving labile or stable cells 3) extracellular matrix must be intact for new cells to build upon |
|
|
What happens if any of the three conditions are not met for successful regeneration?
|
scarring/fibrosis
|
|
|
What are the 4 conditions that must occur for scarring to be successful?
|
1) angiogenesis/neovascularization
2) migration and proliferation of fibroblasts 3) deposition of ECM components, including collagen 4) organization of fibrous tissue into mature scar (remodeling) |
|
|
What is remodeling with respect to fibrosis in pathological healing?
|
organization of fibrous tissue into mature scar
|
|
|
growth factors
|
chemicals that are released for the first 24 hours after injury that guide fibroblasts and vascular endothelial cell proliferation leading to the formation of granulation tissue (soft, pink, appears 3-5 days after injury)
|
|
|
what four specific functions do growth factors serve?
|
1) mitogenesis - reentry of G0 into cell cycle
2) cell differentiation 3) chemotaxis 4) angiogenesis |
|
|
Where does Type III collagen come into play during scarring/fibrosis?
|
during fibroblast proliferation, new fibroblasts will secrete Type III collagen refore remodeling is complete
|
|
|
What are MMPs?
|
matrix metalloproteinases are enzymes that will degrade portions of the ECM in order to create the correction structure in the final, remodeled scar.
|
|
|
What mineral do MMPs depend on?
|
zinc
|
|
|
What is the difference between granulation tissue and scar tissue?
|
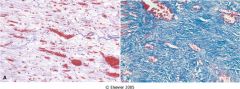
granulation tissue is made as a precursor to scar tissue. it had less collagen and more vascularization than scar tissue.
(pic) |
|
|
What is the difference between cutaneous wound healing by the first intention compared to healing by the second intention?
|
1) first intention - wound with opposed edges healing
2) second intention - wound with separated edges healing |
|
|
What are the steps of healing by the first intention?
|
Day 1 - scalpel blade makes incision
Day 1 - space fills with clotted blood Day 1 - acute inflammation w/ influx of neutrophils Day 3 - now chronic inflammation w/ influx of macrophage Day 3 - granulation tissue starts to form, and regeneration of epidermis Day 5 - granulation tissue has filled incision space 2 weeks - collagen has accumulated, decline in vascularization 1 month - epidermis is fully regenerated, remodeling is almost complete 3 months - complete scarring/healing has occurred |
|
|
What are the steps of healing by the second intention?
|
wound contracts by myofibroblasts to close wound edges
everything else is like first intention except exaggerated |
|
|
Wound strength guidelines
|
when sutures are removed = 10% strength of original strength
3 months after removal = 80% of strength of original strength |
|
|
hypertrophic scar
|
raised red, shiny scar appearing over site of the initial wound due to excess fibroblast activity and collagen deposition (type 3)
|
|
|
Keloid
|
scar that grows outside of the boundaries of the original wound, can be tumor-type, excessive production of Type 3 collagen
African Americans are more susceptible like hypertrophic scars that get out of hand! |

